* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download TB disease - Croydon Health Services NHS Trust
Common cold wikipedia , lookup
Sociality and disease transmission wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Kawasaki disease wikipedia , lookup
Behçet's disease wikipedia , lookup
Transmission (medicine) wikipedia , lookup
Childhood immunizations in the United States wikipedia , lookup
Neuromyelitis optica wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Ankylosing spondylitis wikipedia , lookup
Schistosomiasis wikipedia , lookup
Germ theory of disease wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Multiple sclerosis research wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Infection control wikipedia , lookup
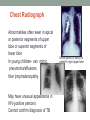
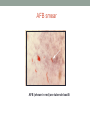
PAEDIATRIC TB Jenny Handforth June 2014 Overview •Why is Paediatric TB important •Epidemiology- know the patients •Adult v child with TB - differences? • Diagnostic challenges: Why do you need to know about Paediatric TB? • 1 million cases estimated globally each year (11%) • 25-40% of all cases are children in high burden countries • 4-7% in low burden countries • Higher risk of severe disease and death in young children • Indicator of effectiveness of TB control programmes Figure 1.1: Tuberculosis case reports and rates, UK, 2000-2012 10,000 15 14 9,000 13 8,000 12 Number of cases 10 6,000 9 8 5,000 7 4,000 6 5 3,000 Rate (per 100, 000) 11 7,000 4 2,000 3 2 1,000 1 0 0 2000 2001 2002 2003 2004 2005 2006 2007 2008 2009 2010 2011 2012 Year Number of cases Rate per 100,000 Source: Enhanced Tuberculosis Surveillance (ETS), Enhanced Surveillance of Mycobacterial Infections (ESMI), Office for National Statistics (ONS) Data as at July 2013 Prepared by: TB Section, Centre for Infectious Disease Surveillance and Control, Public Health England 4 Tuberculosis in the UK: 2013 report Figure 1.3. Three-year average tuberculosis case rates by local area*, UK, 2010-2012 *England – Local authorities, Wales and Scotland – Health Boards, NI – data not available London © Crown copyright and database rights 2013 Ordnance Survey 100016969 Source: Enhanced Tuberculosis Surveillance (ETS), Enhanced Surveillance of Mycobacterial Infections (ESMI), Office for National Statistics (ONS) Data as at July 2013 Prepared by: TB Section, Centre for Infectious Disease Surveillance and Control, Public Health England 5 Tuberculosis in the UK: 2013 report Figure 1.4: Tuberculosis case reports and rates by region*, England, 2012 4,000 3,500 50 41.9 Number of cases 45 Rate (per100,000) and 95% CI 40 3,000 Number of cases 2,500 30 2,000 25 19.4 20 1,500 1,000 11.3 11.5 9.3 15 10.8 7.8 5.8 500 0 Region * HPA region CI – 95% confidence intervals Source: Enhanced Tuberculosis Surveillance (ETS), Office for National Statistics (ONS) Data as at July 2013 Prepared by: TB Section, Centre for Infectious Disease Surveillance and Control, Public Health England Tuberculosis in the UK: 2013 report 10 5 0 6 6.4 Rate (per 100, 000) 35 Figure 1.6: Tuberculosis case reports by place of birth and country, UK, 2012 Non UK-born UK-born 100% 90% 2,020 Percentage of cases 80% 39 142 56 48 185 73 70% 60% 50% 40% 5,819 30% 20% 10% 0% Country (% where place of birth known) Source: Enhanced Tuberculosis Surveillance (ETS), Enhanced Surveillance of Mycobacterial Infections (ESMI) Data as at July 2013 Prepared by: TB Section, Centre for Infectious Disease Surveillance and Control, Public Health England 7 Tuberculosis in the UK: 2013 report Figure 1.8: Non UK-born tuberculosis case reports by time since entry to the UK to tuberculosis diagnosis, UK, 2012 600 Number of cases 500 400 300 200 100 0 0 5 10 15 20 25 30 35 Years since entry to diagnosis Source: Enhanced Tuberculosis Surveillance (ETS), Enhanced Surveillance of Mycobacterial Infections (ESMI) Data as at July 2013 Prepared by: TB Section, Centre for Infectious Disease Surveillance and Control, Public Health England 8 Tuberculosis in the UK: 2013 report 40 45 50+ Figure 1.10: Tuberculosis case reports and rates by age group and place of birth, UK, 2012 1,200 140 1,100 Number of cases 900 100 800 700 80 600 60 500 Rate (per 100,000) 120 1,000 400 40 300 200 20 100 0 0 Age group (years) UK-born Non UK-born Rate in UK-born Rate in non UK-born Source: Enhanced Tuberculosis Surveillance (ETS), Enhanced Surveillance of Mycobacterial Infections (ESMI), Office for National Statistics (ONS) Data as at July 2013 Prepared by: TB Section, Centre for Infectious Disease Surveillance and Control, Public