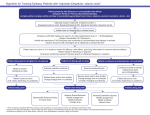
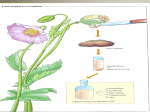
* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download a55f476935070a0
Pharmacognosy wikipedia , lookup
Lithium (medication) wikipedia , lookup
Adherence (medicine) wikipedia , lookup
Discovery and development of cyclooxygenase 2 inhibitors wikipedia , lookup
Drug design wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Drug discovery wikipedia , lookup
Discovery and development of direct thrombin inhibitors wikipedia , lookup
Dextropropoxyphene wikipedia , lookup
Discovery and development of proton pump inhibitors wikipedia , lookup
Prescription costs wikipedia , lookup
Neuropharmacology wikipedia , lookup
Plateau principle wikipedia , lookup
Drug interaction wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Theralizumab wikipedia , lookup
Dydrogesterone wikipedia , lookup
College of Pharmacy UQU UNIVERSITY Vancomycin Vancomycin is an antibiotic with grampositive spectrum of activity that is effective in treatment of nafcillin or Methicillin Resistant Staphy-lococcus aureus ( NRSA or MRSA ) . it is also an alternative to penicillin in patients , Vancomycin is bactericidal for most gram-positive organism, except against enterococci and it is synergistic with gentamicin against most strain of S. aureus and enterococci it is not effective gram-negative bacteria. Vancomycin is poorly absorbed orally and has been used to treat gastrointestinal overgrowths of gram-positive bacteria when used to treat systemic infection , vancomycin must be given by the IV route for those patients receiving continuous ambulatory peritoneal dialysis the usual dose , in patients with normal renal function is 1g ( 10 to 15 mg/kg ) over 60 minutes every 8 to 12 hours . Drug Name ( generic ) Vancomycin Class / Therapeutic Category Antibiotic Cell wall biosynthesis Action inhibition PG synthesis by binding directly to the D-Ala - D- Ala end of the peptide , forms a cap over the end of the chain , blocks cross linking Pharmacokinetics ● Vancomycin is poorly absorbed from the intestinal tract ● The drug is widely distributed in the body. Cerebrospinal fluid levels 7– 30% of serum concentrations ● Metabolism Excreted unchanged <3% ● percent of the drug is excreted by glomerular filtration. ● The drug has a serum elimination half-life of about 6 hours. Factor affecting Pharmacokinetic ● Age ● Gender ● Body Weight. Indications For the treatment of serious or severe infections caused by susceptible strains of methicillin-resistant (beta-lactam-resistant) staphylococci. Contraindication / precautions ● Poisoning by Antibiotic Vancomycin ● Hearing Problem ● Kidney Disease ● Clostridium difficile colitis ● systemic mastocytosis ● Decreased Neutrophils a Type of White Blood Cell Adverse Reaction Interactions The most common adverse reactions (≥ 10%) were nausea (17%), abdominal pain (15%), and hypokalemia (13%). Dosing Information Based on Total Body weight and renal function (15 - 20 mg/kg ) Monitoring ● 10 – 15 mcg/mL: bacteremia, skin and soft tissue infections ● 15 – 20 mcg/mL: osteomyelitis, meningitis, pneumonia Overdose ● Ototoxicity ● nephrotoxicity. ● “red man” or “red neck” syndrome College of Pharmacy UQU UNIVERSITY Digoxin Digoxin is an inotropic agent primarily used to treat CHF and atrial fibrillation. It is incompletely absorbed and once absorbed a substantial fraction is cleared by kidneys . in the acute care seting historically digoxin loading dose of = 1 mg/70 kg were administered before the initiation of the usual maintenance dose were from an era when target levels were 1 to 2 mcg/L and probably tody doses of approximately one half would be more common in patients with heart failure Because it has a relatively long elimination half life in adults , Digoxin is given once daily. Dosage adjustments can be important for patients who are being converted from parenteral to oral therapy patients with renal impairment CHF or thyroid abnormalities or patients who take amiodarone concurrently Drug Name ( generic ) Digoxin Class / Therapeutic Category Cardiac Glycosides Action Digoxin inhibits the Na-K-ATPase membrane pump, resulting in an increase in intracellular sodium. The sodium calcium exchanger (NCX)in turn tries to extrude the