* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Ophthalmology Expert questions Evaluation of the red eye E H
Survey
Document related concepts
Idiopathic intracranial hypertension wikipedia , lookup
Visual impairment wikipedia , lookup
Contact lens wikipedia , lookup
Vision therapy wikipedia , lookup
Retinitis pigmentosa wikipedia , lookup
Diabetic retinopathy wikipedia , lookup
Mitochondrial optic neuropathies wikipedia , lookup
Eyeglass prescription wikipedia , lookup
Cataract surgery wikipedia , lookup
Dry eye syndrome wikipedia , lookup
Transcript
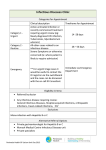
Ophthalmology Expert questions Evaluation of the red eye EH There are many conditions that can lead to a patient presenting with a red eye. A useful distinguishing feature is whether the condition is painful or painless, and with further slit lamp examination for specific features. Painless Red eye: It is rare for a painless red eye to require urgent ophthalmological assessment. Conjunctival redness can be diffuse or localized as follows: Diffuse: Lids Abnormal: Blepharitis – non specific generalized inflammation of the eyelids o Treat with daily lid hygiene, lubrication as required and non-urgent referral Ectropion – lids turning outward with exposure of conjunctival sac o Topical lubrication with non-urgent referral Trichiasis o Epilate, lubricate with non-urgent referral Entropion – lids turning inwards with eyelids abrading cornea o Check cornea with fluorescein o Intact cornea – lubrication with non-urgent referral o Epithelial defect – tape back eyelid from the cornea and manage as corneal foreign body Eyelid lesion o no overt infection/inflammation and no ocular involvement – non-urgent referral, consider topical antibiotics Lids Normal Conjunctivitis – most cases are painful Localised Pterygium – raised yellowish fleshy lesion at limbus, may become painful and red if inflamed o Lubrication and sunglasses o Non-urgent referral Corneal foreign body o Remove foreign body and treat with topical antibiotics Ocular trauma o Treatment as for blunt or penetrating trauma o Topical antibiotics for superficial trama Subconjunctival hemorrhage – o blood redness, unilateral, localized and sharply circumscribed o Underlying sclera not visible o No inflammation, pain or discharge o h/o minor injuries, coughing, sneezing o common with antiplatelet agents and anticoagulants check manage BP if on warfarin- check INR use lubricating eyedrops refer if worsens or pain develops Painful Red Eye Cornea Abnormal Use fluorescein to ascertain nature of any epithelial defect Herpes simplex infection o Dendritic ulcer o Treatment with topical acyclovir o Urgent ophalmologist review within 24 hrs Bacterial ulcer o Often h/o contact lens use o o Epithelial defect with opacified base Immediate consult by phone, may require admission for microbial investigation and antibiotic treatment Marginal ulcer o Secondary to blepharitis o Ulcer at corneal periphery o Immediate consult by phone and urgent referral Foreign body/ corneal abrasion o Remove foreign body treat with topical antibiotics o Treatment for corneal abrasion Eyelid Abnormal Chalazion, stye o Localized eyelid inflammation with minimal ocular involvement o Treat with antibiotic ointment if indicated o If acutely inflamed treat with oral antibiotics and warm compresses o Non-urgent referral Acute blepharitis o Localized eyelid inflammation with minimal ocular involvement o Treat with antibiotic ointment is indicated o Non-urgent referral Herpes Zoster o Vesicular rash o Treat with oral antivirals within 72 hrs of appearance of rash o Non-urgent referral – if cornea normal Diffuse conjunctival injection Viral conjunctivitis o Contact history o Burning sensation and watery discharge – not purulent o Highly contagious – standard precautions Wash hands and separate tissues to avoid infection of other eye Cool compresses Lubricants Antibiotic drops if indicated Never steroids! Photphobia or marked decrease in visual acuity – urgent referral Allergic conjunctivitis o Itch!!! o Atopic history: asthma, eczema, conjunctivitis o Cool compresses, ocular lubricant o Semi-urgent referral – within 3 days if symptoms not controlled Bacterial conjunctivitis o Tender inflamed conjunctiva with purulent discharge – often bilateral o No corneal or anterior chamber involvement o Systemically well – common in children and elderly Regular hygiene Wash hands and separate tissues Topical antibiotics QID for 5 days o Refer if vision affected, symptoms not improving or persists without improvement in 5days Dry eyes o Chronic ocular condition o Symptoms worsen in