* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download NAME: Carbamazepine (Tegretol)
Survey
Document related concepts
Discovery and development of proton pump inhibitors wikipedia , lookup
Psychedelic therapy wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Neuropharmacology wikipedia , lookup
Prescription costs wikipedia , lookup
Drug discovery wikipedia , lookup
List of comic book drugs wikipedia , lookup
Drug design wikipedia , lookup
Drug interaction wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Lamotrigine wikipedia , lookup
Pharmacokinetics wikipedia , lookup
Transcript
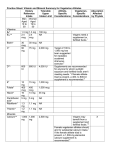
NAME: Carbamazepine (Tegretol) MOA: Chemically related to imipramine; reduces polysynaptic responses, blocks post-tetanic potentiation, and may depress thalamic potential possibly by inhibiton of voltage gated sodium channels Efficacy (Indication/Use): - FDA indications: Epilepsy, Partial, generalized, and mixed types of seizures Should be considered first line therapy for newly diagnosed partial seizures and in generalized convulsive seizures SAFETY: Adverse Effects: DIPLOPIA, dizziness, HYPONATREMIA (SIADH), blood dyscrasias, lethargy Major Drug Interactions: any drug that inhibit or induces CYP 3A4 Contraindications: - concomitant use of monoamine oxidase inhibitors - hypersensitivity to carbamazepine or tricyclic compounds - history of previous bone marrow depression Precautions: - breast feeding - do not discontinue abruptly - elderly patients - increased intraocular pressure - kidney dysfunction and liver dysfunction - patients with underlying mental illness may experience activation of latent psychosis or agitation - pregnancy (especially the first trimester) Pregnancy Category: D Kinetics: - - Food may enhance bioavailability Absorbtion from IR tablets is slow and inconsistent due to poor water solubility Suspension absorbed faster than tablets Controlled release formulations dosed twice daily are bio-equivalent with QID IR dosing and provide lower peaks & higher troughs Tegretol XR should be taken with food; drug casing will be excreted in feces Metabolized by the liver, primarily by CYP-3A4 Induces own metabolism; AUTOINDUCTION begins within 3-5 days and takes 21-35 days to completely level off Therapeutic range 4 to 12 mcg/mL Dosage & Administration Initial: 200 mg twice daily (tablets, extended release tablets, or extended release capsules) or 100 mg of suspension 4 times/day (400 mg daily); increase by up to 200 mg/day at weekly intervals using a twice daily regimen of extended release tablets or capsules, or a 3-4 times/day regimen of other formulations until optimal response and therapeutic levels are achieved; usual dose: 800-1200 mg/day; some patients have required up to 1.6-2.4 g/day Monitoring CBC with platelet count, reticulocytes, serum iron, lipid panel, liver function tests, urinalysis, BUN, serum carbamazepine levels, thyroid function tests, serum sodium; ophthalmic exams (pupillary reflexes); observe patient for excessive sedation, especially when instituting or increasing therapy References (Guidelines, Drug Info Sources) http://www.thomsonhc.com.db.usip.edu/hcs/librarian/ND_PR/Main/SBK/1/PFPUI/Hy3XhRC1syYGxd/ND_PG/PRIH/CS/DE6542/ND_T /HCS/ND_P/Main/DUPLICATIONSHIELDSYNC/552D96/ND_B/HCS/PFActionId/hcs.common.RetrieveDocumentCommon/DocId/010 3/ContentSetId/31/SearchTerm/carbamazepine/SearchOption/BeginWith#secN66838 (Accessed 8/16/06) Lexi-Comp On-line. Carbamazepine. Updated 8/11/06; Accessed 