* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download The Argyle Care Home Service - Primary Care Pharmacists
Survey
Document related concepts
Orphan drug wikipedia , lookup
Polysubstance dependence wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Prescription drug prices in the United States wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Pharmacognosy wikipedia , lookup
Prescription costs wikipedia , lookup
Neuropharmacology wikipedia , lookup
Drug interaction wikipedia , lookup
Psychopharmacology wikipedia , lookup
Transcript
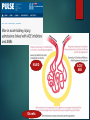
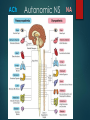
Primary Care Pharmacists Association Practice Pharmacists Group Symposium 2016 10th March 2016 : The Studio, Birmingham Priorities in the Management of Older People DR GRAHAM STRETCH, PRESCRIBING LEAD ARGYLE SURGERY & FLORENCE ROAD SURGERY, EALING, LONDON [email protected] @GRAHAMSTRETCH Well, the Glaxo pill protects my heart from the side effects of the Pfizer pill that prevents potential liver failure due to the Merck pill that minimises the risk of stroke posed by the Novartis pill that reduces blood clots caused by the Glaxo pill… The devil of it is I can’t remember the illness that started all this Activity Three ‘Brainstorm’ Walls 1. Physiological changes in aging 2. Common morbidity in the elderly 3. Drugs associated with adverse reactions / poor outcomes in the Elderly Post-it Notes Pharmacokinetics PB, Metabolism, Clearance, Elimination, BBB Pharmacodynamics GI motility = Constipation Sensitivity, Response, Compensation Orthostatic circulatory responses Blunting of reflex tachycardia=postural hypotension, On rising from rest, BP should increase doesn’t = postural hypotension = FALLS Postural control in dopamine receptors in stratum Static postural reflexes FALLS/fractures Prostatic hypertrophy, OAB, urethral dysfunction = Incontinence Cognitive function change in CNS = confusion The Geriatric Giants Bernard Isaacs (1924-1995) Professor of Geriatric Medicine, Birmingham, 1972 Geriatric Giants incontinence immobility instability(falls) intellectual impairment Falls Cognitive Constipation Impairment Delirium Incontinence Frailty Dehydration Pain Immobility Malnutrition Depression Resilience Functional abilities Minor Illness in Fit Older Person Minor Illness in Frail Older Person INDEPENDENCE DEPENDENCE Clegg et al, Lancet, Volume 381, Issue 9868, 2–8 March 2013, Pages 752–762 ADRs Most common drug groups associated with admission: NSAIDs 29.6% Diuretics 27.3% Warfarin 10.5% ACE 7.7% Antidepressants 7.1% Beta blockers 6.8% Opiates 6.0% Digoxin 2.9% Prednisolone 2.5% Clopidogrel 2.4% Pirmohamed, et al. BMJ 2004. 329; 15-19 Case 1 Case 1 AKI - iotrogenic 5 “Usual Suspects” NSAID ACE ARB Diuretic Antibiotics (aminoglycosides, cephalosporins) ‘Triple Whammy’ ACE, NSAID, Diuretic NSAID Diuretic ACE/ ARB Suspend metformin (risk of lactic acidosis) diuretic (worsening of dehydration) ACE (risk of AKI) NSAID (risk of AKI) At Review Aspirin - CHA2DS2-VASc=3, HASBLED=3 Anti Coag? eGFR 45 – metformin? Sulphonylurea? DPP-4 inh? CKD3A – review NSAID ‘Triple Whammy’ – combination of NSAID, diuretic and ACE in elderly (High risk combination BP, renal and cardiac) eGFR 45 (stop naproxen?) Bleeding risk – on Aspirin, Naproxen and SSRI – review & add PPI (stop naproxen?), also had prn gaviscon, Hb = 11.2, slightly low – Ferritin? Amlodipine and simvastatin 40mg – MHRA alert (risk of myopathy) switch statin or reduce to 20mg Citalopram 30mg >65yrs max 20mg (risk of QT prolongation) Switch naproxen, to paracetamol +/- codeine, topical NSAID Case 2 Hx 20 Mar 2000 Essential hypertension (XE0Uc) 01 Feb 2008 Rheumatoid Arthritis (N040..) 