* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Final Exam Study Guide
Survey
Document related concepts
Transcript
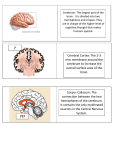
BIOBASES FINAL EXAM STUDY GUIDE Topics/Cues Genderal Nervous System Structure CNS PNS SNS ANS P-SyNS SyNS General Nervous System Organization wrapping dorsal vs. ventral Gray and white matter Major Brain Landmarks (6) Major Brain Lobes (4) Imaging Modalities and Uses (7) Nervous System Development Divisions and Subdivisions Central Nervous System Brain, spinal cord Peripheral Nervous System Divisions: Somatic Nervous System: receives sensory information from periphery conscious control of muscles WILLFUL or CONSCIOUS aspects of movement/sensation Autonomic Nervous System: UNCONSCIOUS aspects of movement/sensation of organs (e.g., heart, lungs, etc.) Divisions: Parasympathetic Nervous System: mostly inhibitory – homeostasis Sympathetic Nervous System: excitatory – fight or flight From Periphery Central neurons wrapped in myelin – endoneurium groups of neurons (fasicles) wrapped in perinuerium groups of fasicles and blood vessles (nerve) wrapped in epineurium Afferent nerves meet at Dorsal root ganglion From Central Periphery Efferent nevers have their somas at the spinal cord on ventral side Gray matter is the cell bodies; found on surface or cortex and center of spinal cord. White matter is b/c of myelin—axons of neurons (send info); inside cortex and on outside of spinal cord. Central sulcus: divides brain in half from anterior to posterior. Pre-central gyrus: anterior to central sulcus primary motor cortex Post-central gyrus: posterior to central sulcus somatosensory cortex Longitudinal fissure: seperates brain hemisphers Lateral fissure: seperates temporal lobe from frontal cortex Parietal-Occipital sulcus (internal): seperates occipital lobe from parietal lobe Frontal lobe: organization, planning, thinking Temporal lobe: memory, hearing Parietal lobe: association area Occipital lobe: visual processing X-ray: good for structural (i.e., bone) imaging can damage cells; projection CT: use X-rays for structural imaging; not projection rotate x-ray around head MRI: use mag rays for structural imaging; clear definition of white/gray matter PET: use radiation for functional imaging: projection; need time for radioactive material to collect in area of brain of interest. SPECT: functional: cheap version of PET fMRI: images of increase O2 flow; functional and structural: not projection DTMRI: used to track motion of fluid in brain (how nerve travels in space) Embryonic Phase: 1 phases (embryonic, infant) piaget’s stages Cortex Development Development Pathologies 4 types, 11 total disorders Pervasive Disorders Pituitary Hormones (8) o simple mitosis until ~32 cells; then, specialization begins o Day 15 = formation of neural streak in ectoderm o Day 22 = neural tube forms o Day 25 = neural tube closes o Day 28 = 3 swellings form: prosen-. mesen-, and rhombencephalon o etc…. o Mylenation isn’t completed until puberty Infant phase: o 9 – 10 months: motor neuron mylenation o 2 – 4 years: occipital lobe fully develops o 5 – 6 years: lateralization completes, plasticity lessened o 12 – 16 year: frontal lobe fully develops Piaget: o Sensorimotor, 0 – 2 years: object perm., lang., myelin of vis., sense, motor; frontal lobe density incr. o Preoperational, 2 – 7: mental rep. of objects; words/pics to express; lateralization completes o Concrete Operational, 7 – 11: logical think; frontal lobe keeps develpng o Formal Operational, 11+: abstract thinking; frntl lobe close to mature develops from inside – out neural precursors divide near ventricles, then migrate to cortex via glial cells chemo attractors and repellents guide path of neuroplasts Dorsal Induction Pathologies: (3 – 4 weeks) o non-closure of neural tube = death o Spina Bifida: incomplete closure of inferior end of tube o Anencephaly: “no brain” – no closure of tube at superior end o Encephalomeningocele: pouch of CSF/water in brain coverings o Hydrocephalus: extremely large ventricles (too much fluid) Ventral Induction Pathologies: (5 – 6 weeks) o Holoprosencephaly: “the brain is one” – does not divide (cyclopia) Proliferation Pathologies: (2 – 4 mn.) o Micocephaly: “small brain” – smaller number of neurons Migration Pathologies: (3 – 5 mn.) o Agryria: “no gyri”; MR, seizures (less surface area for neurons) o Pachygyria: “elephant gyri”; developmental delays o Polymicrogyria: “many small gyri”; often due to uterine infection; MR, seizures o Heterotopia: homogenous white and gray matter; males = stillborn, females = normal + seizures; less efficient processing PDDs: compulsions, social, language o Austistic: onset prior to age 3; genetic (MZ = 36 – 96%), brain diffs = corpus collasum, frontal lobe, neural migration probs o Asberger’s: normal or above avg intell; stereotyped