* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download 9cd41c0f1293979
Survey
Document related concepts
Transcript
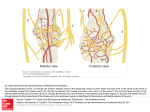
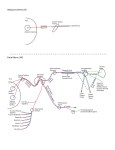
AL-Qassim University Faculty of Medicine (third year- 1435-2014) Overview of the anatomy of cranial nerves (from I-XII) Prepared by : Dr / Amani Almallah Cranial Nerves: I - XII 12 Pairs of nerves, Numbered from one (I) to twelve (XII). Attach to Ventral surface of brain & exit brain through foramina in skull I + II attach to Forebrain (cerebrum + diencephalon) From III to XII attach to Brainstem 2 attached to mid brain Middle 4: are attached to the pons Lower 4 are attached to the medulla Functional classification of cranial nerves AFFERENT (SENSORY) SOMATIC VISCERAL GENERAL VII, IX, X Exteroceptice nerves sensation V SPECIAL (special sense hearing & vision II &VIII GENERAL EFFERENT (MOTOR) SOMATIC SPECIAL GENERAL smell and taste (I,VII,IX& X muscles of eye and tongue Cranial nerves III, IV, VI, XII. VISCERAL GENERAL visceral motor nuclei of nerves relayed in parasympathetic ganglions (III, VII, IX & X). SPECIAL muscles derived from brachial (pharyngeal) arches V, VII , IX and X & XI Functional classification of fibers of cranial nerve General somatic afferent fibers (GSA): transmit exteroceptive and proprioceptive impulses from head and face to somatic sensory nuclei through the trigeminal nerve. Special somatic afferent fibers (SSA): transmit sensory impulses from special sense organs of vision CN II, equilibrium and hearing to the brain (CN VIII). General visceral afferent fibers (GVA): transmit interoceptive impulses from the viscera to the visceral sensory nuclei of VII, IX, X nerves . Special visceral afferent fibers (SVA): transmit sensory impulses from special sense organs of smell and taste to the brain sensation VII, IX, X & smell sensation cranial nerve (CN I). General somatic efferent fibers (GSE): innervate skeletal muscles of eye and tongue Cranial nerves III, IV, VI, XII. Special visceral efferent fibers (SVE): transmit motor impulses from the brain to skeletal muscles derived from brachial (pharyngeal) arches of embryo. These include the muscles of mastication, facial expression and swallowing Cranial nerves V(1ST arch), VII (2nd arch), IX (3rd arch) and X & XI (cranial part) for (4th& 6th arch). General visceral efferent fibers (GVE): transmit motor impulses from the general visceral motor nuclei and relayed in parasympathetic ganglions. The postganglionic fibers supply cardiac muscles, smooth muscles and gland as Edinger-westphal nuceus of III, superior and inferior salivary of VII, IX respectively, dorsal nucleus of vagus (X). Olfactory Nerve (= CN I) Functional classification: SVA(special visceral afferent) – purely sensory Carry smell sensation Originated from: Olfactory Epithelium in nasal cavity & filaments passes through cribriform plate of ethmoid. Only CN directly attached to Cerebrum Optic Nerve Type: Special Somatic Afferent (SSA) Function: Vision Formed by axons of the ganglion cells in the retina. • The nerve passes posteromedially in the orbit, exits through the optic canal to enter the middle cranial fossa, running postero-medially towards the optic chiasma where partial decussation of its fibres occurs. . Deep origin of III, IV and VI nerves Functions and nuclei: The oculomotor: GSE , GVE (Motor nucleus of III & Edinger-Westphal nucleus). The trochlear: GSE: Motor nucleus of IV. The abducent: GSE: Motor nucleus of VI IV nucleus VI nucleus VII nucleus VI IV III 7 Cranial Nerves Controlling the Extra-ocular Muscles The Oculomotor nerve Functions: GSE .GVE Deep origin: 1-Motor nucleus of oculomotor (GSE): located in the mid brain, at the level of superior colliculus 2- Edinger-Westphal nucleus (GVE) situated behind main motor nucleus. Axons from the Edinger-Westphal nucleus terminate in the Ciliary ganglion. Postganglionic fibers pass through the short ciliary nerves to the eyeball, where they supply the sphincter pupillae muscle of the iris and the ciliary muscle. Superficial origin: it emerges on the anterior surface of the midbrain in the interpeduncular fossa, on the medial border of cerebral peduncle & passes forward between the posterior cerebral and superior cerebellar arteries. In the middle cranial fossa lies in the lateral wall of the cavernous sinus. As it leaves the sinus, it divides into two divisions, superior and inferior both will enter the orbital