10 May 2002 Hypothyroidism (X40IQ) 01 Feb 2008 Dyspepsia - symptoms Dyspepsia 02 Sep 2002 Deep vein phlebitis (XE0VY) 27 Jun 2008 Morbid obesity (X40YQ) 02 Sep 2002 H/O: pulmonary embolus (14AC.) 19 Mar 2010 Osteoarthritis Hip pain (X75rv) 24 Nov 2005 Urinary incontinence (1A23.) 11 Oct 2010 Haemorrhoid (G84..) 24 Oct 2006 Knee joint operations (7K3..) 25 Sep 2012 Dry eyes (1B88.) 13 Dec 2006 Asthma monitoring (XM1Xb) 07 Jun 2013 Microcytic hypochromic anaemia (D00y1) 04 Aug 2007 Glaucoma 07 Jun 2013 Anaemia - iron deficiency 18 Dec 2007 Serum cholesterol raised (44P3.) 05 Sep 2013 Hodgkin's disease (B61..) 18 Dec 2007 Hyperlipidaemia 27 Mar 2014 Supraventricular tachycardia (Xa0k6) 01 Feb 2008 Indigestion (1954.) • • • Repeat File Amitriptyline 10mg Tablets Buprenorphine 10micrograms/hour transdermal patches Celluvisc 1% eye drops 0.4ml unit dose (Allergan Ltd) Co-dydramol 10mg/500mg tablets Dilzem XL 180 capsules (Teva UK Ltd) Domperidone 10mg tablets Folic acid 5mg tablets Gabapentin 100mg capsules Lacri-lube eye ointment (Allergan Ltd) Lactulose 3.1-3.7g/5ml oral solution Latanoprost 50micrograms/ml eye drops Levothyroxine sodium 25microgram tablets Levothyroxine sodium 50microgram tablets • • Omeprazole 20mg gastro-resistant capsules Oramorph 10mg/5ml oral solution (Boehringer Ingelheim Ltd) Paracetamol 500mg tablets Promethazine 25mg Tablets Salazopyrin EN-Tabs 500mg (Pfizer Ltd) Salbutamol 100micrograms/dose inhaler CFC free Scheriproct ointment (Bayer Plc) Seretide 125 Evohaler (GlaxoSmithKline UK Ltd) Simvastatin 40mg tablets Solifenacin 5mg tablets Trospium chloride 60mg modified-release capsules Warfarin 1mg tablets Warfarin 3mg tablets Warfarin 5mg tablets • • • • • • • • • • • • • • • • • • • • • • • Rationalise Try mirabegron for OAB - replace anti cholinergics, No INR recorded requested warfarin – indication? stop Pain relief Butrans 20, paracetamol 2 qds and oramorph 2.5-5mg 4hr prn record usage Stop amitriptyline / promethazine / domperidone repeat levothyroxine, salazopyrin, salbutamol and seretide. Simvastatin to be reviewed non-concordant - stop? New Rx Buprenorphine 20micrograms/hour transdermal patches - 4 patch - apply one as directed Gabapentin 100mg capsules - 100 capsule – I tds Mirabegron 50mg MR Tabs – 30 tabs – 1 OD Oramorph 10mg/5ml oral solution (Boehringer Ingelheim Ltd) - 300 ml - 5MLS WHEN REQUIRED UPTO 4-6 HOURLY Scheriproct ointment (Bayer Plc) - 30 gram - apply twice daily as needed (R) Levothyroxine sodium 25microgram tablets - 56 tablet - EVERY DAY (R) Levothyroxine sodium 50microgram tablets - 56 tablet – OD (R) Paracetamol 500mg tablets - 224 tablet - 2 FOUR TIMES A DAY regularily (R) Salazopyrin EN-Tabs 500mg (Pfizer Ltd) - 224 tablet - 2 TABLETS TWICE DAILY (AS ADVISED BY HOSPITAL) (R) Salbutamol 100micrograms/dose inhaler CFC free - 200 dose - 1-2 PUFFS WHEN REQUIRED (R) Seretide 125 Evohaler (GlaxoSmithKline UK Ltd) - 120 dose - ONE PUFF TWICE A DAY ADRs Constipation Opiates, antihistamines, iron, calcium channel blockers, anticholinergics Nausea and vomiting Many drugs Postural hypotension, falls Sedatives, Antiparkinson drugs, antihypertensives, alcohol, psychotropics Impaired cognition Most CNS drugs e.g TCAs, , anticholinergics Blood disorders Methotrexate, Carbemazepine, Sulphasalazine GI bleeds Aspirin, NSAIDs, Warfarin, SSRIs, Prednisolone Confusion Cimetidine, hypnotics, anticholinergics Blurred vision Anticholinergics, antihistamines, TCAs Renal failure ACEI, NSAIDs Hypertension NSAIDs Extrapyramidal effects Metoclopramide, prochloperazine, antipsychotic Anorexia Digoxin Altered taste ACEIs, metronidazole, zopiclone ACh Autonomic NS NA “Higher cumulative anticholinergic use is