* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download The Vision - Legacy Health
Survey
Document related concepts
Optical coherence tomography wikipedia , lookup
Keratoconus wikipedia , lookup
Visual impairment wikipedia , lookup
Blast-related ocular trauma wikipedia , lookup
Idiopathic intracranial hypertension wikipedia , lookup
Eyeglass prescription wikipedia , lookup
Visual impairment due to intracranial pressure wikipedia , lookup
Vision therapy wikipedia , lookup
Mitochondrial optic neuropathies wikipedia , lookup
Corneal transplantation wikipedia , lookup
Cataract surgery wikipedia , lookup
Dry eye syndrome wikipedia , lookup
Transcript
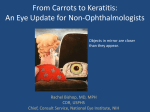
The Vision Information for supporters from Legacy Devers Eye Institute Inside this issue Helping people to see is very gratifying A story of faith, family and joy. . . . . 2 By James T. Rosenbaum, M.D., chief of ophthalmology Treating dry eye disease. . . . . . . . . . . . 3 Telemedicine aids eye screenings. . . . . 4 Emanuel clinic is thriving. . . . . . . . . . . 5 New physicians and fellows. . . . . . 6, 7 Publications, honors and awards, invited lectures . . . . . . . . 8–11 Summer 2014 People sometimes wonder, paid. He learned that he could earn a living “Do you like being a physifor doing something that could make him feel cian?” Or they ask a slightly good. What could be better? different version of the Medicine has changed dramatically in many same question, “Would you bureaucratic ways since my dad graduated want your daughters to be medical school in 1939. But maybe the biggest physicians?” Sometimes the change of all is how successfully we can treat James T. questioner appends “today,” or diseases, some of which are potential causes of Rosenbaum, M.D. asks, “Would you want your blindness. daughters to be physicians today?” — a slight Devers as an institution is the realization of change that recognizes how much medicine has what my father learned as an individual. Helpchanged. I come from a family ing people to see is very, very of physicians: my father, my gratifying. We do this one Helping people to see is brothers, my wife, both our patient at a time in the clinic; very gratifying. We do it daughters. So I do have some we do it for many at the for one patient in the clinic, perspective on doctoring. research bench; we do it for for many at the research My father wrote a famous the next generation when we book about being a physician. teach. We cannot do it withbench, for the next generaInitially the book was pubout our patients. We cannot tion when we teach. We lished as “A Taste of My Own do it without our patrons, cannot do it without our Medicine.” It was his story of who have generously suppatients or our patrons. battling cancer at age 70 after ported our ability to provide a lifetime of caring for others. care for those who cannot The book was retitled simply, “The Doctor.” afford it, and who support our mission to purDisney bought the rights to the book and made sue the discovery of new knowledge. a movie that starred William Hurt. TwentyInside the second issue of The Vision you will three years after its release, the book or movie learn about some of our endeavors to extend are required reading or viewing at medical cenwhat we can accomplish. You’ll learn about a ters around the world. blind patient who dedicates her life to inspirI tell you about my dad’s book because near ing others, a new clinic in an underserved area the start, he tells the story of one of his first of Portland and new technologies. The staff experiences as a physician. He made a house call at Devers derives gratification from helping and helped someone get well. Helping someone patients see. Thank you for reading our newsletwith health is a gratification that is virtually ter and giving meaning to our quest. impossible to top. But then as a bonus, he got The Vision ~ Summer 2014 2 Uveitis patient Joy Ross discovers what is truly important However, as we mentioned before, Joy is a stubborn sort, and she set her mind to working harder to regain herself and raise her children. They needed her. Daughters Isabella (now 11) and Georgianna (now 8) both were diagnosed with juvenile arthritis. ‘I learned to cope’ Isabella suffered with swelling The first thing Joy tells people in her joints; her vision was not when she meets them is that she Joy Ross with her daughters, Georgianna affected. Georgianna had the is blind. In part, because it can be and Isabella opposite — her joints were fine difficult to detect her blindness. but she was diagnosed with uveitis, which can lead She wears life-like prosthetic shells over her natural to a loss of vision. eyes and carries herself with the kind of spirit and Joy knew whom to call. She had begun receiving attitude of someone who knows where she is going. care from Jim Rosenbaum, M.D., chief of ophthal“If you tell me that I can’t do something, that gives mology at Legacy Devers Eye Institute and an me more reason to do it,” she says. expert in uveitis. In 2000, her care under Dr. RosenJoy was diagnosed at age 3 with juvenile onset baum was interrupted when the family moved to arthritis. Children with arthritis can sometimes Texas, but it resumed when they returned to Oredevelop uveitis — an inflammation of the inner gon. She quickly involved Dr. Rosenbaum in caring parts of the eye that can lead to a loss of vision. for her daughters. “We love him so much,” Joy