cavity through the superior orbital fissure . Its distribution: The superior division passes above the optic nerve and ends by supplying: ▪The superior rectus ▪The levator palpebrae superioris. The inferior division passes below the optic nerve and ends by supplying: ▪The inferior rectus ▪ The medial rectus ▪The inferior oblique ▪ Branch from the nerve to inferior oblique to the ciliary ganglion. Occulomotor nerve palsy • Lesion results in: – Lateral squint – Ptosis – Diplopia – Pupillary dilatation – Loss of accommodation – Impaired downward & outward movement of the eye ball on the damaged side. The preganglionic parasympathetic fibers run superficially in the nerve and are therefore the first axons to suffer when a nerve is affected by external pressure. Consequently, the first sign of compression of the occulomotor nerve is ipsilateral slowness of the pupillary response to light. The Trochlear nerve Function: GSE (purely motor) Deep origin: The motor nucleus of the trochlear nerve in located in the anterior part of the periaqueductal grey matter at the level of inferior colliculus. Superficial origin: From the back of the midbrain below the inferior colliculus on the sides of the frenulum veli. The nerve emerges immediately from the posterior surface of brain stem then passes on the lateral border of the cerebral peduncle to passes anteriorly. It passes through middle cranial fossa in the lateral wall of the cavernous sinus below the oculomotor and above the ophthalmic nerves, then enters the orbit through the superior orbital fissure outside the common tendinous ring. In the orbit it passes medially to enter the orbital surface of the superior oblique muscle (SO 4). So: The tochlear nerve the only cranial nerve exits from the posterior aspect of the brain stem. It supplies superior oblique muscle of the eye ball (SO4) Trochlear nerve palsy Lesion results in diplopia & inability to rotate the eye infero-laterally. The eye deviates; upward and slightly inward. Person has difficulty in walking downstairs The Abducent nerve Function: GSE Deep origin: 1- Motor nucleus of the abducent nerve in floor of upper part of 4th ventricle beneath the facial colliculus. Superficial origin: The nerve exits At the junction of the pons and the Upper border of medulla at the pyramid (pontomedullary angle) It then, enters the floor of the cavernous sinus lying lateral to the internal carotid artery. It enters the orbit through the superior orbital fissure within the common tendinous ring to end by supplying the lateral rectus (LR 6). So The Abducent nerve then enters the orbit through the superior orbital fissure Abducent nerve palsy Lesion results in: Medial squint with an inability to direct the affected eye laterally A nuclear lesion may also involve the nearby nucleus or axons of the facial nerve, causing paralysis of all the ipsilateral facial muscles. The 3rd, the 4th and the 6th nerve motor nuclei receive: Corticonuclear fibers from both cerebral hemispheres. Tectobulbar fibers from superior colliculus. Fibers from medial longitudinal bundle (MLB) by which the nuclei are connected to each other. Trigeminal nerve Functions: it is the largest cranial nerve. It has four nuclei one motor & three sensory. It carries motor supply to the muscles of mastication and transmits sensory information from the face, oral and nasal cavities, and most of the scalp. Its function classification: its four nuclei give (GSA &SVE) 1- Motor nucleus supplies: Special visceral efferent (SVE) Its axon form the motor root of trigeminal which join the mandibular nerve. It lies in the middle of pons in line with nucleus amniguus and facial nucleus. It supplies: 1- Muscles of mastication ;temporalis, masseter, medial & lateral pterygoid. 2- Anterior belly of digastric & mylohyoid muscles. 