* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download SBRT: AAPM Task Group 101 Report
Backscatter X-ray wikipedia , lookup
Brachytherapy wikipedia , lookup
Positron emission tomography wikipedia , lookup
Proton therapy wikipedia , lookup
Radiation therapy wikipedia , lookup
Radiation burn wikipedia , lookup
Nuclear medicine wikipedia , lookup
Medical imaging wikipedia , lookup
Neutron capture therapy of cancer wikipedia , lookup
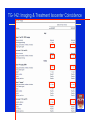
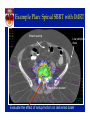
MEDİKAL FİZİK DERNEĞİ Stereotaktik Radyo Cerrahi ve Radyobiyoloji Kursu Istanbul, 20 Haziran 2014 SBRT: AAPM Task Group 101 Report Kamil M. Yenice, Ph.D. University of Chicago Department of Radiation Oncology An Introduction to the Recommendations for Physicists and Physicians from the AAPM Task Group No. 101….. Benedict, et al Medical Physics (2010) Major Topics Covered in TG101: 1. History and Rationale for SBRT 2. Current status of SBRT patient selection criteria 3. Simulation Imaging and Treatment Planning 4. Patient Positioning, Immobilization, Target localization, and Delivery 5. Special Dosimetry Considerations 6. Clinical Implementation of SBRT 7. Future Directions What is SBRT? • SBRT refers to the precise irradiation of an image defined extra-cranial lesion associated with the use of high radiation dose delivered in a small number of fractions. (NCAT-UK definition) • In SBRT, confidence in this accuracy is accomplished by the integration of modern imaging, simulation, treatment planning, and delivery technologies into all phases of the treatment process; from treatment simulation and planning, and continuing throughout beam delivery (TG 101) So What is SBRT? Image Guidance SBRT Stereotactic Radiosurgery Slide: Courtesy of Stanley H. Benedict, PhD IMRT and Conformal 3D Delivery Conventional RT vs. SBRT Characteristic Conventional RT SBRT Dose / Fraction 1.8 – 3 Gy 6 – 30 Gy No. of Fractions 10 – 30 1-5 Target definition CTV / PTV GTV / CTV / ITV/ PTV well-defined tumors: GTV=CTV Margin gross disease + clinical extension: tumor may not have a sharp boundary. Centimeters Millimeters (From Table 1: AAPM TG 101) Although SBRT employs similar basic principles as in conventional modalities including IMRT and IGRT, its extreme hypofractionated treatment delivery demands the utmost consideration for safety! Frame Based Immobilization and Localization Systems Frame systems provide a link between patient immobilization and localization: accurate localization relies on patient setup reproducibility. Assumption: variations in the stereotactic location of the target are due only to organ motion and not to setup uncertainties. Not true for most situations! Frame Based Immobilization and Localization Systems Frame systems provide a link between patient immobilization and localization: accurate localization relies on patient setup reproducibility. Assumption: variations in the stereotactic location of the target are due only to organ motion and not to setup uncertainties. Not true for most situations! Patient Positioning, Immobilization, Target Localization, and Delivery Recommendation (TG 101): • Body frames and fiducial systems are OK for immobilization and positioning aids • They shall NOT be used as a sole localization technique! Recommendations (TG 101) Targeting: For SBRT, image-guided localization techniques shall be used to guarantee the spatial accuracy of the delivered dose distribution with a high confidence level. The patient position should be monitored during the entire treatment and any deviations in treatment/target position as assessed from available visual, optical, and radiographic tools such as repeat imaging should be recorded for the entire treatment duration. IGRT Technology for SBRT Commissioning of a SRS Program “Quality and Safety Considerations in SRS and SBRT”, Solberg et al, Practical Rad Onc, 2011 SBRT Commissioning (I) • “Commissioning tests should be developed by the institution’s physics team to explore in detail every aspect of the system with the goal of developing a comprehensive baseline