says. Through childhood, Joy lost more sight. “The Through Legacy Devers, along with treatment for best I can ever remember seeing was only in one juvenile arthritis through Randall Children’s Hospieye, the big “E” at the top of the eye chart,” says Joy, tal at Legacy Emanuel, the girls are doing well. The now 36. “In elementary school, it was enough to see future seems promising. “The treatments have shapes and colors. But it was everything I knew, so I improved since I was a kid,” Joy says, noting that learned tricks, learned to cope.” Georgianna has not lost vision despite having uveitis. Joy Ross has quite a story to tell. A story of faith and family. Of happiness and hope. Of medicine, caring and, well, joy. It’s a story about what life is really about. “I have found true happiness,” Joy says. “I discovered what is truly important.” A dark curtain Fast forward several years into a life with a marriage and two small daughters, and Joy is in Disneyland at Christmastime. “The most magical place, the most magical time,” she recalls. “Then, it was surreal; a dark curtain came over me.” At age 30, Joy had lost all of her vision; the retina had detached because of all of the years of uveitis. “It was the death of my life as I knew it,” she says. “It was hard for me; I had to re-find my independence to be a mother and a wife.” A new life After receiving a guide dog, Joy helped start a group called Mommies with Guides. She has found a purpose and a passion — in raising her children and helping others to live with blindness. “Our faith in God helped us,” Joy says. “We are just so thankful. I have the most amazing family, so many blessings that it makes my life so special. And being blind helped me discover those blessings. I discovered what is truly important.” 3 By Peter Veldman, M.D. Dry eye disease is one of the most common ocular conditions and a cause of significant symptoms, ranging from mild discomfort and redness to pain, light sensitivity and decreased vision. Many factors can cause dry eyes, including decreased tear production, increased tear evaporation, inflammatory conditions, medications, age and climate, among other causes. The Cornea Service at Legacy Devers Eye Institute has extensive experience in the assessment, diagnosis and management of dry eyes. They may recommend lubrication with artificial tears, blood serum drops, anti-inflammatory therapy, plugs in the tear drains or surgery to permanently close the tear drains. Fish oil, flaxseed oil and increased water intake can be helpful as well. Also, we are currently enrolling patients in a multicenter phase 2 clinical study, evaluating a testosterone ophthalmic emulsion versus placebo in This picture of the cornea, taken using a green diagnostic dye, shows areas of dryness in the lower half. the management of meibomian gland dysfunction, a common contributor to eye dryness. If you are experiencing symptoms of dry eye disease such as redness, tearing, grittiness, sensitivity or vision changes, please call 503-413-8202 to set up an appointment for an evaluation. JoAnne Fraser is retiring after 24 years at Legacy Devers JoAnne Fraser, certified ophthalmic technician, is retiring in June after 24 years of working at Legacy Devers Eye Institute in the Glaucoma Department. The University of Minnesota certified her as an JoAnne Fraser, ophthalmic technician in 1969. She COT worked in remote Alaskan villages for two years in the early ’70s and then migrated to Portland. She has been an ophthalmic technician for 45 years! The ophthalmic technicians nicknamed her “Dr. Fraser” because of her breadth of knowledge. She has trained hundreds of ophthalmic technicians, ophthalmology residents, ophthalmology fellows, and other eye doctors in the art of ophthalmology testing, surgery and patient education. She developed the annual Thorny Issues Ophthalmic Technician Program and has been an examiner for the Oregon Ophthalmic Certification Program. Eye care in Portland is spectacular, and JoAnne has helped create this reputation. JoAnne will spend more time with her family (three children and eight grandchildren), backpacking, rock climbing, snowshoeing and working on her house and garden. We are grateful to her for all of her teaching and patient care. The Glaucoma Department is donating $1,000 in her name to the Devers Cioffi Fellowship Education Fund. Others interested in donating can use the enclosed envelope or visit www. legacyhealthgiving.lhs.org/bbis/deversgiving. The Vision ~ Summer 2014 Not a dry eye in the house: Treating dry eye disease at Devers The Vision ~ Summer 2014 4 Telemedicine aids screenings for diabetic retinopathy By Christina Sheppler Can a screening at your primary care clinic replace your yearly visit to the eye doctor? Telemedicine refers to the electronic transfer of information for the purpose of providing medical care. It can improve access to health care, especially for those in rural areas. In ophthalmology, telemedicine is most often used to screen for diabetic retinopathy. Diabetic retinopathy (DR) is a disease that damages the blood vessels in the eye, and it is the leading Dr. Mansberger using a nonmydriatic camera, which works without the need for dilation. The camera provides access to diabetic eye exams and helps prevent cause of blindness in U.S. adults blindness in patients with diabetes. age 20–74. DR usually progresses significantly more likely to be screened for DR when in