3-Tensor tympani & tensor palati. (muscles of 1st pharyngeal arch) Nuclei of General somatic afferrent: (GSA) 2- Principal (main) sensory nucleus: it is GSA nucleus, lies in the middle of the pons lateral to the motor nucleus. It receives tactile impulses from face. 3- Mesencephalic nucleus: it is GSA nucleus, called mesencephalic as it extends to the midbrain & junction between (pons & midbrain). It receives proprioceptive fibers from face. 4- Spinal nucleus: it is GSA nucleus. Lies in the lower part the pons, Extending to the whole length of medulla & upper 2-3 cervical segments of spinal cord). It receives pain & temperature sensations from face. Superficial origin: Emerges From the ventral surface of the pons by a short trunk has small motor root & large general sensory root. Course and relations: It is the shortest cranial nerve, its trunk is formed of small motor and large sensory roots The trigeminal ganglion which lies near the apex of the petrous bone on trigeminal impression. On the surface of the ganglion it divided into its three main divisions The three main divisions of the trigeminal nerve: I-The ophthalmic nerve (sensory) II- The maxillary nerve (sensory) III- The mandibular nerve (which is joined with the motor root). Distribution of the function of the trigeminal nerve divisions The Ophthalmic nerve (V1) Function: GSA (pure sensory) Course and relations: It is the smallest of the three branches of the trigeminal. It passes forwards in the lateral wall of the cavernous sinus below the trochlear nerve and above the maxillary nerve. Just before it enters the orbit through the superior orbital fissure, it divides into three branches; lacrimal, frontal & nasociliary. 1- The lacrimal nerve: Enters the orbit in the lateral part of the superior orbital fissure it passes along the lateral wall of the orbit. It receives communication (parasympathetic) from the zygomatico-temporal nerve which carries secretory fibres to the lacrimal gland. It supplies the lacrimal gland, and gives a palpebral branch to the upper eyelid. 2- The frontal nerve: It Is the largest branch of the ophthalmic nerve, Enters the orbit through the superior orbital fissure medial to the lacrimal nerve. In the orbit, the frontal nerve ends by dividing into: 1-Supratrochlear nerve: to the forehead and the scalp. 2- Supraorbital nerve: to the frontal air sinus, face and the scalp. 3-The nasociliary nerve Enters the orbit through the superior orbital fissure. It ends by giving the following branches: 1- Sensory branch to the ciliary ganglion 2- Long ciliary nerves : to the eye ball. 3- Posterior ethmoidal nerve: through the posterior ethmoidal canal to the ethmoidal and sphenoidal air sinuses 4- Infratrochlear nerve: to the lower eyelid and the face. 5- Anterior ethmoidal nerve Summary of ophthalmic nerve It is the smallest branch of the trigeminal. Only sensory Supplies : cornea, conjunctiva, upper lid, forehead anterior part of the scalp & nose. Its course: emerges from trigeminal ganglion lat wall of cavernous sinus Three branches in anterior part of cavernous sinus Lacrimal, Nasociliary & Frontal Superior orbital fissure orbit The maxillary nerve a.Function: GSA (pure sensory) b.Course and relations: It passes in the lateral wall of the cavernous sinus below the ophthalmic nerve. It leaves the cranial cavity through the foramen rotundum to the pterygopalatine fossa, then through the pterygomaxillary fissure to the infratemporal fossa. It passes through the infraorbital groove and canal in the floor of the orbit, continues as the infraorbital nerve which it appears in the face through the infraorbital foramen. Branches: I- In the cranial cavity: meningeal branch to the dura matter of middle meningeal fossa II- In the pterygopalatine fossa: 1- Ganglionic: sensory branch to the pterygopalatine ganglion 2- Zygomatic nerve: divides into zygomaticotemporal and zygomaticofacial nerves to the face and scalp (the zygomaticotemporal nerve carries secretory fibers to the Maxillary nerve Maxillary nerve during its passage through the infra-temporal fossa (to sphenopalatine fossa) lacrimal gland from the ganglion to the lacrimal nerve). . 3- Posterior superior alveolar nerve: pierces the infratemporal surface of the maxilla to supply the maxillary sinus and the molar teeth, it give branches to the cheek and gum. III- In the infraorbital canal (branches of the infraorbital nerve): 1- Middle superior alveolar: to the upper premolar teeth 2- Anterior superior alveolar nerve: to the incisor and canine teeth, it sends a nasal branch to the nose and the nasal septum IV- Finally; In the face: to supply the face 1- Palpebral nerve 2- Nasal nerve 3- Superior labial nerve Summary of maxillary nerve 2nd division of the trigeminal nerve. It is pure sensory. Its course: emerges from trigeminal ganglion lat wall of cavernous sinus To the foramen rotundum To pterygopalatine fossa then in groove on the posterior surface of maxilla Continues through the infra-orbital fissure in the floor of the orbit as Infra-orbital nerve through the infra-orbital foramen to appears in the face, dividing