* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Etiology
Epidemiology of metabolic syndrome wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Epidemiology wikipedia , lookup
Transmission (medicine) wikipedia , lookup
Diseases of poverty wikipedia , lookup
Focal infection theory wikipedia , lookup
Compartmental models in epidemiology wikipedia , lookup
Public health genomics wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
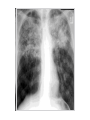
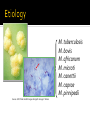
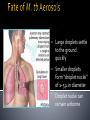
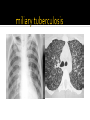
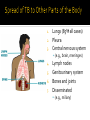
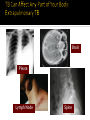
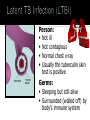
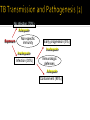
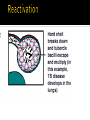
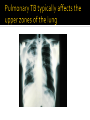
Mohammad Tohidi M.D. Professor of Internal Medicine Department of Pulmonary Diseases Ghaem Hospital MUMS Mashhad IRAN Tuberculosis Transmission and Pathogenesis 21Y O woman referred with the CC of cough for 2 months.She has had small amount of yellow sputum,no fever &night sweat &hemoptysis, but she had 2 kg weight loss.Past medical HX was unremarkable.On PE she was slightly pale,but otherwise normal.She received antibiotics & antitussive with no significant effect. Chest radiography may be particularly helpful in suggesting or confirming the cause of the cough What we should do next? Evaluate based on likely clinical possibilities: Sputum for AFB Stain &culture PFT HRCT Sputum for AFB: ++++ Pulmonary Tuberculosis Tuberculosis (TB) remains the leading cause of death worldwide from a single infectious disease agent. Indeed up to 1/2 of the world's population(3.1 billion) is infected with TB. The registered number of new cases of TB worldwide roughly correlates with economic conditions: the highest incidences are seen in those countries of Africa, Asia, and Latin America with the lowest gross national products. WHO estimates that eight million people get TB every year, of whom 95% live in developing countries. An estimated 2 million people die from TB every year. M. tuberculosis M. bovis M. africanum M. microti M. canettii M. caprae M. pinnipedii Source: CDC Public Health Image Library/Dr. George P. Kubica With the exception of M. pinnipedii, all of the species in the Mycobacterium tuberculosis complex have been shown to cause disease in humans; however, M. tuberculosis is by far the most prevalent Slightly curved, rod shaped bacilli 0.2 - 0.5 microns in diameter; 2 - 4 microns in length Acid fast - resists decolorization with acid/alcohol Multiplies slowly (every 18 - 24 hrs) Thick lipid cell wall Can remain dormant for decades Aerobic Non-motile Mycobacteria commonly found in the environment rarely cause disease in humans and are not spread from person to person Mycobacteria other than tuberculosis (MOTT) most often cause disease in individuals with weakened immune systems Mycobacterium avium and M. intracellulare are the more common MOTT sometimes seen in patients co-infected with HIV Transmission of M.tb Person-to-person through the air by a person with TB disease of the lungs Source: CDC, 2000 Less frequently transmitted by: Ingestion of Mycobacterium bovis found in unpasteurized milk products Laboratory accident Millions of tubercle bacilli in lungs (mainly in cavities) Coughing projects droplet nuclei into the air that contain tubercle bacilli One cough can release 3,000 droplet nuclei One sneeze can release tens of thousands of droplet nuclei When a person with TB disease of the lungs or larynx coughs, sneezes or sings, droplet nuclei containing the TB bacilli are expelled into the air These droplets or particles, called droplet nuclei, are about 1 to 5 microns in diameter - less than 1/5000 of an inch Droplet nuclei can remain suspended in the air for several hours, depending on the environment The average TB patient generates 75,000 droplets per day before therapy This falls to 25 infectious droplets per day within two weeks of effective therapy Large droplets settle to the ground quickly Smaller droplets form “droplet nuclei” of 1–5 µ in diameter Droplet nuclei can remain airborne When a person inhales air that contains droplets, most of the larger droplets become lodged in the upper respiratory tract (the nose and throat), where infection is unlikely to develop. However, the droplet nuclei may reach the small air sacs of the lung (the alveoli), where infection begins The alveoli contain a type of white blood cell, called a macrophage, that eats up any foreign objects in the air sac. When the TB bacteria reaches the air sac it gets eaten up by the macrophage Once the TB bacteria is inside of the macrophage it begins to multiply No infection (70%) Adequate Exposure Non-specific immunity Inadequate Infection (30%) Not everyone who is exposed to TB will become infected When the concentration of TB bacteria circulating in the air is greater Coughing; smear +; cavitary disease Exposure occurs indoors –Poor air circulation and ventilation; small, enclosed space –Poor or no access to sunlight (UV light) The greater the time spent with the infectious person or breathing in air with infectious particles CASE Site of TB Cough Bacillary load Treatment CONTACT Ventilation Filtration U.V. light Closeness and duration of contact Immune status Previous infection Sharing dishes and utensils Using towels and linens Handling food Sharing cell phones Touching computer keyboard This next section describes the pathogenesis of TB (the way TB infection and disease develop in the body) At first, the tubercle bacilli multiply in the alveoli