8/16/06; http://www.crlonline.com/crlsql/servlet/crlonline Garnett W. Gidal BE. Epilepsy. In Pharmacotherapy: A Pathophysiologic Approach Sixth Ed. Editors: DiPiro JT. Talbert RL. Yee GC. Matzke GR. Wells BG. Posey LM. 2005. New York. pgs 1023-1048. NAME: Phenytoin (Dilantin) MOA: - Primary site of action is in motor cortex; stabilizes the threshold against hyperexcitability. -Alteration of ion fluxes associated with depolarization, repolarazation and membrane stability; alteration of Ca++ uptake in presynaptic terminals and influence on Ca++ dependent synaptic neurotransmitter release; alteration of Na+/K+ ATP-dependent ionic membrane pump. Place in Therapy: - FDA approved indications: complex partial seizures, tonic-clonic seizures, seizure prophylaxis during neurosurgery - First line agent for primary generalized convulsive and partial seizures. Also a first line agent for treatment of status epilepticus. SAFETY: Adverse Effects: Behavior changes, skin thickening, GINGIVAL HYPERPLASIA, HIRSUTISM, coarsening of facial hair, acne, blood dyscasias, rash, ataxia, NYSTAGMUS, dizziness, VISUAL BLURRING Major Drug Interactions: - Phenytoin levels may be increased by many drugs that displace it from albumin, or inhibit its metabolism: allopurinol, amiodarone, calcium channel blockers, cimetidine, fluconzole, gemfibrozil, isoniazid, ketoconazole, NSAIDs, methylphenidate, metronidazole, omeprazole, salicylates, SSRIs, sulfonamides, ticlopidine, TCAs, trazadone, trimethoprim, etc. Contraindications: - Hypersensitivity to phenytoin, other hydantoins, or any component of the formulation - Pregnancy Precautions: - alcohol use (acute use: increases levels; chronic use: decreases levels) - avoid abrupt withdrawal (may precipitate status epilepticus) - diabetes mellitus (hyperglycemia has occurred in diabetics) - discontinue if skin rash occurs (do not resume if rash is exfoliative, purpuric, or bullous, or if lupus erythematosus or Stevens-Johnson syndrome is suspected) - impaired liver function - patients with a history of renal or liver disease should not receive the oral loading dose regimen - pregnancy Pregnancy Category: D Kinetics: - Metabolized by the liver via CYP 2C9 and CYP 2C19 Therapeutic range between 10-20 mcg/ml Usual unbound concentrations associated with optimal therapy being between 1 to 2 mcg/ml Levels peak between 4 – 8 hours after dose Therapeutic range of phenytoin is based on conditions of normal protein binding o Phenytoin is 90-95% bound to albumin In states of decreased protein binding, the observed level is falsely decreased, so either the therapeutic range or the observed concentration must be adjusted. o A more common approach is to correct the observed concentration Hypoalbuminemia Corrected Level = (measured concentration) 1 [(0.2)(measured albumin) + 0.1] Renal Failure (CrCl < 10mL/min) Corrected Level = (measured concentration) 1 [(0.1)(measured albumin) + 0.1] Hypoalbuminemia Renal Failure Measured Concentration Measured Albumin Corrected Level Measured Concentration Measured Albumin Corrected Level 5 mcg/mL 5 mcg/mL 5 mcg/mL 5 mcg/mL 10 mcg/mL 10 mcg/mL 10 mcg/mL 10 mcg/mL 3.5 g/dL 3 g/dL 2.5 g/dL 2 g/dL 3.5 g/dL 3 g/dL 2.5 g/dL 2 g/dL 6 mcg/mL 7 mcg/mL 8 mcg/mL 10 mcg/mL 13 mcg/mL 14 mcg/mL 17 mcg/mL 20 mcg/mL 5 mcg/mL 5 mcg/mL 5 mcg/mL 5 mcg/mL 10 mcg/mL 10 mcg/mL 10 mcg/mL 10 mcg/mL 3.5 g/dL 3 g/dL 2.5 g/dL 2 g/dL 3.5 g/dL 3 g/dL 2.5 g/dL 2 g/dL 11 mcg/mL 13 mcg/mL 14 mcg/mL 17 mcg/mL 22 mcg/mL 25 mcg/mL 29 mcg/mL 33 mcg/mL 