* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Coronary artery disease (CAD)
Survey
Document related concepts
Electrocardiography wikipedia , lookup
Heart failure wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Saturated fat and cardiovascular disease wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Cardiac surgery wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
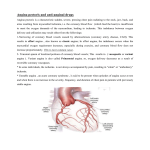
Coronary artery disease (CAD) By far, the most common form of coronary artery disease (about 90%) is atherosclerosis (gr. Athero – gruel, paste, porridge, sclerosis – hardening). Atherosclerosis is caused by deposition of fibro-fatty lesions on the intimal lining of the large and medium arteries (common sites include aorta and branches, coronary arteries, and in the brain). Lesions (referred to as the atheroma) usually begin as grayish/pearly white slightly elevated thickenings of the intimal layer. Atheromas contain a core of lipid material (primarily cholesterol), and are covered by a fibrous cap (consisting of connective tissue and proliferated smooth muscle cells) Cholesterol - (your body needs cholesterol!!! and in fact the liver produces most if not all you would need on a daily basis). A fatty, wax like material used by the body to help construct cell membranes, and is essential to nerves and brain function. It also makes hormones and is a constituent of the bile, which aids in digestion. All the cholesterol we need is manufactured in the liver. If we eat foods high in cholesterol such as organ meats, egg yolks, and dairy fat, we risk the possibility of heart disease and clogged arteries. Since cholesterol is a fat, it is not soluble in blood. Certain substances called lipoproteins act as carriers to usher the cholesterol through the body. Lipoprotein = cholesterol + it’s transport protein (cholesterol is not soluble in the blood) High Density Lipoproteins - These fatty proteins act as brooms, sweeping out undesirable cholesterol from the arteries. The more the merrier for these little housekeepers. Keep them happy and abundant with normal weight, plenty of exercise and monounsaturated foods. Low Density Lipoproteins - These bad guys are the opposite of HDL's. They contain high amounts of cholesterol and low amounts of protein. They deposit their cholesterol in arteries where it forms plaque. To keep them at bay, use the same formula as for HDL's and add some soluble fibre, such as oats and beans, to your diet. LDL's are the most common type of cholesterol in your blood stream Atheroma: Possible hypothesis of atheroma development: An injurious agent (smoking, dysfunctional immune mechanisms, mechanical stress from conditions such as hypertension etc.) injures the endothelial layer. Low density lipoproteins (LDL’s), and cholesterol infiltrate the area, while smooth muscle cells proliferate to the area (theory has it that following injury platelets congregate in the area. Platelets contain a strong mitogenic (cell division and growth) factor which causes the development and proliferation of smooth muscle cell to the injured area) Arteriosclerosis is caused by the deposition of calcium as opposed to fatty substances (or calcification on “old” atheroma’s) and causes hardening of the arteries, limiting the ability of blood vessels to change their diameters Complications of coronary artery disease: Silent myocardial Ischemia Angina pectoris Myocardial infarction Silent myocardial Ischemia Chronic sub – clinical myocardial malnutrition due to partial occlusion of coronary arteries Episodes of cardiac ischemia that produce no type of angina at all. Hence, the name “silent” myocardial ischemia. This type of cardiac ischemia is usually diagnosed from an exercise stress test. Ultimate result congestive heart failure Angina pectoris (angina = L. Angere – to choke) Angina is not a disease; it is a symptom of coronary artery disease Angina (angina pectoris) is a type of temporary chest pain, pressure or discomfort. Condition is caused by intermittent ischemic attacks of the myocardium Intermittent Ischemic Attacks Episodic symptoms occur when a partially occluded artery cannot deliver enough blood for high metabolic need circumstances, but delivers enough in low metabolic need situations. Remember: Ischemia = inadequate perfusion. Cardiac ischemia is a situation in which the blood flow within a coronary artery is limited to the point where the oxygen needs of the heart muscle cannot be met (hypoxia). Cardiac ischemia occurs when a coronary artery (which delivers oxygen-rich blood to the heart) is either partially or completely blocked. As a result of this blockage, blood flow and oxygen delivery to the heart muscle are limited. Intermittent Ischemic Attacks of cardiac muscle causing pain in the heart distribution pattern = Angina Pectoris