sodium and in so doing, pumps in more calcium. Increased intracellular concentrations of calcium may promote activation of contractile proteins (e.g., actin, myosin). Digoxin also acts on the electrical activity of the heart, increasing the slope of phase 4 depolarization, shortening the action potential duration, and decreasing the maximal diastolic potential. Pharmacokinetics ● Absorption 80 % absorbed after oral administration of (tablets 75-80 % absorbed) after administration of (elixir 75-80 % absorbed from liquid filled) (capsule 80 % absorbed) IM but not recommended ● Distribution Bound tightly to muscles tissues Vd Correlated well with lean body Tissues , very large distribution volume Vd = 7.3 L/kg x IBW ● metabolism via stepwise cleavage of the sugar moieties and lactone ring reduction Less than 10 % undergoes hepatic metabolism not dependent of the cytochrome P450 system a ● Elimination follows first-order kinetics 50-70% is excreted almost entirely unchanged by the kidney Affected by some drugs interactions & diseases conditions Half life 3648 hours and increase in case of renal impairment Elimination Factor affecting Pharmacokinetic ● Age ● Gender ● Body Weight. Indications For the treatment of congestive heart failure and atrial fibrillation Contraindication / precautions ● Digoxin toxicity ● Advanced A-V block without pacemaker ● Bradycardia or sick sinus without PM ● PVC’s and VT ● Marked hypokalemia ● W-P-W with atrial fibrillation Adverse Reaction Interactions ● Amiodarone ● Propafenone ● Quinidine ● Ritonavir Dosing Information Loading Dose ( 1.0 to 1.5 mg/ 70kg ) Maintenance dose ( ( 0.25 mg/kg ) Monitoring obtain level within 24 hours of digitalization weekly until stable, and at steady state , Measure every two days, or every day in unstable renal function Overdose ● anorexia ● nausea ● Vomiting ● visual changes and cardiac arrhythmias College of Pharmacy UQU UNIVERSITY Valproic Acid Valproic acid is currently used to treat various seizure disorder and variety of psychiatric such as anxiety , depression and other behavioral disturbances the mechanism of action for valproic acid is uncertain , the usual initial dose of valproic acid for treatment seizure is 15mg/kg/day and the usual starting dose of valproic acid is 25mg/kg/day , the metabolism of phenobarbital and the major metabolite of carbamazepine appear to be inhibited by valproic acid Drug Name ( generic ) Valproic Acid Class / Therapeutic Category Antiepileptic Action It purportedly increase the brain concentration of gamma aminobutyric acid (GABA) , an inhibitory neurotransmitter in the central nervous system Pharmacokinetics ● Rapid absorption from gastrointestinal tract ● Distribution 11 L/1.73 m2 [total valproate] 92 L/1.73 m2 [free valproate] ● Valproate is metabolized almost entirely by the liver ● Valproic acid is almost entirely eliminated from the body through hepatic metabolism less than 5% of the drug is eliminated by the renal route Factor affecting Pharmacokinetic ● Age ● Gender ● Body Weight. Indications For treatment and management of seizure disorders, mania, and prophylactic treatment of migraine headache. In epileptics, valproic acid is used to control absence seizures, tonic-clonic seizures (grand mal), complex partial seizures, and the seizures associated with Lennox-Gastaut syndrome. Contraindication / precautions ● hepatic disease ● mitochondrial disorders caused by mutations in mitochondrial DNA polymerase ● hypersensitivity to the drug ● urea cycle disorders Adverse Reaction Interactions ● Rifampin ● Felbamate ● Carbapenem Antibiotics ● Aspirin Dosing Information ● Complex partial seizures: Initial dose: 10 to 15 mg/kg Maintenance dose: 10 to 60 mg/kg ● Simple and complex absence seizures: Initial dose: 15 mg/kg Monitoring ● General: Patients receiving doses near the maximum recommended daily dose should be monitored more closely. ● Hematologic: Platelet counts ● Hepatic: Liver function tests ● Nervous system: Seizures ● Psychiatric: Emergence or worsening of depression, suicidal thoughts or behavior, and/or unusual changes in mood or behavior Overdose ● heart block ● deep coma ● hypernatremia ● Fatalities College of Pharmacy UQU UNIVERSITY Phenobarbital Phenobarbital is a long acting barbiturate used