stages, and people in the early stages of the discompared to those in the eye care provider group. ease often have no symptoms. For this reason, it is After participating in the study for two years, those important for those diagnosed with diabetes to be in the eye care provider group were also given access screened yearly for retinopathy. If DR is diagnosed to telemedicine. and treated early, the chance of vision loss can be Over the next three years, the percentage of pargreatly reduced. Unfortunately, only about half ticipants screened for retinopathy in the eye care of the people diagnosed with diabetes obtain the provider group increased by nearly 20 percent. annual screening. They also found that many people do not realize Steven L. Mansberger, M.D., has spent nearly 10 diabetic eye exams are covered by medical insurance years investigating the use of telemedicine to improve rather than vision insurance. This finding suggests screening rates. Screening for DR with telemedithat patients need to know that diabetic eye exams cine involves the use of a special camera that can are covered by their medical benefits. take pictures of the eye without requiring dilation Dr. Mansberger believes that offering telemediwhen patients visit their primary care doctor. The cine during routine visits in primary care clinics is images are then sent electronically to Legacy Devers a promising way to increase the number of people Eye Institute. screened for retinopathy. Most recently, Dr. Mansberger partnered with the Legacy Devers is currently working to make Oregon Prevention Research Center at OHSU to telemedicine available in primary care clinics at conduct a telemedicine study with Native AmeriLegacy. This effort will make getting screened for cans. This study was funded by the Centers for DR easier for the patient and will aid in the goal of Disease Control and Prevention (CDC). Results detecting and treating diabetic retinopathy before showed that those with access to telemedicine were vision loss occurs. 5 By Blake Acohido, M.D., Legacy Devers Eye Institute–Emanuel Legacy Devers Eye Institute–Emanuel turned six months old in early May. We developed the clinic to serve Legacy Emanuel and its Level 1 Trauma Center, Randall Children's Hospital at Legacy Emanuel, our Blake Acohido, north and northeast neighbors and M.D. Legacy Emanuel Medical Center employees and their families. The clinic has officially blossomed from snuggly newborn to squirming infant. It has been an exciting first six months as we zoomed past our Jennifer Prunty, developmental milestones. In O.D. addition to smiling, rolling over and sitting up, we have seen significant growth in the clinics of both Blake Acohido, M.D., and Jennifer Prunty, O.D. Outside of the clinic, we have taken strides to build our presence in our surrounding community — Northeast Portland. In January, Steven Mans berger, M.D., Dr. Acohido and Dawn Brunelle partnered with the Oregon Academy of Ophthalmology and the American Academy of Ophthalmology in a program known as “Screening with your Legislator,” in which they provided glaucoma screenings to senior citizens at the Urban League’s Multicultural Senior Center. They provided screening for 43 patients, who were all very excited to discover that there is now comprehensive eye care available in their neighborhood. What is more, State Representative Lew Frederick and State Senator Chip Shields each made an appearance, taking time to chat with patients (their constituents) as they waited to undergo screenings. In April, Dr. Prunty teamed up for a vision screening with the Lions Club and Casey Eye Institute to provide eye examinations and eyeglasses to those in need. More than 100 people were screened and provided with much-needed care. Also in April, Dr. Prunty participated in Legacy Emanuel Medical Center’s Stepping On program, a community-based program aimed at reducing the incidence of falls in the elderly. Dr. Prunty discussed vision and fall prevention, emphasizing the importance of routine eye examinations, early treatment for cataracts, and how certain eye diseases can increase the risk for falls. The talk concluded with examples of how patients coping with vision loss can reduce hazards in the home that could contribute to their risk of falling. Community optometrists are now sending patients to Legacy Devers Eye Institute–Emanuel for urgent same-day evaluations, subspecialty care appointments and routine ancillary testing. As Legacy Devers Eye Institute–Emanuel continues in its maturation, there remain numerous developmental milestones to surpass and smile upon. Our clinic at Legacy Emanuel’s team looks forward to further innovation and steady growth. To make an appointment, call 503-413-3030. The Vision ~ Summer 2014 This new clinic is thriving: Legacy Devers Eye Institute–Emanuel The Vision ~ Summer 2014 6 Three providers join Legacy Devers Eye Institute Jennifer Prunty, O.D. Dr. Prunty received her degree from Ferris State University Michigan College of Optometry and performed her optometric residency with a focus in ocular disease management at Bascom Palmer Eye Institute in Florida. She is a fellow with the American Academy of Optometry. Dr. Prunty’s clinical interests include glaucoma, cornea, diabetic eye care and ocular oncology. She enjoys traveling, camping and hiking. Sirichai Pasadhika, M.D. Dr. Pasadhika was born in Thailand. He went to medical school and did ophthalmologic