into its three terminal branches; Palpebral, Nasal & Superior labial nerves. The mandibular nerve Functions: GSA, SVE (mixed nerve) Course and relations: Is the largest branch of the trigeminal nerve, formed of two roots a large sensory and small motor It leaves the skull through the foramen ovale to the infratemporal fossa where the two roots unite to form the nerve trunk The trunk lies medial to the lateral pterygoid muscle It is very short trunk which divides into anterior and posterior divisions Branches: From the trunk then from the anterior & posterior division. I- Branches From the trunk 1- Nervus spinosus (sensory, meningeal): it passes up to the cranial cavity through the foramen spinosum to supply the dura matter of the middle cranial fossa. 2- Nerve to medial pterygoid (motor): is the motor to the medial pterygoid muscle, it passes through the otic ganglion without relay then exits to supply the tensor palati and tensor tympani muscles. II-Branches from the anterior division: (3 motor branches to 3 muscles of mastication + 1 sensory): 1- Deep temporal nerves: to the temporalis muscle 2- Nerve to lateral pterygoid: supplies lateral pterygoid muscle. 3- Masseteric nerve: pass through the mandibular notch to masseter. 4- Buccal nerve (sensory): passes between the two heads of the lateral pterygoid to the face to supply (sensation) to the skin over the cheek. III- Branches from the posterior division 1- The auriculotemporal nerve (sensory): It arises by two roots which surrounds the middle meningeal artery. And unites behind the artery, then it passes deep to the neck of the mandible within the substance of the parotid gland to leave the gland through its upper end of the gland to the scalp. The auriculotemporal nerve is sensory supply to: I- auriculotemporal nerve carries postganglionic secretormotor fibres from the otic ganglion & sensory fibers to the parotid gland. II- skin of upper 2/3 of the lat surface of the auricle & skin of the external acoustic meatus and the outer covering of the ear drum . III- posterior ½ of temporal area. IV- atricular branches to Tempro-mandibular joint (TMJ). 2- The lingual nerve (sensory): As it originates deep to the lateral pterygoid muscle, it is joined by the chorda tympani branch of the facial nerve in the infratemporal fossa. Then descends downwards between the medial pterygoid muscle and the ramus of the mandible, then it lies behind the root of the (last) third molar tooth where is covered by the mucous membrane of the mouth (dangerous position). In the submandibular region, it passes between the mylohyoid laterally and the hyoglossus muscles deep to the submandibular gland. Termination: The terminal branches of the lingual nerve carries sensations from the mucous membrane of the mouth, the gum, the anterior 2/3 of the tongue. The chorda tympani through it, supplies the submandibular and the sublingual glands and carries taste fibres from the anterior 2/3 of the tongue. 3- The inferior alveolar nerve: (Mixed motor & sensory nerve) It descends deep to the lateral pterygoid, then between the ramus of the mandible and the sphenomandibular ligament to enter the mandibular canal. It runs in the canal opposite the mental foramen t divides into its terminal branches; mental and incisive branches. Before it enters the mandibular canal it gives its mylohyoid branch which descends in a groove on the medial side of the ramus of the mandible to end by supplying the mylohyoid and the anterior belly of digastric muscle. Summary of mandibular nerve It is the largest branch of trigeminal nerve. It is a mixed nerve. It is the nerve of the 1st pharyngeal arch (muscles of mastication). Motor root with the sensory root exit through foramen ovale in greater wing of sphenoid. The trunk of the mandibular lies in the infra-temporal fossa. It is divided into small anterior division Branches of anterior division: 1- Masseteric nerve (M) 2- deep temporal nerve (M) 3- N. to lat pterygoid muscle (M) 4- Buccal nerve (S) Large posterior division Branches of poterior division: 1- Auricul-temporal nerve (S) 2- Lingau nerve (S) 3- Inferior alveolar nerve( contains sensory & motor fibers). Facial nerve (CN VII) Function of the facial nerve It is a mixed nerve (sensory for the tongue & motor for the face) and sharing in two of H & N parasympathetic ganglia. Motor supply for the muscles of the face (Buccinator , Orbicularis occuli, Orbicular oris, Platysma , Stapedius and etc. Functional classification: Special visceral efferent (SVE) facial muscle s are muscle of the 2nd pharyngeal arch. General visceral efferent (GVE): (sharing in two Parasympathetic ganglia; submandibular ganglion to Submandibular & sublingual & sphenopalatine ganglion to lacrimal ). FACIAL NERVE: COURSE & DISTRIBUTION Taste Special visceral afferent (SVA ): taste sensation for the anterior 2/3 tongue. General somatic afferent (GSA): (skin over the back of ear) Deep origin: nuclei of facial nerve: 1- Motor nucleus of facial nerve (SVE): lies in the lower part of the pons . 