15 mcg/mL 15 mcg/mL 15 mcg/mL 15 mcg/mL 3.5 g/dL 3 g/dL 2.5 g/dL 2 g/dL 19 mcg/mL 21 mcg/mL 25 mcg/mL 30 mcg/mL 15 mcg/mL 15 mcg/mL 15 mcg/mL 15 mcg/mL 3.5 g/dL 3 g/dL 2.5 g/dL 2 g/dL 33 mcg/mL 38 mcg/mL 43 mcg/mL 50 mcg/mL Dosage & Administration - Food increases the absorption of phenytoin - May dose QD or up to QID - Empiric dosing: o o o Monitoring - IV loading dose: 10 – 15 mg/kg (infused 25-50 mg/min) PO loading dose: 15 – 20 mg/kg in 3 divided doses every 2-4 hrs Maintenance dose: 5 – 7 mg/kg/day (begin 12 hrs after LD) Plasma phenytoin level and decrease in seizure frequency For toxic effects, monitor blood sugar levels, neurological function, hepatic function, plasma albumin References (Guidelines, Drug Info Sources) http://www.thomsonhc.com.db.usip.edu/hcs/librarian/ND_PR/Main/SBK/2/PFPUI/q13GLHS1szV0pI/ND_PG/PRI H/CS/B625F1/ND_T/HCS/ND_P/Main/DUPLICATIONSHIELDSYNC/C12500/ND_B/HCS/PFActionId/hcs.com mon.RetrieveDocumentCommon/DocId/0031/ContentSetId/31/SearchTerm/Phenytoin%20/SearchOption/BeginWit h#secN104992 (accessed on 8/17/06) Lexi-Comp On-line.Phenytoin. Updated 8/14/06; Accessed 8/18/06; http://www.crlonline.com/crlsql/servlet/crlonline Garnett W. Gidal BE. Epilepsy. In Pharmacotherapy: A Pathophysiologic Approach Sixth Ed. Editors: DiPiro JT. Talbert RL. Yee GC. Matzke GR. Wells BG. Posey LM. 2005. New York. pgs 1023-1048. NAME: Levetiracetam (Keppra) MOA: - The precise mechanism by which levetiracetam exerts its antiepileptic effect is unknown. - unrelated to other seizure drugs - However, several studies have suggested the mechanism may involve one or more of the following: o o o o inhibition of voltage-dependent N-type calcium channels blockade of GABA-ergic inhibitory transmission through displacement of negative modulators reduction of delayed rectifier potassium current binding to synaptic proteins which modulate neurotransmitter release Efficacy (Indication/Use): - FDA Approved Indications: Partial seizure; Adjunct SAFETY: Adverse Effects: Sedation, fatigue, co-ordination difficulties, behavior disturbances (agitation, irritability, depression) Major Drug Interactions: None Contraindications: hypersensitivity to levetiracetam or any component of the product Precautions: - hemodialysis; reduced levels of levetiracetam - renal impairment; potential toxicity due to total body clearance reductions of 40% (creatinine clearance (Clcr) 50 to 80 mL/min), 50% (Clcr 30 to 50 mL/min), 60% (Clcr less than 30 mL/min), and 70% (anuria) - sudden withdrawal of therapy; increased seizure frequency possible - suicides have occurred Pregnancy Category: C Kinetics: - Negligible protein binding 66% renally clearance; the rest is metabolized in the blood by enzymatic hydrolysis No therapeutic drug level monitoring Dosage & Administration - Initial: 500 mg twice daily; may increase every 2 weeks by 500 mg/dose to a maximum of 1500 mg twice daily. Doses - >3000 mg/day have been used in trials; however, there is no evidence of increased benefit. Renal Impairment Clcr >80 mL/minute: 500-1500 mg every 12 hours Clcr 50-80 mL/minute: 500-1000 mg every 12 hours Clcr 30-50 mL/minute: 250-750 mg every 12 hours Clcr <30 mL/minute: 250-500 mg every 12 hours End-stage renal disease patients using dialysis: 500-1000 mg every 24 hours; a supplemental dose of 250-500 mg following dialysis is recommended Monitoring - Patients should be monitored for a reduction in the frequency and severity of seizures. Patients receiving levetiracetam should be monitored for signs