* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Name that Lesion It`s Catchy!
African trypanosomiasis wikipedia , lookup
Microbicides for sexually transmitted diseases wikipedia , lookup
Cryptosporidiosis wikipedia , lookup
Sarcocystis wikipedia , lookup
Clostridium difficile infection wikipedia , lookup
Onchocerciasis wikipedia , lookup
Gastroenteritis wikipedia , lookup
Hepatitis C wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Leptospirosis wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Trichinosis wikipedia , lookup
Hepatitis B wikipedia , lookup
Herpes simplex virus wikipedia , lookup
Oesophagostomum wikipedia , lookup
Neonatal infection wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Herpes simplex wikipedia , lookup
Schistosomiasis wikipedia , lookup
Epidemiology of syphilis wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
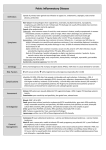
It’s Catchy! Creepy Crawlers/ Lumpy Bumpys Pediatric Pearls 100 100 100 100 200 200 200 200 200 300 300 300 300 300 400 400 400 400 400 500 500 500 500 500 It Burns! Name that Lesion 100 A 26 year old woman presents to ED with fever, chills, nausea, dysuria, lower abdominal pain, and vaginal discharge. What is the diagnosis? Name 2 causes. Name 2 complications. Pelvic Inflammatory Disease A spectrum of infections of the female genital tract that includes endometritis, salpingitis, tubo-ovarian abscess, and perotinitis. Caused by an ascending infection from the vagina or cervix. Most commonly chlamydia or gonorrhea. Most common serious infection in women. Complications include sepsis, perihepatitis (FitzHugh-Curtis), infertility, chronic pelvic pain and ectopic pregnangy. PID History and Physical Exam History may include bilateral lower abdo pain, low back pain, vaginal discharge, and irregular vaginal bleeding in a sexually active woman. May have systemic/toxic symptoms of fever, nausea, vomiting, chills. Exam may show tender lower abdomen, mucopurulent cervical discharge, cervical motion tenderness, uterine tenderness, adnexal tenderness. PID work-up and treatment Should do pregnancy test, urinalysis and urine culture, and cervical cultures or urine for GC and chlamydia. Consider testing for other STIs (HIV, syphilis). Toxic, pregnant, or patients with tubo-ovarian abscess should be admitted. Outpatient treatment is usually one dose of IM ceftriaxone and a 2 week course of PO doxycycline. Should discuss safe sex, abstinence until treatment completion, and referral of partners for treatment. A 30 y.o. man presents to ED with dysuria and urethral discharge, myalgias and conjunctivitis. What is the likely diagnosis? What is one cause? Urethritis Inflammation of the urethra is most commonly caused by STIs and is classified as gonococcal urethritis (GCU) or non-gonococcal urethritis (NGU). NGU is associated with reactive arthritis. GCU is usually abrupt in onset over 3-4 days, NGU can have a more insidious onset of symptoms. History may include urethral discharge, dysuria, hematuria, urethral pruritis and painful intercourse in a sexually active male. Ask about arthritis/conjunctivitis and systemic symptoms. Urethritis cont… Exam may show an inflammed urethral meatus and/or urethral discharge. The urethra can be milked to try and express discharge. Look for other STI lesions as well. Work-up should include urethral swabs or urine for GC/chlamydia and screening for other STIs. Treatment is a single IM dose of ceftriaxone and either a single oral dose of azythromicin or a one week course of oral doxycycline. A 35 y.o. woman presents to ED with a vaginal pruritis and increased vaginal discharge. What is the likely diagnosis? What are 2 possible causes? Vulvovaginitis Inflammation of the vulva and vagina. Diagnosis is based on the presence of symptoms of a change in vaginal discharge and/or vulvovaginal discomfort. Bacterial vaginosis resulting from a loss of normal vaginal lactobacilli is the cause in 40-50% of cases. Candidiasis accounts for 20-25% and trichomoniasis accounts for 15-20%. Chemical irritation and poor hygiene are also contributing factors. Vulvovaginitis Physical exam may show erythema and edema of the vulva and vagina, discharge that may be foul, thin and grey, white , yellow or green, and/or curd-like. Vaginal foreign bodies may be seen. Work-up should include vaginal pH, and microscopy for wet mount and KOH testing. Cultures/swabs for trichomonas, yeast, and STIs may be considered. Clinical