2- Superior salivatory nucleus (GVE): lies in the pons lateral to the main motor nucleus of VII and gives rise to secretomotor parasympathetic fibers that pass in greater superficial petrosal nerve and chorda tympani. 3- Nucleus solitarus (SVA): lies in the medulla, receives the taste sensation from the anterior 2/3 of the tongue via the central processes of the cell of the geniculate ganglion of the facial nerve. 4- GSA fibers : through fibers to acoustic meatus & back of auricle through communication from auricular branch of vagus. This fibers terminate in main sensory nucleus & spinal nucleus of trigeminal Internal course: the motor fibres passes dorsally and medially forming a loop around the abducent nucleus in the floor of the 4th ventricle forming facial colliculus. FACIAL NERVE •GVE (parasympathetic) from Superior salivary nucleus SVE from Motor nucleus of VII •GSA & GVA both to Nucleus solitarius Superficial origin: at the pontomedullary angle above the inferior cerebellar peduncle. The facial nerve is formed mainly of two parts: 1- Facial nerve proper (motor): arising from facial motor nucleus in pons. 2- Nervus intermedius: it is the sensory root of facial lies position between the facial proper and vestibulcochlear nerve in the pontocerebellar angle. Carrying parasympathetic fibers (from superior salivary nucleus) and taste fibers ( to the solitary nucleus). Course and relations: I- Intracranial (intrapetrosal) course II- Extracranial course I- The intrapetrous course: (L B D) The nerve passes laterally with the vestibulocochlear nerve (CN VIII) to the internal auditary meatus. At the bottom of the meatus the nerve enters the facial bony canal where it runs Laterally above the vestibule of inner ear. Reaching the medial wall of the middle ear, it bends sharply Backwards above the promontory (forming its genu where the genicular ganglion is found). COURSE OF FACIAL NERVE 1 2 3 F A C I A L CANAL To posterior belly of digastric & stylohyoid (To muscles of facial expression) 3- It then arches downwards in the medial wall of the middle ear to reach the stylomastoid foramen. 2- II- Extracranial course As it emerges from the stylomastoid foramen, it runs forwards in the substance of the parotid gland crosses the styloid process, the retromandibular vein and the external carotid artery and divides behind the neck of the mandible into its terminal branches which come out of the anteromedial surface of the gland. Branches of the facial nerve I- Within the facial canal: 1- Nerve to stapedius: supplies the stapedius muscle. 2- Greater superfacial petrosal nerve (GSPN) : arises from the genicular ganglion The greater superficial petrosal nerve joines the deep petrosal nerve from the sympathetic plexus on the internal carotid artery in carotid canal to form the nerve of the pterygoid canal (vedian nerve) which passes through the pterygoid canal to the pterygopalatine fossa and ends in the pterygo-palatine ganglion. 3- Chorda tympani nerve: It arises from the facial nerve 6 mm above the stylomastoid foramen and runs upwards to perforate the posterior bony wall of the tympanic cavity. then passes forwards on the medial surface of the tympanic membrane between its fibrous and mucous layers crossing the handle of the malleus. It comes out of the tympanic cavity through the petrotympanic fissure to the infratemporal fossa where it joins the lingual nerve. Through the lingual nerve, it supplies both the submandibular and sublingual salivary glands by secretomotor fibres and taste fibers from the anterior 2/3 of the tongue II- At the exit from the stylomastoid foramen 1- Posterior auricular nerve: to the auricularis posterior and the occipital belly of the occipitofrontalis muscle. 2- Digastric branch: to the posterior belly of digastric muscle 3- Stylohyoid branch: to the stylohyoid muscle II- Terminal branches On the face: inside the substance of the parotid: 1- Temporal branch. 