* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Integration of 3D Imaging Data in the Assessment of Aortic Stenosis
Remote ischemic conditioning wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Marfan syndrome wikipedia , lookup
Pericardial heart valves wikipedia , lookup
Turner syndrome wikipedia , lookup
Artificial heart valve wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Jatene procedure wikipedia , lookup
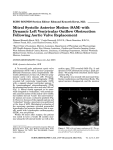
Integration of 3D Imaging Data in the Assessment of Aortic Stenosis Impact on Classification of Disease Severity Bridget O’Brien, MD; Paul Schoenhagen, MD; Samir R. Kapadia, MD; Lars G. Svensson, MD, PhD; Leonardo Rodriguez, MD; Brian P. Griffin, MD; E. Murat Tuzcu, MD; Milind Y. Desai, MD Downloaded from http://circimaging.ahajournals.org/ by guest on May 11, 2017 Background—In patients with aortic stenosis (AS), precise assessment of severity is critical for treatment decisions. Estimation of aortic valve area (AVA) with transthoracic echocardiographic (TTE)-continuity equation (CE) assumes a circular left ventricular outflow tract (LVOT). We evaluated incremental utility of 3D multidetector computed tomography (MDCT) over TTE assessment of AS severity. Methods and Results—We included 51 patients (age, 81⫾8 years; 61% men; mean gradient, 42⫾12 mm Hg) with calcific AS who underwent evaluation for treatment options. TTE parameters included systolic LVOT diameter (D) and continuous and pulsed wave (CW and PW) velocity-time integrals (VTI) through the LVOT and mean transaortic gradient. MDCT parameters included systolic LVOT area, ratio of maximal to minimal LVOT diameter (eccentricity index), and aortic planimetry (AVAp). TTE-CE AVA [(D2⫻0.786⫻VTIpw)/VTIcw] and dimensionless index (DI) [VTIpw/VTIcw] were calculated. Corrected AVA was calculated by substituting MDCT LVOT area into CE. The majority (96%) of patients had eccentric LVOT. LVOT area, measured on MDCT, was higher than on TTE (3.84⫾0.8 cm2 versus 3.03⫾0.5 cm2, P⬍0.01). TTE-AVA was smaller than AVAp and corrected AVA (0.67⫾0.1cm2, 0.82⫾0.3 cm2, and 0.86⫾0.3 cm2, P⬍0.01). Using TTE measurements alone, 73% of patients had congruence for severe AS (DI ⱕ0.25 and CE AVA ⬍0.8 cm2), which increased to 92% using corrected CE. Conclusions—In patients with suspected severe AS, incorporation of MDCT-LVOT area into CE improves congruence for AS severity. (Circ Cardiovasc Imaging. 2011;4:566-573.) Key Words: aortic stenosis 䡲 transthoracic echocardiography 䡲 multidetector computed tomography 䡲 aortic valve area A equation is based on the assumption of a circular shape of the left ventricular outflow tract (LVOT). However, previous studies describe a high prevalence of oval LVOT shape, potentially causing underestimation of AVA calculation with the continuity equation.4 – 8 The recent use of multidetector computed tomography (MDCT) for preprocedural assessment of the aortic valve/ root in the context of TAVI allows us to evaluate the impact of 3D image analysis on the congruence between severity criteria.4 –7,9 –13 The aim of our study was to evaluate (1) differences in echocardiographic and MDCT-derived AVA and (2) whether incorporation of MDCT LVOT area into continuity equation improves congruence between various criteria for severity of AS. ortic stenosis (AS) is the most common acquired valve disease in the developed world, with an age-related increase in prevalence.1 In symptomatic patients with severe AS, conventional aortic valve replacement still remains the standard of care; however, elderly patients frequently have several comorbidities that make surgery potentially prohibitive. Because of recent advances in percutaneous techniques such as transcatheter aortic valve implantation (TAVI), the therapeutic options have expanded to include patients considered at high risk for surgery.2 Clinical Perspective on p 573 Precise assessment of AS severity is essential for appropriate treatment decision-making. Standard echocardiographic assessment of aortic valve area (AVA) relies on congruence of several criteria including transaortic gradients and AVA, calculated by continuity equation and/or planimetry.3 The standard 2D estimation of AVA using the continuity Methods Fifty-one consecutive symptomatic patients, with suspected severe AS referred to our institution for evaluation for potential surgical versus percutaneous treatment options between the years 2006 to Received March 4, 2011; accepted June 29, 2011. From the Heart and Vascular Institute (B.O., P.S., S.R.K., L.G.S., L.R., B.P.G., E.M.T., M.Y.D.) and Imaging Institute (P.S., L.R., M.Y.D.), the Cleveland Clinic, Cleveland, OH. Correspondence to Milind Y. Desai, MD, Tomsich Department of Cardiovascular Medicine, Heart and Vascular Institute, Cleveland Clinic, 9500 Euclid Ave, Desk J1-5, Cleveland, OH 44195. E-mail [email protected] © 2011 American Heart Association, Inc. Circ Cardiovasc Imaging is available at http://circimaging.ahajournals.org 566 DOI: 10.1161/CIRCIMAGING.111.964916 