training in Bangkok and was trained to be a retina specialist in Sydney, Australia. He completed a uveitis and surgical internship at OHSU, a retinal degeneration fellow- ship at the University of Illinois at Chicago, and an ophthalmology residency in Arizona. Dr. Pasadhika is married and has two children. Ashley Hayden, M.D. Dr. Hayden, a native Oregonian, graduated from Lakeridge High School and continued on to Yale University. She received her medical degree from the University of Southern California and completed her ophthalmology residency at the University of Washington in 2011. She returned to Portland to be close to family, and worked with Dr. Rosenbaum at Casey Eye Institute to further her understanding of the diagnosis and treatment of uveitis. She joins the ophthalmology group at Legacy as a volunteer, and will continue her working relationship with the uveitis service. She has two boys and tries to take them skiing as often as possible. Save the date • Save the date Legacy Devers Eye Institute presents Thorny Issues in Ophthalmology Goes to the Movies (cornea, glaucoma and oculoplastics) A medical education conference for ophthalmologists and optometrists Sept. 19–20, 2014 Legacy Emanuel Medical Center • Lorenzen Auditorium 2801 N. Gantenbein Ave., Portland An ophthalmic technician program will take place on Friday, Sept. 19. For more information email [email protected] or call 503-413-6540. 7 Eliesa Ing, M.D. Dr. Ing is coming on a fellowship after completing three years of service in Landstuhl, Germany, as a comprehensive ophthalmologist in the United States Air Force. She completed her residency training at the University of Texas Health Science Center at San Antonio and medical school at the University of Vermont College of Medicine in Burlington. Dr. Ing is interested in glaucoma surgical treatments and newly emerging technologies to diagnose and track disease. She enjoys long-distance running and is excited to be back in her home state. Shivali Menda, M.D. Dr. Menda is originally from Seattle, Washington. She went to medical school at Oregon Health & Science University and completed an ophthalmology residency at University of California, San Francisco. She is excited to be back in Portland to pursue a glaucoma fellowship. Her hobbies include spending time with family and friends, traveling and yoga. Christopher Sales, M.D., MPH Dr. Sales graduated from Brown University. After working for two years in a health policy institute at Columbia University College of Physicians and Surgeons in New York, he attended a four-year dual-degree program in medicine and public health at Tufts University School of Medicine in Boston. As a medical student, he was awarded honors in research after completing a one-year fellowship in the epidemiology of ocular disease at the University of California, San Francisco, and was inducted into the Alpha Omega Alpha Honor Medical Society. He interned at Harvard’s Beth Israel Deaconess Medical Center and was trained in ophthalmology at Stanford University, where he was recognized as consultant of the year at both the university and county hospitals. As this year’s cornea fellow, Dr. Sales joins Mark Terry, M.D., and Michael Straiko, M.D., at Legacy Devers Eye Institute. Amde Selassie Shifera, M.D. Dr. Shifera was born and grew up in Ethiopia. He attended medical school at Addis Ababa University in Ethiopia, graduating in 1989. After working in Ethiopia as a general medical practitioner for 10 years he relocated to the United States to further his training and prepare for a career as a physician scientist. He attended graduate school at the Albert Einstein College of Medicine in New York and graduated with a Ph.D. in microbiology and immunology in 2007. Subsequently he completed a residency in ophthalmology at the University of Florida. As an ophthalmologist, Dr. Shifera is interested in the medical and surgical management of inflammatory and infectious diseases affecting the eye. As an immunolgist, he is interested in conducting basic and clinical research to gain a better understanding of inflammatory diseases affecting the eye. His hobbies include watching sports, reading and travelling. How to donate to Legacy Devers Eye Institute Legacy Devers Eye Institute provides some of the world’s best research, education and clinical care. We are also the largest provider of free and lowcost eye care in Oregon. We appreciate the grateful patients and donors who support our mission of research, education and clinical care through the Good Samaritan Foundation. Every donation regardless of the amount makes a difference to saving someone’s sight. To make a donation, contact Rena Whittaker at the Good Samaritan Foundation at 503-413-5585 or [email protected], or visit www.legacyhealth. org/giving. The Vision ~ Summer 2014 Legacy Devers welcomes four fellows for 2014–15 The Vision ~ Summer 2014 8 Publications Fortune B, Reynaud J, Wang L, Burgoyne CF. Does optic nerve head surface topography change prior to loss of retinal nerve fiber layer thickness: a test of the site injury hypothesis in experimental glaucoma. PLoS One 2013. In press. Gardiner SK, Fortune B, Demirel S. Signal-to-Noise Ratios for Structural and Functional Tests in Glaucoma. Trans Vis Sci Tech 2013. In press. Campbell JP, Davis S, Flaxel C, Rosenbaum JT, Lin P. Acquired Drusenoid Deposits on Infrared Imaging as a Sign of Vitreoretinal Lymphoma. Ocul Immunol Inflamm. 