* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download loading dose
Plateau principle wikipedia , lookup
Polysubstance dependence wikipedia , lookup
Orphan drug wikipedia , lookup
Compounding wikipedia , lookup
Psychopharmacology wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Pharmacognosy wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Drug design wikipedia , lookup
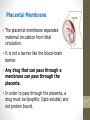
Pharmacogenomics wikipedia , lookup
Prescription costs wikipedia , lookup
Neuropharmacology wikipedia , lookup
Drug discovery wikipedia , lookup
Theralizumab wikipedia , lookup
Introduction to Drug Action The Interplay of Pharmacotherapeutics, Pharmacokinetics and Pharmacodynamics 1 Pharmacotherapeutics Pharmacotherapeutics is the achievement of the desired therapeutic goal from drug therapy. • Pharmacotherapeutics is the study of the clinical purpose—the indication—for giving a drug. • The clinical purpose can be to induce a cure or prevent a problem. Nurses should question medication orders if the intended pharmacotherapeutics of a drug does not correlate with the patient’s reason for receiving drug therapy. 2 Off-label Medications • Off-label use is defined as the use of a medication for any purpose that is not FDA studied or approved. • May be off-label for: • Non-approved Diagnosis • Non-approved dosage of medication (higher or lower than approved) • Non-approved client population (child, pregnancy, etc.) 3 Pharmacokinetics (Kinetic=Movement) Pharmacokinetics is the movement of the drug particles throughout the body. • Absorption - The movement of the drug from the site of administration into the bloodstream. • Distribution - The movement of the drug into the cells. • Metabolism - The conversion of the drug into another substance or substances. • Excretion - is the removal of the drug from the body. 4 Process by Which Drugs Move Through the Body Drugs cross cell membranes in one of three ways: 1. They can pass between the spaces or channels between the molecules in the membrane. 2. Drugs can pass through the cell membrane with the help of a transport system. 3. Drugs can penetrate the cell membrane directly. The chemistry of the drug particles also affects the movement of particles throughout the body. 5 Absorption • Several variables affect the rate of drug absorption. – Absorption is dependent partly on the route of administration – Absorption is affected by the speed at which the drug dissolves • Drugs that are administered orally generally take the longest to be absorbed. – Food or other drugs can interfere with absorption. 6 Absorption (cont.) Drugs given parenterally (IM, IV, SubQ) are absorbed more rapidly than drugs given orally. – Intramuscular absorption is somewhat more rapid than subcutaneous absorption. – Drugs that are administered intravenously are placed directly into the bloodstream. • Lipid (fat) solubility alters absorption. • pH affects absorption. • Blood flow also affects the rate of absorption—the greater the volume of blood flow > the faster the rate of absorption. 7 Distribution The distribution of a drug throughout the body depends on three factors: 1. Blood flow to the tissues, 2. The drug’s ability to leave the blood, and 3. The drug’s ability to enter cells. • The drug is transported to the tissues and cells through the circulatory system. • Most drugs do not produce their effect while in the blood. 8 Protein-Bound Drugs Protein binding of drugs affects the distribution of a drug. • When the drug is bound to protein, it is unable to pass through the capillary walls as protein molecules are large. • The bonds will dissolve in time, and the drug molecules will become free and active. • When the patient has a lower-than-expected protein level, the distribution of the drug is altered. 9 The Effects of Administering ProteinBound Drugs Highly Protein Bound Drug Loosely Protein Bound Drug 10 Blood–Brain Barrier • The capillary bed that services the brain is different from other capillary beds. • Instead of wide spaces between the cells in the capillary walls, the cells are packed tightly together. • This prevents drug molecules & other foreign substances from passing through and entering the brain. • The purpose of the blood–brain barrier is to keep toxins and poisons from reaching the brain. • This can prevent medication distribution. 11 Placental Membrane • The placental membrane separates maternal circulation from fetal circulation. • It is not a barrier like the blood–brain barrier. • Any drug that can pass through a membrane can pass through the placenta. • In order to pass through the placenta, a drug must be lipophilic (lipid-soluble) and not protein bound. 