* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Appendix A
History of invasive and interventional cardiology wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Jatene procedure wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Coronary artery disease wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
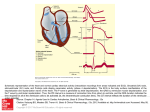
Appendix A Ventricular Tachycardia: Rapid succession of three or more ventricular complexes. Atypical Run: Rapid succession of three or more ventricular complexes. The rate is less than the 120 bpm. ST Level: Depression CH 1 CH 2 -4 mm 00:00 00:00 -3 mm 00:00 00:00 -2 mm 00:00 00:00 -1 mm 00:15 00:12 Elevation CH 1 CH 2 +4 mm 00:00 00:00 +3 mm 00:00 00:00 +2 mm 00:00 00:00 +1 mm 00:00 00:00 The above gives the amount of time the ST was above or below the measure ST level. For an ST episode to be declared the ST Detection Level can be set from the analysis parameters dialog box. This can be from 1 mm to 4 mm depression or elevation. The J-Point can also be set in milliseconds from the analysis parameters dialog box. The ST level is measured relative to the PR interval. While the U-P level theoretically would be preferred it cannot be used because it disappears with tachycardia. When there is a short PR interval, it can be particularly difficult for computer algorithms to find the isoelectric reference level. The direction of the ST vector and the relative position of the electrode measuring the vector determine whether the ST amplitude is positive (elevation) or negative (depression). For instance at rest, since the main ST vector projects along the long axis of the heart toward the apex, AVR will register a negative ST amplitude and V5 will register a positive ST amplitude (early repolarization). With tachycardia or ischemia the direction changes, as does the ST amplitude. As for any vector shift that is perpendicular to an electrode, no amplitude will be registered. Pathological processes that cause ST elevation shift the entire vector from it's long axis of the heart orientation and move it through the area of inflammation (pericarditis) or transmural ischemia (infarction or spasm). Thus, pathological ST depression does not localize but reflects a global subendocardial process while pathological elevation occurs directly over the involved area. It is important to determine if the ST elevation was documented on previous ECGs and if the ST level is currently changing or is stable. Acute or dynamic ST elevation can be due to severe transmural ischemia secondary to thrombus, spasm or a tight fixed coronary artery lesion or a combination of these situations. It can be the first ECG manifestation of an evolving myocardial infarction and it represents the ECG criteria for thrombolytic therapy. However, if the pain does not persist, it more likely is due to variant or unstable angina. The elevation localizes the ischemic lesion to the coronary artery supplying the area of myocardium reflected by the ECG leads. It represents transmural ischemia and is very arrythmogenic. Chronic or persistent ST elevation could be due to an aneurysm when it occurs over Q waves or to chronic pericarditis (i.e., with uremia), but it most commonly occurs with a normal ECG pattern and is known as early repolarization. It may actually be due to late depolarization and is a very normal finding even to 3-4 mm in amplitude. Normally early repolarization lessens with increases in heart rate while ischemic ST elevation increases.