in the treatment of seizure disorder , insomnia and anxiety. Ti is most commonly administered orally may it administered IM , IV as well. The usual adult maintenance dose of 2 mg/kg/day produced steady state concentrations of approximately 20 mg/L. It has half life of approximately 5 days a loading dose of 15 mg/kg can be administered, usually in three divided doses of 5 mg/kg given every 2 to 3 hours Drug Name ( generic ) Phenobarbital Class / Therapeutic Category Anticonvulsant Action Pharmacokinetics Chloride Channel opener (Gaba operated) ● ABSORPTION - Oral bioavailability: 100% - Oral Tmax: 4-12 hours. (absorption rate depends on food and on pharmaceutical preparation) ● DISTRIBUTION - Bound in plasma: » 50% - Vd (70 Kg): » 40 L - Bound and free drug concentrations in brain are equal to those in plasma ● METABOLISM- 75% by the liver (biotransformation rate is low) ● EXCRETION - By the kidney: 25% (acid urine) up to 75% (in alkaline urine) Total Clearance: » 4.5 mL/min(70 Kg) Half-life: adults: » 100 hours children: » 50 hours Factor affecting Pharmacokinetic ● Age ● Gender ● Body Weight. Indications is a central nervous system depressant. In ordinary doses, the drug acts as a sedative and anticonvulsant. Its onset of action occurs within 30 minutes, and the duration of action ranges from 5 to 6 hours. It is detoxified in the liver. Contraindication / precautions ● Absence seizures, myoclonic seizures, atonic seizures ● Porphyria (acute intermittent, variegata) ● Previous history of serious allergic reactions to barbiturates ● Serious respiratory or liver diseases ● Patients with severe pain Pregnancy Adverse Reaction Interactions ● Griseofulvin ● Phenytoin, Valproic Acid ● Doxycycline ● Corticosteroids ● CNS Depressants Dosing Information The most commonly recommended dose in dogs is 2-3 mg phenobarbital per kilogram of body weight given every 12 hours Monitoring Phenobarbital serum concentrations (as clinically indicated); CNS status; liver enzymes (periodic); CBC with differential (periodic); renal function (periodic); seizure activity; signs and symptoms of suicidality (eg, anxiety, depression, behavior changes) IV use: Respiratory rate, heart rate, blood pressure, IV site (stop injection if patient complains of pain in the limb) Overdose The signs and symptoms of barbiturate poisoning are referable especially to the central nervous system and the cardiovascular system. but late in the course of barbiturate poisoning they may show hypoxic paralytic dilatation. Respiration is affected early. Breathing may be either slow or rapid and shallow; Cheyne-Stokes rhythm may be present. College of Pharmacy UQU UNIVERSITY Lithium Lithium is a monovalent cation that has been used ofr more than 50 years in the treatment and prevention of various psychiatric conditions , lithium salts have been prescribed to prevent future manic or depressive episodes , lithium is administered as the carbonate salt formulation which contains 8.12 mEq of lithium pre 300mg tablet or capsule and it is available as extended release the usual daily dose range from 600 to 1,500 mg Drug Name ( generic ) Lithium Class / Therapeutic Category Psychotropic Drugs Action Preclinical studies have shown that lithium alters sodium transport in nerve and muscle cells and effects a shift toward intraneuronal metabolism of catecholamines, but the specific biochemical mechanism of lithium action in mania is unknown. Pharmacokinetics The digestive absorption of lithium is complete and the maximum plasma concentration is observed two to four hours after an oral intake of a non sustained release form. The average plasma half-life of lithium is about 22 hours. Its plasma level at steady state regarded as therapeutically effective ranges from 0.5 to 0. 