Health England 9 Tuberculosis in the UK: 2013 report 800 40 700 35 600 30 500 25 400 20 300 15 200 10 100 5 0 0 Rate (per 100,000) Number of cases Figure 1.11: Tuberculosis case reports and rates by age group and sex, UK, 2012 Age group (years) Male cases Female cases Rate in males Rate in females Source: Enhanced Tuberculosis Surveillance (ETS), Enhanced Surveillance of Mycobacterial Infections (ESMI), Office for National Statistics (ONS) Data as at July 2013 Prepared by: TB Section, Centre for Infectious Disease Surveillance and Control, Public Health England 10 Tuberculosis in the UK: 2013 report Figure 1.14: Child to adult ratio in notifications rate, UK, 2000-2012 Ratio: case notification rate children/adults 0.40 0.30 0.20 0.10 0.00 2000 2001 2002 2003 2004 2005 2006 2007 2008 2009 2010 2011 2012 The child-to-adult ratio is the ratio of the case notification rate in children under 15 years of age, to that in adults. A declining trend in the ratio suggests a decrease in ongoing transmission (European Centre for Disease Prevention and Control). Source: Enhanced Tuberculosis Surveillance (ETS), Enhanced Surveillance of Mycobacterial Infections (ESMI) Data as at July 2013 Prepared by: TB Section, Centre for Infectious Disease Surveillance and Control, Public Health England 11 Tuberculosis in the UK: 2013 report Questions that must be asked... • Has this child been exposed to TB? • Has the child been infected with TB? • If yes does this child have Tb disease? • Who has infected this child? • …and answered! 3 scenarios for investigating TB in children 1. 2. 3. Screening healthy children - screen for TB risk factors Known contact with infectious case - usually adult Child with symptoms and/or signs of TB or abnormal CXR - high index of suspicion required Pathogenesis of TB in childhood • • • No infection • heals Exposure to bacilli from adult Dissemination to lung apices, meninges,bone spine,nodes Primary complex • progresses • Active disease • Dormant TB disease (TB) or Latent TB (LTB) • TB: active M. tuberculosis in some part of child’s body • May be asymptomatic • Abnormal CXR and/or abnormal clinical exam • LTB: dormant M. tuberculosis • Clinical exam normal • X rays normal • Diagnosis is made by • History • Clinical examination • CXR/imaging/microbiology Risk of Disease following primary infection Marais BJ et al. Int J Tuberc Lung Dis 2004;8:392-402 Disseminated TB Pulmonary No disease comments TB <1 years 10-20% 30-40% 50% High rates of morbidity & mortality 1-2 years 2-5% 10-20% 75-80% High rates of morbidity & mortality 2-5 years 0.5% 5% 95% 5-10 years <0.5% 2% 98% >10 years <0.5% 10-20% 80-90% Safe school years Adult disease Table 1.2: Tuberculosis case reports by site of disease, UK, 2012 Site of disease* Number of cases 4,563 Percentage** 52.1 Extra-thoracic lymph nodes 1,872 21.4 Intra-thoracic lymph nodes 946 10.8 Other extra-pulmonary 619 7.1 Pleural 651 7.4 Gastrointestinal 471 5.4 Bone – spine Cryptic ± 394 4.5 46 0.5 ± 197 2.3 Bone – other 218 2.5 CNS – meningitis 187 2.1 Genitourinary 137 1.6 CNS – other 80 0.9 Laryngeal 16 0.2 Unknown extra-pulmonary 15 0.2 Pulmonary Miliary *With or without disease at another site ±For **Percentage of cases with known sites of disease (8751) Scotland cases, this includes both cryptic and miliary site CNS - Central Nervous System Total percentage exceeds 100% due to infections at more than one site Source: Enhanced Tuberculosis Surveillance (ETS), Enhanced Surveillance of Mycobacterial Infections (ESMI) Data as at July 2013 Prepared by: TB Section, Centre for Infectious Disease Surveillance and Control, Public Health England 17 Tuberculosis in the UK: 2013 report Evaluation for TB Medical history Physical examination Mantoux tuberculin skin test IGRAs Chest radiograph Bacteriologic or histologic exam Medical History Symptoms of disease History of TB exposure, infection, or disease Past TB treatment Demographic risk factors for TB Medical conditions that increase risk for TB disease Systemic Symptoms of TB Fever Cough Chills Night sweats Appetite loss Weight loss Tiredness Testing for TB Disease and Infection Factors that May Affect the Skin Test Reaction Type of Reaction False-positive False-negative Possible Cause Nontuberculous mycobacteria BCG vaccination Anergy Recent TB infection Very young age (< 6 months old) Live-virus vaccination Overwhelming TB disease Anergy • Do not rule out diagnosis based on negative skin test result • Consider anergy in persons with no reaction if - HIV infected - Overwhelming TB disease - Severe or febrile illness - Viral