O’Brien et al Aortic Stenosis, MDCT, and Echocardiography 567 Downloaded from http://circimaging.ahajournals.org/ by guest on May 11, 2017 Figure 1. Patient with suspected severe aortic stenosis. Ejection fraction was 55%. On transthoracic echocardiography, left ventricular outflow tract (LVOT) diameter was measured as 1.8 cm (A). Notice the heavily calcified valve in short axis (B). AorticVTI was 127 and LVOTVTI was 35 (C and D). Based on that, aortic valve area (AVA) was measured as 0.70 cm2. However, after multiplanar reformatting, the LVOT was elliptical on multidetector computed tomography, with an eccentricity index of 1.2, measured as a ratio of the largest (dark line)/shortest (white line) diameter (E), and measured LVOT area was 3.24 cm2. Putting that in the continuity equation gave a corrected AVA of 0.9 cm2. CT planimetry AVA was 0.98 cm2 (F). 2007, were included in this observational study. Patients were included if they had undergone clinically indicated comprehensive standard and Doppler echocardiography and contrast-enhanced MDCT of the aortic root at our institution within 1 week of each other. We excluded patients with bicuspid aortic valve morphology because there is a high proportion of aortic root and annular eccentricity. Patients with advanced renal insufficiency or other contraindications to intravenous contrast dye were excluded. Baseline, clinical, demographic, and imaging data were collected. Surgical risk was assessed, based on clinical and imaging data, and a Euroscore was calculated in each patient.14 This observational study was approved by the institutional review board, with waiver of individual informed consent. Transthoracic Echocardiography Surface echocardiograms were obtained using commercially available systems (Siemens, Erlangen, Germany; General Electric, Milwaukee, WI, and Philips, Best, The Netherlands). Left ventricular ejection fraction (EF) was calculated according to guidelines.15 Peak and mean transaortic valvular gradients were measured in all patients using continuous wave Doppler in standard echocardiographic views. Velocity time integrals (VTI) across aortic valve (using continuous wave Doppler) and LVOT (using pulsed wave Doppler) were also recorded. Diameter of the LVOT was measured from the parasternal long-axis in a standard fashion during midsystole. LVOT area was derived from this measurement in a standard fashion. Transthoracic AVA (TTE-AVA) was calculated by using the continuity equation in a standard fashion using the following formula (Figure 1A through 1D): (LVOT diameter2⫻0.786⫻LVOTVTI)/ Aortic valveVTI. In addition, dimensionless index (DI) was recorded as follows: LVOTVTI/Aortic valveVTI. All measurements were performed according to previously published guidelines.3 MDCT Acquisition and Analysis All subjects were scanned on standard MDCT scanner (Siemens Medical Solutions, Definition Dual Source, Erlangen, Germany) after administration of an iodinated contrast agent (80 to 100 mL of Ultravist 370) at 4 to 5 mL/s followed by 30 to 50 mL of normal saline at the same rate. A contrast bolus tracking technique using a region of interest in the ascending aorta was used. Once the desired attenuation was reached, scanning was initiated in the craniocaudal direction during a single inspiratory breath-hold. All patients were scanned from the level of the carina to the mid left ventricle. Spiral data were acquired with retrospective ECG gating using the follow- 568 Circ Cardiovasc Imaging September 2011 Downloaded from http://circimaging.ahajournals.org/ by guest on May 11, 2017 Figure 1 (Continued). ing parameters: gantry rotation time⫽330 ms; beam collimation⫽32⫻0.6 mm; tube voltage⫽120 kVp; tube current-time product per rotation⫽250 to 410 mAs/rotation; and beam pitch of 0.2 to 0.5. ECG-based tube current modulation was used for all patients, with maximum current turned on between 30% to 70% phases of the cardiac cycle. For the remaining phases, the current was reduced. Images were reconstructed during 10 to 14 phases of the cardiac cycle, depending on the patient heart rate with a temporal resolution of 83 ms and section thickness of 0.75 mm. Typical radiation in the study sample was ⬍12 mSEV. MDCT images were analyzed on a dedicated CT workstation (Terra Recon, CA). The investigator (M.D.), experienced in interpreting cardiac CT, was blinded to the subject’s clinical status and TTE images. The largest cross-sectional area of the LVOT was measured in systole (30% to 40% of the R-R phase), using double oblique images to identify the true short axis, approximately 0.5 to 0.7 cm below the aortic valve “hinge point.” The maximum and minimum diameters of the LVOT were also measured to calculate the eccentricity index (maximum/minimum LVOT diameter after multiplanar reformatting, Figure 1E). Quantitatively, the AVA was determined by planimetry of the aortic valve using a plane parallel to the short axis of the aortic root. The time point of maximal aortic valve opening was identified during