bxs o Rett’s: 5 – 48 months onset; decelerated head growth, loss of social engagement; MR o Child Disintegrative Disorder: loss of previously acquired skills by age 10 FSH – grow follicles LH – ovulation Prolactin – milk production ACTH – adrenocorticotropic hormone; sends to adrenal glands to produce cortisol 2 Sexual Development Milestones Arousal and Consciousness Circadian Rhythms Motivation, Eating, Addition Relationships Leptin Mechanism of Hunger/Satiety Cannabinoid Visual Pathway Growth hormone TSH – thyroid stimulating hormone Oxytocin – contractions, lactation, bonding ADH – anti-diuretic hormone (blood volume) 6 Weeks: o H-Y antigen in males causes gonads become testes o lack of antigen in females; gonads become overares 3 months: o Testes Mullerian inhibiting substance and androgens o MIS degeneration of mullerian ducts o androgens male organs Pathologies: o Androgen Insensitivity Syndrome: no male sex organs (except testes b/c of H-Y antigen) no mullerian tubes (b/c of MIS) o Persistent Mullerian Duct Syndrome: mullerian tubes stay Reticular Activating System: nuclei in the pons, medulla, and brainstem o locus coeruleous (novel stimuli) o raphe nuclie (sleep) o substantia nigra, ventral teg area (DA) o cholinergenci basal forebrain receives inputs from above nuclei and projects to entire cortex SCN: suprachiasmic nuclei (over optic chiasm) uses genetic transcription to oscillate over a long time period DA pathway in ventral teg and nucleus acumbens (increase of DA in nucleus acumbens is necessary for natural reinforcers). produced by fat tissues (adipose) high levels increases metabolism, low levels decrease metabolism Too much fat: adipose leptin leptin hypothalamus (arcuate nucleus) TSH and ACTH = increased metabolism increased MSH decreased feeding bxs Too little fat: adipose not enough leptin low leptin hypothalamus (arcuate nucleus) low TSH and ACTH = decreased metabolism decreased orexin production = feeding bxs Satiety: gastric dimension and nutrients intestinal nutrients liver senses glucose levels brain estimation of time delay INCREASED 5-HT = less eating Receptors found in hypothalamus, limbic system, intestines, liver, adipose tissue, pancrease Retina (with rods, cones, horizontal cells, bi-polar cells, ganglion cells) Optic Tract (optic chiasm) – splits and retinal hemisphers project to ipsilateral LGN 3 Primary Emotions (6) Secondary Emotions Theories of Emotion Fear (brain parts) Agression (types and parts) Facial Emotion Wernicke-Geschwind Model of Language (7 areas, functions, deficits) Dual-Route Theory and deficits Lateral Geniculate Nucleus (of thalamus) Superior Colliculus (topographically mapped) – controls attention, head/eye move Visual cortex Definition: biologically based, innate; same for all humans Joy, sadness, fear, disgust, surprise, anger Sensory inputs go directly to limbic areas Definition: dependent on learning and social environment pride, shame, embarrassment, anxiety Sensory inputs must first go to cortex and then to limbic areas Frontal cortex is largely responsible James – Lange: physiological changes perceived emotion Cannan – Bard: emotional experience can be independent of physiological changes Cortex is not necessary Amygdala: largely responsible for fear response lesion = lack of fear response Hypothalamus: hormone release b/c of fear Predatory Agression: o for killing; low SNS activation o lateral HYPOTHALAMUS Offensive Agression: o emotional; high SNS activation o medial HYPOTHALAMUS AMYGDALA is CRITICAL Left half of face is more expressive for SPONTANEOUS: right brain is where emotional processing is concentrated Right half of face is more expressive for POSED: left brain is where language is processed. Broca’s area: generates speech; deficit = problems creating speech, good RC Primary motor cortex: sends commands to muscles of mouth for verbal speech, to hand/arms for written. Arcuate fasciculus: connects perceptive and productive areas of language. deficit = problems in repetition – ok speak and RC. Angular Gyrus: interpretation of visual language input. deficit = ok speech, no reading, no writing. Primary visual cortex: sensing visual information Wernicke’s area: language comprehension (association of language inputs). deficits = no comp, non-sensical speech, no semantics Primary Auditory cortex: sense auditory language Example: Response to heard question = o audtory cortex Wernicke’s area arcuate fasciculus broca’s area motor cortex Received words are processed either through lexical or non-lexical processing Lexical Route (temporal lobe): o known and practiced words o lexicon of known words located near WERNICKE’S AREA o Deficit: left temporal lobe lesions = inability to pronounce words based on specific memories i.e., well-known words Non-Lexical Route (frontal lobe): o uses rules of phonetics to