Elements Symptoms Signs Microscopy Bacterial Vaginosis Trichomoniasis Vaginal Candidiasis Vaginal odor + +/- - Vaginal discharge Thin, gray, homogenous Green-yellow White, curdlike Vulvar irritation +/- + + Dyspareunia - + - Vulvar erythema - +/- +/- Bubbles in vaginal fluid + +/- - Strawberry cervix - +/- - Clue cells + - - Motile protozoa - + - - - + Saline wet mount KOH test Pseudohyphae A 13 y.o. boy presents to ED with dysuria, urinary frequency, urgency, scrotal pain and swelling. What is the most likely diagnosis? What are 2 causes? What do you need to rule out? A 13 y.o. boy presents to ED with dysuria, urinary frequency, urgency, scrotal pain and swelling. What is the most likely diagnosis? What are 2 causes? What do you need to rule out? Epididymitis Inflammation of the epididymis, most commonly caused by infection. In sexually active men it’s usually from gonorrhea or chlamydia. In the non-sexually active population it’s most commonly caused by e.coli. Most common cause of scrotal inflammation. Need to rule out testicular torsion in any presentation of testicular pain. Symptoms usually progress over 24 hours and can include scrotal pain, swelling, urinary frequency, urgency, dysuria, nausea, fever, chills, and discharge. Epididymitis Exam may show edematous tender epididimus, erythematous/edematous scrotum, may have scrotal abscess. May see urethral discharge. Prehn sign= scrotal elevation relieves pain in epididimytis but not in torsion. But it’s not reliable. Work-up may include urinalysis/culture, urine for GC and chlamydia, gram stain/culture of any discharge, ESR/CRP may help differentiate from torsion if it’s elevated. U/S may help distinguish from torsion. Treatment is with antibiotics. Septra for non-sexually active patients, ceftriaxone and doxycycline for sexually active. A 32 y.o. man presents to ED with fever, chills, dysuria, urinary frequency, urgency, hesitancy, and incomplete voiding. What’s the likely diagnosis? What is one possible physical exam finding? What is one possible cause? Bacterial Prostatitis Inflammation of the prostate most commonly caused by sexually transmitted bacteria. Symptoms can include fever, chills, malaise, arthralgias, myalgias, perineal pain, dysuria, urinary frequency, urgency, nocturia, hesitancy, incomplete voiding, weak stream, lower back and abdominal pain, and urethral discharge. Bacterial Prostatitis Exam may show a tender, nodular, hot, boggy, or normal prostate on DRE. May have suprapubic abdominal pain. Potential causes include gonorrhea, chlamydia, trichomonas, e.coli, and other gram negative bacteria. Urine culture may identify the causative agent. Patients should be admitted if any systemic symptoms are present. Otherwise treatment can be a 2-4 week course of PO abx. Septra or floroquinolones are options but also need to treat for GC/chlamydia if they’re suspected. Balanitis/Balanopsthitis Inflammation of the glans of the penis, +/- foreskin inflammation. Occurs in up to 3% of uncircumcised males. History of penile discharge, inability to retract foreskin, tenderness and itching of glans. Exam shows erythema/edema of glans/foreskin, discharge, ulcerations, phimosis. Balanitis/Balanopsthitis In adults most common underlying condition seen with it is diabetes. Can also be from poor hygiene, chemical irritants, etc. Infectious causes include candida, HPV, gardnerella, syphilis, trichomonas, strep. Work-up with culture of discharge, glucose check, wet mount, syphilis serology. Treatment depends if it’s infectious and what the infectious agent is. Herpes Simplex Virus HSV is very common. Approximately 65% of the United States population is seropositive for HSV-1 by the fourth decade of life and 25% for HSV-2. Primary infections can be asymptomatic or have symptoms of local pain, tingling, itching, and burning and then the development of the typical lesions which are vesicular or ulcerative on an erythematous base. After primary infection the infection becomes latent in the sacral sensory ganglia. The viruses become reactivated secondary to a wide variety of stimuli and secondary infection can occur. Herpes Simplex Virus Lesions coalesce and then heal over the next several weeks. Tender bilateral lymphadenopathy occurs with genital lesions. Viral culture from skin vesicles can be done to help establish diagnosis. A pregnant woman near term should be referred to obstetrics. Antivirals can inhibit virus replication and suppress clinical