systole (usually at 30% to 40% of the R-R interval). The area of the aortic valve opening was found by scrolling through the short axis images toward the tip of the cusps until the smallest opening was found. The planimetered AVA on MDCT (AVAp) was determined by tracing the inside borders of the coronary cusps with electronic calipers and reported in square centimeters (Figure 1F). Corrected Multimodality AVA We then used the LVOT area, measured on MDCT, as part of the continuity equation, to generate a corrected multimodality AVA as follows: (Maximum LVOT areaMDCT⫻LVOTVTI)/Aortic valve VTI. Statistical Analysis All values presented are mean⫾SD values for continuous variables and as percentage of total patients for categorical variables. The 2 independent samples and paired t tests were used to compare continuous variables for comparison between and within groups, respectively. 2 was used for comparison of categoric variables. Pearson correlation coefficient was used to test associations between continuous variables. In addition, interobserver (B.O. and M.D.) and intraobserver (M.D.) reproducibility of various MDCT parameters was measured by using intraclass correlation coefficients. BlandAltman analysis was performed to systematically assess the differences between LVOT area measured using 2 different imaging techniques (echocardiography and MDCT).16 All probability values were 2-sided. A probability value of ⬍0.05 was considered significant. Data assembly statistical comparisons were performed with JMP Software version 6.0.2 and SPSS version 11.5 (SPSS Inc, Chicago, IL). Results Baseline Characteristics The baseline characteristics of the total group and 2 subgroups divided on basis of preserved or low LV EF are shown in Table 1. Mean age was 81⫾8 years, of which 61% were men (with a significantly higher proportion of men in the depressed LV EF subgroup). The mean Euroscore was high, suggesting a fairly high-risk sample at baseline. Approximately two-thirds of the study group had a history of prior open heart surgery. In the study sample, 10 (20%) patients qualified and subsequently underwent TAVI, as part of a clinical trial, whereas 15 (29%) underwent aortic valve replacement and 4 (8%) underwent percutaneous balloon valvuloplasty. The baseline echocardiographic measurements of the total group and 2 subgroups, divided on the basis of preserved or low LV EF, are shown in Table 2. As shown in Table 2, only 31 (59%) patients had an EF ⬎50%, whereas 9 (18%) had EF between 40% and 50% and 11 (24%) had EF ⬍40%. In terms of mean transaortic gradients, 27 (53%) had values ⱖ40 mm Hg, 15 (29%) between 30 to 40 mm Hg and 9 (18%) ⬍30 mm Hg. Only 8% of patients had greater than 2⫹ aortic regurgitation. The MDCT characteristics are also shown in Table 2. The maximum LVOT diameter measured on MDCT O’Brien et al Table 1. Baseline Characteristics of the Study Sample Aortic Stenosis, MDCT, and Echocardiography 569 (96%) had an oval-shaped LVOT (based on an eccentricity index ⬎1.0) as measured on CT. Intraclass correlation coefficients, used to measure reproducibility of various MDCT measurements, were as follows: LVOT area (intraobserver: 0.98 [0.92 to 0.99], interobserver: 0.92 [0.68 to 0.98], both P⬍0.001) and MDCT AVA (intraobserver: 0.93 [0.70 to 0.98], interobserver: 0.82 [0.26 to 0.95], both P⬍0.001). Downloaded from http://circimaging.ahajournals.org/ by guest on May 11, 2017 Variable Total Group (n⫽51) LV EF ⬍50% (n⫽21) LV EF ⱖ50% (n⫽30) P Value Age 81⫾8 82⫾7 80⫾8 0.2 Male sex 31 (61%) 18 (86%) 13 (43%) Hypertension 37 (73%) 13 (62%) 24 (65%) 0.2 Diabetes mellitus 23 (45%) 7 (33%) 16 (53%) 0.2 Smoking history 28 (55%) 11 (52%) 17 (57%) 0.8 Assessment of AVA Documented coronary artery disease 42 (82%) 19 (90%) 23 (77%) 0.2 Documented stroke 7 (14%) 4 (19%) 3 (10%) 0.4 Chronic obstructive pulmonary disease 21 (41%) 8 (38%) 13 (43%) 0.7 Previous cardiac surgery 35 (69%) 17 (81%) 18 (60%) 0.1 Serum creatinine 1.3⫾0.8 1.5⫾1.1 1.2⫾0.4 0.1 AVAp was significantly higher than what was measured by continuity equation on echocardiography (0.82⫾0.25 cm2 versus 0.67⫾0.13 cm2, P⬍0.001). The mean corrected AVA was 0.86⫾0.28 cm2 (which was similar to AVAp, P⫽NS). The mean corrected AVA was similar in patients with preserved versus depressed LV EF, 0.8⫾0.3 cm2 versus 0.9⫾0.3 cm2 (P⫽NS). Body mass index 27⫾5 28⫾5 27⫾5 0.6 Euroscore 25⫾18 37⫾19 16⫾12 ⬍0.001 0.002 LV EF indicates left ventricular ejection fraction. was significantly greater than that on echocardiography (2.73⫾0.4 cm versus 1.96⫾0.15 cm, P⬍0.001). Similarly, LVOT area measured on MDCT was significantly higher than that measured on transthoracic echocardiography (3.84⫾0.8 versus 3.03⫾0.5, P⬍0.01). Bland-Altman analysis (Figure 2) demonstrates that transthoracic echocardiography systematically underestimates LVOT area. Also, 49 patients Table 2. Imaging Characteristics of the Study Sample Congruence Between MDCT and Echocardiography Parameters We subsequently tested the correlation between various Doppler-derived