* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Safety lessons learned from aviation
Cardiovascular disease wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Cardiac surgery wikipedia , lookup
Down syndrome wikipedia , lookup
Turner syndrome wikipedia , lookup
Jatene procedure wikipedia , lookup
Marfan syndrome wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Electrocardiography wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Coronary artery disease wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
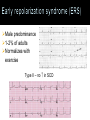
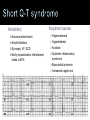
Joseph P. Ornato, MD, FACP, FACC, FACEP Professor & Chairman, Department of Emergency Medicine Self-limited loss of consciousness and postural tone Relatively rapid onset Variable warning symptoms Spontaneous, complete, and usually prompt recovery without medical or surgical intervention Underlying mechanism is transient global cerebral hypoperfusion. Brignole M, et al. Europace, 2004;6:467-537. Real or Apparent TLOC Syncope Neurally-mediated reflex syndromes Orthostatic hypotension Cardiac arrhythmias Structural cardiovascular disease Brignole M, et al. Europace, 2004;6:467-537. Disorders Mimicking Syncope With loss of consciousness (i.e., seizure disorders, concussion) Without loss of consciousness, i.e., psychogenic “pseudosyncope” Structural CardioPulmonary NeurallyMediated Orthostatic 1 2 3 4 • Vasovagal syndrome • Carotid sinus syndrome • Situational • Drug-induced • Autonomic nervous system failure • Bradyarrhythmia • Acute myocardial ischemia • Aortic stenosis • Hypertrophic cardiomyopathy • Pulmonary hypertension • Aortic dissection Cough PostMicturition Primary Secondary Cardiac Arrhythmia Sinus node dysfunction AV block •Tachyarrhythmia VT SVT • Long QT syndrome Unexplained Causes = Approximately 1/3 Acute intoxication (e.g., alcohol) Seizures Sleep disorders Somatization disorder (psychogenic pseudo-syncope) Trauma/concussion Hypoglycemia Hyperventilation Brignole M, et al. Europace, 2004;6:467-537. 40% will experience syncope at least once in a lifetime1 1-6% of hospital admissions2 1% of emergency department visits per year3,4 10% of falls by elderly are due to syncope5 Major morbidity reported in 6%1 (fractures, motor vehicle crashes) Minor injury in 29%1 (lacerations, bruises) 1Kenny RA, Kapoor WN. In: Benditt D, et al. eds. The Evaluation and Treatment of Syncope. Futura;2003:23-27. 2Kapoor W. Medicine. 1990;69:160-175. 3Brignole M, et al. Europace. 2003;5:293-298. Blanc J-J, et al. Eur Heart J. 2002;23:815-820. 5Campbell A, et al. Age and Ageing. 1981;10:264-270. 4 Estimated hospital costs exceeded $10 billion1 Estimated physician office expenses exceeded $470 million2 Over $7 billion is spent annually in the US to treat falls in older adults4 1Kenny RA, Kapoor WN. In: Benditt D, et al. eds. The Evaluation and Treatment of Syncope. Futura;2003:23-27. v. 6.0. Solucient LLC, Evanston IL. 3Farwell D, et al. J Cardiovasc Electrophysiol. 2002;13(Supp):S9-S13. 4Olshansky B. In: Grubb B and Olshansky B. eds. Syncope: Mechanisms and Management. Futura. 1998:15-71. 2OutPatientView 100 80 73%1 71%2 60%2 60 37%2 40 20 0 1Linzer 2Linzer Anxiety/ Depression M. J Clin Epidemiol. 