manifestations but are not a cure. Rates of relapse are similar in treated and untreated patients. Genital HSV should be treated with a 10 day course of oral acyclovir. Patients should be advised to be abstinent when lesions are present and use condoms all the time. Chancre The characteristic lesion seen in primary syphilis. Develops after an incubation period of 3-6 weeks. Frequently solitary, may be multiple. Sometimes seen as "kissing" lesions on opposing skin surfaces, for example, the labia. The lesion has a punched-out base and rolled edges and is highly infectious. It resolves 4-6 weeks after it forms and does not typically leave a scar. Chancroid Sexually transmitted infection caused by Haemophilus ducreyi, characterized by painful ulcers, bubo formation (swelling of lymph nodes), and painful inguinal lymphadenopathy. Uncommon in North America but much more common in Africa and part of Asia- take a travel hx. Much more common in men than women. Organisms enter through breaks in the skin on the genitals, and an erythematous papule forms, becoming a pustule in 2-3 days. The pustule ulcerates in a matter of weeks, and lymphadenopathy also usually is seen. Painful inguinal lymphadenopathy or bubo formation is present in 50% of patients. Chancroid Diagnosis is made clinically based on the patient having one or more painful ulcers (ulcers with painful adenopathy are pathognomonic) with no evidence of syphilis or herpes simplex virus. For treatment, ulcers should be cleaned and buboes should have I & D. Treatment is a single dose of PO azithromycin or a single dose of IM ceftriaxone. Should test for HIV, syphilis, and other STIs. Perianal Group A Strep Perianal Group A Strep is one of the causes of vulvovaginitis, most commonly seen in children. Usually results in a beefy red perineal area that is edematous and tender and has well defined margins. Fissures, drainage, and hemorrhagic spotting may be present. Diagnosis is made by bacterial culture of the area. Treatment involves topical antibiotic treatment with mupirocin or erythromycin, or oral penicillin V. What is the most common bacterial STI in North America, and what are 2 possible physical exam findings? Chlamydia Caused by Chlamydia trachomatis bacterium, has an overall prevalence of 5% in North America. The incubation period is 1-3 weeks. Approximately 50% of infected males and 80% of infected females are asymptomatic, but infection may cause a mucopurulent cervicitis in females and urethritis in males. Forty percent of women and 20% of men with chlamydial infection are co-infected with gonorrhea. Chlamydia On exam may find mucopurulent urethral discharge, rectal discharge, cervical/vaginal discharge, or epididymal tenderness/swelling. Cervical motion tenderness, adnexal tenderness, and lower abdominal pain are also common. Can test by doing nucleic acid amplification to detect chlamydial DNA either in urine or with a genital swab. Should also test for pregnancy and other STIs. Treatment is a single oral dose of azythromycin or 7 days of doxycycline. Consult gyne for severe PID or if patient is pregnant. Contact partners for treatment as well. Should also treat for co-infection with gonorrhea. What is the second most common bacterial STI in North America and name 2 associated diseases? Gonorrhea Gonorrhea is a purulent infection of mucous membrane surfaces caused by a sexually transmitted microorganism, Neisseria gonorrhoeae. Retrograde spread of the organisms occurs in as many as 20% of women with cervicitis, often resulting in PID. Epididymitis or epididymo-orchitis may occur in men after gonococcal urethritis. Disseminated gonococcal infection (DGI) occurs following approximately 1% of genital infections. Gonorrhea Most common symptoms in men are dysuria and urethral discharge. Women usually have vaginal discharge as main symptom. On exam may find mucopurulent urethral discharge, rectal discharge, cervical/vaginal discharge or epididymal tenderness/swelling. Cervical motion tenderness, adnexal tenderness, and lower abdominal pain are also common. Gonorrhea Can test with a culture of discharge or with nucleic acid amplification for DNA in urine or swabs of infected areas. Should also test for syphilis and Chlamydia and look for signs of other STIs on exam. Consult gyne for severe PID or pregnant women. Treat with a single dose of PO cefixime or IM ceftriaxone. Also treat for Chlamydia. Partners need to be referred for treatment. What