* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Implantation
Survey
Document related concepts
Transcript
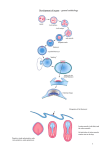
CRANIOFACIAL DEVELOPMENT PRENATAL dr.Indriati Dwi R, M.Kes Dep. Anatomi-Histologi FKUB We cannot teach people anything; we can only help them discover it within themselves. Galileo Galilei Why? • Pregnancy dentocraniofacial development • Early diagnosis clinical decision making, avoid harmful treatment • Future : – fetus in utero + potential patient – Biomedik : stem cell engineering Contoh (populer) cranio/orofacial malformation: • Cleft lip/palate Birth defects Birth defects can be classified based on : • severity, medical or social consequences, • pathogenetic mechanism • their clinical presentation Classification based on severity • Major anomalies: these are birth defects that have medical or social consequences for the affected child. Ex : cleft lip and palate, atrial septal defect, & radial aplasia • Minor anomalies: birth defects that have no significant health or social implications for the affected child. Ex : partial syndactyly of the second and third toes. Multiple minor anomalies can provide clues to the diagnosis of multiple congenital anomaly syndromes and they may also be a marker for a chromosomal aberration • Common variants : end of the spectrum of normal development rather than birth defects. Ex : fetal finger pads, sacral dimple Classification based on pathogenesis • Deformation : aberrant mechanical force distorting normally developing structures • Disruption : destructive processes that alter a structure after it has formed normally • Malformation : failure or inadequate completion of normal developmental processes. • Dysplasia : abnormal cellular organisation or function within a specific tissue type throughout the body Ruang lingkup – Production of egg and sperm gametogenesis 1st week – Transport gametes and fertilization development – Cleavage and Embryo transport – implantation – Formation of germ layers Embryonic – Establishment of the Basic Embryonic stage (2 to 2) Body Plan – Production of egg and sperm gametogenesis –Transport gametes & fertilization – Cleavage and Embryo transport – implantation – Formation of germ layers – Establishment of the Basic Embryonic Body Plan Transport of Gametes and Fertilization • Ovulation : – Mid point of menstrual cycle – Under the influence LH and FSH floats out of the ovary • Oocyte transport Before ovulation, fimbriae of the oviduct sweep over the ovary, and tube contract rhytmically. Oocyte is carried into the tube by motion of cilia on the epithelial lining. Transport of Gametes and Fertilization (Contd..) Sperm transport • Seminiferous tubules epididymis, biochem (environment condusive to independent motion) • reflex ejaculation of semen (emission & ejaculation) • Capasitation : A period conditioning in the female reprod tract. Transport of Gametes and Fertilization Contd.. Fertilization : • the process by which male and female gametes fuse • Occurs in the ampullary region of the oviduct VIABILITY OF GAMETES • the oocyte cannot be fertilized after 24 hours and that it degenerates shortly thereafter . • Most human sperms probably do not survive for more than 48 hours in the female genital tract Fertilization sperma vs ovum The phase : (1) Sperm penetration of corona radiata (2) Sperm binding and penetration of the zona pellucida (3) one sperm enters the egg Fuse zygote Acrosome reaction : • Occurs after binding zona pellucida(zp) • Release of enzymes (acrosin & trypsin like substance ) needed to penetrate zp. zygote embryoblast Approximately 6 days after fertilization, the cell mass is termed a blastocyst. Human chorionic gonadotropin now is produced in amounts that may be detected by commercial laboratories. – Production of egg and sperm gametogenesis – Transport gametes & fertilization –Cleavage and Embryo transport – implantation – Formation of germ layers – Establishment of the Basic Embryonic Body Plan Inner cell mass = embryo Outer cell mass = trophoblast Pre-embyonic developmental stages Cleavage === a series of mitotic division that result in increase in cells, blastomere, which become smaller with each division • Fertilization zygote 2 cell stage mitotic divisionnumber of cells Blastomeres Cleavage Blastocyst Formation : • At the time morula enter the uterine cavity, fluids penetrate through zona pellucida into intercellular spaces of inner cell mass(icm). Single cavity (blastocele) • Embryo =blastocyst • Inner cell mass = embryo • Outer cell mass = trophoblast Heading to Implantation • Zona pellucida is covering the embryo until its reach uterus preparation for