8 mmol/L. When blood sampling is performed in the morning before the first daily intake or in the evening before the single intake of a sustained-release formulation the plasma level should be between 0.8 and 1.2 mmol/liter. Its volume of distribution is close to 0.8 L/kg corresponding to a very broad distribution, approximately equal to that of total water. Although lithium is not bound to plasma proteins, its transfer into the brain and the cerebrospinal fluid is slow, and at equilibrium, the cerebrospinal fluid contains approximately 40% of the plasma concentration. The elimination is more than 95% urinary and any renal impairment delays it. Approximately 80% of lithium filtered by the glomerulus is reabsorbed from the proximal tubule; its clearance is approximately 20% of that of creatinine. A decrease of sodium intake increases lithium retention by the kidney and conversely. Thiazide diuretics, nonsteroidal antiinflammatory drugs, ACE inhibitors reduce its renal elimination and increase its plasma concentratio Factor affecting Pharmacokinetic ● Age ● Gender ● Body Weight. Indications Lithium carbonate is indicated in the treatment of manic episodes of manicdepressive illness. Maintenance therapy prevents or diminishes the intensity of subsequent episodes in those manicdepressive patients with a history of mania. Contraindication / precautions ● Dysfunction of the Brain ● Brugada Syndrome ● Abnormal Heart Rhythm ● Chronic Heart Failure ● Kidney Disease ● Excess Urination ● Pregnancy Adverse Reaction Interactions Convulsions, Cardiac arrhythmias, Cardiac arrhythmias, Dehydration, Hypercalcemia, Sinus bradycardia, Hyperthyroidism, Leukocytosis, Dysarthria. Dosing Information The usual daily dose range from 600 to 1,500 mg because lithium possesses a relatively narrow therapeutic range and exhibits fairly predictable pharmacokinetic behavior , it serves as an excellent candidate for routine therapeutic drug monitoring Monitoring To insure proper AND safe administration of phenobarbital, it is very important to monitor the level in the blood. Overdose ● Central Nervous System: blackout spells, epileptiform seizures, slurred speech, dizziness. ● Cardiovascular: cardiac arrhythmia, hypotension, peripheral circulatory collapse. ● Gastrointestinal: anorexia, nausea, vomiting, glycosuria. College of Pharmacy UQU UNIVERSITY Carbamazepine Is an anticonvulsant compound that is structurally similar to the tricyclic antidepressant agents it is the drug of choice for treatment of trigeminal neuralgia and used for seizure and also for pain syndromes , Carbamazepine is available in many dosage forms including oral , chewable tablet , oral tablet . it is labeled use in adults and children . it ia in pregnancy class D , effective doses for adults with seizure disorder are the range of 15 to 25 mg/kg/day or 800 to 1200 mg/day at steady state and it is eliminated primairly by the metabolic route by the P450 , less than 2% of carbazepine is excreted uncahnged in the urine Drug Name ( generic ) Carbamazepine Class / Therapeutic Category Anticonvulsants decreasing nerve impulses that cause Action Pharmacokinetics seizures and pain ● Absorption: ● VD: 0.7 to 2.7 L/kg ● Pb: 60-80% ● Metabolism: Primarily hepatic ● Route of Elimination : by kidney. ● Cl: 0.64 +/- 0.18 L/min ● Half-life:109 mins Factor affecting Pharmacokinetic age of the patients and total daily dose Indications For the treatment of epilepsy and pain associated with true trigeminal neuralgia. Contraindication / precautions ● Hypersensitivity to this drug or tricyclic antidepressants ● History of bone marrow suppression ● MAO inhibitor use within 14 days Use with caution Adverse Reaction Interactions Atracurium, Cisatracturium, Pancuronium, Vecuronium: May decrease the effects of nondepolarizating muscle relaxant, causing it to be less-effective Dosing Information ● Adults and Children Over 12 Years of Age: Initial: 200 mg b.i.d. Increase at weekly intervals by adding up to 200 mg/day using a t.i.d. or q.i.d. regimen until the optimal response is obtained. Dosage generally should not exceed 1000 mg daily in children 12 to 15 years of age, and 1200 mg daily in patients above 15 years of age. Doses up to 1600 mg daily have been used in adults in rare instances. Maintenance: Adjust dosage to the minimum effective level, usually 800 to 1200 mg daily. ● Children 6 to 12 Years of Age: Initial: 100 mg b.i.d. Increase at weekly intervals by adding up to 100 mg/day using a t.i.d. or q.i.d. regimen until the optimal response is obtained. Dosage generally should not exceed 1000 mg daily. Maintenance: Adjust dosage to the minimum effective level, usually 400 to 800 mg daily. Monitoring Patients should be monitored for concrelated side effects: ● Nausea ● vomiting ● lethargy ● dizziness Overdose ● Respiration: Irregular breathing, respiratory depression. ● Gastrointestinal Tract: Nausea, vomiting. ● Kidneys and Bladder: Anuria College of Pharmacy UQU UNIVERSITY Lidocaine Is local anesthetic agent with antiarrhythmic it is used for acute treatment of severe ventricular arrhythmias and is one of the most common agents for the acute treatment of ventricular arrhythmias , also used for neonatal seizures that do not respond to conventional anticonvulsants , maintain lidocaine levels at 3 to 6 mg/L for seizure control or <9 mg/L to minimize potential cardiac toxicity , and it is poor oral bioavailability is almost exclusively metabolized by liver and has short action for these reasons administered initially as bolus dose followed by continuous infusion . Drug Name ( generic ) Lidocaine Class / Therapeutic Category Analgesics and Anesthetics Action stabilizing the neuronal membrane Pharmacokinetics ● Absorption : completely absorbed following parenteral administration ● Distribution (VD) : 0.7 to 2.7 L/kg [healthy volunteers] ● Metabolism : by hepatic ● Elimination : Lidocaine and its metabolites are excreted by the kidneys. Factor affecting Pharmacokinetic Hepatic metabolism mainly by CYP3A4 Indications For production of local or regional anesthesia by infiltration techniques such as percutaneous injection and intravenous regional anesthesia by peripheral nerve block techniques such as brachial plexus Contraindication / precautions ● Bradycardia ● Accelerated idioventricular rhythm ● Pacemaker ● Porphyria, especially acute porphyria (AIP); Adverse Reaction Interactions ● arbutamine ● bupropion ● dofetilide ● GenESA (arbutamine) Dosing Information 1-1.5 mg/kg followed by continuous infusion 1-9 mg/min Monitoring there may be a desire to maintain lidocaine levels at 3 to 6 mg/L for seizure control or <9 mg/ L to minimise potential cardiac toxicity .Lidocaine has poor oral bioavailability , is almost exclusively metabolised by the liver , and has a relatively short duration of action . For these reasons , lidocaine is almost always administered initially as a bolus dose of 1 to 1.5 mg\kg, followed by a continuous infusion of approximately 1 to 4 mg/min . Overdose ● Hypoxia ● acidosis ● bradycardia ● Arrhythmias ● cardiac arrest College of Pharmacy UQU UNIVERSITY Ethosuximide Is an anticonvulsant used primarily for the treatment of uncomplicated absence seizure it is available as 250 mg capsule and as solution containing 250 mg of ethosuximide per 5 mL and is eliminated primarily by metabolism to an inactive hydroxyethyl metabolite which excreted in urine as the glucuronide approximately 20% of unchanged . the usual dosage range 15 - 30 mg/kg/day , maintenance dose of 15 - 40 mg/kg/day , divided into two daily doses given every 12 hours Drug Name ( generic ) Ethosuximide Class / Therapeutic Category Succinimide anticonvulsants Action reducing low threshold Ca2+ channel current (T-type channel) in thalamus At high concentrations: Inhibits Na+/K+ ATPase Depresses cerebral metabolic rate Potentiates GABA Pharmacokinetics ● Bioavailability :93% . ● VD :0.7 l/kg . ● metabolism: Hepatic, via CYP3A4 and CYP2E1. ● CL:17-38%. ● half-life: 53-56 hr. Factor affecting Pharmacokinetic ● Age ● Gender ● Body Weight. Indications Ethosuximide is indicated for the control of absence (petit mal) epilepsy. Contraindication / precautions Ethosuximide should not be used in patients with a history of hypersensitivity to succinimides. Adverse Reaction Interactions Dosing Information Monitoring gastrointestinal intolerance 20-30mg/kg/day, Available as syr./caps. Seizure frequency; trough serum concentrations, CBC, platelets, liver enzymes (periodic), urinalysis (periodic); signs of rash; suicidality (eg, suicidal thoughts, depression, behavioral changes) Overdose ● Drowsiness ● Headache ● Lethargy ● Dysequilibrium ● Unsteadiness College of Pharmacy UQU UNIVERSITY Theophylline Is a bronchial smooth muscle relaxant used to treat bronchial asthma and other diseases , is relegated to third line agent in the treatment of asthma , the low dose theophylline leading to concentrations of 5 -10 mg/L has anti inflammatory and immunomodulatory effect is poorly soluble in water about 1% and in the past usually