and a small number enter the bloodstream and spread throughout the body (dissemination) Bacilli may reach any part of the body, including areas where TB disease is more likely to develop. These areas include the upper portions of the lungs, as well as the kidneys, the brain, and bone Disseminated TB refers to TB that simultaneously involves multiple organs. While “miliary” is given as an example of disseminated TB, it really refers to a radiographic manifestation of disseminated TB. It’s important to note that not all patients with disseminated TB have a miliary pattern on CXR Lungs (85% all cases) 2. Pleura 3. Central nervous system 1. • (e.g., brain, meninges) Lymph nodes 5. Genitourinary system 6. Bones and joints 7. Disseminated 4. (e.g., miliary) Brain Pleura Lymph Node Spine Within 2 to 10 weeks, however, the body's immune system usually intervenes, halting multiplication and preventing further spread The immune system is the system of cells and tissues in the body that protect the body from foreign substances Person: Not ill Not contagious Normal chest x-ray Usually the tuberculin skin test is positive Germs: Sleeping but still alive Surrounded (walled off) by body’s immune system If the immune system is compromised, then the bacilli multiply and spread to other sites in the body. People who have TB infection but not TB disease are NOT infectious - in other words, they cannot spread the infection to other people Persons with LTBI have a low bacillary load (e.g., ≤~103) It is very important to remember that TB infection is not considered a case of TB No infection (70%) Adequate Exposure Non-specific immunity Early progression (5%) Inadequate Inadequate Infection (30%) Immunologic defenses Adequate Containment (95%) If a person has a healthy immune system, the body will wall off the bacteria and keep it asleep (latent). In areas where the prevalence of HIV is low, the majority of people exposed and infected with TB are able to contain the infection A small proportion, however, will progress to primary, active TB disease. This generally will be individuals with a weakened immune system or, as with infant, sbecause their immune system is not fully developed The highest risk period for early progression to disease is within the first year or two following infection •This typically occurs when the immune system becomes weak allowing the TB bacteria to multiply out of the control of the immune system •The TB bacteria can then escape from the granuloma and enter the airway •This is the usual mechanism of development of active TB among adults TB Germs: Awake and multiplying Cause damage to the lungs Person: Most often feels sick Contagious (before pills started) Usually have a positive tuberculin skin test Chest X-ray is often abnormal (with pulmonary TB) Granuloma breaks down and tubercle escape and multiply No infection (70%) Adequate Exposure Non-immunologic defense Early progression (5%) Inadequate Inadequate Infection (30%) Immunologic defenses Late progression(5%) Inadequate Adequate Containment (95%) Immunologic defenses Adequate Continued containment (90%) Evaluate for risk factors that increase the likelihood: that a person may have LTBI (high prevalence) for progression of LTBI to active TB disease (high risk) To diagnose TB you must first think of TB Knowing when to consider TB in the differential diagnosis = knowing who is at risk risk for infection risk for disease Known contact to person with TB disease Persons who live or spend time in certain congregate settings facilities for the elderly jails, prisons shelters for the homeless drug treatment centers Overcrowded habitation (housing) Persons born in countries with high prevalence of TB Persons more likely to progress from LTBI to TB disease include: HIV-infected persons Persons with a history of prior, untreated TB or fibrotic lesions on chest X-ray Recent TB infection (within past 2 years) Injection drug users Age (very young or very old) Persons with certain medical conditions such as: Diabetes mellitus Chronic renal failure or on hemodialysis Solid organ transplantation Certain types of cancer (e.g., leukemia) Gastrectomy or jejunoileal bypass Underweight or malnourished persons Silicosis Persons taking immunosuppressive agents: Prolonged corticosteroid therapy (>15mg daily for over 4 weeks) Cancer chemotherapy Cyclosporine Persons taking blocking agents against Tumor Necrosis Factor-Alpha: Etanercept (Enbrel®) Infliximab (Remicade®) Adalimumab (HumiraTM) Risk Factor HIV/AIDS How many times higher is the risk of TB disease 113-170 Diabetes 4.1 “old TB” on CXR 13.6 Chronic renal failure Other conditions 25 3-16 Increased risk of reactivation of LTBI (10% annual risk among HIV+ vs. 10% lifetime risk among HIV-negative individuals) More likely to have early progression to TB disease following infection TB can occur at any point in the progression of HIV infection (any CD4 ct.) High risk of recurrent TB (either relapse or reinfection) Source: TB/HIV: A Clinical Manual. Second Edition. WHO, 2004 TB increases HIV replication by activating the immune system Co-infected persons often have very high HIV viral loads Immuno-suppression progresses more quickly, and survival may be shorter despite successful treatment of TB Co-infected patients have a shorter survival period than persons with HIV who never had TB disease Reported TB Cases by Form of Disease United States, 2001 Both (7.4%) Extrapulmonary (20.1%) Pleural (18.3%) Lymphatic (42.5%) PulPulPlnary (72.5%) oary (72.5%) mona (2.5%)حححح Other (12.3%) Bone/joint (10.2%) Genitourinary (5.9%) Peritoneal (4.6%) Meningeal (6.0%) Pulmonary manifestations