2013 Sep 24. [Epub ahead of print] Mansberger SL. “Cataract surgery: The ‘New’ glaucoma procedure” Book chapter in Surgical Innovations in Glaucoma. Editors: Samples and Ahmed. 2013. In press. Estrovich I, Mansberger SL. “Does cataract extraction produce a significant and sustained IOP reduction? When should I perform a combined procedure versus cataract surgery alone?” Curbside Consultation Glaucoma: 49 Clinical Questions, second edition. Editors: Heuer, Lewis, Panarelli and Gedde. 2013. In press. Lin P, Suhler EB, Rosenbaum JT. The Future of Uveitis Treatment. Ophthalmology. 2013 Oct 26. doi:pii: S0161-6420(13)00777X.10.1016/j.ophtha.2013.08.029. [Epub ahead of print] PMID: 24169255 [PubMed — as supplied by publisher] Related citations Select item 24143861[ ]2 Ali A, Rosenbaum JT. TINU (Tubulointerstitial Nephritis Uveitis) Can Be Associated with Chorioretinal Scars. Ocul Immunol Inflamm. 2013 Oct 21. [Epub ahead of print] PMID: 24143861 [PubMed — as supplied by publisher] Rosenbaum JT. The E Coli Made Me Do It, The New Yorker, online, November 11, 2013 http://www.newyorker.com/online/ blogs/elements/2013/11/the-e-coli-made-me-do-it.html Shih YY, De La Garza BH, Huang S, Li G, Wang L, Duong TQ. Comparison of retinal and cerebral blood flow between continuous arterial spin labeling MRI and fluorescent microsphere techniques. J Magn Reson Imaging 2013. In press. Gardiner SK, Ren R, Yang H, Fortune B, Burgoyne CF, Demirel S. A Method to Estimate the Amount of Neuroretinal Rim Tissue in Glaucoma: Comparison with Current Methods for Measuring Rim Area. Am J Ophthalmol 2013. In press. Sheppler CR, Lambert WE, Gardiner SK, Becker TM, Mansberger SL. Predicting Adherence to Diabetic Eye Exams: Development of the Compliance with Annual Diabetic Eye Exams Survey. Ophthalmology. In press. Abbott CJ, Choe TE, Lusardi TA, Burgoyne CF, Wang L, Fortune B. Evaluation of retinal nerve fiber layer thickness and axonal transport 1- and 2-weeks after 8-hours of acute intraocular pressure elevation in rats. Invest Ophthalmol Vis Sci. 2013. In press. Levy-Clarke G, Jabs DA, Read RW, Rosenbaum JT, Vitale A, Van Gelder RN. Expert Panel Recommendations for the use of AntiTumor Necrosis Factor Biologic Agents in Patients with Ocular Inflammatory Disorders. Ophthalmology. 2013 Dec 17. pii: S01616420(13)00893-2. doi:10.1016/j.ophtha.2013.09.048. [Epub ahead of print] Artornsombudh P, Pistilli M, Foster CS, Pujari SS, Gangaputra SS, Jabs DA, Levy-Clarke GA, Nussenblatt RB, Rosenbaum JT, Suhler EB, Thorne JE, Kempen JH. Factors Predictive of Remission of New-Onset Anterior Uveitis. Ophthalmology. 2014 Mar;121(3):778-84. doi: 10.1016/j.ophtha.2013.09.041. Epub 2013 Dec 15. Levin MH, Pistilli M, Daniel E, Gangaputra SS, Nussenblatt RB, Rosenbaum JT, Suhler EB, Thorne JE, Foster CS, Jabs DA, LevyClarke GA, Kempen JH; Incidence of Visual Improvement in Uveitis Cases with Visual Impairment Caused by Macular Edema. Systemic Immunosuppressive Therapy for Eye Diseases Cohort Study. Ophthalmology. 2013 Dec 11. pii: S0161-6420(13)00843-9. doi: 10.1016/j.ophtha.2013.09.023. [Epub ahead of print] Zhang Z, Liu Q, Leskov KS, Wu X, Duan J, Zhang GL, Hall M, Rosenbaum JT. Roscovitine suppresses CD4+ T cells and T cell-mediated experimental uveitis. PLoS One. 2013 Nov 18;8(11):e81154. doi: 10.1371/journal.pone.0081154. Erratum in: PLoS One. 2013;8(12). Huston RK, Markell AM, McCulley EA, Pathak M, Rogers SP, Sweeney SL, Dolphin NG, Gardiner SK. Decreasing Necrotizing Enterocolitis and Gastrointestinal Bleeding in the Neonatal Intensive Care Unit: the Role of Donor Human Milk and Exclusive Human Milk Diets in Infants <1500 Grams Birth Weight. Infant Child Adolesc Nutr 2014. In press. Ren R, Yang H, Gardiner SK, Fortune B, Hardin C, Demirel S, Burgoyne CF. Anterior Lamina Cribrosa Surface Depth, Age and Visual Field Sensitivity in the Portland Progression Project. Invest Ophthalmol Vis Sci 2014. In press. Gardiner SK, Swanson WH, Goren D, Mansberger SL, Demirel S. Assessment of the reliability of standard automated perimetry in regions of glaucomatous damage. Ophthalmology. 2014. In press. Rafael L. Furlanetto RL, De Moraes CG, Teng CC, Liebmann JM, Greenfield DS, Gardiner SK, Ritch R, Krupin T for the Low-pressure Glaucoma Treatment Study Group. Risk factors for Optic Disc Hemorrhage in the Low-pressure Glaucoma Treatment Study. Am J Ophthalmol. 2014. In press. Gritsiou Y, Hegsted DA, Schlesinger P, Gardiner SK, Gubler KD. A Retrospective Analysis of the Effectiveness of Low Molecular Weight Heparin for Venous Thromboembolism Prophylaxis in Trauma Patients. Am J Surg 2014. In press. He L, Yang H, Gardiner S, Williams G, Hardin C, Strouthidis NG, Fortune B, Burgoyne CF. Longitudinal Detection of Optic Nerve Head Changes by Spectral Domain Optical Coherence 9 Ali A, Ku JH, Suhler EB, Choi D, Rosenbaum JT. The course of retinal vasculitis. Br J Ophthalmol. 