infections - Live-virus vaccinations - Immunosuppressive therapy. • Anergy skin testing no longer routinely recommended Interferon Gamma Release Assays (IGRAs) • Recommended in NICE guidelines • Quantiferon-TB gold and T-spot.TB • Incubate patients blood with M. tuberculosis specific antigens (ESAT 6 & CFP-10) • Measure production of gamma interferon • More specific than TST • Cannot distinguish between active and latent TB • Expensive • Technically difficulties with sampling • Lack of data for children Chest Radiograph Abnormalities often seen in apical or posterior segments of upper lobe or superior segments of lower lobe In young children- can mimic pneumonia/effusions hilar lymphadenopathy Arrow points to cavity in patient's right upper lobe . May have unusual appearance in HIV-positive persons Cannot confirm diagnosis of TB Specimen Collection Obtain 3 sputum specimens for smear examination and culture Persons unable to cough up sputum, induce sputum, bronchoscopy or gastric aspiration Consider lymph node biopsy Notoriously difficult to achieve in children AFB smear AFB (shown in red) are tubercle bacilli Cultures • Use to confirm diagnosis of TB • Culture all specimens, even if smear negative • Results in 4 to 14 days when liquid medium systems used Colonies of M. tuberculosis growing on media Treatment • Doses weight adjusted • TB disease • Latent TB • 6 months of isoniazid • 3 months of isoniazid & rifampicin • Pyrazinamide and ethambutol for first 2 months • CNS- total 12 months plus dexamethasone at start and rifampicin • Or • 6 months isoniazid Things to consider • Baseline LFTS • Eye check up • HIV testing Young Children with TB • Differ from Adults with TB: • Signs/symptoms • Generally not infectious • Pattern of progression to disease • Response to treatment • Side effects • Don’t forget parent! Adolescents with TB • Differ from young children: • Signs/symptoms • Delay in diagnosis • Adherence issues • Side effect profile • May be infectious! Monitoring Patients Establish rapport with patient and emphasize Benefits of treatment Importance of adherence to treatment regimen Possible adverse side effects of regimen Establishment of optimal follow-up plan Monitoring Patients (cont.) At least monthly, evaluate for Adherence to prescribed regimen Signs and symptoms of active TB disease Signs and symptoms of hepatitis Preventing and Controlling TB Three priority strategies: Identify and treat all persons with TB disease Identify contacts to persons with infectious TB; evaluate and offer therapy Test high-risk groups for LTBI; offer therapy as appropriate 36 Tuberculosis in the UK: 2013 report Table 2.1: Number and proportion of tuberculosis cases with drug resistance by age group, UK, 2012 Isoniazid Resistant to any Multi-drug resistant first line drug* resistant Age Group Total** n % n % n % 0-14 10 9.7 10 9.7 7 6.8 103 15-44 240 7.2 264 7.9 65 2.0 3,333 45-65 77 7.6 78 7.7 8 0.8 1012 65+ 24 3.4 27 3.8 1 0.1 703 *First line drugs - isoniazid, rifampicin, ethambutol and pyrazinamide**First line drugs – isoniazid, rifampicin, ethambutol and pyrazinamide **Culture confirmed cases with drug susceptibility results for at least isoniazid and rifampicin Source: Enhanced Tuberculosis Surveillance (ETS), Enhanced Surveillance of Mycobacterial Infections (ESMI) Data as at July 2013 Prepared by: TB Section, Centre for Infectious Disease Surveillance and Control, Public Health England Tuberculosis in the UK: 2013 report Table 4.1: Treatment outcome at 12 months for tuberculosis cases, UK, 2011* Treatment outcome n % 7,302 82.9 Died 434 4.9 Lost to follow-up 435 4.9 Still on treatment 289 3.3 88 1.0 257 2.9 100 Completed Stopped Not evaluated Total 8,805 * Excludes MDR-TB and RMP-resistant TB cases. Not evaluated includes missing, unknown and transferred out Source: Enhanced Tuberculosis Surveillance (ETS), Enhanced Surveillance of Mycobacterial Infections (ESMI) Data as at July 2013 Prepared by: TB Section, Centre for Infectious Disease Surveillance and Control, Public Health England 37 NHS Evidence Visit NHS Evidence for the best available evidence on tuberculosis diagnosis, treatment and management NHS Evidence Tuberculosis topic page Find out more • www.nice.org.uk/guidance/CG117 Take home messages • • • • • • • Think about TB TB is a family disease Ask about risk factors TB contacts BCG Hx Travel history IGRA can be useful, but a negative IGRA does not exclude TB • Liaise with TB nurses/doctors • TB therapy requires a lot of support • TB should be managed by specialists-discuss/refer early Questions?