* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Slide 1
Cardiovascular disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Coronary artery disease wikipedia , lookup
Cardiac surgery wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
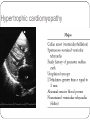
Hypertrophic cardiomyopathy wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
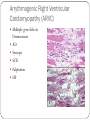
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
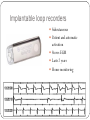
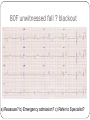
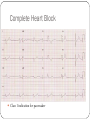
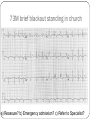
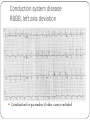
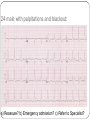
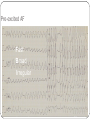
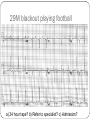
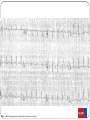
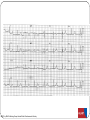
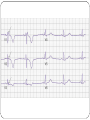
"Blackouts” Dr Paul Venables Consultant Cardiologist [email protected] Blackouts Introduction Epidemiology NICE Clinical Guideline Historic standard of care Key recommendations Practice points Red Flags Blackout: Definition Character: Loss of consciousness Rapid onset Transient/Short duration Spontaneous recovery Epidemiology Increase with old age Peak in teenage² Incidence 2.6 -19.5/1000¹ Incidence according to age and sex Often unreported Affects half population during lifetime 1. 2. Soteriades et al. NEJM 2002 Ganzeboom et al. J Cardiovasc Electrophysiol 2006 Blackout in the UK: Scale 4% ED attendances 550,000 per annum Primary care Finished consultant episodes: Syncope /collapse 6% Acute admissions >100,000 per annum¹ Average Length of stay 3.9 days Falls not included 1 .NHS Health and Social care information centre (2009): Hospital episode statistics Blackout: Causes Reflex syncope Orthostatic Hypotension 56-73% 1-10% Cardiac Neurological Unexplained Psychogenic Rare 6-37% 1-6% 5-20% Survival after presentation Soteriades et al. NEJM 2002 NICE Clinical Guideline 109: Historic standard of care Range of clinicians Non-Standardised investigation: Underuse of ECG Overuse of EEG Poor Referral: Wrong speciality or unnecessary Delayed diagnosis: Dangerous conditions missed Inaccurrate: 20-30% “epilepsy” had cardiac cause¹ Inefficient: Resource implications 1. NICE CG20 Epilepsy in adults and children 2004 NICE Clinical Guideline: Key priorities Define pathways: Algorithm Initial assessment: History ECG Risk stratification Appropriate referral for specialist assessment Initial assessment: History and examination • Exact history of event: • Personal and collateral history • Posture, prodrome etc • Previous blackout? • Medical history and family history • Medication • Examination • Vital signs • Other cardiovascular and neurological signs +/- Lying and standing blood pressure 1.1.4.2 Red flags: Urgent assessment and treatment Refer for specialist cardiovascular assessment within 24 hours, patients with: ECG abnormality Heart failure TLoC during exertion Family history of SCD <40 or ICC New or unexplained breathlessness Heart murmur Consider referring >65 years and TLoC without prodromal symptoms 1.1.2.3 ECG “Red Flags" Use automated interpretation...... if not possible obtain expert opinion! Conduction abnormality Inappropriate persistent bradycardia Any ventricular arrhythmia (including ventricular ectopic beats) Long QT (corrected QT > 450 ms) and short QT (corrected QT < 350 ms) Brugada syndrome Ventricular pre-excitation Left or right ventricular hypertrophy Abnormal T wave inversion Pathological Q waves Atrial arrhythmia (sustained) Paced rhythm Diagnosis based on the initial assessment: Diagnose uncomplicated faint when: There are features suggestive of uncomplicated faint such as: Posture Provoking factors (such as pain or a medical procedure) Prodromal symptoms Diagnose situational syncope when: Syncope is clearly and consistently provoked by straining during micturition or by coughing or swallowing Diagnose orthostatic hypotension when: The history is typical and Lying and standing blood pressure confirms postural drop 