* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Chest X Rays
Survey
Document related concepts
Transcript
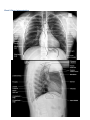
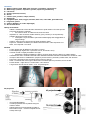
Chest X Rays: Interpretation DRSABCDE D – Details (patient name, DOB, date, film type, orientation, supine/erect) R – RIPE image (rotation, inspiration, picture, exposure (penetration)) S – soft tissue A – airways (trachea, bronchi) B – bones C – cardiac (size, position, shape, borders) D – diaphragm E – equipment (ETT, ECG, oxygen, NG tube, PICC line, chest tube, pacemaker etc) F – lung fields, pleura G – gastric (bubbles, air under diaphragm) H – hila and hardware Quality assessment - rotation: medial ends of the clavicles should be an equal distance from the spinous processes of thoracic vertebrae o If R clavicle closer rotated to left, and vice versa - inspiration: 5-7 ribs should be visible anteriorly (curly red ribs) or 9-10 posteriorly (straight ribs that meet the spine) o incomplete x-rays can lead to perceived cardiomegaly and exaggeration of lung markings - position: entire thoracic cage and lung fields should be visible - exposure: vertebrae should be just visible behind the heart. under-exposed = too white, over-exposed = too black Normals - L hilum higher than R (difference should be <2.5cm) - R hemidiaphragm higher than L (because of liver, should be <3cm) - Trachea central or slightly deviated to the right o deviated by collapse (towards the lesion), tension (away from the lesion) or patient rotation - Cardiothoracic ratio: maximal horizontal heart diameter/maximal horizontal chest diameter, should be <50% - 3 lumps of left border of mediastinum (supinf): aortic knuckle, pulmonary outflow track, left ventricle - Pulmonary vasculature less prominent higher up due to gravity - Heart: 1/3 of diameter to the right of the thoracic vertebrae spinous processes, 2/3 to the left - R heart border = right atrium; L heart border = left ventricle - Lung fissures should not be visible – if so, it’s pathological PA projection - conventional/standard not always possible due to patient being too unwell to stand patient places arms around detector plate or with hands on hips – ensures scapulae do not overlap the lungs AP projection - heart size exaggerated due to the heart being further from the detector can be taken by mobile X-ray scapulae are not retracted laterally Consolidation - any pathologic process that fills the alveoli with fluid, pus, blood, cells (including tumour cells) or other substances resulting in lobar, diffuse or multifocal illdefined opacities. Interstitial - involvement of the supporting tissue of the lung parenchyma resulting in fine or coarse reticular (net like) opacities or small nodules. Nodule or mass - any space occupying lesion either solitary or multiple. Atelectasis - collapse of a part of the lung due to a decrease in the amount of air in the alveoli resulting in volume loss and resulting increased density. Tracheal displacement - Volume loss pulls trachea to the same side as the pathology o Causes: obstruction (mass in bronchus), compression (effusion/pneumothorax), contraction (previous inflammation) Direct signs: displaced septa, increased radiodensity in affected lobe, crowding of vascular and bronchial markings - increased pressure/volume pushes trachea to the contralateral side - Causes: pneumothorax, pneumonectomy, atelectasis, pleural effusion, pleural fibrosis, space occupying lesions, lymphomas Hilar abnormalities - bilateral hilar enlargement o sarcoidosis, lymphoma, metastatic malignancy, infection (TB, IMN, Brucellosis, taxoplasmosis), SLE, RA - uni/bilateral hilar enlargement o lymphadenopathy o hilar malignancy (e.g. small cell carcinoma) o vascular disease (e.g. pulmonary hypertension or proximal pulmonary artery aneurysm) - abnormal hilar position o loss of volume in hemithorax pulling of hilum o increase in volume/pressure in hemithorax pushing of hilum Lung abnormalities Consolidation - alveoli filled with material: o pus – pneumonia o blood – haemorhhage, DIC o water – pulmonary oedema, renal/liver failure, ARDS, near drowning ARDS = non cardiogenic pulmonary oedema – onset within 1 week. CXR: bilateral opacification o cells – lymphoma, bronchioalveolar carcinoma o protein – alveolar proteinosis, ARDS, fat emboli - produces silhouette sign = loss of border between thoracic structures o loss of R heart border R middle lobe pathology (e.g. consolidation) o loss of L heart border lingular pathology (e.g. consolidation) o loss of aortic knuckle left upper lobe/middle mediastinum pathology - consolidated lung becomes dense and white – if the larger airways are spared, they are relatively blacker (lower density) = air bronchogram - ARDS - bilateral, predominately peripheral, asymmetric consolidations with air bronchograms Hyperlucency - due to alveolar distension (air retention) and/or reduced arterial flow - causes: pneumothorax, obstructive emphysema, PE Lung masses Solitary pulmonary nodule - malignancy – primary lung cancer, metastasis - benign – granuloma (80%), hamartoma (10%), pulmonary infarct (late stage: wedge shape pleural based opacification), AV malformation Cavitary lung lesions - abscess (typically thick walls and may have air/fluid levels) - TB (usually upper lobe) - carcinoma - Wegener’s granulomatosis (smaller lesions, can be multiple) - metastatic cancer (typically thin walled, may have a variable appearance) - septic emboli (smaller lesions) Pleural disease Pneumothorax = air/gas in pleural space - a pneumothorax may be identified by a discrete shadowed line beyond which no lung markings are present o most commonly occur in the lung apices, which are the least dependent part of the lung o expiratory projections make a pneumothorax more obvious (expiration reduced lung volume increased density of parenchyma makes the distinction clearer) - tension pneumothorax = the accumulation of air under pressure in the pleural space o develops when injured tissue creates a one-way valve for air to enter, but not leave, the pleural space. o ipsilateral lung collapse with widened intercostal spaces and contralateral tracheal/mediastinal deviation o With a left pneumothorax, the left hemidiaphram may be depressed, but the liver prevents this from developing on the right side. Hydropneumothorax - air and fluid within pleural space - oesophageal rupture, trauma, infection with gas forming organism, bronchopleural fistula, iatrogenic after surgery - horizontal air fluid level that extends across the whole length of the hemithorax Pleural effusion = collection of fluid in pleural space - settles with gravity - causes blunting of the costophrenic angles and hemidiaphragm if the patient is erect - meniscus sign = concavity of fluid surface Pleural thickening - unilateral – malignant mesothelioma (can be either plaque or nodular; caused by asbestos exposure), empyema, trauma, post-op scarring, metastatic disease o Malignant mesothelioma = primary pleural neoplasm well circumscribed, homogeneous soft tissue mass closely related to pleura shadowing over whole lung due to circumferential pleural thickening Lesions may be found anywhere along the lung periphery (shown), pulmonary fissures, mediastinum, or diaphragm. Large lesions may be confused for lobar consolidation - bilateral – metastases, trauma, asbestosis Pleural plaques - calcified plaques due to asbestos exposure with peripheral pleural thickening - bilateral well defined irregular shadows as dense as bone Diaphragmatic abnormalities Loss of diaphragmatic outline - fluid, consolidation or collapse of adjacent lung (i.e. R/L lower lobe) Pneumoperitoneum - = free gas under diaphragm = rupture of abdominal hollow viscus (e.g. bowel perforation) - crescents of relatively low density (black) under diaphragm Raised hemidiaphragm - causes: lung volume loss, damage to the phrenic nerve, diaphragmatic hernia, trauma Hyperexpansion – COPD - >7 ribs visible, bilateral flattening of hemidiaphragms, narrowing of heart (decreased cardiothoracic ratio), prominent lower zone markings, blunting of costophrenic angles - Emphysema o hyperinflation + bullae present Heart contour abnormalities Increased cardiothoracic ratio (cardiomegaly) - ventricular dilatation (usually left) - atrial enlargement o LA enlargement splaying of the carina to >90 degrees (the carina lies directly above the left atrium) - cardiac failure o look for other signs of heart failure ABCDE of cardiac failure: A – alveolar batwinging (pulmonary oedema) B – Kerley B lines (pulmonary oedema) C – cardiomegaly D – distribution of vasculature increased in upper lobes E – pleural effusion - left ventricular aneurysm o uncommon complication of MI o bulging left heart border with a circular rim of calcification - pericardial effusion - pneumopericardium o caused by ruptured alveoli (in pneumothorax), tracheobronchial rupture, oesophageal rupture, blunt chest trauma continuous diaphragm sign – diaphragm continuous crossing spine Pulmonary oedema - Pulmonary oedema: 3 stages o 1 – pulmonary venous congestion (= upper lobe diversion) normally: veins higher more wispy, those lower thicker (due to gravity) pulmonary venous congestion: “juicy, fat” veins in upper zones o 2 – interstitial oedema transudate from pulmonary veins seeps into interstitial spaces Kerley B lines o 3 – alveolar oedema looks like airspace disease – fluffy white opacification with loss of hemidiaphragms and heart borders in pattern of ‘bat wings’ looks the same as pneumonia superimposed on interstitial oedema airspace disease will disappear quickly with diuretic therapy - Kerley B lines (fluid leaking into interlobular septae) = short 1-2cm white horizontal lines near costophrenic angles, running perpendicular to the pleura - bilateral increased lung markings classically perihilar and shaped like bats wings - Kerley A lines - longer (at least 2cm and up to 6cm) unbranching lines coursing diagonally from the hila out to the periphery of the lungs. Caused by distension of anastomotic channels between peripheral and central lymphatics of the lungs. Kerley A lines are less commonly seen than Kerley B lines. Kerley A lines are never seen without Kerley B or C lines also present. - Kerley C lines - the least commonly seen of the Kerley lines. They are short, fine lines throughout the lungs, with a reticular appearance. They may represent thickening of anastomotic lymphatics or superimposition of many Kerley B lines. Mediastinal abnormalities Widened mediastinum - AP CXR view - unfolded aortic arch (not pathological) - thoracic aortic aneurysm - mediastinal lymphadenopathy - mediastinal mass – 4 T’s – teratoma, teratodermoid cyst, thymoma, thyroid mass + paravertebral mass, lymphoma - retrosternal thyroid - oesophageal dilatation - ruptured aorta - mediastinal emphysema (secondary to penetrating wound +/- lacerated lung, perforated oesophagus/trachea, asthma or whooping cough (pneumomediastinum) o pneumomediastinum = free air in mediastinum - most commonly occurs following trauma or iatrogenic injury to the esophagus or adjacent alveoli o On chest radiography free air may outline anatomic structures. o Common findings are a thin line of radiolucency that outlines the cardiac silhouette (white arrow), vertically oriented streaks of air in the mediastinum, a double bronchial wall sign, or lucency around the right pulmonary artery, the "ring around the artery" sign. o most easily detected retrosternally on lateral chest radiographs - pericardial effusion o accumulation of fluid within the pericardial space. o enlarged cardiac silhouette – globular, water droplet shaped with loss of LA – LV notch o If fluid accumulates rapidly, minimal cardiomegaly may be present. o Other potential findings include pleural effusion and rarely pericardial calcifications. o Pericardial effusion in an Asian patient - always think of TB. o Other causes are uremia and metastatic carcinoma Bone abnormalities - Typical findings of acute osteomyelitis on plain radiographs o soft tissue swelling, periosteal reaction, cortical irregularity, and demineralization. - In chronic osteomyelitis, there is thick, irregular, sclerotic bone with radiolucencies and an elevated periosteum. - Primary and metastatic cancer to the bones may be evident on chest radiographs. - Boney lesions may be sclerotic or lytic and can give clues as to the etiology. - Common malignancies giving rise to sclerotic metastasis: o prostate cancer, breast cancer and lymphoma - Common malignancies giving rise to lytic metastasis: o renal cell cancer, multiple myeloma and thyroid cancer. Soft tissue abnormalities - surgical/subcutaneous emphysema (gas/air trapped in layer under skin) o causes: trauma, pneumothorax, pneumopericardium, pneumomediastinum, iatrogenic, infection (skin necrotising infections such as gangrene)