measurements and AVA measured by different techniques, as shown in Table 3 and Figure 3A through 3C. Correlation of mean transaortic gradient with TTE-AVA (measured on continuity) was only modest. However, the correlation of mean transaortic gradient with AVAp measured on MDCT and corrected” AVA was significantly improved as compared with TTE-AVA (probability value for “improvement” in correlation was ⬍0.01). When contrasting patients with normal and abnormal EF, the correlation between mean gradient and TTE-AVA, AVAp, and corrected AVA were much lower in patients with EF ⬍50% than in patients with EF ⱖ50% (probability value for “improvement” in various corresponding correlations were ⬍0.01). Total Group (n⫽51) LV EF ⬍50% (n⫽21) LV EF ⱖ50% (n⫽30) P Value LVOT diameter, cm 1.96⫾0.2 2.02⫾0.2 1.92⫾0.2 0.03 Congruence Between DI and AVA LVOT area 3.03⫾0.5 3.21⫾0.5 2.92⫾0.5 0.03 In terms of TTE-AVA (by continuity equation), 40 (78%) patients had an AVA of ⬍0.8 cm2. The DI was ⱕ0.25 in only 30 (59%) cases. In the study sample, only 37 (73%) of the patients had congruence of criteria for severe AS (DI ⱕ0.25 and TTE-AVA ⬍0.8 cm2). However using an AVAp (MDCT-based) cutoff of ⬍0.8 cm2 for severe AS, the congruence increased to 80% patients. Similarly, if corrected AVA with a cutoff of ⬍0.8 cm2 was used, the number of patients with congruence increased to 92% (probability value for comparison ⬍0.05). Variable Echocardiography 25⫾12 20⫾5 28⫾15 0.02 Aortic valve VTI LVOT VTI 113⫾51 100⫾25 123⫾62 0.1 AVA, continuity equation, cm2 0.67⫾0.1 0.65⫾0.1 0.68⫾0.2 0.5 Peak aortic valve gradient, mm Hg 73⫾18 71⫾23 74⫾14 0.6 Mean aortic valve gradient, mm Hg 42⫾12 41⫾14 42⫾10 0.9 Dimensionless index Aortic insufficiency (⬎2⫹) 0.23⫾0.06 0.21⫾0.05 0.24⫾0.06 4 (8%) 1 (5%) 3 (10%) 0.09 0.5 MDCT Maximum LVOT diameter, cm 2.73⫾0.4 2.84⫾0.3 2.66⫾0.4 0.08 Minimum LVOT diameter, cm 2.2⫾0.3 2.3⫾0.3 2.1⫾0.3 0.02 Eccentricity index 1.27⫾0.2 1.24⫾0.1 1.29⫾0.2 0.3 LVOT area, cm2 3.84⫾0.8 3.83⫾0.8 3.84⫾0.8 0.9 AVA, cm2 0.82⫾0.3 0.74⫾0.2 0.87⫾0.3 0.07 LV EF indicates left ventricular ejection fraction; LVOT, left ventricular outflow tract; VTI, velocity-time integral; AVA, aortic valve area; and MDCT, multidetector computed tomography. Discussion In the present study, we found that in patients with suspected severe AS, integration of 3D imaging data are associated with increased congruence between DI and AVA, leading to improved classification of stenosis severity. Specifically, TTE-AVA calculated using standard continuity equation with assumed circular LVOT geometry was significantly smaller than corrected AVA, based on MDCT-derived LVOT area. Corrected AVA showed good correlation with AVAp measured on MDCT. The differences in standard and corrected AVA appear secondary to consistently smaller LVOT dimensions mea- 570 Circ Cardiovasc Imaging September 2011 Difference Differenc ce in LVOT T area CT-TTE, cm m) (MDC 1 Mean Difference 0.5 Mean Diff. ± 2SD 0 -0.5 25 2.5 3 35 3.5 4 45 4.5 5 Figure 2. Bland-Altman analysis demonstrating the association between multidetector computed tomography (MDCT) left ventricular outflow tract (LVOT) area and transthoracic (TTE) LVOT area. -1 -1.5 -2 -2.5 3 -3 -3.5 Mean LVOT area (MDCT and TTE, cm) Downloaded from http://circimaging.ahajournals.org/ by guest on May 11, 2017 sured with TTE as compared with MDCT. TTE calculates LVOT based on a single measured diameter, whereas the LVOT was measured with CT by planimetry. The calculation from a single diameter is limited because of the known frequent eccentricity of the annulus and squaring of the Table 3. Correlation Between Aortic Valve Area Measurements Using Various Techniques and Transaortic Gradients and Dimensionless Index Linear Regression r Value P Value Mean transaortic gradient Total group TTE-AVA (continuity) ⫺0.28 0.05 AVAp ⫺0.39 0.004 Corrected AVA ⫺0.39 0.005 LV EF ⱖ50% TTE-AVA (continuity) ⫺0.37 0.05 AVAp ⫺0.43 0.02 Corrected AVA ⫺0.45 0.04 LV EF ⬍50% TTE-AVA (continuity) ⫺0.21 0.4 AVAp ⫺0.43 0.05 Corrected AVA ⫺0.37 0.05 Dimensionless index Total group TTE-AVA (continuity) 0.69 ⬍0.001 AVAp 0.77 ⬍0.001 Corrected AVA 0.73 ⬍0.001 LV EF ⱖ50% TTE-AVA (continuity) 0.77 ⬍0.001 AVAp 0.79 ⬍0.001 Corrected AVA 0.75 ⬍0.001 LV EF ⬍50% TTE-AVA (continuity) 0.54 0.01 AVAp 0.73 ⬍0.001 Corrected AVA 0.70 ⬍0.001 TTE indicates transthoracic echocardiography; AVA, aortic valve area; AVAp, AVA by computed tomography planimetry; and LV EF, left ventricular ejection fraction. diameter to derive the area augments even small errors. Our study sample was consistent with this observation as a vast majority of patient had an elliptical LVOT. Prior groups have also found that a high proportion of patients have an elliptical LVOT.4 – 8 Previous studies have also demonstrated that TTE underestimates AVA compared with MDCT, cardiac magnetic resonance, transesophageal echocardiography, Gorlin formula, and even surgical sizers.8,12,17–20 One study compared AVA from planimetry on MDCT to AVA calculated using traditional