2- Zygomatic branch 4- Marginal Mandibular branch. 3- Buccal branch. 5- Cervical branch Corticonuclear (corticobulbat) tracts Fibers derived from area 4 descend crossing the midline & terminate in the motor nuclei of the cranial nerves (except 1, 2,& 8). The descending fibers to motor nuclei of 5, 7, 9, 10,11 & 12 called (lateral corticobulbar tracts) while The descending fibers to motor nuclei of 3, 4 &6 called (medial corticobulbar tracts). 1- Lateral corticobulbar tracts arise from the lower 1/3 of area 4 (Motor area). Descend in corona radiata then in the genu of internal capsule Then descend in midbrain where occupying a small area in basis pedunculi dorsolateral to the corticospinal. In the pons & medulla they end on the motor nuclei of CN 5, 7, 9, 10, 11 & 12. 2- Medial corticobulbar tract: arise from area 8 (Motor eye field) descend in corona radiata then genu of internal capsule then to midbrain in cerebral peduncle close to the midline finally end on the motor nuclei of CN 3, 4, & 6. All the corticobulbar fibers end in the motor nuclei of the cranial nerves in the brain stem of both sides except lower ½ of the facial nerve, accessory & hypoglossal nerve nuclei receive fibers from opposite side only. Upper motor neuron (UMN) lesion of facial nerve: result from lesion of the pyramid tract above the level of facial nucleus (supranuclear lesion) It commonly occurs with capsular hemiplegia, There is hemiplegia accompanied by paralysis of lower ½ of the face of the opposite side of the capsular lesion. The upper part of the face is not affected as It recieves corticobulbar from both sides. While the lower ½ of facial nucleus receives corticobulbar pyramid fibers only from the opposite side. II- Lower motor neuron (LMN) lesion of facial nerve (called Bell’ s palsy): results from affection of the facial nucleus & facial nerve fibers. Manifested by Complete Paralysis of the facial muscles of the side of lesion. If the injury is proximal to geniculate ganglion: there is also loss of secrtion from lacrimal, nasal, buccal, sunmandibular & sublingual glands in addition to loss of taste sensation from the anterior 2/3 of the tongue on the affected side. There is hyperacusis (increase sound perception ) due to paralysis of the stapedius muscle. If the injury is distal to the geniculate ganglion & above the origin of chorda tympani, glands will not affected. BELL’S (FACIAL) PALSY Lesion of facial nerve (below sytlomastoid foramen) results in paralysis of muscles of facial expression. It is of the lower motor neuron lesion type (whole face, at same side of lesion, is affected). Distortion of face : sagging of angle of mouth, dribbling of saliva, loss of facial expressions, loss of chewing, blowing, sucking, unable to show teeth or close eye. Bell’s Palsy Vestibulocochlear (CN VIII) Vestibulo-cochlear nerve nuclei Vestibular nuclei (SSA): four in number Superior, lateral & medial vestibular nuclei lies in the lower part of pons, inferior vestibular nucleus forms an elevation in the lateral part of the floor of the 4th vectricle (lies in the open medulla). They carry sense of equilibrium from the labyrinth some of fibers pass directly to the cerebellum. Inferior vestibular nucleus (SSA): It is one of 4 nuclei for vestibular part of the CN VIII. It lies in the open medulls in the lateral part of the floor of 4th ventricle Cochlear nerve nuclei (SSA): Carrying ahearing sensation from the inner ear. They are two somatic afferent nuclei 1- ventral cochlear nucleus lies in front of inferior cerebellar peduncle while dorsal cochlear nucleus lies behind it. The Glossopharyngeal nerve Functions: GSA GVA SVA GVE SVE Deep origin: in the medulla oblongata : through 1- Nucleus ambiguus (SVE) 2-Solitary Nucleus (GVA SVA) 3- Inferior salivatory nucleus (GVE) 4- Spinal nucleus of trigeminal nerve (GSA) Deep nuclei of glossopharyngeal nerve 1- Nucleus ambiguus (SVE): It lies dorsal to the inferior olivary nucleus in the medulla. Its upper parts gives fibers to glossopharyngeal nerve, its middle part gives fibers to vagus and its lower part gives fibers to the accessory. It is a special visceral efferent as it supply striated muscles of the 3rd, 4th & 6th pharyngeal arch respectively. 2-Solitary Nucleus (GVA SVA) Lies medial to the inferior cerebellar peduncle. It receives taste sensation (SVA) from the tongue & epiglottis through facial, glossopharyngeal & vagus. It also receives general visceral sensation (GVS) from glossopharyngeal & vagus. 