associated with an increased risk for dementia” Gray et al. Cumulative use of strong anticholinergics and incident dementia: a prospective cohort study. JAMA Intern Med. 2015;175:401-7 The Headlines Study suggests sleeping drugs can increase risk of Alzheimer’s. The Guardian, 27 January 2015 Popular sleep remedies and hay fever pills 'increase risk of Alzheimer's by more than 50%'. Daily Mail, 26 January 2015 Hay fever and sleeping tablets 'can increase risk of Alzheimer's and dementia'. Daily Mirror, 26 January 2015 Routine drugs for elderly ‘raise risk of dementia’. The Times, 26 January 2015 Hayfever pills and sleeping aids can 'significantly increase' risk of Alzheimer’s, says US study. The Independent, 26 January 2015 Hayfever drugs raise risk of Alzheimer's disease, say scientists. The Daily Telegraph, 26 January 2015 Dementia 'linked' to common over-the-counter drugs. BBC News, 27 January 2015 AChE Inh (eg Donepezil) Anticholinergics Risk for incident dementia and Alzheimer disease with 9-year cumulative anticholinergic use with 2-year lag time TSDD Follow-up time (person-years) Dementia Alzheimer Disease 0 6137 Number of Events 154 1-90 7861 208 0.89 0.71-1.11 172 0.94 0.74-1.20 91-365 4849 171 1.21 0.96-1.52 128 1.19 0.92-1.55 3661095 2461 94 1.15 0.88-1.52 80 1.30 0.96-1.75 >1095 3712 170 1.49 1.17-1.89 133 1.59 1.22-2.08 HR (95% CI) 1.00 Reference Number of Events 124 HR (95% CI) 1.00 Reference n=3434, mean follow-up 7.3y, 797 (23.2%) dementia (637 [79.9%] AD) “The use of medications with anticholinergic activity increases the cumulative risk of cognitive impairment and mortality.” Fox et al. Anticholinergic medication use and cognitive impairment in the older population: the medical research council cognitive function and ageing study. J Am Geriatr Soc. 2011 Aug;59(8):1477-83 Fox et al. 2011 Thirteen thousand and four participants from UK aged 65 and older. Worsening brain function: participants ACB score 5 + scored 4% lower test (MMSE). Increased death rate: End year 2: 20% people scoring 4 + vs. 7% scoring 0. Every extra ACB point scored odds dying ↑ 26% Cumulative risk both no. anticholinergic drugs & strength each drug’s anticholinergic effect “…a risk increase for dementia by the chronic use of drugs with anticholinergic properties…In terms of dementia prevention, centrally acting anticholinergic drugs should be strictly avoided, because of long-term dementia risk increase in addition to acute negative effects on cognition..” German, n=2600, Use anti-cholinergics associated ↑ risk dementia (HR: 2.081; p < 0.001), Classified strength AC activity (1 to 4) - dose effect – Level 1 – HR: 1.800; p < 0.001 – Level 2 – HR: 1.534; p = 0.105 – Level 3 – HR: 2.584; p = 0.002 – Level 4 – HR: 3.361; p < 0.001 Jessen et al. Anticholinergic drug use and risk for dementia: target for dementia prevention. Eur Arch Psychiatry Clin Neurosci (2010) 260:111–115 “Eighteen studies …(124 286 participants). Exposure …was associated with increased odds of cognitive impairment (OR 1.45, 95% CI 1.16- 1.73)...a unit increase in the ACB scale was associated with a doubling in odds of allcause mortality (OR 2.06, 95% CI 1.82- 2.33).” Ruxton, K., Woodman, R. J., and Mangoni, A. A. (2015) Drugs with anticholinergic effects and cognitive impairment, falls and all-cause mortality in older adults: A systematic review and meta-analysis. Br J Clin Pharmacol. doi: 10.1111/bcp.12617. (MAY 2015) “Prescribers should be aware…when considering anticholinergic medications for their older patients and should consider alternatives when possible” Gray et al. Cumulative use of strong anticholinergics and incident dementia: a prospective cohort study. JAMA Intern Med. 