the evening Lubricants Non-urgent referral Acute angle closure glaucoma Cornea usually has hazy appearance Anterior chamber shallow with irregular semidilated pupil Affected eye very tender and tense to palpation Systemic symptoms of headache, nausea and vomiting o Urgent referral and immediate consult Ciliary injection/ Scleral involvement Scleritis o Vision may be impaired o Sclera thickened and discoloured o Associated h/o vasculitis or connective tissue disease to be sought o Urgent referral – within 24 hrs Anterior chamber involvement Acute anterior uveitis (Iritis) o Pain, photophobia and red eye o Anterior chamber cloudy from cells and flare o Urgent referral < 24 hrs. Hypopyon o Visible accumulation of white cells inferiorly seen in severe uveitis o Urgent referral + consult by phone – to investigate infection, inflammation or ocular malignancy Hyphaema o Usually trauma related but consider non accidental injury in children and blood dyscrasias o Bed rest o Urgent referral <24hrs Evaluation of the painful eye EH Painful eye is one of the common presentations to emergency department and though most causes may be managed well, some serious disorders need urgent evaluation and early recognition and management. Eye pain can be broadly divided into ocular pain and orbital pain. Ocular pain: pain arising from the anterior structures of the eye i.e. cornes, anterior chamber, iris and may be described as sharp, aching, burning or foreign body sensation. Orbital pain: a more dull aching deep seated pain originating from the posterior and retrobulbar structures of the eye. Both types of pain may co-exist and the type of pain is not sensitive enough to suggest a diagnosis and all patients need to undergo a detailed ophthalmologic and sometimes physical examination to rule out serious disorders. The most common causes overall are Corneal abrasion Foreign bodies However, most corneal disorders can cause eye pain. A feeling of scratchiness or of a foreign body may be caused by either a conjunctival or a corneal disorder. Cause Suggestive findings Disorders affecting the cornea Contact lens keratitis h/o contact lens use, ocular pain, bilateral red eyes, lacrimation and corneal edema Corneal foreign body or h/o injury, unilateral pain abrasion on blinking, FB sensation lesion/FB visible on fluorescein examination Diagnostic approach Treatment Clinical evaluation Urgent referral Clinical evaluation incl. Eyelid eversion Corneal ulcer Scrapings may be needed for cultures done by opthal. Clinical evaluation and viral swabs Topical antibiotics and cycloplegic agent, analgesia Removal of foreign body Urgent referral, topical acyclovir or antibiotics depends on cause Urgent referral Symptomatic management, preventive measures and analgesia Epidemic keratoconjunctivitis Herpes zoster ophthalmicus Herpes simplex keratitis Flash burns Symptoms as in FB. Ulcer visible on fluorescein examination Gittiness, bilateral red eys, often eyelid edema, copious discharge, preauricular lymphadenopathy, chemosis, occasionally severe temporary loss of vision. Punctuate staining on fluorescein Unilateral vesicles and crusts in typical dermatome distribution, eyelid edema, severe pain delayed, associated with uveitis Onset after conjunctivitis with blisters on eyelids Classic dendritic lesion on fluorescein Onset after exposure to excessive UV light e.g. welding, bright sun on snow, bilateral with marked injection, Clinical diagnosis, viral cultures if unclear Oral retrovirals within 72 hrs of rash Non urgent referral unless corneal involvement Clinical diagnosis, viral cultures if unclear Topical acyclovir, urgent referral Clinical evaluation Topical antibiotic QID and cyclopegic for comfort, oral analgesia PRN punctuate staining on fluorescein Other Ocular disorders – most cause orbital pain as well Acute angle-closure Severe ocular/ orbital pain, glaucoma systemic symptoms, halos around light, hazy cornea. Marked erythema, raised IOP Anterior uveitis Ocular pain, ciliary flush, photophobia. H/o systemic disorder. Cells and flare on slit lamp, rarely hypopyon Endophthalmitis Severe orbital pain and decreased visual acuity, intense conj. Hyperaemia. H/o recent surgery. Cells and flare Optic neuritis Mild pain may worsen with eye movement, vision loss(blind spot), afferent pupillary defect, swollen optic disk Orbital cellulitis Orbital pain, periorbital pain, unilateral propotosis, impaired eye movements, periorbital edema, systemic findings Orbital pseudotumor Pain. Limited movements, propotosis and congestion. h/o systemic disorder Scleritis Very severe pain, photophobia, lacrimation, discoloured