* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Early morphogenesis of persistent hyperplastic tunica
Survey
Document related concepts
Transcript
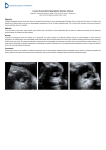
Investigative Ophthalmology & Visual Science, Vol. 29, No. 7, July 1988 Copyright © Association for Research in Vision and Ophthalmology Early Morphogenesis of Persistent Hyperplostic Tunica Vasculosa Lentis and Primary Vitreous The Dog os on Onrogeneric Model Michael H. Boeve,* Tineke von der Linde-Sipmaaf and Frans C. Srodes* Observations on (postnatal) persistent hyperplastic tunica vasculosa lentis/persistent hyperplastic primary vitreous (PHTVL/PHPV) in man and dog have been published previously. Up to the present, no evidence on the etiology of this entity was available. The hereditary occurrence of the disease in the Dobermann pinscher dog and the similarity of ocular development in mammals has provided a useful model in providing ontogenetic data. The present study deals with the early morphogenesis of PHTVL/PHPV, from day 25 to 44 post-coitum (D25-D44), in genetically affected dog fetuses. Normal beagle dog fetuses served as reference material, which has been described separately. At D30, the hyaloid system, including the tunica vasculosa lentis posterior, had developed further than in the reference fetuses. From that stage onward, a retrolental fibrovascular membrane developed. In some of the eyes of D37, posterior polar subcapsular cataracts and preretinal glial proliferations were observed. Capsular anomalies and distortions of the lens shape as seen in clinical PHTVL/PHPV were not observed, and are believed to be secondary entities. Extrapolation of some of the obtained data from dog to man is possible by the use of comparable gestational time scales. The anterior form of (PHTVL/PHPV) in man probably develops its main features in the period of approximately 43 to 66 days of pregnancy. Recently, anti-angiogenetic properties of normal vitreous have been described. This, and the fact that overdevelopment and subsequent incomplete regression of the hyaloid system plays a major role in the pathogenesis of PHTVL/PHPV, gives rise to the hypothesis that a changed amount or effectiveness of such (humoral) factors is an important factor in the etiology of this disease. Invest Ophthalmol Vis Sci 29:1076-1086,1988 The anterior form of persistent hyperplastic tunica vasculosa lentis/persistent hyperplastic primary vitreous (PHTVL/PHPV) is a congenital eye anomaly, in most cases leading to cataract. The occurrence of this entity has been described in man and in dogs. In man, over 200 cases, mainly unilateral and supposedly nonhereditary, have been described under different names.1 The entity can be distinguished into an anterior and a posterior form.2"4 The first description of PHPV in a dog was published by Grimes and Mullaney in 1969,5 and confirmed by other case reports as summarized by Stades.6 Only in recent years has the frequent occur- rence of PHTVL/PHPV been described in specific dog breeds, at first in the Dobermann pinscher6 and lately also in the Staffordshire bull terrier.7-8 Clinical,6 surgical,9 pathological10 and genetic" aspects of the disorder have been described for the Dobermann pinscher; in this breed a hereditary basis of the disease was demonstrated.'' The close resemblance of the clinical manifestations in man and dog, as well as the frequent (inherited) occurrence of PHTVL/PHPV in the Dobermann pinscher breed provide a useful model for research on the ontogenesis. In addition, the high degree of similarity in development of the eye in different mammals12"15 allows extrapolation of some of the results of this study to PHTVL/PHPV of man. The embryonic and neonatal development of the normal canine eye13 and the early morphogenesis of the lens, lens capsule, hyaloid system and vitreous in particular have been described.16 On the ontogenesis of PHTVL/PHPV only one preliminary communication17 has been published. The present study was undertaken to establish when and how the morphogen- From the *Small Animal Clinic and the fDepartment of Pathology, Faculty of Veterinary Medicine, University of Utrecht, Utrecht, The Netherlands. Submitted for publication: November 17, 1987; accepted January 18, 1988. Reprint requests: Michael H. Boeve, DVM, Small Animal Clinic, University of Utrecht, Yalelaan 8, 3584 CM Utrecht, The Netherlands. 