implantation • Four to 5 days after fertilization, the zona pellucida is shed and the trophoblast adjacent to the embryoblast attaches to the endometrial epithelium. – Production of egg and sperm gametogenesis – Transport gametes & fertilization – Cleavage and Embryo transport –implantation – Formation of germ layers – Establishment of the Basic Embryonic Body Plan embryoblast Approximately 6 days after fertilization, the cell mass is termed a blastocyst. Human chorionic gonadotropin now is produced in amounts that may be detected by commercial laboratories. Implantation • = kontak fisik & fisiologis pertama; antara blastocyst vs mucosa uterus (6th 8th day), • 3 phase : – Preparation of the uterus for adhesion and implantation – Trophoblast-uterus adhesion – Blastocyst movement into the uterus (mid portion of the posterior/anterior) Implantation • Processes : zona pellucide disappear → polar trophoblast touch the endometrium→secrete proteolytase →dissolve the endometrium → embedded into endometrium→coagulation plug seal the space • Day 8 – The blastocyst embeded partially in endometrium – Trophoblast has differentiated into 2 layer : • Inner layer of mononucleated cellCytotrophoblast • Outer layer of multinucl Syncytiotrophoblast – Embryoblast also differentiated into 2 layer : • An upper layer of cuboidal cells epiblast • A lower layer of collumnar cells hypoblast • Day by day of the conceptus Week 2, days 8 – 14 Week 3 -8 [embryonic periode] Month 3 to birth [fetus] : • The Placenta and Fetal Membranes • Day by day of the conceptus Week 2, days 8 – 14 Week 3 -8 [embryonic periode] Month 3 to birth [fetus] • lacunar stage • Primary yolk sac • Blastocyst is completely embedded in the endometrial stroma • uteroplacental circulation. Day by day of the conceptus Week 2, days 8 – 14 Week 3 -8 [embryonic periode] Formation of Germ Layers and Early Tissue and Organ Differentiation: Third Week Organogenetic Period: Fourth to Eighth Weeks Month 3 to birth [fetus] – Production of egg and sperm gametogenesis – Transport gametes & fertilization – Cleavage and Embryo transport – implantation –Formation of germ layers – Establishment of the Basic Embryonic Body Plan Formation of Trilaminar Germ Disc Formation of mesoderm: early of 3 weeks Gastrulation : – primitive streak: cells of epiblast proliferate to form a longitudinal arranged cell cord – primitive groove – primitive node – primitive pit [ Third week of development] Formation of Trilaminar Germ Disc Trilaminar germ disc = endoderm + mesoderm + ectoderm determination of head and tail of germ disc • endoderm: hypoblast cells are replaced by epiblast cells • ectoderm: epiblast changed the name into ectoderm • mesoderm: intraembryonic mesoderm Formation of Trilaminar Germ Disc • Head process (The notochordal process gives an appearance of being a prolongation of the primitive streak in the direction of the future head region of the embryo) → notochordal tube → notochord : – buccopharyngeal membrane – cloacal membrane * : by mesodermal cells • The notochordal process immediately rostral to the primitive node and streak • Mesenchymal cells from the primitive streak and notochordal process migrate laterally and cranially , among other mesodermal cells, between the ectoderm and endoderm until they reach the margins of the embryonic disc. • blood islands of the umbilical vesicle (yolk sac), allantois, and chorion intraembryo 3rd to eight week Differentiation of trilaminar germ disc: 3th – 8th weeks • differentiation: same cells which are primordial and immature differentiate into different cells which have specific structure and function • induction: some tissues effect the differentiation, and determine the differentiating orientation of another tissue 4 to 8 week of development (organogenesis) • Differentiation of ectoderm: CNS • Differentiation of mesoderm: dermis, bone, cartilage, CT, muscles, pleura, peritoneum and pericardium, cardiovascular and lymph system • Differentiation of endoderm: digestive, respiratory and urinary system CRANIOFACIAL DEVELOPMENT inside organogenesis Differentiation of ectoderm: from 18th –19th days • neural plate: neuro-epithelium(neural ectoderm): pseudostratified columnar epithel. • neural fold • neural groove • neural tube: →CNS /anterior neuropore: closed by 25th days /posterior neuropore: closed by 27th days • neural crest(mesoectoderm): two lines of cell cords→ganglion embryonic organogenesis Differentiation of mesoderm: 17th days • paraxial mesoderm – somite: 20th days, 3 pairs/per day, 42-44 pairs by the end of 5th weeks – sclerotome: →bone, cartilage – myotome: →skeletal muscle – dermatome: dermis and hypodermis • Intermediate mesoderm:→kidney reproductive gland – nephrotome: segmentation – nephrogenic cord: and organogenesis • lateral mesoderm: – intraembryonic coelom: →body cavity – somatic or parietal mesoderm: →muscle, CT, parietal layer of pleura, peritoneum and pericardium – splanchnic or visceral mesoderm: →muscle, CT of digestive tract, visceral layer of pleura, peritoneum and pericardium – mesenchyme: →cardiovascular and lymph system organogenesis Differentiation of endoderm: • primitive gut: →digestive, respiratory and urinary system Recaps Recaps Fourth Week - Major changes in body form - Early brain development ( till closing neuropore) - limb buds - otic pits - lens placodes - fourth pair of pharyngeal arches fifth week - growth of the head - rapid development of the brain and facial prominences A teratogen is any infectious agent, drug, chemical, or irradiation that alters fetal morphology or fetal function if the fetus is exposed during a critical stage of development. 1. The resistant period (week 1 of development) the “all-ornone” phenomenon (i.e., the conceptus will either die as a result of the teratogen or survive unaffected). 2. The maximum susceptibility period (weeks 3–8; 18 to 60 days postconception = embryonic period). All organ morphogenesis occurs at this time. Teratogenic exposures may result in structural anomalies. 3. The lowered susceptibility period (weeks 9–38; fetal period) All organs systems have already formed; Teratogen exposure at this period generally results in a functional derangement of an organ system. may result in structural anomalies. • Day by day of the conceptus Week 2, days 8 – 14 Week 3 -8 [embryonic periode] Month 3 to birth [fetus] : • The Placenta and Fetal Membranes The Placenta components: • The fetal part : formed by the villous chorion. The chorionic villi that arise from it project into the intervillous space containing maternal blood. • The maternal part : formed by the decidua basalis By the end of the fourth month, the decidua basalis is almost entirely replaced by the fetal part of the placenta. The placenta and fetal membranes perform the following functions and activities: protection, nutrition, respiration, excretion, and hormone production head formation apparatus pharyngeal face palata Odontogenesis Other : tongue , salivary gland , sense organ Head formation • Occurs at the earliest stages • Orofacial from CNC (ectoderm origin) • Calvaria from mesoderm (paraxial) • Brain : ~ brain development Neural crest PHARYNGEAL APPARATUS • CNC : the major source of connective tissue components, including cartilage, bone, and ligaments in the facial and oral regions. • myoblasts, originating from paraxial and prechordal mesoderm, contribute to the craniofacial voluntary muscles. • The lower jaw and lower lip are the first parts of the face to form. They result from merging of the medial ends of the mandibular prominences in the median plane (will be discussed later……) face Neural crest Paraxial mesoderm Lateral plate mesoderm neurocranium (shaded area) and the viscerocranium ( black area). The bones of the neurocranium and viscerocranium are derived almost entirely from neural crest cells, except for the basilar part of the occipital bone (asterisk), which forms from mesoderm of the occipital sclerotomes, and the laryngeal cartilages (asterisk), which form from mesoderm within pharyngeal arches 4 and 6. OSSIFICATION of the SKULL Neurocranium (basis cranii) • Endochondral – os.occipital, os.sphenoid, os.ethmoid • Intramembranous – Calvaria Viscerocranium From neural crest • Endochondral – Maleus, incus, stapes, proc.styloid os temporal – Os hyoid • Intramembranous – Os temporal, os maxilla, os zygomaticum – Os mandibula At 12 weeks showing the cartilaginous base of the cranium or chondrocranium formed by the fusion of various cartilages. D, At 20 weeks indicating the derivation of the bones of the fetal cranium. head formation apparatus pharyngeal face palata odontogenesis Other : tongue , salivary gland , sense organ Pharyngeal apparatus • Very dominat, typical feature in head&neck dev; esp. lateral and ventral regions of the head and neck. • tdd : lateral plate mesoderm + ekstensi lateral dari pharyngeal endoderm + CNC migration + ectoderm • Inti : jar.mesenchymal, diselubungi ectoderm di permukaan, dan lap.dalam dilapisi epithelia derivat endoderm • @ : 4th week Tdd : • Pharyngeal arches : 5* • Pahryngeal pouches : 4* • Pharingeal grooves/cleft : 4 • [Pharyngeal membrane] : 4 Pharyngeal arches Pharyngeal pouches Pharingeal grooves/cleft [Pharyngeal membrane] End of part ONE Anatomi.lecture.ub.ac.id FB : Anatomi FKUB Twitter : Anatomi_FKUB