* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Notes - Haiku Learning
Developmental biology wikipedia , lookup
Cell theory wikipedia , lookup
Homeostasis wikipedia , lookup
Organ-on-a-chip wikipedia , lookup
Evolution of metal ions in biological systems wikipedia , lookup
Gaseous signaling molecules wikipedia , lookup
Biochemistry wikipedia , lookup
High-altitude adaptation in humans wikipedia , lookup
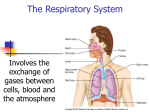
Chapter 15: Respiratory System • The lungs are actively ventilated to ensure that gas exchange can occur passively. • Red blood cells are vital in the transport of respiratory gases. I. Respiratory System: carry oxygen to the cells and eliminate carbon dioxide A. Lungs: site of gas exchange between atmosphere and blood and located in thoracic (thorax) cavity (closed to the outside air) 1. Right side has three lobes and left side has two lobes 2. Inside chest cavity and surrounding by membranes called pleura B. Passage of air 1. Mouth and nose: air enters and small hairs in the nose filters the air and mucus warms and moistens the air 2. Pharynx: tube at the back of the nasal cavities and mouth and is passageway for air and food 3. Epiglottis: flap of cartilage that covers the opening to air passage 4. Trachea: air passageway made of cartilage which contain cilia and mucus to trap particles 5. Larynx: upper end of trachea that contains the vocal cords 6. Bronchi: two branches that lead to the lungs from trachea 7. Bronchioles: smaller tubes into the lungs 8. Alveoli: clusters of tiny air sacs surrounded by capillaries a) Gases are exchanged between the alveoli and blood b) 300 million alveoli per lung alveoli Overview clip The Respiratory System Mouth Pharynx Larynx Trachea Lung Epiglottis Bronchus Nose Bronchiole Alveoli Bronchioles Diaphragm Edge of pleural membrane Capillaries C. Gas exchange and transport 1. Gas exchange in lungs a) Oxygen crosses two cells: alveolus cell and capillary wall cell and enters the blood b) Carbon dioxide crosses capillary wall cell and alveolus cell and enters the alveoli c) Concentration gradient of these two gases will ensure diffusion of each gas in the correct direction Gas exchange Higher level gas exchange Gas Exchange in the Lungs Alveoli Bronchiole Capillary 2. Alveoli are composed of specialized cells called pneumocytes a) Pneumocytes: cell type that makes up the single cell layer of the alveolus b) Type I pneumocytes i) Very thin ii) Very large membrane surface area: well designed for diffusion iii) If damaged, cannot be replaced by mitosis c) Type II pneumocytes i) Cuboidal in shape and have little membrane surface area ii) Produce and secrete a solution that acts as a surfactant to reduce the surface tension of the moist inner surface of alveoli and prevents the sides of the alveoli form sticking together iii) Can go through mitosis for replacement of both types of alveolar cells if they are damaged Pneumocyte cells D. Mechanism of breathing 1. Breathing: process of moving air into and out of the lungs a) Based on the inverse relationship between pressure and volume b) Increase in volume will lead to a decrease in pressure c) Whatever pressure does, volume will do the opposite 2. Ventilation: repeated process of filling our lungs with air and then expelling that air 3. Inspiration: inhaling, is the process of taking air into the lungs a) Tissues that makes up the lungs is passive and not muscular, so lungs are in capable of purposeful movement b) Muscles surrounding the lungs i) Diaphragm: large flat muscle Clip ii) External intercostal muscles: surround ribs iii) Internal intercostal muscles 4. Actions that lead to inspiration a) Diaphragm contracts and external intercostal muscles and one set of abdominal muscles raise the rib cage: Increases the volume of the thoracic cavity b) Increased volume in chest cavity results in the pressure inside the cavity to decrease: leads to less pressure “pushing on” the passive lung tissue c) Lung tissue increases its volume because there is less pressure exerted on it d) Leads to a decrease in pressure inside the lungs: known as partial vacuum e) Air comes in through your open mouth or nasal passages to counter the partial vacuum within the lungs and fills the alveoli 5. Expiration: exhaling, process of expelling air from lungs a) Reverse process of inspiration b) Diaphragm relaxes c) Volume