1076 Downloaded From: http://iovs.arvojournals.org/ on 05/10/2017 No. 7 1077 EARLY MORPHOGENESIS OF PHTVL/PHPV / Doeve er ol. esis of the eye in genetically PHTVL/PHPV-affected dog fetuses becomes aberrant. Materials and Methods Table 1. The average diameters (AD) of the eyes (n) of genetically PHTVL/PHPV-affected Dobermann pinscher fetuses, from D25 to D44 (values are given in millimeters) Fetuses From matings of severely (grade 2-6) PHTVL/ PHPV-affected Dobermann pinschers, 41 fetuses were collected at ages of 25, 28, 30, 33, 35, 37 and 44 days post-coitum (D25-44). The amounts per age are stated in Table 1. Sixty-eight of the obtained eyes were available for this study. The fetuses were collected as previously described.16 Seventeen fetuses D25 D28 D30 D33 D35 D37 D44 (n) AD Min Max (14) 0.284 0.618 0.747 1.43 2.20 2.56 0.275 0.598 0.675 1.35 2.08 2.37 3.5 0.294 0.631 0.830 1.49 2.46 2.73 (4) (10) (10) (4) (14) (12) 3.7 3.9 Fig. 1. D25; optic cups. Transverse sections; overall views. H & E; X25. (LV = lens vesicle; HA = hyaloid artery; R = retina; SE = surface ectoderm). (A) The lens vesicle is still open. A clump of cells from the surface ectoderm (epitrichia) is present (arrow). (B) The lens vesicle is closed, but still attached to the surface ectoderm. Some loose epitrichial cells are present (arrows), (C) The lens vesicle is closed and detached from the surface ectoderm. The annular vessel (A V) at the anterior edge of the optic cup is present. e Downloaded From: http://iovs.arvojournals.org/ on 05/10/2017 1078 INVESTIGATIVE OPHTHALMOLOGY & VISUAL SCIENCE / July 1988 Vol. 29 «•*• Fig. 2. D30; equatorial region of the lens. Capillaries (arrows), connect the anterior and posterior portion of the tunica vasculosa lentis. (R = retina; PLF = primary lens fibers). PAS; X40. 25 2 I from normal beagle parents, with ages up to D35, served as reference material. The results of that study have been published separately.16 In order to minimize the variation of gestational ages, matings were carried out as soon as possible after ovulation, as determined by plasma progesterone measurements.16 Animal care and treatment in this study were in compliance with the ARVO Resolution on the Use of Animals in Research. (Fig. 1 a-c). In eight eyes the process of invagination, by which the lens vesicle is formed, had not yet been completed and the anterior central part of the lens vesicle was still open (Fig. la). In these eyes, a clump of epitrichial cells was present at this location. In four eyes the lens vesicle had closed (Fig. lc); in two of these it was still attached to the surface ectoderm (Fig. lb). In most sections, the cavity of the closed lens Histology Following collection and death of the fetuses, the heads or the eyes alone were fixed in 4% buffered formaldehyde, processed and stained as described before.16 Because of damage to some of the D28 material, a few 1 jtm sections of specimens fixed and embedded for electron microscopy were stained with the periodic acid-Schiff (PAS) reaction. The development of all eyes was examined by light microscopy. The average diameters of the fetal eyes were measured according to a previously described method.16 Results Optic Cup Throughout this study, the eyes at all ages were round to oval, double-layered structures. The average diameter values of the eyes of D25 up to D44 showed a steady increase from 0.284 to 3.7 mm (Table 1). Lens At D25, the lens vesicles consisted of epithelial cells, and had a rounded to somewhat conical shape Downloaded From: http://iovs.arvojournals.org/ on 05/10/2017 Fig. 3. D33; transverse section; overall view. A fibrovascular membrane (arrows) is present retrolentally. The peripheral detachment appears artificial (see also Fig. 8). Sections of hyaloid vasculature are not present within the vitreous (V). (L = lens; R = retina; N = optic nerve). H & E; X4. No. 7 EARLY MORPHOGENESIS OF PHTVL/PHPV / Doeve er ol. 1079 vesicles contained some amorphous and cellular (epitrichial) material. At D28, the primary lensfibers,formed by elongation of the posterior cells of the lens vesicle, had filled the posterior half of the lens vesicle. At D30, the lens vesicles were almost obliterated by the primary lensfibers,thus leaving a flat cavity anteriorly (Fig. 2). From this developmental stage onwards the lens sphere was oval. At D33 (Fig. 3) the flat cavity as at D30 was barely detectable in most specimens. At D35 (Fig. 4) the lens spheres were obliterated. At D37 posterior polar subcapsular cataracts were observed in two of the eyes (Fig. 5). At D44, a small posterior polar subcapsular cataract was observed in one lens. Lens Capsule At D25, the anlage of the lens capsule was observed as a very thin basement membrane-like layer of faintly PAS-positive material, surrounding the lens vesicle. The histologic appearance of this layer was similar to that of thefibrillarcontents of the primitive vitreous. At D28, the lens capsule was observed as a faintly stained, straight and continuous structure (Fig. 6). At D30, the posterior part of the capsule, as well as the equatorial region, where the vasculature of the tunica vasculosa lentis (TVL) was very well developed, PAS-positive and lying in close proximity to the capsule, was thicker than the anterior part. From D33 onward, except in some eyes at D37 and D44, the capsule had a wrinkled appearance. Fig. 5. D37; posterior part of the lens (L), the lens capsule (LC) and anterior part of the plaque (P). A posterior polar subcapsular cataract is present (arrows). (H = main ramification of hyaloid artery; Tp = capillary of tunica vasculosa lentis). PAS; X40. Downloaded From: http://iovs.arvojournals.org/ on 05/10/2017 0.5 mm Fig. 4. D35; transverse section; overall view. The posterior lens capsule is completely covered by afibrovascularplaque (arrows). (L = lens; V = vitreous; R = retina). PAS; X2.5. Vascular System At D25 (Fig. la-c), a short and straight hyaloid artery was present in all eyes. No indication of a ramification of the hyaloid artery into vasa hyaloidea propria or the future tunica vasculosa lentis posterior was observed. The annular vessel at the distal edge of the optic cup was present. In the D28 material, numerous cross-sections of vessels of the hyaloid-TVL system were observed. 1080 INVESTIGATIVE OPHTHALMOLOGY & VISUAL SCIENCE / July 1988 Vol. 29 Fig. 6. D28; posterior part of the lens (L), the lens capsule (LC) and capillary of the tunica vasculosa lentis posterior (Tp). Cell (c) might be a pericyte or a primitive fibroblast, indicating a first onset of the retrolental membrane. Hy = hyalocyte. PAS; XI00. i Hy TVL vasculature was present, positioned directly against the lens capsule (Fig. 6). At D30 (Fig. 7), sections through vessels of the hyaloid-TVL system were more numerous than in the reference material.15 Predominantly in the central region, a proliferated layer of TVL vasculature was located against the posterior lens capsule, covering that region almost completely. The vascularization of the anterior side of the lens was similar to the normal controls. This vasculature was connected with the TVL posterior by capillaries in the equatorial region of the lens. At D33 a distinct but thin retrolental fibrovascular layer, which characterizes PHTVL/PHPV postnatally, was present in all eyes (Figs. 3, 8). In these plaques, cross-sections of the TVL vasculature were present. At this stage, the central part of the plaque was locally attached to the posterior lens capsule (Fig. 3). At the periphery, the plaque was detached from the capsule. Still, capillaries and cellular components, including fibroblasts, were in contact with the capsule (Fig. 8). Cross-sections through the vasa hyaloidea propria in the vitreous space were less numerous than at D30 (Figs. 3, 7). Fig. 7. D30; transverse section of the vitreous. The hyaloid-TVL system is very well developed. (L = lens; Hp = vasa hyaloidea propria; Tp = tunica vasculosa posterior; R = retina). H & E; X25. Downloaded From: http://iovs.arvojournals.org/ on 05/10/2017 No. 7 EARLY MORPHOGENESIS OF PHTVL/PHPV / Doeve er d : 1081 Fig. 8. D33; peripheral part of the posterior lens capsule (LC) and retrolental fibrovascular membrane (P), which has (most probably as an artefact) been detached. (L = lens). See also Figure 3. PAS; X40. 