TTE and found good concordance between the 2 measurements with small underestimation of area by TTE.18 A previous report has also demonstrated good concordance between TTE-AVA and AVAp on MDCT, with a tendency for underestimation of AVA by TTE (similar to the current study).21 Another study also measured the coronal and sagittal diameter of the aortic annulus on MDCT and found that MDCT-derived diameters were significantly larger than diameters measured on echocardiography.12 On further analysis, it was also apparent that patients with low LV EF had a significantly higher LVOT diameter on TTE, probably reflecting changes concomitant with LV remodeling. These patients also had a lower LVOTVTI, as would be expected. As a result, there was a significant impact of LV EF on the association between TTE-AVA and transaortic gradient, with lower EF resulting in much poorer correlation. The correlation between corrected AVA and mean gradient improved significantly in particular in the low EF group. Similarly, EF had a significant impact on the association between TTE-AVA and DI, with low EF resulting in much poorer correlation. The most likely reason behind this is the improved accuracy of measurements using MDCT LVOT area. Importantly, we demonstrate that when using AVAp and corrected AVA, more patients had congruent criteria for severity of AS, especially low EF patients. This is potentially important because severity of AS is the ultimate deciding factor in timing of intervention. Based on the results of this study, it appears that in patients with discrepant calculated valve areas, transaortic gradients, and DI, an accurate 3D assessment of LVOT area would be crucial to classifying severity of AS. Further, severity of AS may be reclassified in a number of patients and potentially alter management. Hence, multimodality imaging could play complementary (as O’Brien et al Aortic Stenosis, MDCT, and Echocardiography 571 Downloaded from http://circimaging.ahajournals.org/ by guest on May 11, 2017 Figure 3. Correlation between dimensionless index and aortic valve area measured by transthoracic echocardiography (TTE) (A), multidetector computed tomography (MDCT) (B), and corrected multimodality imaging technique (C). opposed to competing) roles in assessment of AS. Of course, with rapid evolution of 3D echocardiography (especially TEE), LVOT assessment can also potentially be performed using that technique.4,17 However, it must be kept in mind that in the current study, we included only patients with severe AS, and, as such, the increased elliptical nature of the LVOT might not be applicable to patients with mild-moderate AS. Similar to our study, others have attempted to measure a cross section of the LVOT or planimetered LVOT area on MDCT and compare it with other imaging modalities as well as incorporate this measurement into assessments of AVA. In one study, it was demonstrated that the ellipse-derived LVOT diameter measurement, when incorporated into the continuity equation, correlated more closely with planimetered LVOT area compared with the traditional circle-derived LVOT area.8 However, only 11 patients in this study had both MDCT and TTE for comparison, and none of the patients had significant AS. Another study compared MDCT planimetered LVOT area to 2D TEE circular-derived LVOT area, 3D TEE circular-derived LVOT area, and 3D TEE planimetered LVOT area in patients with severe AS.4 All TEE methods significantly underestimated LVOT area compared with MDCT. Recalculating AVA using 3D TEE circular, 3D TEE planimetered, and MDCT planimetered LVOT areas, a respective 10%, 25%, and 25% of patients were reclassified as moderate stenosis highlighting the importance of accurate LVOT measurements. However, the sample was different from the current study such that the EF was substantially higher, all patients in that study underwent TAVI (despite ⬇25% being reclassified as moderate AS in retrospect), and a substantially smaller number had a history of prior open heart surgery. Finally, another group also substituted CT planimetered LVOT area into the continuity equation and their corrected AVA was not only systematically larger compared with AVA derived from standard continuity equation but also improved correlation between various severity measurements.22 However, this study sample was much younger (average age, 58 years) and included only 10 patients with moderate to severe AS. Our study predominantly included patients with severe AS (that had a need for invasive therapies). In addition, we included a sizable proportion of patients with abnormal EF (where multimodality imaging evaluation is likely to have the most significant impact). Recently, MDCT has evolved as an important modality for aortic valve assessment and its therapeutic planning; perhaps out of necessity. With an increasing number of redo cardiac surgical procedures, MDCT has become an invaluable tool for preoperative planning. Indeed, in our study sample, a substantial proportion of patients