Intermittent Ischemic Attacks of skeletal muscle causing pain in the legs (often limiting exercise tolerance) = Intermittent Claudication Intermittent Ischemic Attacks of Brain Tissue = Transient Ischemic Attack (T.I.A.) Angina and Atherosclerosis: Atherosclerosis causes narrowing of lumen size by virtue of plaque formation/occlusion. Narrowing of coronary arteries limits blood flow (perfusion) to the myocardium. As metabolic needs of heart muscle increase, ischemia results (not enough blood = not enough oxygen). Lactic acid accumulates (myocardium must revert to anaerobic energy) and pain ensues. Angina is a strong predictor of heart attack / myocardial infarction (M.I.). The heart can only function anaerobically for short period of time. Angina pectoris 90% caused by atherosclerosis 10% caused by stenosis (thinning, narrowing, thickening, fusing or blockage of a passage way) of one or more arteries o Scarring o Vasospasm Stable Angina The angina attacks happen only when the heart needs extra oxygen, like when a person climbs a long flight of stairs or jogs across the street. Unstable Angina angina attacks may occur even when a person is at rest Distribution pattern (similar to M.I. and pec major/ minor trigger points) Chest wall (upper ½) Left arm and shoulder Left neck and jaw Maybe right sided in some people Tight squeezing feeling under the sternum *Signs and symptoms subside with decrease in metabolic need.* Medications: Are taken at the beginning of an attack and typically act to quickly vasodilate vessels to improve perfusion of the myocardium. The most common medication for Angina is nitroglycerin. It was initially thought that nitroglycerin selectively affected the coronary arteries, but recent studies show that peripheral arteries are also affected, helping to further lessen the load on the heart. Nitroglycerin, when used to rapidly relieve occasional Angina symptoms, is usually administered sublingually (rapid absorption into the blood stream through mucus membranes) and takes effect within 2 to 3 minutes. It may be administered in tablet or spray form. More severe/unstable types of angina may involve the client wearing a nitroglycerine skin patch (provides a more constant supply of mediation to keep the arteries dilated) Possible complications Angina attacks usually pass with little long-term damage to the heart, but the episodes of cardiac ischemia that cause the attacks can progress to problems if untreated: They can cause arrhythmias (alterations in normal heart beat pattern), which in turn can lead to either syncope (fainting) or sudden cardiac death. Severe or lengthy episodes can trigger a heart attack. The small effects of minor episodes can eventually add up and lead to permanent weakening of the heart muscle (cardiomyopathy). Typical precipitators of angina attacks Overexertion, sudden physical exertion Emotional stress, Strong emotions, such as anger or frustration — even during a dream Sudden large scale temperature changes or altitude changes Smoking (causes micro-injury and contributes mutagenic agents) Eating very large meals Reactions to certain medications and other chemicals Possible massage therapy precautions Hydro – extremes – temperatures ( eg. Thermaphore of back, cold applications), full body applications (e.g. sauna, affusions) Manipulations – which result in significant increase in sympathetic activation o Heavy tapotement o Frictions and other painful techniques (trigger points, deep petrissage) Depending on how weak the heart function is overall, manipulations, which increase venous return overall, may be enough to promote angina. Clinical issues for the R.M.T. During case history taking get a clear picture of the frequency and severity of the attack, and the persons typical precipitators. Very unstable angina (erratic frequent attacks, attacks are precipitated very easily) may not be a good match with massage therapy but in most cases angina pectoris clients can be massaged with appropriate attention to possible precipitators. Meds issues – know in advance where their medication is and the prescribed dose o With patches – don’t physically manipulate them o Can increase delivery rate to the client and can dose themselves (the therapist) o Don’t wet or oil the patch (avoid touching the patch by 4 inches in all directions) If attack develops during a massage o Stop the treatment o Do what’s appropriate: vis a vis meds o Position in supine with trunk elevated or seated comfortably o Monitor and maintain calm environment o Be ready to call for medical assistance (911) if needed What lifestyle changes can the client make? A heart-healthy diet that is low in cholesterol and fats and oils Good control of diabetes and high blood pressure (hypertension) Regular exercise Quitting smoking and staying away from second-hand tobacco smoke