patches under bulbar conjunctiva, sclera edema. h/o AI disease Disorders causing referred pain Cluster headache Prior history, ass headaches, rhinorrhea, flushing, lacrimation, photophobia Sinusitis Periorbital edema nil other ocular signs unless orbital contents involved s/o sinusitis Clinical and by tonometry Clinical evaluation Topical β-blocker, topical α-agonist, azetazolamide, mannitol, pilocarpine (mydriatic). Urgent referral Topical steroids by ophth. Treat underlying cause Clinical evaluation, cultures by ophth. Sedation, analgesics, subconjunctival and IV antibiotics guided by cultures Ophthalmoscopy, MRI Urgent referral, systemic steroids if demyelinating lesions Clinical evaluation, CT or MRI Urgent referral, admission, IV antibiotics Difficult, early referral, CT or MRI Trial of systemic steroids Clinical evaluation Treatment for underlying cause NSAID and/or steroids Clinical evaluation, eye exam may be difficult Treat underlying cause Clinical evaluation, +/- CT Management of sinusitis Key Points Most diagnoses can be made by clinical evaluation. Infection precautions should be maintained when examining patients with bilateral red eyes. Important danger signs are vomiting, halos around lights, fever, decreased visual acuity, proptosis, and impaired extraocular motility. Pain in the affected eye in response to shining light in the unaffected eye when the affected eye is shut (true photophobia) suggests a corneal lesion or uveitis. If pain resolves with a topical anesthetic (eg, proparacaine) cause of pain is a corneal lesion. Hammering or drilling on metal is a risk factor for occult intraocular foreign body. Sudden visual loss EH All presentations of sudden persistent loss of vision require an urgent ophthalmology consult. Transient Ischemic attack – Amaurosis Fugax Monocular viasul loss usually lasts seconds to minutes, may last 1-2 hrs. vision returns to normal Essentially normal fundus exam, sometimes embolus seen Other neurological signs associated with TIA Investigate as for TIA Management as for TIA Central retinal vein occlusion Sudden painless loss of vision Risk factors – age, HT and DM Visual acuity changes depending on severity and duration of illness Fundus – large areas of hemorrhage Screen for DM/HT and manage same Urgent referral to Ophthalmologist Central retinal artery occlusion Sudden painless loss of vision Visual acuity< 6/60 Relative afferent papillary defect marked Fundus – pale arteriolar and venular narrowing, abnormal red reflex Urgent ESR/CRP to rule out arteritis Urgent referral to ophthalmologist Management as for TIA Optic neuritis Painless loss of vision over hours to days Varying degress of visual loss Reduced visual acuity, colour and contrast vision Usually unilateral but may be bilateral Females 18-45 most commonly Signs: o RAPD o Decreased colour vision o Patchy visual field defects o Swollen optic disc o Other focal neurologic signs Urgent referral to ophthalmologist and neurologist for urgent MRI and Need for systemic steroids Giant cell arteritis Typically age >50 years Raised ESR and CRP Symptoms o Temporal headache o Scalp tenderness o Jaw claudication o Fever and night sweats o Muscle pain and weakness Signs o RAPD o Poor visual cuity o Papable, tender nin-pulsatile temporal artery o Swollen optic disc Management: o Urgent markers – ESR/CRP o Urgent referral ophthalmologist/ neurologist o Temporal artery biopsy to confirm diagnosis o Oral steroids Retinal detachment Separation of sensory retina from retinal pigment epithelium commonly due to predisposing retinal defect Painless loss of vision, recent h/o increased visual floaters/flashes; dark shadow in vision of affected eye h/o myopia and previous trauma increases risk signs o reduced visual acuity o abnormal red reflex o detached retina may be seen management: o bed rest o urgent ophthalmology consult o surgery Foreign bodies Conjunctival Corneal DIS H DIS H One of the commonest eye related presentation to the emergency department. Though most case may be managed expediently, the condition is associated with significant patient discomfort and morbidity if not properly managed. Any foreign body penetration of the cornea or retained foreign body will require urgent referral to ophthalmologist - immediate consult by phone. History: Type of foreign body: organic vs. inorganic material o Organic material may lead to infection o Metallic FB – rust rings with persistent inflammation and epithelial defect Velocity of impact o High speed motor drilling without eye protection – penetrating corneal/ sclera injury Examination Visual acuity Slit lamp o