* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Runge - Auditory Neuropathy Spectrum Disorder
Survey
Document related concepts
Specific language impairment wikipedia , lookup
Telecommunications relay service wikipedia , lookup
Sound localization wikipedia , lookup
Speech perception wikipedia , lookup
McGurk effect wikipedia , lookup
Hearing loss wikipedia , lookup
Olivocochlear system wikipedia , lookup
Noise-induced hearing loss wikipedia , lookup
Sensorineural hearing loss wikipedia , lookup
Auditory processing disorder wikipedia , lookup
Audiology and hearing health professionals in developed and developing countries wikipedia , lookup
Transcript
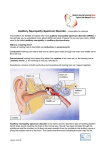
Auditory Neuropathy Spectrum Disorder Christina L. Runge PhD, CCC-A Chief, Division of Communication Sciences Director, Koss Cochlear Implant Program Department of Otolaryngology and Communication Sciences Medical College of Wisconsin, Milwaukee, WI Acknowledgements NIH/NIDCD K23DC008837 Genotype-Phenotype Relationships in Auditory Neuropathy Koss Cochlear Implant Program Department of Otolaryngology and Communication Sciences Medical College of Wisconsin Milwaukee, WI Masters Family Speech and Hearing Center Children’s Hospital of Wisconsin Milwaukee, WI Learning Objectives • Define the clinical audiologic findings necessary to diagnose ANSD • Be familiar with medical conditions requiring further evaluation due to a strong association with ANSD • Understand assessment and intervention option for children with ANSD 1 Multi-Disciplinary Program ANSD Background Nomenclature • Auditory neuropathy (AN) • Auditory dys-synchrony (AD) • Auditory neuropathy/dys-synchrony (AN/AD) • Auditory neuropathy spectrum disorder (ANSD) 2 Clinical Definition • Present outer hair cell function – Otoacoustic emissions (OAEs) – Cochlear microphonic (CM) • Dys-synchronous neural activity – Absent or abnormal ABR – Absent or elevated middle ear reflexes Clinical Definition • Various audiometric configurations • Unusually poor speech perception – Particularly in noise • Temporal processing disorder Speech Perception with ANSD • Temporal information is important for encoding speech – Low to mid frequencies • Temporal impairment and/or degraded signal (i.e., in noise) significantly impacts speech perception 3 Model of ANSD Zeng et al., J. Neurophysiol 2005 Sensorineural Hearing Loss X X Unaided X X X X Aided Adapted from: http://www.ucihs.uci.edu/hesp/Simulations/simulationsmain.htm Auditory Neuropathy - Mild X X Unaided X X X X Aided Adapted from: http://www.ucihs.uci.edu/hesp/Simulations/simulationsmain.htm 4 Auditory Neuropathy - Severe X X Unaided X X X X Aided Adapted from: http://www.ucihs.uci.edu/hesp/Simulations/simulationsmain.htm Diagnosis of ANSD Newborn Hearing Screening • Newborn Hearing Screening – OAE screen will miss ANSD – ABR screening needed for babies in the NICU or with risk factors • Neonatal risk factors – Family history of ANSD – Anoxia – Hyperbilirubinemia – Premature birth – Exchange transfusion 5 Evoked Potentials • OAEs and/or CM – Outer hair cell function • ABR – Auditory nerve and brainstem function • Middle ear reflexes – Auditory reflex pathway function Otoacoustic Emissions • Transient-Evoked (TEOAEs) or Distortion Product (DPOAEs) • General criteria for present OAEs – Must be 4-6 dB above the noise floor – Must be reproducible – Must be present across multiple frequencies/octave bands • Present in approximately 75% with ANSD Transient-evoked OAEs 6 Auditory Brainstem Response • Use ANSD protocol when ABR absent at high stimulus levels (80-90 dB HL) • Test parameters: – Insert earphones – Click stimuli at 80-90 dB HL – Record ABR to both condensation (+) and rarefaction (-) stimuli – Record ABR to alternating polarity (+,-) stimuli – Record with insert earphone tube pinched Auditory Brainstem Response Amplitude (0.1 mV / div) Present cochlear microphonic Condensation and rarefaction recordings Absent neural response 0 2 4 6 Alternating polarity recording 8 10 Time (ms) *Do a condensation or rarefaction recording with pinched tube ABR Interpretation • Cochlear microphonic – Initial peak latency ~0.4 ms – Persists for several milliseconds – 180° phase shift follows reversal in stimulus polarity • ABR – Observed when CM is cancelled out – Absent or abnormal morphology – Pinched tube recording should show no response 7 Middle Ear Muscle Reflexes • Absent if no reflex ≥ 110 dB HL • Elevated if reflex > 95 dB HL • Caution with interpretation in young infants – High frequency probe tones for MEMRs are not established in this population • MEMRs should be confirmed with ABR using the ANSD protocol Imaging Considerations for ANSD MRI Evaluation • Abnormalities found in 64% with ANSD – 18% have absent/deficient auditory nerve • • • • Assess status of brain Assess the status of the auditory nerve Para-sagittal oblique reconstructions CN VIII > CN VII (about twice as thick) – at level of brainstem 8 Nerves of the IAC Facial nerve Cochlear nerve Superior vestibular nerve Inferior vestibular nerve Normal MRI Abnormal MRI 9 PHACE Syndrome •Infantile hemangiomas •Posterior fossa malformations •Aorta and cardiac defects •Eye abnormalities Genetic Testing for ANSD Candidate Genes • Associated with ANSD: – OTOF, PJVK, SLC19A2 • Associated with SNHL and peripheral neuropathy: – PMP22, MPZ, FXN • Screen for common GJB2 and GJB6 10 Mutations associated with ANSD • Otoferlin (OTOF) – OTOF is expressed in the inner hair cells – Affects calcium binding and vesicle docking Pujol, 2007 Encyclopedia Britannica, 2004 Otoferlin Mutations • DFNB 9 Phenotype – Profound bilateral hearing loss • Fluctuating Hearing Phenotype – Temperature-sensitive – May be heterozygous for mutation Temperature-Sensitive ANSD • 14 year-old boy • Hx of hearing fluctuation – Illness/fever – Physical exercise/exertion – Exposure to warm temperatures • Otoferlin mutation – Allele 1: 2389 T>C – Allele 2: Wildtype 11 Temperature-Sensitive ANSD Baseline (-6 mo) Fever w/ strep (0) After Illness (+16 d) Charcot-Marie Tooth • Peripheral neuropathy • Later manifestations: – Foot deformity (very high arch to feet) – Foot drop (inability to hold foot horizontal) – Loss of lower leg muscle, which leads to skinny calves – Numbness in the foot or leg – "Slapping" gait (feet hit the floor hard when walking) – Weakness of the hips, legs, or feet • No cure Freidereich’s Ataxia • Most common ataxia • Nervous system degeneration • Manifestations between 5-15 years old: – – – – – – Difficulty walking Muscle weakness Speech problems Involuntary eye movements Scoliosis Heart palpitations 12 Candidate Mutation Summary Pheno Gene/Locus Mutation AN/AD OTOF 2p23 1469 C>A DFNB9 1544T>C 1651 delG 1886_1887 insA 2122 C>T 2348 delG 2381 G>A 2485C>T 3032 T>C 4275G>A 4491 T>A 5473 C>G 5860_5862delATC 6014 G>A 6158 C>G 709C>T IVS 18+1 G>T IVS 24+1 G>A IVS 28-2 A>C IVS 36+2T>G IVS39+1G>C IVS 8-2 A>G Updated 765G>C OTOF muts 1180dupG R-B 2008 1236delC Codon P490Q I515T K629fs R708X G783fs R794H Q829X L1011P W1425X Y1497X P1825A I1954de R1939Q P1987R R237X Ex/Intr Ex15 Ex15 Ex16 Ex17 Ex19 Ex21 Ex21 Ex22 Ex26 Ex36 Ex37 Ex44 Ex48 Ex48 Ex48 Ex8 In18 In24 In28 In36 In39 In8 Ex9 Ex13 Ex14 Pheno Gene/Locus AN/AD OTOF 2p23 updated cont'd AN/AD PJVK 2q31.1-3 DFNB59 Mutation Codon 1601delC 2239G>T 2649C>A 2684.2685delGG 2732.2735dupAGCT 2891C>A 2905.2923delinsCTCC… 3400C>T 3413T>C 4227+1G>T 4351G>T 4483C>T 5011dupT 5384T>G 5800dupC Ex/Intr Ex16 Ex20 Ex23 Ex24 Ex24 Ex25 Ex25 Ex28 Ex29 Int35 Ex36 Ex37 Ex41 Ex44 Ex46 547C-T 