administered by IV and it is slowly absorbed , aminophylline is the most widely used salt of theophylline , loading dose of 300 - 500 mg and is followed by IV infused and the usual oral maintenance dose is 200- 300 mg three to four times a day or 200 - 400 mg twice daily Drug Name ( generic ) Theophylline Class / Therapeutic Category bronchodilator Action Theophylline relaxes smooth muscles of respiratory tract and suppresses the response of the airways to stimuli, may increase tissue concentration of cyclic adenine monophosphate (cAMP) by inhibiting 2 isoenzymes of phosphodiesterase (PDE III and, to a lesser extent, PDE IV), which ultimately induces release of epinephrine from the adrenal medulla cells Pharmacokinetics ● Absorption: well oral absorption. ● Vd:0.45. ● Pb: 40-50%. ● Metabolism: Hepatic via demethylation (CYP 1A2) and hydroxylation (CYP 2E1 and 3A4) ● Elimination: in urine ● Half-life:8h Factor affecting Pharmacokinetic Smoking can affect the pharmacokinetics of the drugs by decreasing the half-life to 4 or 5 hours. Indications Theophylline is indicated for the treatment of the symptoms and reversible airflow obstruction associated with chronic asthma and other chronic lung diseases, e.g., emphysema and chronic bronchitis. Contraindication / precautions Theophylline (Anhydrous) Extended-Release Tablets are contraindicated in patients with a history of hypersensitivity to Theophylline or other components in the product. Adverse Reaction Interactions adding a drug that inhibits Theophylline metabolism (e.g., cimetidine, erythromycin, tacrine) or stopping a concurrently administered drug that enhances Theophylline metabolism (e.g., carbamazepine, rifampin). Dosing Information 10-15 mcg/mL Monitoring Monitor heart rate, CNS effects (insomnia, irritability); respiratory rate (COPD patients often have resting controlled respiratory rates in low 20s); arterial or capillary blood gases (if applicable) Overdose Adenosine receptors are widely distributed throughout the body. Antagonism of these receptors has both therapeutic and toxic effects, including: Bronchodilatation, Tachycardia, Cardiac arrhythmias, Seizures, Cerebral vasoconstriction. College of Pharmacy UQU UNIVERSITY Warfarin Drug Name ( generic ) Warfarin Class / Therapeutic Category Anticoagulants Action Interferes with hepatic synthesis of vitamin K-dependent coagulation factors (II, VII, IX, X) Pharmacokinetics ● Absorption : Rapidly absorbed following oral administration with considerable interindividual variations. Also absorbed percutaneously. ● Distribution (VD) : 0.14 L/kg ● Metabolism : by hepatic microsomal enzymes. S-warfarin is predominantly metabolized by cytochrome P450 ● Elimination : by metabolism. Very little warfarin is excreted unchanged in urine. The metabolites are principally excreted into the urine; and to a lesser extent into the bile. Factor affecting Pharmacokinetic ● Age ● Gender ● Body Weight. Indications For the treatment of retinal vascular occlusion, pulmonary embolism, cardiomyopathy, atrial fibrillation and flutter, cerebral embolism, transient cerebral ischaemia, arterial embolism and thrombosis. Contraindication / precautions ● Pregnancy ● Hemorrhagic tendencies or blood dyscrasias ● Bleeding tendencies ● Threatened abortion, eclampsia, and preeclampsia Adverse Reaction Interactions Dosing Information bivalirudin naproxen, oxaprozin venlafaxine, vilazodone aspirin The dosage and administration of Warfarin sodium tablets must be individualized for each patient according to the patient’s International Normalized Ratio (INR) response to the drug. Adjust the dose based on the patient’s INR and the condition being treated. Consult the latest evidence-based clinical practice guidelines regarding the duration and intensity of anticoagulation for the indicated conditions. Monitoring Prothrombin time, hematocrit; INR (frequency varies depending on INR stability); may consider genotyping of CYP2C9 and VKORC1 prior to initiation of therapy, if available Overdose Bleeding (e.g., appearance of blood in stools or urine, hematuria, excessive menstrual bleeding, melena, petechiae, excessive bruising or persistent oozing from superficial injuries, unexplained fall in hemoglobin) is a manifestation of excessive anticoagulation.