had a history of prior cardiac surgeries and were being considered for redo procedures, in which MDCT has been demonstrated to have incremental diagnostic utility and is considered an appropriate indication.23–25 Furthermore, TAVI is rapidly emerging as a viable therapeutic option in patients with severe AS.2 However, due to lack of direct visualization during TAVI, the operator is more reliant on preprocedural and intraprocedural imaging both for appropriate patient selection and to guide the procedure. One of the major advantages of a traditional open surgical approach is that direct visualization of the valvular apparatus is feasible, enabling appropriate valve prosthesis selection. Hence, MDCT has become routine in assessment of such patients to evaluate for aortic valve/aortic calcification, assessment of aortic root morphology, and evaluation of the anatomic relationship between coronary artery takeoff and aortic annulus.4 –7,9 –13 On the basis of the results of this study, we can potentially use information about LVOT area obtained on MDCT for the above indications at no additional cost of radiation or nephrotoxicity in this sample. However, it must be recognized that most outcomes data in AS are based on echocardiographic measures, and multimodality evaluation of severity of AS needs validation for its potential incremental value. 572 Circ Cardiovasc Imaging September 2011 Downloaded from http://circimaging.ahajournals.org/ by guest on May 11, 2017 The current study has following limitations. This is an observational study with a relatively small sample size. Hence, there is low power to detect differences between groups of patients. Also, there is a possibility of severely inflated type I error because of multiple testing without adjusting the significance level. MDCT is limited by the need for iodine-based contrast administration, which brings in the added burden potential nephrotoxicity, especially in an older sample (typical of severe, nonbicuspid AS). Although MDCT is also associated with significant radiation exposure, the risks of long-term deleterious effects of radiation are of lesser concern in an elderly population of AS patients. Still, for the MDCT community, it is important to continue to work on minimizing radiation exposure. With availability of newer scanners and newer imaging techniques, the concept of aggressive radiation reduction is rapidly evolving. Another limitation is that of establishing the gold standard for assessment of AVA: planimetry by standard TTE, TEE, and 3D TEE MDCT, or the Gorlin formula. Unfortunately, not all patients in the study sample had a transesophageal echocardiogram performed in the current study sample; with no one having 3D TEE images. As a result, that data are not presented for the study sample. It is possible that the LVOT assessment can potentially be performed using that technique. Indeed, previous studies have attempted to incorporate that in assessment of AS. However, transesophageal echocardiography is invasive, necessitating sedation in this already frail sample. As demonstrated in the current study, information on LVOT area on MDCT is available without any additional ramifications to the patient. Also, AVA estimated by the Gorlin formula was not uniformly available in the study sample, probably reflecting the current practice of increased reliance on noninvasive measures. Conclusions We demonstrate that in the vast majority of older patients with severe AS, AVA is typically underestimated using standard surface echocardiography measurements alone. Incorporating the LVOT area, which is frequently elliptical when measured using a 3D technique such as MDCT, into the continuity equation reduces the discrepant classification of severity of AS, especially in patients with lower EF. Improved congruence in AVA measurements could help selection of appropriate patients for both conventional surgical treatment and TAVI. In addition, it could also help in further refinements in shape and size of future percutaneous aortic valves. Disclosures None. References 1. Carabello BA, Paulus WJ. Aortic stenosis. Lancet. 2009;373:956 –966. 2. Leon MB, Smith CR, Mack M, Miller DC, Moses JW, Svensson LG, Tuzcu EM, Webb JG, Fontana GP, Makkar RR, Brown DL, Block PC, Guyton RA, Pichard AD, Bavaria JE, Herrmann HC, Douglas PS, Petersen JL, Akin JJ, Anderson WN, Wang D, Pocock S. Transcatheter aortic-valve implantation for aortic stenosis in patients who cannot undergo surgery. N Engl J Med. 2010;363:1597–1607. 3. Baumgartner H, Hung J, Bermejo J, Chambers JB, Evangelista A, Griffin BP, Iung B, Otto CM, Pellikka PA, Quinones M. Echocardiographic 4. 5. 6. 7. 8. 9. 10. 11. 12. 13. 14. 15. 16. 17. 18. 19. assessment of valve stenosis: EAE/ASE recommendations for clinical practice. J Am Soc Echocardiogr. 