8 From D35 (Fig. 4) onward, a plaque, completely attached to the posterior lens capsule, was observed in all eyes. The central thickness of the plaques ranged from 29.0 to 45.1 (mean 37.9) ^m. Except for the main trunk of the hyaloid artery, no vasa hyaloidea propria were present in the vitreous space. At D37, the central thickness of the plaques was 45.1 to 119.1 (mean 73.4) fim. Many cross-sections of TVL and hyaloid vasculature were present within the plaques (Figs. 5, 9). Except for a straight main trunk of the hyaloid artery, no parts of the hyaloid system were found in the vitreous space (Fig. 10). Glial tissue was observed for the first time in the plaques, but no melanocytes were observed. At D44 (Fig. 11), the Fig. 9. D37; magnification of the retrolental plaque (P). Fibrovascular tissue, with an embedded capillary of the hyaloidTVL system (Hs). (L = lens; LC = lens capsule; V = vitreous). PAS; X40. Downloaded From: http://iovs.arvojournals.org/ on 05/10/2017 appearance of the anomalies was similar to that at D37 (Figs. 5, 9, 10). The central thickness of the plaques varied from 22.5 to 157.8 ^.m (mean: 95.4; median value: 106.3 pm). In 11 plaques varying numbers of melanocytes were present. The thinnest plaque did not contain any melanin-containing cells. Vitreous At D25 (Fig. la-c), the primitive vitreous contained some amorphous and fibrillar material but very few cellular components. At D28, apart from the vascular elements as described above, the vitreous space contained cells with 1082 Vol. 29 INVESTIGATIVE OPHTHALMOLOGY b VISUAL SCIENCE / July 1988 \ 10 "empty" image, ie, a few loose cells within a randomly oriented, seemingly fibrillar matrix. At D37, a proliferation of neuroglial tissue, intimately attached to and originating from the retina, was present in four eyes (Fig. 12a, b). These proliferations, followed by serial sections, protruded into the vitreous and reached the retrolental plaque in three of these eyes. The thickness of these strands varied substantially; the average size was about 50 jum. In these three eyes, as well as in six others, additional, very thin strands of neuroglia were present (Fig. 13a, b). These originated from the retrolental plaque, extended into the vitreous and connected with a larger, retina-derived proliferation (Fig. 12a, b), if such was present. At D44 (Fig. 11) the vitreous showed a concentration of cells (fibroblasts, hyalocytes) in the proximity of the plaque. Retina and Pigment Epithelium Fig. 10. D37; transverse section. A retrolental, fibrovascular plaque is present (arrows). The vitreous does not contain sections of hyaloid vasculature). (L = lens; V = vitreous; R = retina; c = cornea; Li = eyelid). H & E; X2.5. the cytological characteristics of fibroblasts and hyalocytes (Fig. 6) amidst an amorphous and slightly fibrillar ground substance. At D30 (Fig. 7), both the vascular and cellular components of the primitive vitreous of the affected fetuses had developed further than those described in the corresponding reference material.16 From D33 onward (Figs. 3, 4, 10, 11) the absence of vasa hyaloidea propria gave the vitreous space an Up to D35 the development of the neural retina and the pigment epithelium did not differ from that described in the reference material.16 Apart from the aforementioned glial tissue, a conical proliferation of glial tissue was present at the anlage of the optic disc in five eyes of D37. In eight of the D44 eyes, the primitive optic disc contained a similarly shaped mass of glial tissue (Fig. 14). Discussion This study has demonstrated a first, marked difference in embryonic development of PHTVL/PHPV- Fig. 11. D44; transverse section of the plaque (P). The cellular components of the vitreous are concentrated in the proximity of the plaque. (L = lens; LC = lens capsule; V = vitreous). PAS; X20. 