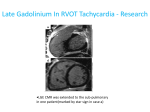
* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download S1936878X15008608_mmc1 - JACC: Cardiovascular Imaging
Survey
Document related concepts
Transcript
ONLINE APPENDIX Echocardiography LV end-diastolic and end-systolic diameters and septal and posterior wall thicknesses were measured from parasternal long-axis views using M-mode echocardiography. LV volumes and LV ejection fraction were measured using the Simpson biplane method from twochamber and four-chamber apical views. Mitral inflow recordings were obtained with pulsed Doppler and used to quantify early and late wave peak velocities and the early-to-late diastolic flow ratio. Tissue Doppler imaging at the lateral and septal mitral annulus was performed to measure the ratio between early transmitral flow and mean lateral and septal early diastolic peak tissue velocity used as an estimate of LV filling pressure. Systolic pulmonary arterial pressure was estimated by applying the modified Bernoulli equation to the maximal tricuspid regurgitation velocity assessed by conventional Doppler imaging. LS was computed from the standard LV apical views (two, three, and four chambers) using 2D speckle-tracking echocardiography analysis by automated function imaging (AFI, ECHO-Pac, GE Healthcare). For LS processing, the R wave peak on the electrocardiogram was taken to indicate the end of diastole. Briefly, after manual initialization of the end-systolic endocardial border, the region of interest was automatically positioned to track the LV speckles frame by frame throughout the cardiac cycle. Endocardial contour and width were adjusted manually when necessary to provide optimal tracking. Segments with poor-quality tracking were discarded manually. Cardiac magnetic resonance imaging (MRI) MRI was performed within 5 days after echocardiography, using a 1.5-T machine (Magnetom Avanto, Siemens Healthcare, Erlangen, Germany). All acquisitions were recorded during a breath-hold, and balanced steady-state free precession sequences were synchronized to the electrocardiogram. Data analysis was performed offline on a dedicated computer workstation (Argus, Siemens Medical Systems, Malvern, PA, USA) by two experienced radiologists (JFD and JT) blinded to the patients’ clinical data. Semi-automated software was used to compute LV ejection fraction from consecutive short-axis slices. The end-systolic and end-diastolic phases were defined, and an auto-level function was then applied for automatic endocardial contour detection. If necessary, the contours of key areas were corrected manually. Special care was taken to avoid partial volume effects at valve planes, and papillary muscles and trabecular structures were included in the ventricular volume. LGE was defined as abnormal myocardial hyperintensity on inverse recovery sequences 10 minutes after an intravenous injection of 0.2 mmol/Kg gadolinium (Dotarem, Guerbet, Aulnay-sous-Bois, France). To determine the optimal inversion recovery time, a specific scouting sequence was acquired before the LGE images. Phase-sensitive inversion recovery images were acquired routinely after the LGE images (repetition time, 835 ms; echo time, 3.3 ms; flip angle, 10°; matrix size, 256x156; field of view, 300x270 mm; slice thickness, 8 mm; and GRAPPA acceleration factor, 2). The image acquisition time ranged from 12 to 20 seconds depending on heart rate. Five phase-sensitive inversion recovery images were acquired in the short-axis plane encompassing the LV. A single slice was acquired in the four-chamber and two-chamber views. Each of the 17 LV segments was evaluated separately for LGE.