is the most common presentation of HSV-2 infection and what percentage of patients present that way? Herpes Simplex Virus 80% of patients with primary HSV-2 infection are asymptomatic. Approximately 65% of the United States population is seropositive for HSV-1 by the fourth decade of life and 25% for HSV-2. Primary infections can be symptomatic with symptoms of local pain, tingling, itching, and burning and then the development of the typical lesions which are vesicular or ulcerative on an erythematous base. After primary infection the infection becomes latent in the sacral sensory ganglia. The viruses become reactivated secondary to a wide variety of stimuli and secondary infection can occur. Herpes Simplex Virus Lesions coalesce and then heal over the next several weeks. Tender bilateral lymphadenopathy occurs with genital lesions. Viral culture from skin vesicles can be done to help establish diagnosis. A pregnant woman near term should be referred to obstetrics. Antivirals can inhibit virus replication and suppress clinical manifestations but are not a cure. Rates of relapse are similar in treated and untreated patients. Genital HSV should be treated with a 10 day course of oral acyclovir. Patients should be advised to be abstinent when lesions are present and use condoms all the time. What is the most common parasitic STI and how is it treated? Trichomoniasis Trichomoniasis is a nonreportable STI caused by the parasite Trichomonas vaginalis. -The prevalence in women is about 2.5%. In females, vaginitis is the most common manifestation of infection. Other complications include infection of the adnexa, endometrium, and Skene and Bartholin glands. Males are usually asymptomatic. When symptoms are present, they usually manifest as urethritis. Infection with T vaginalis is a marker of high-risk sexual behavior. Co-infection with other STDs is common. Trichomoniasis Presenting signs and symptoms may include vaginal or urethral discharge, odor, irritation, itch, dysuria, abdominal pain, and dyspareunia. In males, if symptomatic, there is usually only scant, thin discharge. If suspected should check vaginal pH and do microscopy for wet mount. Should also test for pregnancy and other STIs. A single oral dose of metronidazole is the treatment. What is the cause of syphilis and how is it treated? Syphilis Syphilis is an STI caused by the spirochete Treponema pallidum. It penetrates abraded skin or intact mucous membranes easily and disseminates rapidly, via the blood vessels and lymphatics. Primary syphilis is characterized by the development of a painless chancre at the site of transmission after an incubation period of 3-6 weeks. Secondary syphilis develops about 4-10 weeks after the appearance of the primary lesion and has a wide range of presentations. Systemic manifestations include malaise, fever, myalgias, arthralgias, lymphadenopathy, and rash. The rash of secondary syphilis typically consists of macular lesions symmetrically distributed over the body and may involve the palms, soles, and oral mucosae. Another skin findings of secondary syphilis is condylomata latum. Syphilis Latent syphilis is a stage at which the features of secondary syphilis have resolved, though patients remain seroreactive. About one third of untreated latent syphilis patients go on to develop tertiary syphilis, whereas the rest remain asymptomatic. Prevalence of approximately 3 per 100,000 in US. Occurs more commonly in men than women. Syphilis Serology is the best test. Should have a nontreponemal test first like VRDL and RPR. These are very sensitive for detecting secondary and tertiary syphilis, a bit less sensitive for primary syphilis. Because of the possibility of false-positive results, confirmation for any positive nontreponemal test should follow with a more specific treponemal test like the treponemal antibody absorption test. Patients with confirmed syphilis should be tested for other STIs including HIV. Treatment for syphilis symptoms present less than 1 year is penicillin G benzathine one dose IM. Follow-up VDRLs need to be done to look for clearance. Partners should be contacted and tested. Safe sex should be encouraged. Crabs (pubic lice) A sexually transmitted ectoparasite that lives on the body. Most common symptoms is itching. The crab louse is found firmly attached to the base of the pubic hair. Nits may also be found. Pubic lice may spread to hair around the anus, abdomen, axillae, chest, and eyelashes. Bluish grey macules, may be seen on the abdomen or thighs and are secondary to the bites of the crab louse. 