11 Downloaded From: http://iovs.arvojournals.org/ on 05/10/2017 50 p No, 7 EARLY MORPHOGENESIS OF PHTVL/PHPV / Doeve er ol. 1083 0.1mm Fig. 12. D37; section of the peripheral retina (R) and vitreous (V). (A) and (B) are sections from the same eye. (A) Proliferation of glial tissue (G), deriving from the retina into the vitreous. (B) Section, parallel to A, showing the glial tissue (G) continuing as a strand. (L = lens). Both H & E; X10. affected and normal canine eyes at D30. From this stage onward the (mesodermal) hyaloid-TVL vasculature is the main structure involved in the development of the anomaly. From D37 neuroglia, an ectodermal component, has also been found to participate. Optic Cup In the dog, microphthalmia is a less common feature of PHTVL/PHPV than in man. The measurements of the optic cup's average diameter values (Table 1) did not differ significantly from those of the reference material.16 For a statistical evaluation of these values, larger numbers would be required. Lens As the eyes of D25 were from fetuses from the same litter, the differences in closure and separation of the lens vesicles must be due to slight differences of developmental stage. Up to D35, the development of the lens was analogous to that described in the reference material.16 At D37 and D44, some posterior polar subcapsular cataracts were observed in the present material. The localization of these cataracts corresponds with the site of their onset in PHTVL/PHPV-affected patients.1'6-10 Abnormal lens shapes, such as lenticonus, microphakia or colobomas were not observed. Downloaded From: http://iovs.arvojournals.org/ on 05/10/2017 Lens Capsule The morphological features of the posterior lens capsule were normal, although frequently wrinkled due to shrinkage, which was also the case in the reference material.16 Recently there has been some discussion as to whether the changes in the posterior lens capsule—as seen in postnatal PHTVL/PHPV10— should be regarded as primary or secondary.18 Up to this moment, changes in the posterior lens capsule, varying from dissolution to capsular tears, have only been seen in severely affected patients.110 This suggests that the development of the frequently found lenticonus posterior10 either is a secondary event, or these matings failed to produce the most severe cases that were clinically found in man and dog.1'610 Vascular System Until D30, the development of the vascular structures of the optic cup matched that described in the reference material.16 From D30 onward the retrolental part of that vasculature, the hyaloid system (predominantly the vasa hyloidea propna and the TVL posterior), showed signs of an increased development and subsequent incomplete regression. The peripheral detachment of the plaque at D33 appears to be an artifact due to the histologic processing (Fig. 8). Vitreous has been reported to inhibit angiogen- 1084 INVESTIGATIVE OPHTHALMOLOGY b VI5UAL SCIENCE / July 1988 Fig. 13. D37; transverse, serial sections of the retrolental plaque (P) from the same eye. (A) A thin strand of glia derives from the plaque (arrow). (B) Section, parallel to (A), showing the continuation of the same glial strand (arrow) into the vitreous. (V = vitreous). Both H & E; X40. 13a 13b esis.19'20 Impaired or defective anti-angiogenetical properties of the (secondary) vitreous might be the cause of the described overdevelopment of intravitreal vasculature in PHTVL/PHPV. Vitreous From D33 the vitreous space showed cross-sections through the main stem of the hyaloid artery only. Its ramifications had become enbodied in the retrolental plaque. This situation gave the vitreous space its "empty" appearance, compared to the reference material of this age group. Thefibrillarappearance of the ground substance is probably due to coagulative artifacts due to fixation technique, as has been described previously.1216 The fact that the D28 material does not show this coarsefibered structure supports this assumption, because it had been (differently) prepared for electron microscopic purposes. Downloaded From: http://iovs.arvojournals.org/ on 05/10/2017 Vol. 29 25 JJ Glial Tissue Proliferations Reference eyes did not contain glial proliferations as were observed in the present material. In his pathologic studies concerning human eyes with (PHTVL/)PHPV, Manschot2 made special reference to preretinal glial proliferation as a pathologic characteristic of the