in chest cavity decreases and air pressure is greater so air rushes out Respiration Video pressure The Mechanics of Breathing E. Regulation of breathing 1. Rate at which oxygen is used depends on the activity of the cell 2. Greater activity requires more oxygen 3. Abdominal and intercostal muscles achieve a greater initial thoracic volume which leads to deeper breathing and more air moving into the lungs Clip II. Causes and consequences of emphysema A. Emphysema: disease whereby the alveoli in the lungs are progressively destroyed 1. Chronic, slowly progressive disease that turns healthy alveoli into large, irregularly shaped structures with gaping holes 2. Reduces the surface area for gas exchange, so less oxygen reaches the bloodstream, so shortness of breath is a symptom and typically occurs first during strenuous activity 3. COPD (chronic obstructive pulmonary disease): group of respiratory diseases including emphysema a) Shortness of breath, especially during physical activities b) Wheezing c) Chest tightness d) Having to clear your throat first thing in the morning, due to excess mucus in your lungs e) A chronic cough that produces sputum that may be clear, white, yellow or greenish f) Blueness of the lips or fingernail beds (cyanosis) g) Frequent respiratory infections h) Lack of energy (Mayo Clinic) 4. Causes a) Smoking b) Marijuana smoke c) Fumes from manufactory plants d) Coal dust e) Air pollution 5. No cure for emphysema, but the progression of the disease can be slowed by stopping smoking or removal of other risk factors 6. Never start smoking and wear protective mask when working around dust or chemical fumes Video III. Causes and consequences of lung cancer A. Lung cancer: cancerous growth that begins in the lungs 1. Cancer that is prone to spreading (metastasizing) 2. Brain, bones, liver, and adrenal glands are likely targets for lung cancer that has metastasized 3. Cancerous growth in the lungs takes over healthy tissues that were bronchioles and alveoli 4. The larger the growth, the more the lung tissue becomes dysfunctional and can result in internal bleeding B. Causes 1. Carcinogen: substance that is known to cause cancer 2. Carcinogen enters the lung tissues and mutates into a cancerous growth a) Cigarette smoke and other fumes b) Asbestos: used to be used in building insulation products and is consider a carcinogen i) Need a special company to safely remove the asbestos from older buildings ii) Asbestos was cheap, durable, fireproof, and ability to insulate iii) Appliances, insulation, flooring, toys, and crayons C. Treatment 1. Best treatment is achieved when the disease is diagnosed early 2. Lung cancer has a high mortality rate 3. Data supports a direct correlation between those countries and cultures that have shown a decrease in the number of people who smoke and a corresponding decrease in the incidence of lung cancer Video Smoking vs. Healthy Lungs IV. Hemoglobin and gas exchange (Haemoglobin) A. Hemoglobin: protein molecule found within erythrocytes that carries most of the oxygen in the bloodstream 1. Contains 4 polypeptides, each with a heme group that has an iron atom 2. Each iron can bind to one oxygen molecule 3. Each hemoglobin molecule is capable of reversibly binding to as many as four oxygen molecules and one CO2 molecule 4. Erythrocytes is made of cell membrane, cytoplasm, few organelles, and hemoglobin (no nucleus) 5. 250 million hemoglobin molecules in each red blood cell Hemoglobin B. Hemoglobin changes shape and affinity when carrying oxygen 1. Proteins have an ability to change their 3D shape (enzyme changes shape as substrate enters active site) 2. Hemoglobin has 4 possible shapes, depending on how many oxygen molecules are bond to the iron atoms 3. Hemoglobin’s affinity for oxygen: the different shapes affect the hemoglobin’s ability to bind with O2 a) Greater the tendency to bind with oxygen, the higher the affinity 4. Hemoglobin molecules that are already carrying 3 O2 molecules have the greatest affinity for oxygen 5. Hemoglobin molecules that are carrying no oxygen molecules have the least affinity for oxygen 6. Each oxygen molecule that binds to hemoglobin changes the hemoglobin shape in a way that increases its affinity for another O2 7. Hemoglobin can carry a maximum of 4 O2, so one that is already carrying 4 has no affinity for O2 8. Affinity for oxygen from