12 Metabolism (Biotransformation) Metabolism of drugs occurs primarily in the liver. • Physiologic factors that impair the functioning of the liver decrease the ability of the liver to metabolize drugs. • When drugs are metabolized, they are changed from their original form to a new form. • Drugs are generally metabolized from substances that are lipophilic into substances that are hydrophilic (water soluble) for easy excretion. 13 Metabolites A product of metabolism is called a metabolite. • Drugs that are metabolized are generally changed into an inactive form. • Metabolism can convert a drug that has little or no therapeutic effect in its original form into an active form. • Drugs that are inactive until metabolized into an active form are called pro-drugs. • An active metabolite may cause a different and potentially harmful effect. 14 First-Pass Effect Metabolism occurs at different rates for different drugs. • The % of drug that is metabolized each time the drug passes through the liver is the same • Drugs that are highly metabolized lose much of their effectiveness after this first pass through the liver. • This loss of effectiveness is called the first-pass effect. • Drugs that experience a high first-pass effect may need higher or more frequent oral doses to achieve a therapeutic level of circulating drug. 15 P-450 System • Liver metabolism is predominantly achieved by specific enzymes. These enzymes make up the cytochrome P-450 system. • P-450 metabolism is genetically determined. When a large quantity of one of these enzymes is present, more metabolism can occur through this pathway. • This increase in metabolism rapidly decreases the amount of circulating drug. • Some drugs either induce or inhibit the P-450 system, altering metabolism of other drugs. 16 Excretion • Excretion is the process of removing a drug, or its metabolites, from the body. • The most common route for drug excretion is through the urine. • Drugs are also excreted through feces, sweat, tears and bile. • Diseases and pathological changes in the kidney decrease the effectiveness of the kidney in drug excretion. 17 Half-Life of a Drug The combined processes of metabolism and excretion are responsible for the elimination of a drug from the body. • The amount of time that is required to remove half (50%) of the blood concentration of a drug is called half-life. • Drugs have various half-lives, based on their pharmacologic properties. • In one half-life rotation, a percentage of the drug molecules present in the blood is eliminated. 18 Steady State The point at which the amount of drug being administered and the amount being eliminated are equal • Increasing the dose has no effect on how quickly steady state can be achieved. • Steady state is achieved based on the amount of time required for 4-5 half-lives to occur. • The full pharmacotherapeutic response of a particular drug dose is measured when the drug has achieved steady state. 19 Clearance The rate at which drug molecules disappear from the circulatory system is effected by several factors. • This rate is called clearance or clearance rate of a drug. • Renal excretion and hepatic metabolism are the major modes of clearance. • Age & gender of the patient can also alter the clearance of some drugs. • Even though a drug’s clearance is shown to be statistically altered, this statistical difference does not necessarily create a clinical difference. 20 Pharmacodynamics Pharmacodynamics is the biologic, chemical, and physiologic actions of a particular drug within the body. • The pharmacodynamics of a drug are responsible for its therapeutic effects and sometimes its adverse effects. • Drugs cannot create new responses in the body; they can only turn on, turn off, promote, or block a response that the body is inherently capable of producing. 21 Drug–Receptor Interactions Most drugs create their effects in the body by attaching to special sites called receptors. • At the receptor site, the drug is able to stimulate the cell to act in a way that the cell is designed to act. • Each type of receptor is responsible for producing a particular effect in the cell. • An agonist causes the cell to act, or “turn on”. • An antagonist prevents something else from attaching to the cell therefore blocking an action. 22 Receptor Occupancy Theory • Single-occupancy theory – The intensity of the body’s response to the drug is directly related to the number of receptors occupied by the drug. – The maximum response occurs when all of the receptors have drug molecules attached. • Modified occupancy theory – Different drugs have different strengths of attractions, or affinity, for receptor sites. – Once a drug is attached to a receptor, it has different abilities to stimulate the receptor. 