Size, site, nature of FB and depth of penetration Examine cornea, AC, iris, pupil and lens for any distortion – evidence for penetrating ocular trauma Evert eyelids to exclude retained FB Treatment/ investigation Topical anesthesia Foreign body removal under slit lamp Rust ring removal by ophthalmologist or experienced ED physician Fluorescein to assess epithelial defect Topical antibiotic (qid) and cycloplegic for comfort No need for continued topical anesthetic If central corneal FB – epeithelial defect to be closely followed up with ophthalmologist Patient to avoid contact lens use for at least a week or resolution. Reasons for urgent referral < 24 hrs. FB not completely removed Underlying opaque defect s/o abscess Persistent epithelial defect after 3 days Ocular burns Caustic Flash burns Thermal DIS H DIS H DIS H Always have high degree of suspicion in case of children presenting with ocular burns for un-explained Non-accidental injury(NAI) Chemical Burns History Time since injury, mechanism of injury Check in patients with facial injuries Type of chemical – acid or alkali o Alkali more harmful – lime, mortar, plaster, drain cleaner or ammonia etc. o Acids – toilet cleaner, car battery fluid, pool cleaner etc. First aid at scene and on transit Examination Topical anesthesia and systemic analgesia if indicated Management of concurrent injuries Assess degress of vascular blanching particularly at limbus → proportional to severity of burn Treatment Eye irrigation for chemical burns – o Check pH optimum 6.5 – 8.5 acceptable, goal neutral pH 7.4 o Commence iriigation with 1L of neutral solution e.g. NS, Hartmanns o Evert eyelid – clear debris o Use Morgan lens if available o Review after 1L irrigation – wait 5 mins before rechecking pH o Recommence irrigation if target pH not reached o May need at least 30 minutes in case of severe burns Test and record visual acuity Contact poisons information or chemical manufacturer for any further information Topical antibiotic drops, cycloplegics and mydriatics. Urgent ophthalmology consult and review if any visual acuity loss or corneal opacification Complications Acid quickly precipitates the superficial tissue proteins of the eye, producing the typical "ground glass" appearance of the cornea. Penetration is limited by local buffering and barrier effects of the precipitated proteins. Damage sustained secondary to acid burns in most cases is immediate and limited to the area of contact. The posterior segment of the eye rarely suffers injury, and there are usually no late effects such as cell disruption or tissue softening. Alkali burns are more severe, and results are frequently unsightly and disastrous. In general, the higher the pH of the alkali, the more damage. In a short period, strong alkali can penetrate the cornea, anterior chamber, and the retina, with destruction of all sensory elements, thus causing complete blindness. Severe chemosis, blanched conjunctiva, and an opacified cornea obscuring view of the iris or lens may occur. The penetration of alkali can continue for hours to days, resulting in globe perforation. The conjunctiva, and scleral blood vessels and collecting veins of the anterior chamber may be destroyed, leading to secondary glaucoma. Chronic inflammation of the iris and ciliary body (iridocyclitis) and adhesions between lens and iris (posterior synechiae) are possible complications of ocular burns. Other complications of eye burns include ectropion (lid deformity), cataract formation, scarring and marked revascularization of the cornea, and scarring of both palpebral and bulbar conjunctiva with resulting adhesions between the lids and globe (symblepharon). Thermal burns Clinical Findings Injury due to thermal burns of the eyelids, cornea, and conjunctiva may range from minimal to extensive. Superficial corneal burns have a good prognosis, though corneal ulcers may occur as a result of loss of corneal epithelium. Thermal burns of the skin of the eyelids may be first, second, or third degree. Conjunctival hyperemia is noted. The cornea may show diffuse necrosis of the exposed corneal epithelium in the interpalpebral area. Corneal haze due to corneal edema is frequently seen in thermal burns of the cornea and may lead to decrease in vision. Treatment Provides systemic analgesia Mydriatic agent instillation and Urgent ophthalmological consult Flash burns History Electric arc welding or sun lamp without eye protection Extreme sunlight exposure especially in snow Symptoms typically occur within several hours Intense pain, red eyes usually bilaterally, blepharospasm and tearing Examination Topical anesthesia