characterization of the performance of the system.” (TG-101) SBRT Commissioning (II) Quality Assurance of Radiation Therapy and The Challenges of Advanced Technologies Symposium (Supplement to IJROBP: 2008) • The modified Winston-Lutz test should be performed at the time any SBRT system is initially commissioned, and it should be repeated monthly. • All SBRT procedures should include detailed information on how the registration software is to be applied. • Special moving phantoms should be used to demonstrate that gating and/ or tracking techniques are accurate. Slide: Courtesy of Hania Al-Hallaq, PhD, Univ. of Chicago MiMi Phantom (Standard Imaging) Slide: Courtesy of Hania Al-Hallaq, PhD, Univ. of Chicago Slide: Courtesy of Hania Al-Hallaq, PhD, Univ. of Chicago Isocenter Coincidence Testing Bissonnette et al, Int J Rad Oncol Biol Phys, 71(1) S57–S61, 2008. MiMi Phantom Axial CT Scans Slide: Courtesy of Hania Al-Hallaq, PhD, Univ. of Chicago Center Phantom in MV Isocenter by Imaging at 4 Gantry Angles Slide: Courtesy of Hania Al-Hallaq, PhD, Univ. of Chicago Measure Offset to kV Isocenter by 2D/2D Match at 4 Angles Slide: Courtesy of Hania Al-Hallaq, PhD, Univ. of Chicago Measure Offset to CBCT Isocenter Slide: Courtesy of Hania Al-Hallaq, PhD, Univ. of Chicago Measure Offset to Laser Isocenter Slide: Courtesy of Hania Al-Hallaq, PhD, Univ. of Chicago Root Mean Square Distances of IGRT Isocenter Offsets Trial number Trilogy couch precision: a factor in larger offset values Slide: Courtesy of Hania Al-Hallaq, PhD, Univ. of Chicago TG-142: Imaging & Treatment Isocenter Coincidence Daily IGRT QA-Varian System UCMC Daily Imaging QA Distance Error Criterion: ≤ 1 mm (TrueBeam) ≤ 2mm (C-series) SBRT Planning Issues Simulation with Motion or Imaging Artifacts Recommendation: If target and/or critical structures cannot be localized accurately due to motion or metal artifacts…… STOP! Do NOT pursue SBRT as a treatment option! Respiratory Motion Management Recommendation: For thoracic and abdominal targets, a patient-specific tumor motion assessment is recommended. • Quantifies motion expected over respiratory cycle • Determines if techniques such as respiratory gating would be beneficial • Helps in defining margins for treatment planning • Allows compensation for temporal phase shifts between tumor motion and respiratory cycle SBRT Target Margins Recommendation: At the current time, it remains difficult to base target margins directly on clinical results. The adequacy of ICRU definitions depend on: • Understanding of how high absolute doses and sharp dose falloffs affect accuracy • Limitations on in-house localization uncertainty • Guidance from current peer-reviewed literature Make an effort to gather and analyze your own clinical results to improve margin design! Normal Tissue Tolerances Recommendation: Normal tissue dose tolerances in the context of SBRT are still evolving. So…. CAUTION! • If part of an IRB-approved phase 1 protocol, proceed carefully • Otherwise, the evolving peer-reviewed literature must be respected! Table of Normal Tissue Tolerances TG 101: Table 3 Table of Normal Tissue Tolerances • There is sparse long-term follow-up for SBRT. • Data in table 3 should be treated as a first approximation! • Doses are mostly unvalidated, but doses are based mostly on observation and theory. • There is some measure of educated guessing! R. Timmerman, 10/26/09, pers. comm. Biological Effects • NOT the same as traditional radiation therapy!!!! • Cannot extrapolate from the linear quadratic model!!!! Biological Dose Equivalents Total Physical Dose (Gy) NTD10 (Gy) Log10 Estimated 30 mo local NTD 3 Cell Kill progression-free (Gy) survival 30 x 2 = 60* (in 6 weeks) 65 9.9 17.7 % (w. repopulation) 60 35 x 2 = 70* (in 7 weeks) 72 10.9 28.4 % (w. repopulation) 70 4 x 12 = 48 83 12.6 78.9 % (no repopulation) 144 3 x 15 = 45 94 14.2 90.8 % (no repopulation) 162 5 x 12 = 60 110 16.7 97.1% (no repopulation) 180 3 x 20 = 60 150 22.7 >99% (no repopulation) 276 3 x 22 = 66 176 26.7 >99% (no repopulation) 330 * NTD = Normalized Tissue Doses estimated