2014 Feb 7. doi: 10.1136/ bjophthalmol-2013-303443. [Epub ahead of print] PMID: 24511084 [PubMed — as supplied by publisher] 24342020. Wang L, Burgoyne CF, Cull G, Thompson S, Fortune B. Static blood flow autoregulation in the optic nerve head in normal and experimental glaucoma. Invest Ophthalmol Vis Sci. 2014 Feb 10;55(2):873-80 Yu J, Liang Y, Thompson S, Cull G, Wang L. Parametric transfer function analysis and modeling of blood flow autoregulation in the optic nerve head. Int J of Physiol, Pathophysiol and Pharmacol 2014;6(1): 13-22. He L, Ren R, Yang H, Hardin C, Reyes L, Reynaud J, Gardiner SK, Fortune B, Demirel S, Burgoyne CF. Anatomic vs Acquired Image Frame Sectoral Discordance in Spectral Domain Optical Coherence Tomography Minimum Rim Parameterization in the Portland Progression Project. PLoS One. First published on March 18, 2014, as doi:10.1371/journal.pone.0092225 http:// www.plosone.org/article/info%3Adoi%2F10.1371%2Fjournal. pone.0092225 Ren R, Yang H, Gardiner SK, Fortune B, Hardin C, Demirel S, Burgoyne CF. Anterior Lamina Cribrosa Surface Depth, Age, and Visual Field Sensitivity in the Portland Progression Project (P3 Study). IOVS 2014; 55: 1531-1539. DOI:10.1167/iovs.13-13382 Pasadhika S, Rosenbaum JT. Biologics. 2014 Feb 15;8:67-81. eCollection 2014. Update on the use of systemic biologic agents in the treatment of noninfectious uveitis.Ophthalmology. 2014 Mar;121(3):778-84. doi: 10.1016/j.ophtha.2013.09.041. Epub 2013 Dec 15. Keck KM, Choi D, Savage LM, Rosenbaum JT. Insights into uveitis in association with spondyloarthritis from a large patient survey. J Clin Rheumatol. 2014 Apr;20(3): 141-5. doi:10.1097/ RHU.0000000000000087. PMID: 24662555 [PubMed — in process]. Suhler EB, Lim LL, Beardsley RM, Giles TR, Pasadhika S, Lee ST, de Saint Sardos A, Butler NJ, Smith JR, Rosenbaum JT. Rituximab Therapy for Refractory Orbital Inflammation: Results of a Phase 1/2, Dose-Ranging, Randomized Clinical Trial. JAMA Ophthalmol. 2014 Mar 20. doi: 10.1001/jamaophthalmol.2013.8179. [Epub ahead of print.] Miller LD, Gardiner SK, Gubler KD. Emergency Department Referral for Organ Donation: More Organ Donors and More Organs per Donor. Am J Surg 2014. In press. Gardiner SK. Effect of a Variability-Adjusted Algorithm on the Efficiency of Perimetric Testing. Invest Ophthalmol Vis Sci 2014. In press. Kinast RM, Barker GT, Day SH, Gardiner SK, Mansberger SL. Factors related to online patient satisfaction with ophthal mologists. Ophthalmology 2014. In press. Fortune B, Reynaud J, Cull G, Burgoyne CF, Wang L. The effect of age on optic nerve axon counts, SDOCT scan quality and peripapillary retinal nerve fiber layer thickness measurements in rhesus monkeys. Translational Vision Science & Technology. 2014. In press. Honors and awards Jim Rosenbaum, M.D., was honored by the American College of Rheumatology with its Distinguished Clinician Scholar Award. The award was presented at the annual meeting of the ACR. One honoree is selected per year. This award is considered one of the highest honors from the ACR. He is the first Oregonian to receive the award. The honor was given for his career-long efforts to understand the relationship between inflammation in and around the eye and inflammation elsewhere in the body. San Diego, Calif., Oct. 26, 2013 Jim Rosenbaum, M.D. — The Rosenbaum lab has received funding from Auventx Pharmaceuticals to study a novel topical approach to treating uveitis in an animal model. Steven L. Mansberger, M.D., MPH, received two awards in November 2013 “Best Doctors in America, 2014” and the American Academy of Ophthalmology, State Society Award, “Free glaucoma screenings with your legislator.” Steven L. Mansberger, M.D., MPH, was added as an executive editor in epidemiology for the American Journal of Ophthalmology. November 2013. Steven L. Mansberger, M.D., MPH, was named a Scientific Advisor for the Glaucoma Research Foundation to review research grants. November 2013. Steven L. Mansberger, M.D., MPH, has been appointed a member of the Academy’s EyeNet Editorial Advisory Board. Steven L. Mansberger, M.D., MPH, was named to Good Samaritan Foundation Board of Directors. Steven L. Mansberger, M.D., MPH, has been appointed as a consultant for the American Academy of Ophthalmology Preferred Practice Pattern-Glaucoma Panel. Steven L. Mansberger, M.D., MPH, was invited by the American Board of Ophthalmology (ABO) to be part of their eightmember Exam Development Committee. This committee writes questions for the written oral board examinations for ophthalmologists. Steven L. Mansberger, M.D., MPH, was named Affiliate Professor of Ophthalmology at Oregon Health & Science University (OHSU). continues on page 10 The Vision ~ Summer 2014 Tomography in Early Experimental Glaucoma. Invest Ophthalmol Vis Sci 2014; 55:574-586. The Vision ~ Summer 2014 10 Honors and awards (continued) Brad Fortune, O.D., Ph.D., began a three-year term of service in December 2013 to the Legacy Research Institute Institutional Animal Care and Use Committee (IACUC). Brad Fortune, O.D., Ph.D., will serve again this year on the Program Committee for the 2014 ARVO-ISIE Conference (International Society for Imaging in the Eye). Stuart Gardiner, Ph.D., received the 2014 Bernard Schwartz Memorial Award, along with a $500 travel grant for presenting a paper at the American Glaucoma Society meeting in Washington, D.C., on March 1: “Assessment of the Reliability of Standard Automated Perimetry in Regions of Glaucomatous Damage.” Michael Straiko, M.D., was interviewed by the ASCRS Eye World publication for their feature story: “DMEK experts offer pearls, pitfalls for performing procedure.” It is in the February issue of Eye World. Lin Wang, M.D. In April, the National Eye Institute (1R21EY02443201 NEI/NIH) and the BrightFocus Foundation (G2014059) awarded Dr. Wang grants to develop equipment, establish techniques (NEI/NIH) and characterize (BrightFocus Foundation) the role of astrocytes in blood flow autoregulation as part of the disease mechanism within glaucoma. The