both therapeutic and for ease of examination Check visual acuity Slit lamp – widespread superficial epithelial defect staining with fluorescein Treatment Topical antibiotic QID and cycloplegic e.g. Homatropine 2% BD for comfort for three days To represent if symptoms have not appreciably improved after 24 hours Follow If required – non-urgent within 3 days. Glaucoma DIS H Glaucoma is an acquired chronic optic neuropathy characterized by optic disk cupping and visual field loss. It is usually associated with elevated intraocular pressure. Etiology Primary glaucoma o Open angle Primary open angle Normal tension o Angle closure Acute Subacute Chronic Congenital glaucoma Secondary glaucoma o Pigmentary o Exfoliation o Lens changes Dislocation Advanced cataract phacolytic o Uveal tract changes Uveitis Posterior synechiae Tumor Ciliary body swelling o Trauma Hyphema Angle contusion Peripheral anterior synechiae o Post operative o Neovascular DM Central retinal vein occlusion IO tumor o Iatrogenic – steroid induced Absolute glaucoma – end point of all types – hard sightless, often painful eye. Pathophysiology The mechanism of raised intraocular pressure in glaucoma is impaired outflow of aqueous resulting from abnormalities within the drainage system of the anterior chamber angle (open-angle glaucoma) or impaired access of aqueous to the drainage system (angle-closure glaucoma). Treatment is directed toward reducing the intraocular pressure and, when possible, correcting the underlying cause. Although in normal-tension glaucoma intraocular pressure is within the normal range, reduction of intraocular pressure may still be beneficial. The most significant type of glaucoma presenting to ED, with significant morbidity outcomes is Acute AngleClosure Glaucoma. Acute Angle-Closure Glaucoma Primary acute angle-closure glaucoma occurs in eyes with narrow anterior chamber angles, such as in the older age groups, hyperopes, Inuits, and Asians Etiology May be precipitated by – Pupillary dilation from sitting in the dark – Stress – Pharmacologic mydriasis for ophthalmologic examination (rarely) – Medications with anticholinergic or sympathomimetic activity Secondary acute angle-closure glaucoma may occur in uveitis Clinical findings Extreme ocular pain Blurred vision, typically with halos around lights Nausea and vomiting Red eye, cloudy cornea, usually with a moderately dilated, non-reactive pupil Intraocular pressure usually over 50 mm Hg, producing a hard eye on palpation Diagnosis Markedly elevated intraocular pressure with shallow anterior chamber in both eys Must be differentiated from conjunctivitis, acute uveitis and other corneal disorders Treatment Immediate referral and early consultation with ophthalmologist with early review 500mg IV acetazolamide, followed by 250mg orally QID If no response, consider 1-2 g/kg of osmotic diuretic e.g. IV mannitol or urea After IO pressure is reduced, topical 4% pilocarpine, 1 drop every 15 min for 1 hour, then QID – used to reverse angle closure Topical β-blocker timolol 0.5% one drop and topical α-agonist Iopidine 0.1% one drop Topical steroids after ophthalmology consult Definitive treatment is generally laser or surgical peripheral iridotomy usually done bilaterally. Ocular trauma Lid Laceration Any laceration other than superficial skin that involves the lid margin will need ophthalmological referral. (Check for tetanus immunisation status). An eyelid laceration is a potential penetrating eye injury until proven otherwise. History Four basic questions are: which eye is injured? how did it happen? when did it happen? what are the symptoms? Nature of injury – was there any possibility of penetration into the lid/orbit? Examination Wound examination – size and depth. All wounds should be explored fully for extent of damage. Visual acuity. Superficial ocular examination with magnification to assess for any corneal/conjunctival laceration or penetration. Further ocular examination including dilated fundus examination as determined by history and examination findings. Treatment/Investigation Orbital X-Ray or CT if indicated for foreign bodies or orbital fracture. If superficial laceration: Clean the area and surrounding skin with antiseptic such as Betadine. Subcutaneous anaesthetic with vasoconstrictor (2% Lignocaine with Adrenaline). Irrigate and debride the wound thoroughly with saline. Identify foreign bodies if applicable. Suture with a 6/0 non-absorbable suture. When to refer? Referral to an ophthalmologist: If the eyelid laceration is associated with ocular trauma requiring surgery such as ruptured globe or intraorbital foreign