2009;22:1–23. Ng AC, Delgado V, van der Kley F, Shanks M, van de Veire NR, Bertini M, Nucifora G, van Bommel RJ, Tops LF, de Weger A, Tavilla G, de Roos A, Kroft LJ, Leung DY, Schuijf J, Schalij MJ, Bax JJ. Comparison of aortic root dimensions and geometries before and after transcatheter aortic valve implantation by 2- and 3D transesophageal echocardiography and multislice computed tomography. Circ Cardiovasc Imaging. 2009;3: 94 –102. Tops LF, Wood DA, Delgado V, Schuijf JD, Mayo JR, Pasupati S, Lamers FP, van der Wall EE, Schalij MJ, Webb JG, Bax JJ. Noninvasive evaluation of the aortic root with multislice computed tomography implications for transcatheter aortic valve replacement. J Am Coll Cardiol Cardiovasc Imaging. 2008;1:321–330. Akhtar M, Tuzcu EM, Kapadia SR, Svensson LG, Greenberg RK, Roselli EE, Halliburton S, Kurra V, Schoenhagen P, Sola S. Aortic root morphology in patients undergoing percutaneous aortic valve replacement: evidence of aortic root remodeling. J Thorac Cardiovasc Surg. 2009;137: 950 –956. Doddamani S, Grushko MJ, Makaryus AN, Jain VR, Bello R, Friedman MA, Ostfeld RJ, Malhotra D, Boxt LM, Haramati L, Spevack DM. Demonstration of left ventricular outflow tract eccentricity by 64-slice multi-detector CT. Int J Cardiovasc Imaging. 2009;25:175–181. Doddamani S, Bello R, Friedman MA, Banerjee A, Bowers JH Jr, Kim B, Vennalaganti PR, Ostfeld RJ, Gordon GM, Malhotra D, Spevack DM. Demonstration of left ventricular outflow tract eccentricity by real time 3D echocardiography: implications for the determination of aortic valve area. Echocardiography. 2007;24:860 – 866. Kurra V, Kapadia SR, Tuzcu EM, Halliburton SS, Svensson L, Roselli EE, Schoenhagen P. Pre-procedural imaging of aortic root orientation and dimensions: comparison between X-ray angiographic planar imaging and 3D multidetector row computed tomography. J Am Coll Cardiol Cardiovasc Interv. 2010;3:105–113. Schoenhagen P, Numburi U, Halliburton SS, Aulbach P, von Roden M, Desai MY, Rodriguez LL, Kapadia SR, Tuzcu EM, Lytle BW. Threedimensional imaging in the context of minimally invasive and transcatheter cardiovascular interventions using multi-detector computed tomography: from pre-operative planning to intra-operative guidance. Eur Heart J. 2010;31:2727–2740. Schoenhagen P, Tuzcu EM, Kapadia SR, Desai MY, Svensson LG. Three-dimensional imaging of the aortic valve and aortic root with computed tomography: new standards in an era of transcatheter valve repair/implantation. Eur Heart J. 2009;30:2079 –2086. Delgado V, Ng AC, van de Veire NR, van der Kley F, Schuijf JD, Tops LF, de Weger A, Tavilla G, de Roos A, Kroft LJ, Schalij MJ, Bax JJ. Transcatheter aortic valve implantation: role of multi-detector row computed tomography to evaluate prosthesis positioning and deployment in relation to valve function. Eur Heart J. 2010;31:1114 –1123. Tops LF, Delgado V, van der Kley F, Bax JJ. Percutaneous aortic valve therapy: clinical experience and the role of multi-modality imaging. Heart. 2009;95:1538 –1546. Nashef SA, Roques F, Michel P, Gauducheau E, Lemeshow S, Salamon R. European system for cardiac operative risk evaluation (EuroSCORE). Eur J Cardiothorac Surg. 1999;16:9 –13. Lang RM, Bierig M, Devereux RB, Flachskampf FA, Foster E, Pellikka PA, Picard MH, Roman MJ, Seward J, Shanewise JS, Solomon SD, Spencer KT, Sutton MS, Stewart WJ. Recommendations for chamber quantification: a report from the American Society of Echocardiography’s Guidelines and Standards Committee and the Chamber Quantification Writing Group, developed in conjunction with the European Association of Echocardiography, a branch of the European Society of Cardiology. J Am Soc Echocardiogr. 2005;18:1440 –1463. Bland JM, Altman DG. Statistical methods for assessing agreement between two methods of clinical measurement. Lancet. 1986;1:307–310. Poh KK, Levine RA, Solis J, Shen L, Flaherty M, Kang YJ, Guerrero JL, Hung J. Assessing aortic valve area in aortic stenosis by continuity equation: a novel approach using real-time three-dimensional echocardiography. Eur Heart J. 2008;29:2526 –2535. Feuchtner GM, Dichtl W, Friedrich GJ, Frick M, Alber H, Schachner T, Bonatti J, Mallouhi A, Frede T, Pachinger O, zur Nedden D, Muller S. Multislice computed tomography for detection of patients with aortic valve stenosis and quantification of severity. J Am Coll Cardiol. 2006; 47:1410 –1417. Babaliaros VC, Liff D, Chen EP, Rogers JH, Brown RA, Thourani VH, Guyton RA, Lerakis S, Stillman AE, Raggi P, Cheesborough JE, Veledar O’Brien et al 20. 21. 22. 23. E, Green JT, Block PC. Can balloon aortic valvuloplasty help determine appropriate transcatheter aortic valve size? J Am Coll Cardiol Cardiovasc Interv. 2008;1:580 –586. Okura H, Yoshida K, Hozumi T, Akasaka T, Yoshikawa J. Planimetry and transthoracic two-dimensional echocardiography in noninvasive assessment of aortic valve area in patients with valvular aortic stenosis. J Am Coll Cardiol. 1997;30:753–759. Ropers D, Ropers U, Marwan M, Schepis T, Pflederer T, Wechsel M, Klinghammer L, Flachskampf FA, Daniel WG, Achenbach S. Comparison of dual-source computed tomography for the quantification of the aortic valve area in patients with aortic stenosis versus transthoracic echocardiography and invasive hemodynamic assessment. Am J Cardiol. 