* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Skin and Soft tissue infections
Survey
Document related concepts
Marburg virus disease wikipedia , lookup
Hepatitis C wikipedia , lookup
Clostridium difficile infection wikipedia , lookup
Hepatitis B wikipedia , lookup
Schistosomiasis wikipedia , lookup
Anaerobic infection wikipedia , lookup
Oesophagostomum wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Leptospirosis wikipedia , lookup
Methicillin-resistant Staphylococcus aureus wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Transcript
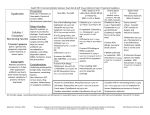
PRMCE ANTI-INFECTIVES SELECTION GUIDELINE FOR ADULTS SKIN AND SOFT TISSUE INFECTIONS: A. Cellulitis: MRSA uncommonly causes cellulitis in the absence of a wound or abscess. Add empiric anti-MRSA therapy if severe disease is present or if risk factors for MRSA are present: Risk factors: 1. H/o MRSA or hospitalization or residence in a long term care facility within 1 year 2. Recent antibiotic therapy within 4 months 3. HIV infection or men who have sex with men or injection drug use 4. Hemodialysis 5. Incarceration 6. Military service 7. Sharing needles, razors or sharing sports equipment Mild Moderate (requires admission) Severe (sepsis) Necrotizing soft tissue infections including necrotizing fasciitis Cephalexin 500mg PO QID for 7-10 days or Clindamycin 300mg PO QID for 7-10 days (if anaphylaxis to penicillin)1 Cefazolin (per protocol) 1g IV q8h equivalent for 10-14 days or Clindamycin (per protocol) 900mg IV q8h equivalent for 10-14 days (if anaphylaxis to penicillin) Vancomycin IV (per protocol, goal trough 15-20) plus Cefazolin (per protocol) 1g IV q8h equivalent for 10-14 days Vancomycin (IV (per protocol, goal trough of 15-20) plus Meropenem (per protocol) 500mg IV q6h equivalent Duration of therapy is guided by clinical course/surgical intervention Note: Consider consultation with ID or general surgery for (1) pain disproportionate to the physical findings, (2) violaceous bullae, (3) cutaneous hemorrhage, (4) skin sloughing, (5) skin anesthesia, (6) rapid progression, and (7) gas in the tissue 1 Clindamycin substantially increases the risk for C. difficile associated diarrhea (OR=32) Dial S, Kezouh A, Dascal A, Barkun A, Suissa S. CMAJ 2008;179:767-772 Order Set: ED Cellulitis/Wound Infection B. Community Acquired MRSA (CA-MRSA). If soft tissue abscess is present, assume MRSA is present; obtain cultures with I+D if no prior cultures are available on records. Duration of therapy: Treat for 14 days. 1 Trimethoprim/sulfamethoxazole DS 1 to 2 tablets PO BID (1st line)2 or Clindamycin 300mg mg PO QID (2nd line) or Minocycline 100mg PO BID (3rd line) or Linezolid 600mg PO BID (formulary restriction; ID approval) Moderate or Vancomycin IV (per protocol, goal trough 10-15) Severe or Linezolid 600mg PO BID (formulary restriction; ID approval) Recurrent MRSA Outpatient ID consultation if patient has frequent MRSA soft tissue abscesses >2 infections. Call 425-261-4905 to schedule. episodes Mild 2 Dose for patients >40kg is 2 tablets BID, however, minor infections may respond to lower dose with lower incidence of nausea Order Set: ED Cellulitis/Wound Infection C. Diabetic foot infection. Uninfected wounds do not require antibiotics, refer to outpatient podiatry for wound management. Obtain cultures for infected wounds. Duration of therapy: Based on clinical response and surgical