* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Adenomatous Polyposis LMN
Frameshift mutation wikipedia , lookup
Genetic engineering wikipedia , lookup
Human genetic variation wikipedia , lookup
Behavioural genetics wikipedia , lookup
Designer baby wikipedia , lookup
BRCA mutation wikipedia , lookup
Population genetics wikipedia , lookup
DNA paternity testing wikipedia , lookup
Microevolution wikipedia , lookup
Public health genomics wikipedia , lookup
Genome (book) wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Oncogenomics wikipedia , lookup
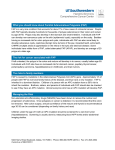
LETTER OF MEDICAL NECESSITY FOR ADENOMATOUS POLYPOSIS GENETIC TESTING (APC and MUTYH analyses) Date: Date of service/claim To: Utilization Review Department Insurance Company Name, Address, City, State Re: Patient Name, DOB, ID # ICD-9 Codes: (quick reference as suggestions: 153.9 malignant neoplasm of the colon, unspecified; V12.72 history colon polyps; unspecified; 211.3 benign neoplasm of the colon; V16.9 family history of unspecified malignant neoplasm) This letter is in regards to my patient and your subscriber, First, Last Name to request full coverage of medically-indicated genetic testing for adenomatous polyposis to be performed by Ambry Genetics Corporation. Familial adenomatous polyposis (FAP) and MUTYH-associated polyposis (MAP) are rare conditions that predispose individuals to developing as many as hundreds to thousands of adenomatous colorectal polyps and a high risk for colorectal cancer. In individuals with classic FAP, polyps begin developing at an average age of 15 years.2 For these people, colorectal cancer is virtually inevitable without colectomy. In untreated patients with classic FAP, the mean age at diagnosis of colorectal cancer is 35-40 years.2 Other tumors and cancers can also occur including: osteomas, soft tissue tumors (like epidermoid cysts, fibromas, and desmoid tumors), central nervous system (CNS) tumors, thyroid cancer, small bowel cancer, stomach cancer, polyps of the gastric fundus and duodenum, dental anomalies, and congenital hypertrophy of the retinal pigment epithelium (CHRPE). Those that develop fewer than one hundred adenomatous colonic polyps may have the attenuated form of FAP (called attenuated FAP or AFAP). Mutations in the APC gene are associated with 7080% of classic FAP cases, and 30-40% of AFAP cases.1,4 Those with fewer than one hundred colonic polyps may also have MAP, which is associated with MUTYH gene mutations. The age at diagnosis of colorectal cancer for those with AFAP or MAP is usually at a later age, as compared to those with classic FAP.1,4 While having a family history of adenomatous polyposis increases the chance of having an APC or MUTYH mutation, there may also be no family history of polyposis, due to the way in which these conditions are inherited. Significant aspects of my patient’s personal and/or family medical history that suggest a reasonable probability of FAP/MAP are below: Based on the above, FAP/MAP is suspected in my patient and I am requesting coverage for this test (APC and MUTYH analyses). According to National Comprehensive Cancer Network (NCCN) published guidelines, germline genetic testing is warranted.3 This genetic testing will help estimate my patient’s risk to develop cancer, and will directly impact my patient’s medical management. If a mutation is identified, we will adjust medical care to reduce my patient’s risk of developing (and potentially dying of) an advanced stage cancer. An aggressive approach following established screening and management guidelines is indicated in individuals that carry a mutation found on this test. Management options may include: Frequent colonoscopy, starting as early as the childhood years Colectomy Upper endoscopy, starting as early as the teenage years Consideration of annual thyroid ultrasound and examination Other: ____________________________________ Due to the cancer risks associated and risk-reducing interventions available, I am requesting coverage for this testing as medically necessary care and affirm that my patient/patient’s family has provided informed consent for genetic testing. A positive test result would confirm a genetic diagnosis and/or risk in my patient, and would ensure my patient is being managed appropriately. I am specifying Ambry Genetics Corporation because this laboratory has highly-sensitive and cost-effective testing for adenomatous polyposis, along with a large database of previously tested patients to ensure highly validated, accurate, and informative test interpretation. I recommend that you support this request for coverage of diagnostic genetic testing for adenomatous polyposis in my patient. Genetic testing can take up to several weeks to complete, and the laboratory will not bill until testing is concluded. Therefore, we are requesting that the authorization be valid for 3 months. Thank you for your time, and please don’t hesitate to contact me with any questions. Sincerely, Ordering Clinician Name (Signature Provided on Test Requisition Form) (MD/DO, Clinical Nurse Specialist, Nurse-Midwives, Nurse Practitioner, Physician Assistant, Genetic Counselor*) *Authorized clinician requirements vary by state Test Details CPT codes: 81201x1, 81203x1, 81479x1, 81406x1 Laboratory: Ambry Genetics Corporation (TIN 33-0892453 / NPI 1861568784), a CAPaccredited and CLIA-certified laboratory located at 7 Argonaut, Aliso Viejo, CA 92656 References: 1. 2. 3. 4. Lipton L, et al. The genetics of FAP and FAP-like syndromes. Fam Cancer. 2006; 5(3):221-226. Bisgaard ML, et al. Familial adenomatous polyposis (FAP): frequency, penetrance, and mutation rate. Hum Mutat. 1994; 3(2):121-125. NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines®). Genetic/Familial High-Risk Assessment: Colorectal. Version 2.2014, 05/19/2014. Filipe B, et al. APC or MUTYH mutations account for the majority of clinically well-characterized families with FAP and AFAP phenotype and patients with more than 30 adenomas. Clin Genet. 2009;76: 242-255.