2015 Mar;175:401-7 Alternatives? TCA Depression SSRI Sertraline Citalopram Duloxetine Trazodone Neuropathic gabapentin pregabalin • ‘1st Gen’ – chlorpheniramine – diphenhydramine – promethazine SNRI Antihistamine Lyrica duloxetine • Current Indication? • ‘2nd Gen’ – loratadine – cetirizine OAB • Anti-Chol – – – – – oxybutynin tolterodine solifenacin trospium darfenacin • SNRI – duloxetine • B3 agonist – mirabegron Polypharmacy “…should be conceptually perceived as a ‘disease’ with potentially more serious complications than those of the diseases these different drugs have been prescribed for” Gafinkel et al. Arch Intern Med. 2010;170(18):1648–1654 Medicines Optimisation “a person-centred approach to safe and effective medicines use, to ensure people obtain the best possible outcomes from their medicines.” NICE guidelines [NG5] March 2015 Deprescribing “the process of tapering, withdrawing, discontinuing or stopping medications to reduce polypharmacy, adverse drug effects and inappropriate or ineffective medication use by re-evaluating the ongoing reasons for, and effectiveness of medication therapy.” Gnjidic et al. Clin Geriatr Med 2012;28:237–253 Overdiagnosis “...the related problems of over medicalisation and subsequent overtreatment, diagnosis creep, shifting thresholds, and disease mongering, all processes helping to reclassify healthy people with mild problems or at low risk as sick.” Moynihan et al. Preventing overdiagnosis: how to stop harming the healthy. BMJ 2012;344 November 2013 http://tinyurl.com/medsopt Stopp Start A Toolkit Gallagher et al. Int J Clin Pharmacol Ther. 2008 46(2):72-83. Gafinkel et al. Arch Intern Med. 2010;170(18):164 8–1654 Everybody’s business Structured approach integrated with clinical judgement is required. Acknowledge some meds may be restarted – it’s a trial Full engagement of patient, family, carers is imperative and honesty all round The MDT Share the workload with pharmacists/specialists Patients, relatives, carers, community pharmacists, OTs, nurses etc can monitor drug effects and feedback Focus on patients with the highest medication related risks and morbidities For individual patients, focus on the drugs with the highest risks or highest benefits …..less is more References [email protected] American Geriatric Society (2012). Updated Beers criteria for potentially inappropriate medication use in older adults. J Am Geriatr Soc Barber ND, Alldred DP, Raynor DK et al 2009.The Care Homes’ Use of Medicines Study. Quality and Safety in Health Care 18, pp.341-6. Cochrane Collaboration 2012 Interventions to improve the appropriate use of polypharmacy for older people. Gallagher P et al. Screening tool of older people’s potentially inappropriate prescriptions. In J Clin Pharmacol Ther 2008;46:72-83 (STOPP) Gallagher P et al. Screening tool to alert doctors to right treatment. In J Clin Pharmacol Ther 2008;46:72-83 Garfinkel D, Mangin D. Feasibility study of a systematic approach for discontinuation of multiple medications in older adults: addressing polypharmacy. Arch. Intern Med 2012;170:1648-54. Hanlon J et al. Medication Appropriateness Index- MAI. J Clin Epidemiol 1992;45:1045-51 NHS Highland. Polypharmacy: Guidance for prescribing in frail elderly 2013 O’Mahony, O’Connor. Pharmacotherapy at the end-of-life. Age and ageing 2011;40;419-22 Steinman M, Hanlon J. Managing medications in complex elders: There’s got to be a happy medium. JAMA 2010;304(14):1592-1601 http://www.prescqipp.info/projects/polypharmacy-and-deprescribing Thanks also to Lelly Oboh, Consultant pharmacist, Care of older people Guys & St Thomas NHS Community Health services, East & South East England NHS Specialist Pharmacy Services