body. If the laceration position is nasal to either the upper or the lower eyelid punctum, for the possibility of damage to the nasolacrimal drainage system. If there is extensive tissue loss or distortion of the anatomy. If there is full thickness laceration or the laceration involves the lid margin. Broad spectrum antibiotic cover if there is significant risk of contamination, or debridement of necrotic tissue. Blunt Ocular trauma Blunt trauma to the eye may result in considerable damage to the intraocular contents. Fracture of the orbital wall may occur due to the transfer of mechanical energy to relatively thin orbital bone. Ruptured globe Trauma of sufficient force may result in globe rupture and typically occurs in the areas where the scleral wall is thinnest: at the limbus (which would be visible via the slit lamp) or Behind the insertion of the rectus muscle (which would result in reduced ocular motility, loss of red reflex and vitreous bleed). Examination Visual acuity. Ocular movements – if there is considerable eyelid oedema, carefully lift up the lid while viewing the eye to ensure there is no obvious rupture. Reduced movement may suggest ruptured globe or orbital wall fracture. Slit lamp – looking for evidence of rupture (often at the limbus). Examine for blood in the anterior chamber. Examine the eyelid for lacerations. Ophthalmoscopy – Red reflex (missing in intraocular haemorrhage or retinal detachment). Look for any retinal pathology (after dilating the pupil). Investigations CT scan (axial and coronal) for orbital wall fracture if indicated Follow up - When to refer? Non-urgent referral within 3 days if the above findings are negative. Urgent referral to ophthalmologist - immediate consult by phone if findings are suggestive of intraocular haemorrhage, ruptured globe or orbital wall fracture Treatment Topical antibiotic drops for superficial trauma Penetrating Ocular trauma All penetrating trauma require urgent referral to ophthalmologist - immediate consult by phone following appropriate pre-op workup. History Mechanism of trauma – any history suggestive of a penetrating trauma. The type of projectile and the likely velocity (e.g. low or high) should be documented. Small projectiles at high velocities increase the likelihood of penetrating trauma. Symptoms include loss of vision, pain on movement and diplopia. Was the patient wearing eye protection? Any previous history of ocular trauma or previous surgery is to be documented and may suggest reduced integrity of the wall of the globe. Examination Examination may only need to be cursory if the trauma is obvious otherwise: – Visual acuity. Direct ophthalmoscopy – loss of red reflex may suggest retinal trauma or detachment. Slit lamp – looking for distorted anterior chamber structures or corneal/scleral breaks. Treatment Ensure nil by mouth status. Strict bed rest. Injectable analgesia/antiemetic if required. CT scan of the orbit to exclude retained ocular/orbital foreign body after discussion with ophthalmologist. Shield (not pad) the eye making sure not to increase the intraocular pressure with further loss of ocular contents. No ointment for penetrating eye injury. Check for tetanus immunisation status as per current protocol. Commence broad spectrum IV antibiotics. Orbital Cellulitis Orbital Pre-orbital DIS H DIS H Cellulitis as previously defined may involve the tissues anterior to the orbital septum (periorbital cellulitis) or within the orbit (orbital cellulitis). Characteristic Age Organisms Pathophysiology Clinical features Periorbital swelling Proptosis Extraocular eye movements Fever Investigations CT scanning Complications Treatment Orbital cellulitis Children less than age 3 S. Aureus, S. Pneumoniae, H. Influenzae (less due to universal immunisation) Hematogenous seeding or direct extension from ethmoid sinus Periorbital cellulitis Any age S. Aureus Present, more prominent Present Present Restricted Absent Normal Contiguous spread most common Usually present Usually absent WCC, cultures may be +/- Indicated if any eye movement disability – positive for collection/ soft tissue swelling Subperiosteal abscess, threatens integrity of eye. Intracranial extension rare IV antibiotic therapy directed against S.aureus, pneumococcus and H.influenzae Ceftriaxone/dicloxacillin Urgent referral to ophthalmology Leucocytosis and blood cultures usually positive Lumbar puncture indicated if systemically unwell Not indicated Retro-orbital changes usually absent May serve as focus for metastatic bacterial disease, particularly meningitis Same as orbital cellulitis Semi-urgent ophthalmology referral