intervention; generally 14 days. Cellulitis without Treat as above for cellulitis open wound Infected diabetic Amoxicillin/clavulanate (Augmentin) 875mg PO BID x 7 days foot ulcer (mild) or Cephalexin 500mg PO QID for 7-10 days (if rash with penicillin) plus Metronidazole 500mg PO TID or (anaphylaxis with penicillin) Clindamycin 300mg mg PO QID plus Ciprofloxacin 500mg PO BID Infected diabetic Ampicillin/sulbactam (Unasyn) 3g IV q6h equivalent foot ulcer or (ModerateCeftriaxone 1g IV q24h (if rash with penicillin) requiring plus admission) Metronidazole 500mg IV q8h Infected diabetic foot ulcer (Severe) Note: Cellulitis extending >2cm, lymphangitic streaking, spread beneath the superficial fascia, deep-tissue abscess, gangrene, and involvement of muscle, tendon, joint or bone Vancomycin IV (per protocol, goal trough 15-20) plus Piperacillin/Tazobactam 4.5g IV (Zosyn per protocol) q6h equivalent Severe includes fever, chills, tachycardia, hypotension, confusion, vomiting, leukocytosis, acidosis, severe hyperglycemia, or azotemia 2 Order Set: None RESPIRATORY INFECTIONS: Community Acquired Pneumonia (CAP) Use CAP Protocol, MRSA is still uncommon in CAP, treat if risk factors are present, or if clinical course is suggestive of MRSA pneumonia: ie rapid progression of lung infection in an otherwise healthy patient, with lung necrosis or sepsis. Ambulatory patients CAP needing hospitalization MRSA risk Azithromycin 500mg PO x 1, then 250mg PO x 4 days (1st line) or Levofloxacin 750 PO q24h x 7 days (2nd line) Ceftriaxone 1g IV q24 h plus Azithromycin 500mg PO q24h (1st line) or Levofloxacin 750 PO q24 hours (2nd line) Vancomycin IV (per protocol, goal trough 15-20) plus Ceftriaxone 1g IV q24h plus Azithromycin 500mg PO q24h Duration of therapy: Treat for 14 days for MRSA, if confirmed Hospital Acquired Pneumonia (HAP)/Healthcare associated pneumonia, obtain sputum cultures: Hospitalized patients Vancomycin IV (per protocol, goal trough 15-20) plus Piperacillin/Tazobactam 4.5g IV (Zosyn per protocol) q6 hours equivalent Duration of therapy: Treat for 7 days 14 days if: MRSA, Pseudomonas, or ESBL G-negative rods Aspiration Pneumonia evaluate for risk factors for HAP/MRSA, obtain sputum cultures, and if no risk factors are present: Hospitalized patients Ampicillin/sulbactam (Unasyn) 3g IV q6h equivalent (1st line) or Ceftriaxone 1g IV q12h plus Metronidazole 500mg IV q8h (2nd line) Duration of therapy: Treat for 7 days. Order Set: IP Community-Acquired Pneumonia Admission URINARY TRACT INFECTION (UTI): Asymptomatic bacteriuria in pregnancy Macrodantin (Macrobid) 100mg PO BID x 5 days (1st line) or Cefixime 200mg PO BID x 5 days (2nd line) or Amoxicillin 250mg PO q8h x 5 days (3rd line) 3 Note: Test of cure should be obtained 7 days post treatment, and then monthly until completion of therapy Acute cystitis in women of childbearing age Macrodantin (Macrobid) 100 mg PO BID x 5 days or Trimethoprim/sulfamethoxazole DS 1 tab PO BID x 3 days (2nd line) or Ciprofloxacin 250mg PO BID x 3 days (3rd line) Mild pyelonephritis (low grade fever < 101.5, only slightly elevated WBC, no nausea/vomiting) UTI with sepsis/ complicated pyelonephritis Ciprofloxacin 500mg PO BID x 7 days Acute uncomplicated pyelonephritis in pregnancy Prostatitis: Note: If beta-lactams are used, duration of therapy is 14-21 days. Vancomycin IV (per protocol, goal trough 10-15) plus Piperacillin/Tazobactam 3.375g IV (Zosyn