30% of patients with crabs have a second STI so they should be investigated for other STIs. Chemical pediculicides are the mainstay of therapy. Treatment should be repeated in 7-10 days (the time needed for the eggs to hatch). Shaving of the hair is also an option. Genital Warts (Condyloma Acuminata) Caused by low risk strains of HPV. Is the most common STI. Annual incidence is 1% and lifetime prevalence is 50% in sexually active individuals. 2/3 of people who had sex with someone with active lesions will develop warts within 3 months. Present as painless bumps, pruritis, and discharge. Usually multiple lesions in more than one area. May have coital bleeding. Most commonly seen on the penile glans and shaft in men and the vulvovaginal and cervical areas in women. Eruptions can be pearly, filiform, fungating, cauliflower or plaque-like. Genital Warts The only work-up needed may be to test for other associated STIs. If visible genital warts are left untreated, they can undergo spontaneous resolution, increase in size, increase in number, or remain unchanged. Complete resolution of lesions after 2 years occurs in 75% of individuals without intervention. No treatment can be offered in ED but you can consider gyne referral if persistent, especially because of risk of malignant transformation. Bartholin Gland Abscess Bartholin glands are two glands that secrete mucous to moisturize the surface of the vaginal mucosa. Can get cysts from the ducts being blocked or abscesses from a cyst or the gland getting infected. Infections are not usually related to STIs. Approximately 2% of women will have bartholin gland swelling. History of a cyst is usually of painless labial swelling, possible dysparunia. An abscess can have acute painful unilateral labial swelling, pain with walking/sitting, dysparunia, and fever. There may be a history of pain relief with rupture of abscess. Bartholin Gland Abscess Exam shows a fluctuant labial mass, tender if it’s abscessed. May have discharge if it’s ruptured (non-purulent if it’s a cyst). For abscess e.coli is most commonly found, staph and strep too. GC and chlamydia are possible. No work-up is usually needed. A simply cyst can be treated with sitz baths TID to promote resolution or rupture of cyst. Abscesses usually need I & D. If it’s recurrent or unusaual may warrant a gyne referral. Condyloma Lata Condyloma lata is a genital manifestation of secondary syphilis. Can be confused with genital warts. The lesions exude highly infectious fluid and the patient will often have other constitutional symptoms of secondary syphilis including malaise, fever, myalgias, arthralgias, lymphadenopathy, and rash. Lymphogranuloma Venerum LGV is an infection of the lymphatics caused by some types of Chlamydia trachomatis. The primary lesion occurs 3-21 days after exposure and is a painless papule, shallow erosion, ulcer, or grouping of lesions with a herpetiform appearance. Can occur on the glans, urethra, penis shaft, or scrotum, in the vagina or on the vulva. The second stage begins about 10-30 days later with the formation of enlarged, tender regional lymph nodes known as buboes and there may be constitutional symptoms. The nodes frequently abscess and rupture. Lymphogranuloma Venerum The third stage is when proctocolitis develops, but most don’t progress to this stage. LGV is uncommon in north America but endemic in parts of Africa and Asia so take a travel history. Can test for Chlamydia, although you need a more specific test to look for the serovars that cause LGV. Can also try culturing the abscess fluid if you aspirate it. Treatment includes heat, NSAIDs, +/- aspiration of bubo and 3 weeks of oral doxycycline or erythromycin. A 4 year old girl presents to ED with anal and vulvar pruritis, sometimes waking her up at night. What is the most likely diagnosis? What is the treatment? Pinworms Most common symptom is anal pruritis but the infection can spread to the vulva and be easily confused with vulvovaginitis. The pale-colored female pinworm may be visibly seen in the perianal region. A specimen is best obtained by dabbing the stretched, unwashed perianal folds in the early morning with cellophane tape and affixing on to a slide. Treatment is not necessary although strict handwashing should be advised. If it’s symptomatic then treatment with anti-helmenthics is an option.