2009;104:1561–1567. Halpern EJ, Mallya R, Sewell M, Shulman M, Zwas DR. Differences in aortic valve area measured with CT planimetry and echocardiography (continuity equation) are related to divergent estimates of left ventricular outflow tract area. AJR Am J Roentgenol. 2009;192:1668 –1673. Kamdar AR, Meadows TA, Roselli EE, Gorodeski EZ, Curtin RJ, Sabik JF, Schoenhagen P, White RD, Lytle BW, Flamm SD, Desai MY. Multidetector computed tomographic angiography in planning of reoperative cardiothoracic surgery. Ann Thorac Surg. 2008;85:1239 –1245. Aortic Stenosis, MDCT, and Echocardiography 573 24. Maluenda G, Goldstein MA, Lemesle G, Weissman G, Weigold G, Landsman MJ, Hill PC, Pita F, Corso PJ, Boyce SW, Pichard AD, Waksman R, Taylor AJ. Perioperative outcomes in reoperative cardiac surgery guided by cardiac multidetector computed tomographic angiography. Am Heart J. 2010;159:301–306. 25. Taylor AJ, Cerqueira M, Hodgson JM, Mark D, Min J, O’Gara P, Rubin GD, Kramer CM, Berman D, Brown A, Chaudhry FA, Cury RC, Desai MY, Einstein AJ, Gomes AS, Harrington R, Hoffmann U, Khare R, Lesser J, McGann C, Rosenberg A, Schwartz R, Shelton M, Smetana GW, Smith SC Jr. ACCF/SCCT/ACR/AHA/ASE/ASNC/ NASCI/SCAI/SCMR 2010 Appropriate Use Criteria for Cardiac Computed Tomography: a Report of the American College of Cardiology Foundation Appropriate Use Criteria Task Force, the Society of Cardiovascular Computed Tomography, the American College of Radiology, the American Heart Association, the American Society of Echocardiography, the American Society of Nuclear Cardiology, the North American Society for Cardiovascular Imaging, the Society for Cardiovascular Angiography and Interventions, and the Society for Cardiovascular Magnetic Resonance. J Am Coll Cardiol. 2010;56:1864 –1894. Downloaded from http://circimaging.ahajournals.org/ by guest on May 11, 2017 CLINICAL PERSPECTIVE In aortic stenosis (AS), the precise assessment of its severity is essential for appropriate therapeutic decision-making. It relies on standard echocardiographic criteria, including transaortic gradients, dimensionless index, and aortic valve area, which is typically calculated by the continuity equation. Continuity equation utilizes left ventricular outflow tract (LVOT) diameter to calculate aortic valve area with the assumption that LVOT is circular. However, LVOT is very often elliptical in shape, potentially creating a discrepancy between the actual and calculated aortic valve area. The discrepancy is more noted in patients with reduced ejection fraction. The use of multidetector computed tomography enables us to 3-dimensionally measure LVOT area, which could be incorporated into the continuity equation. The current study of patients with severe AS demonstrates that integration of 3D LVOT area significantly increases the congruence between various AS severity criteria (including corrected aortic valve area, transaortic gradients, and dimensionless index), leading to improved classification of AS severity, especially in the setting of reduced ejection fraction. Improved congruence in aortic valve area measurements could help in selection of appropriate timing for surgical and percutaneous treatments. In addition, it could also help in further refinements in shape and size of future percutaneous aortic valves. Integration of 3D Imaging Data in the Assessment of Aortic Stenosis: Impact on Classification of Disease Severity Bridget O'Brien, Paul Schoenhagen, Samir R. Kapadia, Lars G. Svensson, Leonardo Rodriguez, Brian P. Griffin, E. Murat Tuzcu and Milind Y. Desai Downloaded from http://circimaging.ahajournals.org/ by guest on May 11, 2017 Circ Cardiovasc Imaging. 2011;4:566-573; originally published online July 7, 2011; doi: 10.1161/CIRCIMAGING.111.964916 Circulation: Cardiovascular Imaging is published by the American Heart Association, 7272 Greenville Avenue, Dallas, TX 75231 Copyright © 2011 American Heart Association, Inc. All rights reserved. Print ISSN: 1941-9651. Online ISSN: 1942-0080 The online version of this article, along with updated information and services, is located on the World Wide Web at: http://circimaging.ahajournals.org/content/4/5/566 Permissions: Requests for permissions to reproduce figures, tables, or portions of articles originally published in Circulation: Cardiovascular Imaging can be obtained via RightsLink, a service of the Copyright Clearance Center, not the Editorial Office. Once the online version of the published article for which permission is being requested is located, click Request Permissions in the middle column of the Web page under Services. Further information about this process is available in the Permissions and Rights Question and Answer document. Reprints: Information about reprints can be found online at: http://www.lww.com/reprints Subscriptions: Information about subscribing to Circulation: Cardiovascular Imaging is online at: http://circimaging.ahajournals.org//subscriptions/