1991;44:1037. M. J Gen Int Med. 1994;9:181. Alter Daily Activities Restricted Driving Change Employment Low mortality vs. high mortality Neurally-mediated syncope vs. syncope with a cardiac cause Soteriades ES, Evans JC, Larson MG, et al. Incidence and prognosis of syncope. N Engl J Med. 2002;347(12):878-885. [Framingham Study Population] Distinguish true syncope from syncope mimics Determine presence of heart disease Establish the cause of syncope with sufficient certainty to: Assess prognosis confidently Initiate effective preventive treatment Initial Examination Detailed patient history Physical exam ECG Supine and upright blood pressure Monitoring Holter Event Insertable loop recorder (ILR) Cardiac Imaging Special Investigations Head-up tilt test Hemodynamics (cardiac cath) Electrophysiology study Brignole M, et al. Europace, 2004;6:467-537. Circumstances of recent event Eyewitness account of event Symptoms at onset of event Sequelae Medications Circumstances of prior events Concomitant disease, especially cardiac Pertinent family history Cardiac disease Sudden death Metabolic disorders Past medical history Neurological history Syncope Brignole M, et al. Europace, 2004;6:467-537. Vital signs Heart rate Orthostatic blood pressure change Cardiovascular exam: Is heart disease present? ECG: Long QT, pre-excitation, conduction system disease Echo: LV function, valve status, hypertrophic cardiomyopathy Neurological exam Carotid sinus massage Perform under clinically appropriate conditions preferably during head-up tilt test Monitor both ECG and BP Brignole M, et al. Europace, 2004;6:467-537. Neurally-mediated Vasovagal Syncope (VVS) Carotid Sinus Syndrome (CSS) Cardiac arrhythmia Tachy-brady syndrome Long QT syndrome Torsade de pointes Brugada syndrome Drug-induced Structural cardio-pulmonary disease Orthostatic Vasovagal syncope (VVS) Carotid sinus syndrome (CSS) Situational syncope Post-micturition Cough Swallow Defecation Blood drawing, etc. Most common form of syncope 8% to 37% (mean 18%) of syncope cases Depends on population sampled Young without structural heart disase, ↑ incidence Older with structural heart disease, ↓ incidence Useful as diagnostic adjunct to confirm vasovagal syncope Useful in teaching patients to recognize prodromal symptoms Brignole M, et al. Europace. 2004;6:467-537. 60° - 80° Etiology Drug-induced (very common) Diuretics Vasodilators Primary autonomic failure Multiple system atrophy Parkinson’s Disease Postural Orthostatic Tachycardia Syndrome (POTS) Secondary autonomic failure Diabetes Alcohol Amyloid Syncope clearly associated with carotid sinus stimulation is rare (≤1% of syncope) CSS may be an important cause of unexplained syncope/falls in older individuals Kenny RA, et al. J Am Coll Cardiol. 2001;38:1491-1496. Brignole M, et al. Europace. 2004;6:467-537. Sutton R. In: Neurally Mediated Syncope: Pathophysiology, Investigation and Treatment. Blanc JJ, et al. eds. Armonk, NY: Futura;1996:138. Method1 Massage, 5-10 seconds Don’t occlude Supine and upright posture (on tilt table) Outcome 3 second asystole and/or 50 mmHg fall in systolic BP with reproduction of symptoms = Carotid Sinus Syndrome 1Kenny RA. Heart. 2000;83:564. M. Ann Intern Med. 1997;126:989. 3Munro N, et al. J Am Geriatr Soc. 1994;42:1248-1251. 2Linzer Absolute contraindications2 Carotid bruit, known significant carotid arterial disease, previous CVA, MI last 3 months Complications Primarily neurological Less than 0.2%3 Usually transient Ambulatory ECG Holter monitoring Insertable loop recorder (ILR) Tilt table test Includes drug provocation (NTG, isoproterenol) Cardiac catheterization Electrophysiology study (EPS) Brignole M, et al. Europace, 2004;6:467-537. OPTION 12-Lead 10 Seconds 1 day Holter Monitor Event Recorders 7-30 days (non-lead and loop) Up to 14 Months ILR 0 1 2 3 4 5 6 7 8 TIME (Months) Brignole M, et al. Europace, 2004;6:467-537. 