lowest to highest is Hb4, Hb4O2, Hb4O4, and finally Hb4O6 C. Oxygen dissociation curves: show the tendency of hemoglobin to bind to O2 (affinity) and separate from O2 (dissociate) 1. Oxygen dissociation curves are graphs that show how various forms of hemoglobin or myoglobin perform under various conditions 2. Partial pressure: pressure exerted from a single type of gas when it is found within a mixture of gases a) Air that we breathe and is a mixture of gases, and O2 is just one part of the mixture b) Bloodstream and tissues contain a mixture of different gases including O2 c) Total pressure: pressure exerted by a mixture of gases d) Partial pressure of O2: portion of the total pressure that is caused by oxygen alone Partial Pressures 3. x-axis measures the partial pressure of oxygen 4. y-axis shows the percentage saturation of hemoglobin with O2 5. Hemoglobin is not saturated until it is carrying 4 oxygen molecules Curve 6. Very steep S-shape is indicative of the affinity changes for O2 that hemoglobin undergoes when at least some O2 is already bound to the molecule a) At the lower end of the graph: little O2 is already bound b) At the upper half of the graph: hemoglobin is already bound to some O2 and has increased its affinity for O2 because of the change in the protein shape 7. Homeostatic range of oxygen partial pressures within the body a) Upper range of normal: 75mmHg or 10kPa is O2 partial pressure in lungs, graph shows that more than 90% of hemoglobin becomes saturated with O2 in lungs b) Lower range of normal: 35mmHg or 5kPa, only about 50% is still saturated with O2 and this is partial pressure of O2 in body tissues undergone cell respiration c) 40-50% of the hemoglobin has recently been to the lungs has given up (dissociates) one or more O2 molecules when it reaches the body tissues d) Hemoglobin typically don’t empty their oxygen load when they reach respiring tissues, but they release a significant amount of O2 within a narrow range of O2 partial pressures D. Comparison of hemoglobin and myoglobin 1. Myogloblin: oxygen-binding protein found in muscles a) Single polypeptide b) Heme group and Fe atom 2. Function: store O2 within muscle tissues until muscles begin to enter an anaerobic situation when exercising heavily 3. During heavy exercise, myoglobin dissociates its O2 and thus delays the onset of lactic acid fermentation 4. Myoglobin has the ability to hold onto its O2 even at low O2 partial pressures in order to provide a final reservoir of O2 when exercising 5. Graph shows myoglobin to the left of hemoglobin (except for upper end) a) Shows that myoglobin is still bound to its O2 even when hemoglobin has dissociated its O2 Hemoglobin and Myoglobin E. Comparison of adult hemoglobin and fetal hemoglobin 1. Fetus hemoglobin is slightly different in molecular composition compared with adult hemoglobin 2. Fetus hemoglobin must have a greater affinity for O2 than an adult 3. In placental capillaries, adult hemoglobin is more likely to dissociate O2 and fetus hemoglobin is more likely to bind to that same O2 4. Fetal hemoglobin dissociates its O2 when it reaches the tissues of the fetus 5. Curve for fetus hemoglobin is always to the left of the adult hemoglobin a) Any point on the x-axis shows that adult hemoglobin binds less O2 at that partial pressure compared with fetus hemoglobin F. The Bohr shift: results when CO2 binds to hemoglobin, causing a shape change that promotes the release of O2 1. Hemoglobin’s affinity for O2 is reduced in an environment where CO2 partial pressure is high a) Found in cells undergoing cell respiration b) Hemoglobin is induced to release (dissociate) O2 within the capillaries of body tissues 2. Curve on left shows what happens to hemoglobin passing through the lungs (partial pressure of CO2 is low): O2 binds easily to hemoglobin 3. Curve on right shows what happens to hemoglobin in respiring tissues that are giving off CO2 : Some CO2 binds with hemoglobin and O2 will dissociate to the tissuesClip G. Carbon dioxide transport in the blood 1. CO2 is a waste product of cellular respiration and diffuses out of the cell and into the capillary 2. Three ways CO2 is transported to lungs a) Small percentage remains as CO2 and dissolves in blood plasma b) Some CO2 enters erythrocytes and becomes reversibly bound within hemoglobin (Bohr shift): each hemoglobin can carry one CO2 c) About 