per protocol) q6h equivalent (14-day course of antimicrobial therapy is recommended; consider changing to ciprofloxacin orally if appropriate based on culture results). Ceftriaxone 1g IV q12h Note: All pregnant patients should be hospitalized for pyelonephritis and treated with parenteral antimicrobials until afebrile for 24 hours. Ciprofloxacin 500mg PO q12h or Trimethoprim/sulfamethoxazole DS 1 tab PO BID Note: Complete 21-28 days of therapy. Initial empiric antibiotics with followup in 1 week for culture results and assessment of clinical improvement as aggressive treatment of acute prostatitis can lessen the chance of developing chronic prostatitis. Order Set: see UTI within “Sepsis” order set for patients who have SIRS and a UTI INTRA-ABDOMINAL INFECTIONS: Changes based on IDSA guideline Mild – to – Moderate Severity Ceftriaxone 1g IV q12h plus Metronidazole 500mg IV q8h or (if beta-lactam allergy): Levofloxacin 750mg IV q24h plus Metronidazole 500mg IV/PO q8h Duration of therapy: Treat for 10-14 days High Risk or Severity Single Agent: (severe physiologic Piperacillin-tazobactam 3.375g IV (Zosyn per protocol) q6h 4 disturbance, advanced age, or immunocompromised state) equivalent or Combination: Cefepime 2g IV q12h (rash with penicillin) or Ciprofloxacin 400 mg IV q12h (anaphylaxis with penicillin) Plus Metronidazole 500mg IV q8h Duration of therapy: Treat for 10-14 days Order Set: see intra-abdominal infection within “Sepsis” order set for patients who have SIRS and an abdominal infection SEPSIS: Initial treatment Bacterial endocarditis Vancomycin IV (per protocol, goal trough 15-20) (1st line) plus Piperacillin/tazobactam 4.5 g IV q6h (Zosyn per protocol) equivalent or Meropenem 500mg IV q6h equivalent plus Vancomycin IV (per protocol, goal trough 15-20) (2nd line) Note: See Sepsis preprinted order form (# 36723) Duration of therapy: Based on site of infection. If no source, treat for 1014 days/consult infectious disease Vancomycin IV (per protocol, goal trough 15-20) plus Ceftriaxone 2g IV q24h Note: Consult ID Order Set: Sepsis and Sepsis - Severe FEBRILE NEUTROPENIA: Initial treatment Meropenem 500 mg IV q6h equivalent Add Vancomycin IV (per protocol, goal trough 15-20) for: 1. Sepsis, 2. Mucositis, 3. Skin or catheter site infection, 4. History of MRSA colonization, 5. Recent quinolone prophylaxis Duration of therapy: Based on clinical course and neutrophiles recovery. Order Set: ED Fever and Neutropenia 5 BACTERIAL MENINGITIS: Duration of therapy: Generally, for all age groups 2-3 weeks; depending on causative organism; consult infectious disease In Adults <50 yrs. >50 yrs. or immunosuppressed Vancomycin IV (per protocol, goal trough 15-20) plus Ceftriaxone 2g IV q12h Administer dexamethasone 0.15 mg/kg (up to 10mg) q6h IV (for 2 to 4 days); first dose to be given 10-20 minutes prior to antibiotics or at the time of first antibiotic administration. add Ampicillin 2g IV q4h equivalent to above regimen Note: CT scan recommended before lumbar puncture in the following cases: 1. >60yrs of age 2. Immunocompromised 3. History of CNS disease 4. Seizure within a week of presentation 5. Abnormal level of consciousness or mentation 6. Focal neurological deficits (NEJM 2001; 345:1727) Order Set: GEN IP Bacterial Meningitis Admission STD TREATMENT: Updated with 2010 CDC guidelines Chlamydia cervicitis Gonorrhea cervicitis/oropharygeal Epididymitis Azithromycin 1gm PO