entity. He described both larger and smaller, fibered and cellular preretinal proliferations in infant eyes with (PHTVL/)PHPV. The fibers of many of these cells were observed to merge into the fibers of Mueller cells of the retina. Consequently, the probable neuroglial origin of these structures was postulated. In the eyes described here, preretinal glial proliferations (Fig. 13a, b), mimicking those described by Manschot in man,2 were observed in nine eyes at D37 and D44. The finding of glial tissue in the plaques of these dog fetuses and in the plaques of (PHTVL/ PHPV-affected) postnatal dogs10 and in man2 sug- No. 7 EARLY MORPHOGENESIS OF PHTVL/PHPV / Doeve er ol. 1085 gests that this material derives from the glial proliferations described here. Apart from the glial proliferations described above, in some eyes there was a small, conical proliferation of glial cells in the center of the presumptive optic disc (Fig. 14). A cone-shaped mass of cells of this kind in postnatal eyes is known as "primitive epithelial papilla" or "Bergmeister's papilla," and is a frequent finding in PHTVL/PHPV in man and dog. Retina and Pigment Epithelium The general development of the sensory retina and pigment epithelium in affected eyes was similar to that in the reference fetuses, except for the cases in which a neuroglial proliferation was present. In the contemporary literature, the most current term for the described anomaly in man is "PHPV." However, other names have been used in the past, such as persistent hyperplastic tunica vasculosa lentis (PHTVL), pseudophakia fibrosa, membranous cataract leucocoria, pseudoglioma and cataracta congenita vasculosa.'' The differences in nomenclature suggest a lack of knowledge about the development of the anomalies. Stades6 used PHTVL primarily, and PHPV secondarily, as names for the disease, as the anomaly appeared to be first of all a persistence and hyperplasia of the TVL posterior. Depending on whether or not the hyaloid system is considered a part of the primitive vitreous and according to the classical embryologic views, the name PHPV would suggest that the retrolental tissue proliferations which are pathognomonic for the condition are solely or mainly of ectodermal origin. However, the results of this and other studies14"16'21 ai indicate a primarily mesodermal origin, although neuroectodermal involvement (the presence of neuroglia) can be demonstrated in some cases. Thus the present study supports the name PHTVL/PHPV, as proposed by Stades,6 although a shorter name would be preferable for clinical use. The results of this study give lead to the following hypothesis about the genesis of (PHTVL/)PHPV in man. The major visible embryological derangements in PHTVL/PHPV in the dog occur during the gestational period of D30 to D45. This developmental period extends from the obliteration of the lens vesicle until the first signs of regression of the hyaloid system. Extrapolating this to the human embryo and taking the difference in time of ocular development in pregnancy into account,16 it would appear that the anterior form of PHPV in man develops its main features in a gestational period of approximately 43 to 66 days of gravidity. Aguirre13 stated that extrapo- Downloaded From: http://iovs.arvojournals.org/ on 05/10/2017 r 14 0.1 mm Fig. 14. D44; section of the optic nerve region. A conically shaped clump of glial tissue (G) is located on the nerve head. (N = optic nerve; HA = hyaloid artery; R = retina; V = vitreous). PAS; X10. lation of ocular developmental events from man to dog could easily be erroneous, because in man the embryological development of the eye occurs relatively earlier in gestation than in dog. Therefore, the above-mentioned gestational period has been placed in comparable time scales for five mammal species, including man and dog.16 Thus, the risk of drawing erroneous conclusions is brought to an acceptable minimum. One of the most remarkable changes observed in the studied fetuses was the overdevelopment of the hyaloid system and TVL. An increased growth promotion or decreased inhibition of intravitreal angiogenesis by humoral factor(s)19 20 is probable. For this reason further studies on the ontogenesis of PHTVL/ PHPV in the Dobermann pinscher dog will involve the regulation of intravitreal angiogenesis, as well as ultrastructural aspects of the entity. Key words: PHTVL/PHPV, eye, vitreous, morphogenesis, dog 1086 INVESTIGATIVE OPHTHALMOLOGY 6 VISUAL SCIENCE / July 1988 Acknowledgments The authors wish to thank the Professors J. A. Oosterhuis (Leiden) and W. A. Manschot (Rotterdam) for their helpful criticism. References 1. Reese AB: Persistent hyperplastic primary vitreous. Am J Ophthalmol 40:317, 1955. 