1.2.3 Referral for specialist cardiovascular assessment Refer all people with TLoC for a specialist cardiovascular assessment except: Uncomplicated faint Situational syncope Orthostatic hypotension Presentation is strongly suggestive of epileptic seizures 1.3.2 Diagnostic tests for different types of syncope Ambulatory ECG: Arrhythmic cause Unexplained cause (after CSM where appropriate) Exertional syncope: Initial investigations negative Criteria to determine type of ambulatory ECG: TLoC at least several times a week: Holter monitoring If no TLoC occurs during monitor, offer external event recorder TLoC every 1–2 weeks: External event recorder Further TLoC outside the period of external event recording, offer an ILR TLoC less than once every 2 weeks: Offer an ILR Holter monitor should not usually be offered unless there is evidence of a conduction abnormality on the 12-lead ECG Implantable loop recorders Subcutaneous Patient and automatic activation Stores EGM Lasts 2 years Home monitoring NICE: ILR vs “Conventional testing” Low diagnostic yield with external recorders Much better symptom–ECG correlation with ILR High initial cost May be more cost-effective Tilt Test Vasovagal syncope: Consider a tilt test only if: Recurrent and affecting their quality of life, or high risk of injury Pacing considered Advice for patients: Condition appropriate advice Driving Safety at work Summary: Practice points History and ECG: Red flags: Refer “urgently” Epilepsy: Refer to Neurology Unclear Cause: Refer to Cardiology Reflex syncope, Situational syncope and Orthostatic hypotension: Advise and Reassure Summary: Loads more ECG’s: ECG red flags Robust diagnosis: Diagnose and treat severe cardiac conditions Avoid misdiagnosis, especially epilepsy Blackouts: Clinical ECG’s not to be missed Sudden cardiac death Inherited cardiac conditions 80F unwitnessed fall ? blackout a) Reassure? b) Emergency admission? c) Refer to Specialist? Complete Heart Block Class 1 indication for pacemaker 73M brief blackout standing in church a) Reassure? b) Emergency admission? c) Refer to Specialist? Conduction system disease RBBB, left axis deviation 2a indication for pacemaker if other causes excluded 24 male with palpitations and blackout: a) Reassure? b) Emergency admission? c) Refer to Specialist? Wolff-Parkinson-White syndrome (WPW) Common 0.1% prevalence AVRT Sudden Cardiac Death: - 0.15 – 0.25% per year Pre-excited AF VF induced by “R on T” Avoid AV Node blocking drugs Pre-excited AF Fast Broad Irregular 29M blackout playing football a) 24 hour tape? b) Refer to specialist? c) Admission? Hypertrophic cardiomyopathy ©2011 by BMJ Publishing Group Ltd and British Cardiovascular Society Brugada Syndrome Gene defect of cardiac Sodium Ion-channels (SCN5A) Associated with SCD Development of VF ICD: Syncope aborted SCD EPS inducibility Identification of families ©2011 by BMJ Publishing Group Ltd and British Cardiovascular Society Long QT-Syndrome QTc >450ms Genetic Ion-channel defect Syncope (seizures) and SCD Drugs Triggered activity Dispersion of refractoriness After depolarisations in phase 3 or 4 Exceed threshold Trigger further depolarisation Torsades de points in LQTS Arrythmogenic Right Ventricular Cardiomyopathy (ARVC) Multiple gene defects: Desmosomes AD Syncope SCD Palpitation HF Sudden cardiac death CHD Cardiomyopathy: Hypertrophic cardiomyopathy Channelopathies: Long QT syndrome Brugada syndrome “Electrical” diseases: Wolff-Parkinson-White 5% Other* 15% Cardiomyopathy 80% Coronary Heart Disease Prevention of SCD >95% patient die after out of hospital cardiac arrest Identify patients at risk before it occurs ICD is proven to improve survival as a primary preventative treatment in: Ischaemic/non-ischaemic cardiomyopathy Inherited cardiac conditions Sudden death syndromes: Technology Impact Diagnostic devices Prevention of SCD Pacemakers Cure Implantable defibrillators Stroke prevention Catheter Ablation Patient reassurance Thankyou www.guidance.nice.org.uk/CG109 www.arrhythmiaalliance.org.uk www.dft.gov.uk/dvla/medical/ataglance.aspx [email protected]