23 Receptor Sensitivity • Changes in receptor sensitivity – Receptors are not static. – Continual stimulation from an agonist usually makes the drug less effective. – Continual blockage from an antagonist usually makes the drug more likely to react. • Non-receptor responses – Drugs exert their effect by reacting physically or chemically with other molecules in the body. 24 Variables that Influence the Dose of a Drug • Potency and efficacy – The level of the drug needed in the body to produce an effect • Maintenance and loading doses – Maintenance dose—daily dose – Loading dose—larger than usual dose to reach a therapeutic effect quicker • Therapeutic index – The difference between an effective dose and a toxic dose 25 Potency and Efficacy A certain level of drug must be present in the body to produce any effect at all. • This level is called the minimum effective concentration. • The strength of the response to a drug increases proportionately as more drug is given. • The amount of a drug that must be given in order to produce a particular response is called the potency of a drug. • How well a drug produces its desired effect is called efficacy. 26 Maintenance and Loading Doses • Because people are unique, how individuals respond to a drug dose varies. • The dose that is required to produce the therapeutic response in 50% of the population is called the effective dose 50% (ED50). • The dose that is given consistently over time is called the maintenance dose. • Patients who are started on drug therapy using the standard maintenance dose arrive at steady state after 4-5 half-lives. 27 Maintenance and Loading Doses (cont.) • The patient’s medical condition may warrant immediate and full drug effect. – If this is the case, a larger dose than usual is given initially. – This initial large dose is called a loading dose. – The loading dose is computed so that after some of the drug is eliminated, the drug concentration in the body is still in the therapeutic range. 28 Therapeutic Index • A lethal dose is computed in a laboratory setting and analyzed statistically. • The point at which the dose would be fatal in 50% of the population receiving that dose is called lethal dose 50% (LD50). • To determine the safety of a drug, the ED50 is compared with the LD50. • The relation of ED50 to LD50 is called the therapeutic index. TI = ED50 / LD50 29 Therapeutic Index (cont.) • If the ED50 is close to the LD50, the mathematical ratio of the two values will equal a number close to one. • When the ED50 and the LD50 are close to 1, the drug is considered to have a very narrow therapeutic index. Questions • Would a drug with TI close to 1 be a safe drug? • Why would we use such a drug? 30 Drug Dosage and Blood Concentration • As drug levels within the body increase, the patient is more likely to experience adverse effects from drug therapy. Drug Dosage = Adverse Effects • To help determine whether a drug’s dose is sufficient to be in the therapeutic range, but not so high as to cause adverse effects, blood levels of the drug may be measured. Narrow T.I. drugs are more likely to use blood levels 31 Assessment and Evaluation The Nursing Process Assess Evaluate Plan Implement 32 Question One aspect of pharmacotherapeutics is the study of the clinical indications of drug therapy. – A. True – B. False 33 Question One aspect of pharmacotherapeutics is the study of the clinical indications of drug therapy. – A. True – B. False Pharmacotherapeutics is the study of desired therapeutic goal from drug therapy, the clinical purpose—the indication—for giving a drug and the desired effect of the drug. 34 Question What will be the result of administering a highly protein-bound drug to a patient with liver failure? – A. There will be no significant difference in the distribution of the drug. – B. The drug will reach the target cells more quickly and therefore will not be as effective. – C. The drug will reach the target cells more quickly, which could result in a toxic effect. – D. The drug will take longer to reach the target cells, delaying the onset of action. 35 Question What will be the result of administering a highly protein-bound drug to a patient with liver failure? – A. There will be no significant difference in the distribution of the drug. – B. The drug will reach the target cells more quickly and therefore will not be as effective. – C. The drug will reach the target cells more quickly, which could result in a toxic effect. – D. The drug will take longer to reach the target cells, delaying the onset of action. 36 Rationale Patients with liver failure have lower levels of protein and albumin in their blood than patients without liver failure; Therefore, the drug will reach the target cells more quickly, which could lead to a toxic effect. Remember that all recommended drug dosages are calculated based on a patient with normal protein levels and liver functioning! 37 Question All drugs have some type of adverse effect(s). – A. True – B. False 38 Question All drugs have some type of adverse effect(s). – A. True – B. False 39 40