project period for both is from spring 2014 to 2016, with a combined total amount of $503,750. Invited lectures Jim Rosenbaum, M.D., SpondyloArthritis Research and Treatment Network meeting and lectured on the microbiome. San Francisco, Calif. September 2013. Jim Rosenbaum, M.D., visiting faculty member lectured to the division rheumatology. University of Chicago, Chicago, Ill., Sept. 10, 2013. Jim Rosenbaum, M.D., delivered the Alta lecture at the University of California on Dec. 5, 2013, in San Francisco, Calif. Jim Rosenbaum, M.D., as a visiting professor delivered two lectures at the Bascom Palmer Eye Institute on Dec. 16, 2013, in Miami, Fla. Jim Rosenbaum, M.D., lectured on “Cytokines and the Immunopathology of Uveitis” at the meeting of the International Ocular Immunology Society on Feb. 27, 2014, in Valencia, Spain. Jim Rosenbaum, M.D., lectured to the University of Pittsburgh Medical Center, Division of Rheumatology on “Eye Disease for Rheumatologists.” March 7, 2014. Jim Rosenbaum, M.D., was a speaker and panelist for the Cleveland Clinic Uveitis Update and spoke on “Laboratory testing to evaluate patients with uveitis.” March 8, 2014. Jim Rosenbaum, M.D., served on two separate National Eye Institute (NIH) review panels: one to evaluate core grants and the other to evaluate career development awards. March 10, 2014. Jim Rosenbaum, M.D., was a panelist in Las Vegas for Retina Today to discuss the use of local and systematic corticosteroids for uveitis and retinal diseases. March 15, 2014. Jim Rosenbaum, M.D., chaired a session for the World Ophthalmology Congress on infection and inflammation, and lectured on HLA B27, the microbiome, and uveitis. Tokyo, Japan. April 5, 2014. Jim Rosenbaum, M.D., was a guest of the Japanese Ophthalmological Society and spoke on S10018/A49, an endogenous TLR4 ligand, and its role in uveitis on April 5, 2014. Claude Burgoyne, M.D., FDA meeting with Gerhard Zinser, Ph.D., president of Heidelberg Engineering, in support of the Heidelberg Spectralis Normative Database. Aug. 27, 2013. Jim Rosenbaum, M.D., DGRh-Kongress — German rheumatology annual meeting, lectured at the meeting via the Internet. Heidelberg, Germany. Sept. 19, 2013. Claude Burgoyne, M.D., Swedish Glaucoma Society Annual meeting: Keynote Lecture: co-delivered via the Internet with Bal Chauhan, Ph.D.: “Paradigm Change to the Clinical Assessment of the Optic Nerve Head.” Stockholm, Sweden. September 19, 2013. Jim Rosenbaum, M.D., Rheumatology Invitational Educational Series (BRIESE). Invited speaker: the lectures were either on the microbiome or the intersection between rheumatology and ophthalmology. British Columbia. Sept. 27–28, 2013. Claude Burgoyne, M.D., Legacy Devers Eye Institute’s Thorny Issues in Ophthalmology: Climate Change conference. Lecture entitled: “Cup to Disc Ratio — Soon to be extinct?” Portland, Ore. Sept. 20, 2013. Jim Rosenbaum, M.D., was an invited guest at Allergan’s Inflammation and Ocular Surface Focus Group. Hamburg, Germany. Oct. 25, 2013 Claude Burgoyne, M.D., International Society for Eye Research (ISER), Keynote Lecture: “Optic Nerve Head Connective Tissue Deformation, Disorganization and Remodeling in Early Monkey Experimental Glaucoma — Implications for Mechanisms.” Saratosa, Fla. Sept. 29–Oct. 2, 2013. Jim Rosenbaum, M.D., was honored by the University of Toronto as the Inman Lecturer. He gave four lectures on the interface between rheumatology and ophthalmology. Toronto, Canada. November 2013. Claude Burgoyne, M.D., Optometric Glaucoma Society’s (OGS) 2013 Honoree at its 12th annual scientific meeting, two lectures: “The Death of Cup to Disc Ratio in Glaucoma — SDOCT Paradigm 11 Claude Burgoyne, M.D., Heidelberg Academy Glaucoma Faculty Inauguration at Moorfields Eye Hospital, three lectures: “Paradigm Change to the Clinical Assessment of the Optic Nerve Head in Glaucoma.”“Clinical Implications of Lamina Cribosa Deformation and Remodeling in Glaucoma.”“Optic Nerve Head Biomechanics and the Clinical Prediction of Susceptibility.” London, England. Oct. 29–30, 2013. Claude Burgoyne, M.D., gave two lectures at the American Academy of Ophthalmology (AAO) meeting, “Spotlight on OCT” Symposium: “Lessons from OCT Imaging of the Lamina Cribrosa.” Heidelberg Engineering Symposium: “Paradigm Change to the Clinical Assessment of the Optic Nerve Head in Glaucoma.” Nov. 17, 2013. New Orleans, La. Claude Burgoyne, M.D., ONHRL Presentation at the American Glaucoma Society Annual Meeting. “Variability of Glaucoma Specialists’ Rim Width Estimates and Their Accuracy Relative to Colocalized Spectral Domain Optical Coherence Tomography (SDOCT)” and “Glaucoma Neurodegeneration and Neurorescue Symposium — What Role Does Aging Play.” Feb. 28–March 1, 2014. Washington, D.C. Brad Fortune, O.D., Ph.D., attended the Glaucoma Progression (GPS) and North American Perimetry Society (NAPS) meetings. At the GPS meeting, Brad presented a talk entitled: “The effect of age on optic nerve axon counts, SDOCT scan quality and peripapillary retinal nerve fiber layer thickness measurements.” Chapel Hill, N.C. Oct. 1–4, 2013. Brad Fortune, O.D., Ph. D., “Axonopathy in Glaucoma: Implications for Diagnosis and Clinical Management.” Ezell Research Symposium, American Academy of Optometry. Seattle, Wash. Oct. 24, 2013. Brad Fortune, O.D., Ph.D., presented an invited lecture entitled “The effect of cytoskeletal changes on imaging,” at the third Optic Nerve Conference. Dec. 