and symptoms of hypersensitivity to it. References (Guidelines, Drug Info Sources) http://www.thomsonhc.com.db.usip.edu/hcs/librarian/ND_PR/Main/SBK/2/PFPUI/q13GLHS1sAcjcx/ND_PG/PRI H/CS/F29CF8/ND_T/HCS/ND_P/Main/DUPLICATIONSHIELDSYNC/84FDDF/ND_B/HCS/PFActionId/hcs.co mmon.RetrieveDocumentCommon/DocId/2017/ContentSetId/31/SearchTerm/levetiracetam/SearchOption/BeginWi th#secN70574 (accessed 8/18/06) Lexi-Comp On-line.Keppra. Updated 8/11/06; Accessed 8/18/06; http://www.crlonline.com/crlsql/servlet/crlonline Garnett W. Gidal BE. Epilepsy. In Pharmacotherapy: A Pathophysiologic Approach Sixth Ed. Editors: DiPiro JT. Talbert RL. Yee GC. Matzke GR. Wells BG. Posey LM. 2005. New York. pgs 1023-1048. NAME: Topiramate (Topamax) MOA: - Blocks neuronal voltage-dependent sodium channels - Enhances GABA(A) activity - Antagonizes AMPA/kainate glutamate receptors - Weakly inhibits carbonic anhydrase Efficacy (Indication/Use): - FDA approved indications: Initial and adjunctive therapy for partial seizures as well as generalized, tonic-clonic seizures SAFETY: Adverse Effects: KIDNEY STONES, WEIGHT LOSS, PSCHOMOTOR SLOWING, ACUTE ANGLE GLAUCOMA, OLIGOHYDROSIS (decreased sweating; heat intolerance; hyperthermia) , METABOLIC ACIDOSIS(non-anion gap; decreases serum bicarbonate), somnolence, fatigue, headache, dizziness Major Drug Interactions: - May increase phenytoin and haldol concentrations - May decrease birth control, digoxin, lithium Contraindications: Hypersensitivity to topiramate or any component of its formulation Precautions: - Behavioral disorders or cognitive deficits - Concomitant use of topiramate with valproic acid (associated with hyperammonemia with or without encephalopathy) - Conditions or therapies that predispose to acidosis (such as renal disease, severe respiratory disorders, status epilepticus, diarrhea, surgery, ketogenic diet or drugs) - Paresthesia - Renal or hepatic impairment - Withdraw gradually to avoid increased seizure frequency Pregnancy Category: C Kinetics: - No significant protein binding - 40-70% of dose is excreted unchanged in urine - Fraction of drug is hepatically metabolized, which would be increased by enzyme inducing drugs - T ½ is 15-23 hours Dosage & Administration - Take with or with out food - Partial onset seizures: Initial: 25-50 mg/day (given in 2 divided doses) for 1 week; increase at weekly intervals by 25-50 - Monitoring - mg/day until response; usual maintenance dose: 100-200 mg twice daily. Doses >1600 mg/day have not been studied. Primary generalized tonic-clonic seizures: Use initial dose as listed above for partial onset seizures, but use slower initial titration rate; titrate upwards to recommended dose by the end of 8 weeks; usual maintenance dose: 200 mg twice daily. Doses >1600 mg/day have not been studied. Therapeutic o A reduction in seizure frequency and severity is indicative of therapeutic response to topiramate Toxic o Baseline and periodic serum bicarbonate levels during treatment o Renal function in the elderly o Body weight o Clinical evidence of cognitive dysfunction (memory impairment, poor judgement, confusion o Clinical evidence of acute or chronic metabolic acidosis, such as hyperventilation, fatigue, anorexia, cardiac arrhythmias or stupor. o Hyperammonemia signs and symptoms References (Guidelines, Drug Info Sources) http://www.thomsonhc.com.db.usip.edu/hcs/librarian/ND_PR/Main/SBK/1/PFPUI/q13GLHS1sAlTuy/ND_PG/PRI H/CS/3A970B/ND_T/HCS/ND_P/Main/DUPLICATIONSHIELDSYNC/2EACD1/ND_B/HCS/PFActionId/hcs.co