using an α/β of 10 (late) an 3 Gy (early) Quantitative Analyses of Normal Tissue Effects in the Clinic (QUANTEC Study) IJROBP Vol 76, No 3, Supplement (2010) Summary of SRS/SBRT Normal Tissue Tolerances SBRT Participation In Trials Recommendation: The most effective way to further the radiation oncology community’s SBRT knowledge base is through participation in formal group trials • Single- or multi- institution • Ideally NCI-sponsored or NCI-cooperative groups (e.g. RTOG) • If no formal trial, look to publications • If no publications, structure as internal clinical trial RTOG SBRT Protocols • 0631 Spine • 0813 and 0915 Lung • 0438 Liver Provide guidelines for treatment planning: Dose Prescription Target Coverage Dose Constraints Example Plan: Spinal SBRT with IMRT Bowel sparing Low peripheral dose Sharp dose gradient Evaluate the effect of setup/motion on delivered dose! Know the limitations of your dose algorithm! (Pay attention to warnings in user’s manual) This vendor safety notice warns against two specific issues for potential inaccurate dose computation due to: 1. Use of conditions that require extrapolation of data beyond measurement range 2. Use of large grid size resulting in unexpected results for small structures Recommendation (TG 101): SBRT commonly includes extremely high-dose gradients near the boundary of the target and often makes use of IMRT techniques. This report recommends the use of an isotropic grid size of 2 mm or finer. The use of grid sizes greater than 3 mm is discouraged for SBRT. Develop checklists for your program. Sample Checklist for SRS Program: Lung “Quality and Safety Considerations in SRS and SBRT”, Solberg et al, Practical Rad Onc, 2011 Checklist for SRS Planning Treatment Delivery (UC) Use a Dry Run Before Patient Treatment • Treatment verification – Reproduce setup – Verify isocenter – Clinically mode up each treatment field Check beam clearance (collision) Check any interlock MLC interlock? Reinitialized but can not clear means corruption of MLC files undeliverable beam Potential MU problem? For example > 1000 for any single field beyond machine capability for non-SRS beams Clearly mark immobilization devices after successful dry run. SBRT Dose Verification with Scintillator 1. Cast the plan in a phantom. 2. Deliver all the beams under treatment conditions. 3. Verify the composite dose with a scintillator dosimeter Exradin W1 Scintillator from Standard Imaging Courtesy of Tianming Wu, PhD SBRT Patient Dose Verification with Scintillator Slide: Courtesy of Tianming Wu, PhD IGRT for SBRT Lung/Liver/Abdominal Cases • If no implanted fiducials, create fluoro beam aperture that hugs GTV. • If there is fiducials, create fluoro beam aperture that use fiducials as corners. • CBCT alignment with GTV, bony landmark secondary but should be less than 1cm discrepancy. Otherwise, reposition patient. • CBCT sometimes do not align well with averaged sim CT due to breathing variation • Fluoro to verify positioning after CBCT. • Fluoro between fields to monitor setup consistency. TG-101: Physicist Presence Single-Fraction SRS Physicist present for entire procedure Multiple-Fraction SRS Physicist present for 1st fraction and at setup of remaining fractions SBRT Physicist present for 1st fraction, and setup for every fraction to verify imaging, registration, gating, immobilization • UC Physics Team – Hania Al-Hallaq, PhD – Karl Farrey, MS – Hyejoo Kang, PhD – Ji Li, PhD – Julien Partouche, MS – Chester Reft, PhD – Chris Stepaniak, PhD – Rodney Wiersma, PhD – Tianming Wu, PhD – Bradley McCabe, PhD – Laura, Padilla, PhD Stanley H. Benedict, PhD Univ. of California- Davis Linac Vendor’s Isocenter Test Set of 63 image Shots (Gantry, Coll., Couch) Specifications: Gantry-Collimator Isocenter Offset ≤0.50 mm (0.30mm) Gantry-Collimator-Couch Iso Offset ≤ 0.75mm (0.61mm) TrueBeam: MV-kV Coincidence Test BB for MV Imaging CBCT Phantom with Markers kV-MV isocenter coincidence ≤ 0.5 mm Typical results < 0.2 mm UC Linac Isocenter Accuracy Test (using a similar system for Lutz test) In-house Matlab code (Ji Li, PhD – UC)