70% of CO2 enters erythrocytes and is converted into hydrogen carbonate ions (HCO3-) which moves into the blood plasma for transport H. Formation of HCO31. Carbonic anhydrase: enzyme in the cytoplasm of erythrocytes that catalyzes the reaction of CO2 and water to form carbonic acid (H2CO3) 2. Carbonic acid then dissociates into H+ and hydrogen carbonate ion (HCO3-) 3. HCO3- exits cell through protein channel in erythrocyte membrane by facilitated diffusion a) One HCO3- moves out and one Cl- moves in b) Chloride shift: movement of ions to keep the charges balanced Video I. Maintaining a narrow homeostatic range of pH in the blood 1. pH of blood plasma: 7.35-7.45 2. Requires a buffering system to maintain pH range due to more H+ when exercising due to an increased produce of CO2 3. H+ made from dissociation of carbonic acid can’t stay in solution in the erythrocyte cytoplasm or blood plasma 4. pH buffering: temporary removal of H+ from solutions a) H+ can be bound at various places on hemoglobin molecules b) H+ can exit erythrocyte and bind with proteins circulating as solutes in plasma Video Video V. Rate of ventilation is controlled by the respiratory control center in the medulla oblongata A. Increase in physical activity leads to an increase demand for ATP in muscles, which means an increase demand for O2 1. Mechanism needed to ensure the rate of transport of respiratory gases meets the needs of the increased demand 2. Increase the ventilation or breathing rate B. Ventilation rate is under the control of an area of the medulla oblongata at the brainstem (respiratory control center) and has two mechanisms when ventilation needs to increase 1. Receptor cells: chemosensor (chemoreceptors) a) Inner wall of aorta and carotid arties b) Detect an increase in CO2 and decrease in blood pH c) When stimulated they send action potentials to medulla’s breathing center 2. Medulla: contains same chemosensors a) Blood passes through capillaries of medulla, increased CO2 and decreased pH levels are detected b) Medulla respiratory control center sends action potentials to the diaphragm, intercostal muscles, and abdominal muscles c) Frequency of breathing is increased 3. Physical exercise decreases a) Chemoreceptors detect the decrease in CO2 levels and slight increase in blood plasma pH b) Leads to decrease in ventilation rate VI. Living and breathing at high altitude A. Common misconception that the air at high altitudes contains less oxygen by percentage than air at sea level 1. Percentage of gases in the air does not change as altitude increases 2. Air pressures changes at different altitudes a) Air at higher altitudes is at a lower pressure b) All the molecules in the mixture are more spread out than in a mixture at sea level 3. When you breathe less dense air, diffusion of oxygen across the alveoli into the bloodstream is less efficient and less oxygen enters the blood B. Symptoms at high altitude 1. Physical activity leads to immediate fatigue 2. Altitude or Mountain sickness: vision problems, nausea, high pulse rate, difficulty in thinking clearly 3. Severe altitude sickness: fluid around brain or lungs, can become life threatening and person suffering should be taken to a lower altitude C. How the body compensates when reaching a higher altitude 1. Increasing ventilation rate and heart rate: stressful for the body and not a long term solution 2. Acclimatization occurs over time a) Increase in the number of erythrocytes and amount of hemoglobin b) Increase in the capillaries in both the lungs and muscles c) Increase in lung size and surface area d) Increase in myoglobin within muscle tissue D. Sport training at high altitudes: some athletes train at a higher altitude in order to take advantage of more erythrocytes and hemoglobin E. Mountaineers will typically spend time at a base camp at higher altitudes before a climb in or to acclimate before climbing Altitude sickness Altitude sickness video VII. Identification of lung tissues with light and electronmicrographs A. Alveoli and capillaries are best viewed under an electron microscope 1. Illustration shows capillary (in section) running in/out of the page 2. Inside the capillary are portions of 3 erythrocytes, cut in section 3. On either side of capillary are portions of 2 alveoli 4.Nucleus of an alveolar cells is shown just to the right of the 3 erythrocytes Textbook image