mmon.RetrieveDocumentCommon/DocId/1742/ContentSetId/31/SearchTerm/topiramate/SearchOption/BeginWith #secN77375 (accessed 8/17/06) Lexi-Comp On-line.Topamax. Updated 8/11/06; Accessed 8/17/06; http://www.crlonline.com/crlsql/servlet/crlonline Garnett W. Gidal BE. Epilepsy. In Pharmacotherapy: A Pathophysiologic Approach Sixth Ed. Editors: DiPiro JT. Talbert RL. Yee GC. Matzke GR. Wells BG. Posey LM. 2005. New York. pgs 1023-1048. NAME: Lamotrigine (Lamictal) MOA: - Blockade of both voltage-gated and use dependant sodium channels - Dose dependent inhibition of Ca++ currents (possibly pre-synaptic) - Blocks release of excitatory amino acid neurotransmitters (glutamate & aspartate) Efficacy (Indication/Use): - FDA approved for use in partial seizures (monotherapy and adjunctive) - Alternative therapy for absence seizures. SAFETY: Adverse Effects: RASH (especially with high doses or given with valproic acid), DIPLOPIA, DROWSINESS, ATAXIA, headache - ADE’s are more common when given with other AEDs Major Drug Interactions: - Other “inducing agents” and oral contraceptives may alter plasma concentrations, reducing lamotigine half life by as much as 50% - Valproic acid inhibits the clearance of lamotrigine even if given in small doses - Lamotigine does not seem to alter the kinetics of any medications Contraindications: hypersensitivity to lamotrigine or any component of the product Precautions: - abrupt drug discontinuation - d/c therapy at first sign of rash - fatal hypersensitivity reactions have occurred - concomitant administration of valproic acid with lamotrigine may increase the risk of Stevens-Johnson syndrome or other potentially life-threatening rashes - blood dyscrasias have occurred with therapy Pregnancy Category: C Kinetics: - 98% bioavailabile - Food has no effect - Metabolized hepatically via glucuronosyl transferase - T ½ ~ 24-29 hours - Clearance is higher in children and lower in the elderly - No serum concentration established Dosage & Administration -Patients receiving AED regimens containing valproic acid: Initial dose: 25 mg every other day for 2 weeks, then 25 mg every day for 2 weeks. Dose may be increased by 25-50 mg every day for 1-2 weeks in order to achieve maintenance dose. Maintenance dose: 100-400 mg/day in 1-2 divided doses (usual range 100-200 mg/day). - Patients receiving enzyme-inducing AED regimens without valproic acid: Initial dose: 50 mg/day for 2 weeks, then 100 mg in 2 doses for 2 weeks; thereafter, daily dose can be increased by 100 mg every 1-2 weeks to be given in 2 divided doses. Usual maintenance dose: 300-500 mg/day in 2 divided doses; doses as high as 700 mg/day have been reported - Can disperse in juice or water Monitoring - Seizure, frequency and duration, - Serum levels of concurrent anticonvulsants, hypersensitivity reactions, especially rash References (Guidelines, Drug Info Sources) http://www.thomsonhc.com.db.usip.edu/hcs/librarian/ND_PR/Main/SBK/1/PFPUI/q13GLHS1sAwGYh/ND_PG/P RIH/CS/5BBDC5/ND_T/HCS/ND_P/Main/DUPLICATIONSHIELDSYNC/83AF78/ND_B/HCS/PFActionId/hcs. common.RetrieveDocumentCommon/DocId/1470/ContentSetId/31/SearchTerm/lamotrigine/SearchOption/BeginW ith#secN74168 (accessed 8/18/06) Lexi-Comp On-line.Lamictal. Updated 8/11/06; Accessed 8/18/06; http://www.crlonline.com/crlsql/servlet/crlonline Garnett W. Gidal BE. Epilepsy. In Pharmacotherapy: A Pathophysiologic Approach Sixth Ed. Editors: DiPiro JT. Talbert RL. Yee GC. Matzke GR. Wells BG. Posey LM. 2005. New York. pgs 1023-1048.