of tuberculosis (TB) include primary, Reactivation, Endobronchial, Lower lung field infection, Tuberculoma. Fever was the most common symptom Chest pain and pleuritic chest pain(25%) One-half of patients with pleuritic chest pain had evidence of a pleural effusion fatigue, cough, arthralgias and pharyngitis(rare). The physical examination was usually normal; pulmonary signs included pain to palpation and signs of an effusion. hilar adenopathy, occurring in 65 percent Approximately one-third :pleural effusions, typically within the first three to four months after infection Lower and upper lobe infiltrates were observed in 33 and 13 percent of adults, respectively. Most infiltrates resolved over months to years. the infiltrates progressed within the first year after skin test conversion, so-called progressive primary TB. Right middle lobe collapse may complicate the adenopathy. Multiple terms have been used to describe this stage of TB: chronic TB, postprimary disease, recrudescent TB, endogenous reinfection, and adult type progressive TB. One-half to two-thirds of patients developed cough, weight loss and fatigue. Fever and night sweats or night sweats alone were present in approximately one-half. Chest pain and dyspnea each were reported in approximately one-third of patients, and hemoptysis in approximately one-quarter. Dyspnea can occur when patients have extensive parenchymal involvement, pleural effusions, or a pneumothorax. fever, sweats and hemoptysis were less common in the elderly, and these patients were less likely to have cavitary disease or a positive (PPD) skin test. reactivation TB typically involves the apicalposterior segments of the upper lobes (80 to 90 percent of patients), followed in frequency by the superior segment of the lower lobes and the anterior segment of the upper lobes In recent large series of TB in adults, 70 to 87 percent had the upper lobe infiltrates typical of reactivation; 19 to 40 percent also had cavities, with visible air-fluid levels in as many as 20 percent CT scan may show a cavity or centrilobular lesions, nodules and branching linear densities, sometimes called a "tree in bud" appearance. Hilar adenopathy, sometimes associated with right middle lobe collapse Infiltrates or cavities in the middle or lower lung zones (see lower lung field TB below) Pleural effusions Solitary nodules the known increasing incidence of primary TB in adults, rather than "atypical" forms of TB. A normal chest radiograph is also possible even in active pulmonary TB. As an example, in one Canadian study of 518 patients with culture-proven pulmonary TB, 25 patients (5 percent) had normal chest x-rays; 23 of these patients had pulmonary symptoms at the time of the normal radiograph. 15 percent of patients had lesions in the tracheobronchial tree at rigid bronchoscopy and 40 percent at autopsy. At least two mechanisms of developing endobronchial TB are possible: Direct extension to the bronchi from an adjacent parenchymal focus, usually a cavity, Spread of organisms to the bronchi via infected sputum from a distant site. Complications of endobronchial TB can include: Obstruction, Atelectasis (with or without secondary infections), Bronchiectasis, Tracheal or Bronchial stenosis . a barking cough, two-thirds of patients, often accompanied by sputum production. Patients rarely develop so-called bronchorrhea Lithoptysis Wheezing and hemoptysis Dyspnea, when present, may signal: obstruction or atelectasis. The clinical manifestations can also be subacute or chronic, resembling bronchogenic carcinoma The most common radiographic finding of endobronchial TB in adults is an upper lobe infiltrate and cavity with ipsilateral spread to the lower lobe and possibly to the superior segment of the contralateral lower lobe Extensive endobronchial TB can also be associated with bronchiectasis on CT scan. When endobronchial TB occurs in patients with primary disease, segmental atelectasis may be the only finding; atelectasis is more frequent in the right middle lobe and the anterior segment of the right upper lobe. Because endobronchial lesions can exist without extensive parenchymal abnormalities, 10 to 20 percent of patients may have normal chest radiographs While it would be natural to expect that rates of AFB smear positivity would be high with extensive endobronchial involvement, rates of 15 to 20 percent have been reported. This lower rate may be due to bronchial inflammatory tissue which might prevent expectoration of infected secretions — Lower lung field TB is defined as disease located below a line traced across the hila, including the perihilar regions, on a standard PA and lateral chest x-ray 2 to 9 percent in incidence in adults, Typical reactivation TB rarely involves the superior segments of the lower lobes. Endobronchial TB can affect lower lung fields in both primary infection, especially when adjacent lymph nodes are involved, and during reactivation, when spread from upper lobe disease secondarily infects the lower lung fields. Typical primary tuberculosis. A non-specific tuberculous pneumonitis, Compared to upper lobe TB, consolidation in the lower lobes tends to be more extensive and homogeneous. Cavitation may be present, and large cavities are reported. Elderly patients and those with diabetes, renal or hepatic disease, those receiving corticosteroids, and those with underlying silicosis appear most at risk for lower lobe TB. However, many patients have no underlying medical illnesses. Pulmonary complications of TB include hemoptysis, pneumothorax, bronchiectasis and extensive pulmonary destruction (including pulmonary gangrene).