161C-T R183W T541I Ex4 Ex2 G172D del242fs/X259 W250X R162X G172R Ex2 Ex2 Ex2 Ex2 Ex2 AN/AD animal SLC19A2 1q23.3 515G>A 724delC 750G>A 484C>T 515G>C animal Pheno Gene/Locus Mutation AN/AD MPZ 1q21.3-q23 434A>C 371C>T 308G>A 293G>C 293G>A 292C>T 290A>T 242A>G Codon Y145S T124M G74E R98P R98H R98C E97V H81R SNHL PMP22 17p11.2 1.5 Mb dup/del 248G>C A67P G94(insG) SNHL FXN 9q Ex/Intr Ex3 Ex3 Ex3 Ex3 Ex3 Ex3 Ex3 Ex3 Ex3 GAA rep Int1 HyperbilUGT1A1 2q37 A(TA)7TAA -3263T>G 211G>A G71R Promoter Promoter Ex1 Screen GJB2 35delG M34T 167delT IVS+1G-A 235delC GJB6-D13S1830 GJB6 Intervention with ANSD: Hearing Aids and Cochlear Implantation ANSD Audiometric Profile 3% 30% Normal Aidable 67% Profound N=258 ears Berlin et al., IntJAud 2010;49;30-43. 13 Hearing Aids • Fit as early as possible • Fit gain to the hearing loss – Ensure audibility – Do not try to ‘protect’ OAEs with mild-gain HAs • Should improve sound detection • Assess auditory skill progress • Assess speech and language development Auditory Skill Assessment • Assessment intervals – Before HA fitting (baseline) – Every 3 months after HA fitting – At end of HA trial (if not on a 3-month interval) • LittlEARS: milestone assessment – Receptive auditory behavior (sound detection) – Semantic auditory behavior (comprehension) – Expressive-vocal behavior LittlEARS • First 24 months of intervention • Standardized on normal hearing children • Track development trajectory – Identify plateaus – Intervention, therapy 14 Speech/Language Assessment • Assessment intervals – At 6 mo of age, or upon identification if older – Every 6 months after – Therapy sessions to become familiar with child • Follow longitudinally – Determine progress – Quantify delay (if present) Cochlear Implant Candidacy • Is a child with ANSD a CI candidate? – Profound hearing loss (30%) Yes (if all CI criteria are met) – Normal to severe loss (70%) Acoustic benefit? • Acoustic benefit – Progress in auditory and speech-language skills – Currently no strict criteria for determining implantation in ANSD Cochlear Implantation • Restore neural synchrony – EABR, ECAP present • Outcomes often positive – 85% successful (Berlin et al., 2010) • Potential contraindications to CI Runge-Samuelson et al., 2007 – Severe or central neuropathy (kernicterus, Freidereich’s Ataxia) – Absent auditory nerve 15 ANSD – Profound HL and CI • • • • • • • • • 250 500 1K 2K 8K 4K 7 year-old girl -10 0 Cystic fibrosis 10 20 Failed NB screen (ABR) 30 40 50 Diagnostic +OAEs, -ABR 60 70 Minimal progress with HAs 80 90 XX Otoferlin homozygous (Runge et al., 2013) 100 O X O O O O 110 120 Cochlear Implant at 1.5 years 56% PBK words 90%(Q), 90% (N) HINT-C Sentences ANSD – Moderate HL and CI • • • • 10 year-old boy Hyperbilirubinemia, preemie 2 mos: +OAEs, -ABR Hearing aids at 1 year – Improved detection only 250 500 1K 2K 4K 8K 8K 8K -10 0 10 20 30 40 50 60 70 80 90 100 110 120 O X X O X O • Cochlear implant at 3 years • 68% PBK words • 94%(Q), 91% (N) HINT-C Sentences ANSD – Moderate HL and HAs 250 500 • • • • • 8 year-old boy Twin-to-twin transfusion 9 months +CM, -ABR Mild-moderate hearing loss Normal speech and language development • 76% PBK words in quiet • Difficulty in noise 1K 2K 4K 8K 8K -10 0 10 20 30 40 50 60 70 80 90 100 110 120 X O X O X O O X Age 2 years 16 Can AN ‘reverse’? • Very rare • High-risk infants: premature, low birth weight, hyperbilirubinemia • Improvement emerging or complete by 712 months of age • Repeat ABR testing to ensure stability – Always before a cochlear implant Summary • ANSD is a unique hearing disorder – Temporal impairment – Distinct from SNHL • Requires special tests and close follow up – Evidence-based protocol • Multi-disciplinary clinical care – Communication among professionals and parents • Research 17