3- Inferior salivary nucleus (GVE): Lies in the upper most part of the medulla in line with the dorsal motor nucleus of the vagus. It gives fibers which run in glossopharyngeal nerve as a preganglionic parasympathetic (secretory motor) which relay in the otic ganglion to parotid. Superficial attachment: Emerges from the posterolateral fissure of the medulla, then outside the skull through middle of the jugular foramen. The nerve passes downwards between the internal and external carotid arteries to reach the posterior border of the stylopharyngeus muscle. •It then curves forwards lying on the muscle to pass between the superior and middle constrictor muscles to end by breaking into its terminal branches. Functions and Nuclei of IX and X nerves VAGUS NERVE GLOSSOPHARYNGEAL NERVE GVA SVA GSA SVE GVE GVA SVA GSA SVE GVE Nucleus solitarius (SVA&GVA) Inferior salivatory n (GVE) IX Nucleus Ambiguus (SVE) X Spinal nucleus of V (GSA) Dorsal motor nucleus of X (GVE) Parasympathetic innervation of parotid glands by glossophayrngeal nerve Ganglia: 1- Superior ganglion: has no branches and considered a detached part of the inferior ganglion 2- Inferior ganglion: its branches carry general sensations from the pharynx, soft palate and tonsils as well as general and taste fibres from the posterior 1/3 of the tongue Branches: 1- Tympanic nerve: is a branch of the inferior ganglion reaches the tympanic cavity through the tympanic canaliculus to form the tympanic plexus on the medial wall of the cavity lesser petrosal nerve arises to the cranial cavity and through the foramen ovale to relay into the otic ganglion. Postganglionic fibres supplies the parotid gland 2- Carotid branch: to the carotid sinus and body, it carry stimuli of blood pressure changes. 3- Pharyngeal branches: is the sensory root of the pharyngeal plexus, carry the general sensations from the pharynx. 4- Lingual branches: carry general and taste fibres from the posterior 1/3 of the tongue . 4- Muscular branch: to the stylopharyngeus muscle 5- Tonsillar branches: carry sensory branches from the palate and the tonsils Lesser petrosal n Tympanic plexus Parotid gland Tympanic br Auditory tube Otic ganglion To stylopharyngeus Carotid br Tonsillar branches Lingual branches Pharyngeal branches On the middle constrictor Glossopharyngeal nerve The Vagus nerve Functions: GSA GVA SVA GVE SVE Deep origin: in the medulla oblongata 1- Dorsal motor nucleus of the vagus (GVE) 2- Nucleus ambiguus (SVE) 3- Nucleus of tractus solitarius (GVA , SVA). Mentioned before 4- Spinal nucleus of trigeminal nerve (GSA) 1- Dorsal nucleus of vagus: Lies in the floor of the 4th ventricle lateral to the hypoglossal nucleus. It gives preganglionic parasympathetic (secretory motor) fibers supplying smooth muscles of the viscera and inhibitory to the heart. Dorsal nucleus of vagus also receives sensation from viscera (gerneral visceral afferent fiber GVA) through the glossopharyngeal & vagus. Hypoglossal N 1 3 4 2 Nuclei of the vagus & hypoglossal 1- Dorsal nucleus of vagus 2- Nucleus ambiguus 3- nucleus solitarius 4- spinal tract & nucleus Superficial origin: Emerges from the posterolateral fissure of the medulla (between the olive and the ICP), then outside the skull through middle of the jugular foramen. Course and relations: •At the base of the skull the nerve lies between the internal jugular vein and the internal carotid artery deep to the styloid process. •The nerve descends vertically within the carotid sheath between common carotid artery and the internal jugular vein until it reaches the root of the neck, it crosses in front of the first part of the subclavian artery to the thorax Ganglia: •Superior ganglion: its branch is the auricular nerve •Inferior ganglion: its branches carries general sensations from the larynx, trachea, bronchial tree, lungs, and the alimentary tract down to the junction between the right 2/3 and left 1/3 of the transverse colon. It also carries taste fibres from the root of the tongue and the epiglottis. Branches in the neck: I- In the jugular foramen: 1- Meningeal branch: to the dura matter of the posterior cranial fossa 2- Auricular branch: to supply the floor and the posterior wall of the external auditory meatus and the outer surface of the drum II- in the neck : 1- Pharyngeal: (consists principally of the cranial part of XI), is the motor part of the pharyngeal plexus through which