9 10 11 12 13 14 Initial Evaluation History, Physical Exam, ECG, Cardiac Massage Yield (%) 38-40 Other Tests/Procedures Head-Up Tilt External Cardiac Monitoring Insertable Loop Recorder (ILR) EP Study Exercise Test EEG 27 5-13 43-883-5 <2-5 0.5 0.3-0.5 EEG Head CT Brignole M, et al. Europace. 2004;6:467-537. Includes cardiac arrhythmias and structural heart disease Often life-threatening Suspect if syncope exercise-induced May be warning of critical CV disease Tachy and brady arrhythmias Myocardial ischemia, aortic stenosis, pulmonary hypertension, aortic dissection Assess culprit arrhythmia or structural abnormality aggressively Initiate treatment promptly Bradyarrhythmias Sinus arrest, exit block High grade or acute complete AV block Can be accompanied by vasodilatation (VVS, CSS) Tachyarrhythmias Atrial fibrillation/flutter with rapid ventricular rate (eg, pre-excitation syndrome) Paroxysmal SVT or VT Torsade de pointes Cardiovascular pathology Coronary artery disease Severe left ventricular dysfunction Cardiomyopathy Hypertrophic cardiomyopathy Arrhythmogenic right ventricular cardiomyopathy Congenital heart disease, especially coronary artery anomalies Valvular heart disease Cardiac pacemaker and conducting system disease Hereditary channelopathies (Sudden Arrhythmic Death Syndrome (SADS)) Brugada syndrome Early repolarization syndrome (ERS) Long QT syndrome (LQTS) Short QT syndrome (SQTS) Catecholaminergic polymorphic ventricular tachycardia (CPVT) Often present as recurrent syncope or brief seizures in children or young adults before sudden death occurs May have young relatives who have had sudden death ECG findings are often diagnostic Effective preventive treatment is available (ICD) Astute emergency physician may be the ONLY healthcare provider who can make the diagnosis and prevent tragic loss of a young life Male predominance Autosomal dominant Common in Asians 40-60% prevalence of life-threatening ventricular arrhythmias and SCD Presents as syncope Downsloping ST-segment elevation in ECG leads V1–3 Type I – 43% ↑ in SCD Male predominance 1-2% of adults Normalizes with exercise Type II – no ↑ in SCD Hereditary Autosomal recessive (Jervell Lange-Nielsen syndrome) with hereditary nerve deafness Autosomal dominant (Romano Ward syndrome w/out deafness) Syncope, VF, SCD Acquired causes Hypocalcemia Hypokalemia Hypomagnesemia Ischemia Anorexia CNS pathology QT-prolonging drugs (www.azcert.org) 𝑄𝑇𝑐𝑜𝑟𝑟𝑒𝑐𝑡𝑒𝑑 = 𝑄𝑇𝑚𝑒𝑎𝑠𝑢𝑟𝑒𝑑 𝑅𝑅𝑖𝑛𝑡𝑒𝑟𝑣𝑎𝑙 Bazett Formula QTc = 0.35-0.44 at HR= 60 Hereditary Acquired causes Autosomal dominant Hypercalcemia Atrial fibrillation Hyperkalemia Syncope, VF, SCD Acidosis Early repolarization inferolateral leads in 65% Systemic inflammatory syndrome Myocardial ischemia Increased vagal tone Anomalous L coronary artery off the pulmonary artery Hypertrophic cardiomyopathy Severe aortic stenosis Catecholaminergic polymorphic ventricular tachycardia Hereditary defect in myocardial calcium handling Stress-related syncope, VF, SCD ECG – unexplained sinus bradycardia at rest 50% carry a diagnosis of epilepsy before correct diagnosis established Syncope is a common symptom with many causes Deserves thorough investigation and appropriate treatment Clinical decision (observation) unit at VCU is an appropriate location to initiate the evaluation