interpret words o rules surround BROCA’S area 4 Memory Brain Areas Lashley vs. Hebb The Learning Neurons Long-Term Potentation / Depression Major Causes of Brain Damage (8) Effects of Brain Damage (3) CVAs how damage Neuronal Degeneration Regeneration (what will and what won’t) Plasticity o Deficit: left frontal lobe damage = inability to sound out new words Short-term: right orbital cortex Episodic / Spatial memory / Learning: hippocampus Object recognition: rhinal cortex (adjacent to hippo) Emotional Memory: Amygdala Sensory Relay: Thalamus Fornix / Mammillary Bodies: pathways in/out of hippo Procedural: Striatum - CEREBELLUM Lashley: thought memories were everywhere in the cortex Hebb: proposed that when a neuron fires at the same time as a post-synaptic neuron, the connection is strengthened. Dendritic spine has NMDA receptors – need two keys, Glut and voltage. when opened, allow influx of Ca++ second messenger AMPA receptors & No2 AMPA receptors allow influx of Na+ (glutamate receptor) LTP: o Ca++ activates CaM-KII enzyme = controls synthesis of receptors, phosphorylates the AMPA receptors, ps NO2 o spine / button splitting o CREB-1 (phosphorylated) permits synthesis of AMPA receptors LTD: o AMPA receptors = dephosphorylated = less sensitive to glut o AMPA receptors decrease in number, not replaced o CREB is turned off Genetic: faulty duplicatin of genes: Down’s, Turner’s, Klinefelter’s, Parkinsons, etc. Usually self-limiting Congenital: exposure to toxins, drugs, STDS, birth trauma Environmental: radiation, toxins, drugs, nutrition Neoplasms: aka cancer Cell Death: aka necrosis – externally causes or apoptosis – normal Cerebrovascular Problems: CVAs, Thrombosis – hypoxia = excess Ca++ Head Impact: trauma to brain – often damages area of brain opposite site of impact Infections: syphillis, strep, rabies, herpes, mumps, etc. inflammation of brain (encephalitis) or meninges (meningitis) Kill neurons: damage to nerve; damage to environment (e.g., glial cells); damage to pre/post-synaptic nerves Pressure: crowd out or place pressure on brain areas (e.g., neoplasms, meningitis, encephalitis) Diable neurons: myelin interference Previous theory: lack of blood supply to designated neurons = death Current theory: hypoxic (lack of O2) conditions cause NMDA receptors to allow Ca++ influx = fossilizing neuron – hippocampus especially affected. phagocytosis: “to eat” cells Anterograde: the distal segments die: swell, fragment in days Retrograde: the proximal segments: might live, might die CNS: almost non-existent growth inhibiting factors high in CNS PNS: hit-or-miss higher growth promoting factors o if myelin sheath still intact, more likely to reconnect o surrounding neurons may take place of dying axon (collateral sprouting) Ability of neurons to reorganize: brain can remap its functioning; more likely in 5 how does it work? Pharmacology terms suffixes kinetics actions Schizophrenia – Anatomical changes (4 + 1 comment) Theories of Schizo Anxiety Disorders (the circuit and pharmacology) Affective Disorders younger Rapid: short-term altered sensitivity of receptors Gradual: long-term; new connections formed Suffixes: PAM = benzodiazapine; AL = barbituate; CAINE = local anesthetic Kinetics: o Metabolism: breakdown of drug by the liver; varies person to person o Elimination: removal of drug by kidneys o Half-life: time required to eliminate half of drug Actions: o availability of neurotransmitter (NT) o release of NT o block reuptake of NT o alter autoregulation o alter synaptic NT (breakdown in synapse) o alter post-synaptic receptors (up/down reg. 2 – 3 weeks) small cortex large ventricles prefrontal cortex and amygdala abnormal smaller hippocampus no ongoing degerneration (seems to already be in place at onset) Dopamine Theory (Primary): o increase DA in mesolimbic path (ventral teg to limbic (amygdala, nucleus acumbens, hypothalamus) positive symptoms o decreased DA in mesocortical path negative symptoms Glutamate Theory: o Glutamate controls inhibition in mesolimbic DA system o Glutamate controls excitation in mesocortical DA system o Lack of glutamate = increase emotional/fear, decrease thinking, logic Other Factors: o pre-natal stress increases risk o pre-natal infections increases risk o stressful precursor prior to onset is common Senses & Thoughts excite amygdala amygdala excites HPA (hypothalamus, pituitary, adrenal) HPA cortisol excites hippocamus hippocampus inhibits HPA 5-HT increases hippocampal suppression of HPA ANXIOUS PERSONS HAVE TOO LITTLE INHIBITION = not enough 5-HT and not enough GABA treat by increasing 5-HT in synapse (SSRIs) or increase GABA (e.g., valium) Too much D, NE, 5-HT MANIA Too little “” DEPRESSION Pharmacology: o MAOIs: keep enzymes from breaking down monamines = more o TCAs: blocks reuptake of 5-HT and NE (safer) o SSRIs: block 5-HT reuptake 6