2. Manschot WA: Persistent hyperplastic primary vitreous. AMA Arch Ophthalmol 59:188, 1958. 3. Pruett RC and Schepens CL: Posterior hyperplastic primary vitreous. Am J Ophthalmol 69:535, 1970. 4. Haddad R, Font RL, and Reeser F: Persistent hyperplastic primary vitreous: A clinicopathologic study of 62 cases and review of the literature. Surv Ophthalmol 23:123, 1978. 5. Grimes TD and Mullaney J: Persistent hyperplastic primary vitreous in a greyhound. Vet Rec 85:607, 1969. 6. Stades FC: Persistent hyperplastic tunica vasculosa lentis and persistent hyperplastic primary vitreous in 90 closely related Dobermann pinschers: Clinical aspects. Journal of the American Animal Hospital Association 16:739, 1980. 7. Curtis R, Barnett KC, and Leon A: Persistent hyperplastic primary vitreous in the Staffordshire bull terrier. Vet Rec 115:385, 1984. 8. Leon A, Curtis R, and Barnett KC: Hereditary persistent hyperplastic primary vitreous in the Staffordshire bull terrier. Journal of the American Animal Hospital Association 22:765, 1986. 9. Stades FC: Persistent hyperplastic tunica vasculosa lentis and persistent hyperplastic primary vitreous in Dobermann pinschers: Techniques and results of surgery. Journal of the American Animal Hospital Association 19:393, 1983. 10. Van der Linde-Sipman JS, Stades FC, and De Wolff-Rouendaal D: Persistent hyperplastic tunica vasculosa lentis and persistent hyperplastic primary vitreous in the Doberman pinscher: Pathologigal aspects. Journal of the American Animal Hospital Association 19:791. 1983. Downloaded From: http://iovs.arvojournals.org/ on 05/10/2017 Vol. 29 11. Stades FC: Persistent hyperplastic tunica vasculosa lentis and persistent hyperplastic primary vitreous in Dobermann pinschers: Genetic aspects. Journal of the American Animal Hospital Association 19:957, 1983. 12. Duke-Elder S: System of Opthalmology: Vol. 3, Normal and Abnormal Development. London, Henry Kimpton, 1963. 13. Aguirre GD, Rubin LF, and Bistner SI: Development of the canine eye. Am J Vet Res 33:2399, 1972. 14. Gloor BP: Zur Entwicklung des Glaskoerpers und der Zonula: I. Ueberblick und chronologischer Ablauf der Glaskoerperund Zonulaentwicklung beim Kaninchen. Graefes Arch Klin Exp Ophthalmol 186:299, 1973. 15. Gloor BP: Zur Entwicklung des Glaskoerpers und der Zonula: II. Glaskoerperzellen waehrend Entwicklung und Rueckbildung der Vasa hyaloidea und der Tunica vasculosa lentis. Graetes Arch KJin Exp Ophthalmol 186:311, 1973. 16. Boeve MH, Van der Linde-Sipman JS, and Stades FC: Early morphogenesis of the canine lens, lens capsule, hyaloid system and vitreous body. Anat Rec 220:435, 1988. 17. Boeve MH, Van der Linde-Sipman JS, and Stades FC: Morphogenesis of persistent hyperplastic tunica vasculosa lentis/ persistent hyperplastic primary vitreous (PHTVL/PHPV) in the dog. IRCS Med Sci 13:255, 1985. 18. Stades FC: Persistent hyperplastic tunica vasculosa lentis and persistent hyperplastic primary vitreous in the Dobermann pinscher. Thesis, Utrecht, 1983. 19. Brem S, Preis I, Langer R, Brem H, Folkman J, and Patz A: Inhibition of neovascularization by an extract derived from vitreous. Am J Ophthalmol 84:323, 1977. 20. Lutty GA, Mello RJ, Chandler C, Fait C, Bennett A, and Patz A: Regulation of cell growth by vitreous humour. J Cell Sci 76:53, 1985. 21. Gloor BP: Zur Entwicklung des Glaskoerpers und der Zonula: III. Herkunft, Lebenszeit und Ersatz der Glaskoerperzellen beim Kaninchen. Graefes Arch Klin Exp Ophthalmol 187:21, 1973. 22. Balazs EA: Fine structure of the developing vitreous. In International Opthalmology Clinics, Ocular Fine Structure for the Clinician, Vol. 15, Zinn K, editor. Boston, Little Brown, 1975