it supplies all muscles of the pharynx except the stylopharyngeus (by XI) and all muscles of the palate except the tensor palati (by mandibular nerve) 2- Branch to the carotid body 3- Superior laryngeal nerve: passes deep to the internal carotid artery on thee lateral wall of the pharynx, it divides into: A- Internal laryngeal nerve: pierces the thyrohyoid membrane with the superior laryngeal vessels, it carries sensations from the pharynx, epiglottis above the vocal cords. Meningeal br The Vagus nerve Cranial part of XI Auricular br Pharyngeal br To Carotid body Internal laryngeal n. Superior laryngeal n. Cardiac br External laryngeal n. Recurrent laryngeal n. B- External laryngeal nerve: supplies the cricothyroid muscle 5- Right recurrent laryngeal nerve: arises from the right vagus where it crosses in front of the right subclavian artery, it curves around the artery and ascends upwards in a groove between the trachea and oesophagus close to the medial surface of the thyroid gland . It supplies all the intrinsic muscles of the larynx except the cricothyroid muscle (by external laryngeal) and sensations from the larynx above the vocal cords. Branches of vagus In the thorax 1- Cardiac branches: superior and inferior branches to the cardiac plexuses 2- Left recurrent laryngeal nerve. 3- Pulmonary 4- Oesophageal Branches of vagus In the abdomen 1- Gastric 2-Coeliac 3- hepatic The Accessory nerve Functions: SVE (cranial root), GSE (spinal root) Deep origin: 1- Nucleus ambiguus (SVE) 2- Upper 5 cervical segments (spinal part) Superficial origin: the cranial part emerges from the postrolateral fissure of the medulla, the spinal part emerges on the side of the spinal cord. Internal course: the spinal part ascends in the vertebral canal then through the foramen magnum to join the cranial root and both leave the cranial cavity through the middle part of the jugular foramen Course and relations: •Just below the base of the skull the cranial part separates to join the vagus nerve. The spinal part curves laterally and backwards posterior to the internal jugular vein it then passes through the upper part of the sternocliedomastoid muscle to the posterior triangle lying on the levator scapulae and ends into the trapezius muscle. Branches of accessory nerve: The cranial part is distributed through the pharyngeal and laryngeal branches of the vagus nerve concerning movements of the soft palate, larynx, pharynx. The spinal part supplies the sternocleidomastoid and trapezius muscles, controlling the movements of neck . Lesion of accessory nerve results into: Difficulty in swallowing and speech Inability to turn the head and raise the shoulder Winging of scapula The Hypoglossal nerve Functions: GSE (pure motor) Deep origin: Hypoglossal nucleus (GSE): Lies in the floor of the 4th ventricle close to the median plane. Its fibers entirely motor (general somatic motor efferent) supply the muscles of the tongue. it is connected to pyramidal (corticobulbar) tract, medial longituidinal bundle & the nucleus of the opposite side. Superficial origin: from the side of the medulla between the olive and the pyramid (through antrolateral fissure) passes through hypoglossal (anterior condylar) canal Course and relations: The XII nerve leaves the skull through the hypoglossal canal where it lie deep to the internal jugular vein then it joins the other nerves (XI, X, XI). In the carotid triangle, it curves medially crossing anterior to the internal and external carotid arteries and the loop formed by the lingual artery, It then ascends upwards in the submandibular region it lies on the lateral surface of the hyoglossus muscle deep to the mylohyoid muscle and the submandibular gland. It passes next on the lateral aspect of the genioglossus and continue in its substance where it breaks into its terminal branches Branches: It supplies all the intrinsic and extrinsic muscles of the tongue except the palatoglossus (by the cranial part of XI through the pharyngeal branch of X from the pharyngeal plexus). So the function of hypoglossal nerve (CN XII): It Controls the movements and shape of the tongue during speech and swallowing Lesion; (LMN paralysis) results into: 1- Loss of tongue movements 2- Difficulty in chewing and speech The paralyzed tongue, atrophies, becomes shrunken and furrowed on the affected side Unilateral lesion; the protruded tongue deviates to the affected side. Bilateral lesion; the person can’t protrude the tongue.