x 1 dose or Doxycycline 100mg PO BID x 7 days Ceftriaxone 250 mg IM x 1 dose (Note: Cefixime PO should not be used, failures are reported with oroesophageal gonorrhea) Coverage for GC and CL as above if less than 35 yrs Pregnancy* Azithromycin 1 gm PO x dose or Amoxicillin 500mg PO TID x 7 days Ceftriaxone 250 mg IM x 1 dose N/A For acute epididymitis most likely caused by enteric organisms: Levofloxacin 500 mg PO once daily x 10 days PID – Outpatient Coverage for GC and CL as above except give Doxycycline 100 mg PO BID for 14 days 6 N/A PID – Inpatient plus Metronidazole 500mg PO q12h x 14 days Cefoxitin 2 g IV q6h plus Doxycycline 100 mg PO q12h Gentamicin 5mg/kg IV q24h plus Clindamycin 900mg IV q8h (Note: Cefotetan is off formulary due to decreased activity against B. fragilis group). Duration of therapy: At least 24 hours after the patient improves; then continue outpatient treatment for 14 days** * Recommend follow up testing 3 weeks after treatment in pregnancy ** CDC guideline for PID treatment Note: CDC guidelines recommend all partners within previous 60 days be treated and that intercourse be refrained from for 7 days after treatment is initiated. Order Set: GYN IP PID Admit GENERAL NOTES: 1. Obtain cultures where indicated (esp. sputum cultures if pneumonia suspected). 2. Be vigilant regarding previously documented resistant organisms that have been cultured. 3. Document specific allergy to Penicillin, if hives are allergy, generally it is OK to use cephalosporins. 4. Order parenteral antibiotics to be dosed per pharmacy protocol (create a pharmacy consult in EPIC); pharmacy services will adjust all dosages for renal or hepatic functions (per target dose equivalent listed in the guideline above), which can vary widely during an admission. 5. Add indication for antimicrobial when ordering per pharmacy dosing: For example: “Ceftriaxone IV per protocol for meningitis” will result in 2g IV q12 hours dosing. 6. Avoid clindamycin and fluoroquinolones where possible. 7. Use established hospital protocols for CAP and Sepsis. Restricted agents (indicate in orders reasoning for use) 1st dose will be administered; subsequent doses will require approval by Infectious Diseases: Linezolid Daptomycin Ertapenem (Exception: ICU) Aztreonam Voriconazole (Exception: ICU) Telavancin Tigecycline Quinupristin/Dalfopristin Meropenem (Exception: Neutropenic fever, ICU, NICU/pediatrics) Imipenem/cilastatin (meropenem is now preferred carbapenem on formulary) Micafungin (Exception: ICU) Caspofungin (micafungin is now preferred echinocandin antifungal on formulary) 7 Agents which prompt review by Antimicrobial Therapy Monitoring Service (ATMS): Vancomycin Piperacillin/Tazobactam Imipenem/Cilastatin Meropenem Ertapenem Aztreonam Telavancin Clindamycin Tigecycline Linezolid Quinupristin/Dalfopristin Daptomycin Voriconazole Caspofungin Micafungin PRMCE ANTI-INFECTIVEs SELECTION GUIDELINE FOR ADULTS: Document created: May 2009 Last revision: September 2013 Authors: George Diaz, MD Ahmet Tural, MD Matthew Beecroft, MD Erika Schroeder, MD, MPH Toby Wu, PharmD candidate Editors: Thomasz Ziedalski, MD Mohammed Alhyraba, MD Enrique Enguidanos, MD William Finley, MD Frank Andersen, MD Paul Grochal, PharmD Infectious disease Infectious disease Emergency medicine Emergency Medicine Pharmacy intern Pulmonology Critical care medicine Emergency medicine General surgery Obstetrics/gynecology Pharmacy 8