4–6, 2013, in Obergurgl, Austria (Tirolean Alps). Brad Fortune, O.D., Ph.D., gave three presentations and moderated one at the annual Association for Research in Vision and Ophthalmology (ARVO) meeting. Invited lecture during the Glaucoma Section Minisymposium: Symposium Title: “Mechanisms of Axonal Damage in Optic Nerve Disease.” Lecture title: “Imaging axonal transport and degeneration.” May 5, 2014. Invited lecture during the “Special Interest Group” (SIG) meeting: SIG Title: “Polarization-sensitive optical coherence tomography for retinal imaging: What needs to be done to transfer the technology from the laboratory to the clinic?” Lecture title: “Early stage axonal cytoskeletal damage detected in vivo by polarization-sensitive imaging in experimental glaucoma.” May 5, 2014. Session moderator for the glaucoma talks session called “Visual Fields and Visual Function.” May 6, 2014. Primary ARVO abstract presentation title: “Evidence of axonopathy during early-stage experimental glaucoma: relationship between in vivo imaging and histological findings.” May 6, 2014. Michael Straiko, M.D., keynote address at ASETCIRC meeting. Seville, Spain. September 2013. Michael Straiko, M.D., Cornea Society meeting. “Reducing complications in DMEK using a novel glass injector for simplified tissue delivery.” New Orleans, La. November 2013. Michael Straiko, M.D., Cornea Society meeting. “Eliminating the Possibility of Upside-Down DMEK Grafts: A Novel Stromal Side S-stamp Technique for DMEK.” New Orleans, La. November 2013. Michael Straiko, M.D., American Academy of Ophthalmology. “Keratoconus in Patients With Fuchs Endothelial Dystrophy Unmasked by Descemet Membrane Endothelial Keratoplasty.” New Orleans, La. November 2013. Michael Straiko, M.D., was an invited speaker at the “Kaiser Permanente Northwest Ocular Pathology 2014 Winter Conference.” He lectured on corneal ectasia diagnosis and management options. The talk focused heavily on the collagen cross linking study he is conducting at Devers. Michael Straiko, M.D., was an invited speaker at the Cleveland Clinic Cole Eye Institute Cornea Summit in Orlando, Fla. He lectured on DMEK techniques. Michael Straiko, M.D., was invited as the keynote speaker at the Philips Eye Institute in Minneapolis for their annual conference. He lectured on a variety of corneal topics. Steven L. Mansberger, M.D., MPH, gave two lectures: “The Great Debate in Glaucoma: For Cataract and Glaucoma Controlled on Medication, I prefer Cataract Surgery” and “Trabeculectomy: How to maximize your success.” Didactic course. American Academy of Ophthalmology. New Orleans, La. November 2013. Steven L. Mansberger, M.D., MPH, gave the President’s Lecture at the Optometric Glaucoma Society Meeting. Cheri Stowell, Ph.D., ONHRL Presentations at the American Glaucoma Society Annual Meeting. “Decrease in Myelin Proteins in the Optic Nerve Head and Optic Nerve in Non-human Primate Early Experimental Glaucoma.” Washington, D.C. Feb. 28–March 1, 2014. Camila Zangalli, M.D., “Comparison of Spectral Domain Optical Coherence Tomography Deep Optic Nerve Head Imaging to Co-localized 3-D Histomorphometry.” Washington, D.C. Feb. 28–March 1, 2014. Tammy Martin, Ph.D., was invited to chair the pre-ARVO American Uveitis Society spring meeting. May 3, 2014. The Vision ~ Summer 2014 Change and its Clinical Implications.”“Onset to Endstage — 20 years of Monkey Experimental Glaucoma.” Seattle, Wash. Oct. 22–23, 2013. Legacy Good Samaritan Medical Center Legacy Devers Eye Institute 1015 N.W. 22nd Ave. Portland, OR 97210 Editors: Steven L. Mansberger, M.D., MPH, Emily P. Jones, M.D., Carly M. Carcione, B.S., Dana Lord Call 503-413-8203 with your questions or comments. Our legacy is yours. Legacy Health strives to make responsible printing and paper choices that minimize our effect on natural resources. The Vision Patient referrals Legacy Devers Eye Institute subspecialty services: cornea, glaucoma, neuro-ophthalmology, oculo plastics and retina Good Samaritan Building 2, second floor 1040 N.W. 22nd Ave., Suite 200, Portland, OR 97210 503-413-8202 Legacy Devers Eye Institute–Memorial Eye Clinic Good Samaritan Building 2, first floor 1040 N.W. 22nd Ave., Suite 168, Portland, OR 97210 503-413-7022 Legacy Devers Eye Institute — Vision Rehabilitation Services Good Samaritan Building 2, second floor 1040 N.W. 22nd Ave., Suite 200, Portland, OR 97210 503-413-8498 Legacy Devers Eye Institute–Emanuel Medical Office Building 3, third floor 300 N. Graham St., Suite 300, Portland, OR 97227 503-413-3030 www.legacyhealth.org/devers DEV-4199 ©2014 Legacy Devers Eye Institute clinicians Neuro-Ophthalmology — 503-413-8015 Contact lenses — 503-413-7022 Jennifer Prunty, O.D. Julie Falardeau, M.D. Karen Rice, O.D. Ophthalmic ancillary services — Cornea — 503-413-6223 503-413-7022 Michael D. Straiko, M.D. Brad Fortune, O.D., Ph.D., electro Mark A. Terry, M.D. physiology Sirichai Pasadhika, M.D. General eye care — 503-413-7022 Ophthalmic plastic and Blake Acohido, M.D. reconstructive surgery — 503-413-8015 Ashley Hayden, M.D. Eric Jones, M.D. John Ng, M.D. Shari Katz, M.A. Eric Steele, M.D. Robert M. Kinast, M.D. Retina — 503-413-7022 Jennifer Prunty, O.D. Sirichai Pasadhika, M.D. Karen Rice, O.D. Elizabeth Verner-Cole, M.D. Glaucoma — 503-413-6453 Uveitis — 503-413-7022 Claude Burgoyne, M.D. Sirichai Pasadhika, M.D. Emily P. Jones, M.D. James T. Rosenbaum, M.D. Robert M. Kinast, M.D. Steven L. Mansberger, M.D., MPH