* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Classification
Chagas disease wikipedia , lookup
Marburg virus disease wikipedia , lookup
Hepatitis C wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Anaerobic infection wikipedia , lookup
Gastroenteritis wikipedia , lookup
Hepatitis B wikipedia , lookup
Sexually transmitted infection wikipedia , lookup
Hookworm infection wikipedia , lookup
Visceral leishmaniasis wikipedia , lookup
Leptospirosis wikipedia , lookup
Sarcocystis wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Neonatal infection wikipedia , lookup
Toxocariasis wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Schistosoma mansoni wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Trichinosis wikipedia , lookup
Fasciolosis wikipedia , lookup
Schistosomiasis wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Loa loa filariasis wikipedia , lookup
Oesophagostomum wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
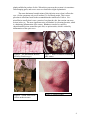
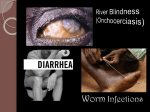
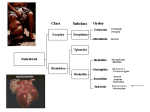
Onchocerca volvulus A. Classification Phylum: Nematoda Superfamily: Filarioidea (filarial worms) Genus/Species: Onchocerca volvulus B. Morphology Adult females are up to 50 cm in length and about 0.5 mm in diameter, whereas males are only 6 cm long. They have a tapered tail that often angles into a hook-like shape. Females are often full of developing microfilariae, which are advanced embryos. The female produces microfilariae rather then eggs, so there is no egg morphology to identify. Many nematodes have a sheath, which is a protective cuticular layer. O. volvulus microfilariae are unusual in that they are unsheathed. Microfilariae are approximately 150 to 350 mm in length and 0.8 mm in diameter. They have sharply pointed curved tails. Figure 2: O. volvulus developing embryo. Figure 1: Adult O. volvulus female. Figure 3: Cross section of a skin nodule containing O. volvulus adults. Note the thick connective tissue surrounding the worms. 1 C. Lifecycle The infection begins when an infected blackfly, which is the intermediate host, bites a human and feeds on the blood. As it bites the human, it transfers the infective J3 larvae from the proboscis of the fly into the bite opening. In the subcutaneous tissues the larvae then develop into the adults, which are usually found in nodules that form around them from reactions by the host. These capsules are about 3cm in diameter and usually contain 2-3 females and 1-2 males. The worms can survive in these capsules for about 15 years and the females can produce microfilaria for about 9 years. Females begin to produce microfilariae about 10-12 months after infection. The unsheathed microfilariae can live for about 2 years in the skin. They are usually found in the skin and lymphatics of connective tissue, but also have been found in the peripheral blood, the urine, and sputum. The blackfly picks up and ingests the microfilariae from an infected human while feeding on blood. After ingestion, the microfilariae migrate to the thoracic muscles of the fly. In these muscles they mature from J1 stage larvae into the infective J3 larvae. The J3 larvae then migrate to the blackfly's proboscis where they are ready to infect another human that the blackfly feeds on. Humans appear to be the only natural definitive host. The normal intermediate hosts are the fly Simulium spp., which have larval stages in streams, and adult flies can only survive where there is high humidity and waterside vegetation. Figure 4. Lifecycle of Onchocerca volvulus 2 Geographic Distribution O. volvulus is found in Africa, Central America, and South America. We have read that 96% of all cases occur in Africa. However, Mexico, Guatemala, Venezuela and Ecuador are also key areas. O. volvulus is found primarily in places near rivers because the vector blackfly requires rivers for breeding. Figure 5. Map of the geographic distribution of O. volvulus. Pathology and Symptoms Onchocerciasis, also known as River Blindness, is a disease caused by the infection of Onchocerca volvulus. Approximately 17-18 million people are estimated to be infected. This disease usually causes blindness and disfigurement. Both the adult worms and the microfilariae can cause the disease. The adults generally cause no symptoms, except the growth of subcutaneous nodules called onchocercomas. Onchocercomas are formed from collagen fibers encompassing a number of adult worms. In the African and Venezuelan strains these nodules usually form near the pelvic area, with some occurring at the spine, the neck and the knees. In infections found in Central America these nodules primarily form above the waist, mostly on the neck and head. The number of nodules formed varies from 1 to 100, and, although they are disfiguring, they are not painful. Elephantiasis can also occur with this infection as well as hernias, specifically femoral hernias in Africa. The microfilariae cause skin inflammation, or dermatitis, when the juveniles are degenerating in the skin. It begins with severe itching, which can be followed by a bacterial infection. If there is a bacterial infection there is usually also irregular pigmentation in that area. Then lichenification occurs and the skin starts to thicken, become discolored and crack. In the final stages it also loses its elasticity. Inflammation along with the loss of elasticity can lead to protruding lymph 3 glands enfolded in pockets of skin. When this occurs near the scrotum it is sometimes called hanging groin, and severe cases are classified as slight elephantiasis. The most detrimental complications of this infection occur when it affects the eyes. Ocular symptoms only occur in about 5% of affected people. This is more prevalent in infections found in the savannah than the rainforests of Africa. Live microfilariae usually don’t cause a reaction, but when they die, the reaction can cause lesions in the eye. The most significant cause of blindness is sclerosing keratitis, which is a hardening inflammation of the cornea. Blindness can also be caused by choroidoretinal lesions around the optic disk, or optic neuritis, which is caused by inflammation of the optic nerve. Figure 6. The intermediate host the blackfly (Simulium spp.) Figure 7. Removed nodules containing adult worms Figure 9. Onchocercoma Figure 8. A man with several visible onchocercomas 4 Figure 10. Hanging groin Figure11. Onchocerciasis-associated blindness F. Diagnosis A skin snip is taken from the area and examined for microfilariae. The skin is raised by a needle and sliced off. Then it is put in saline and put on a slide for observation of 304 to 315 long µm by 5-9 µm wide microfilariae that have a sharply flexed pointed end with no nuclei. There are no sheaths on the microfilariae. Mansonella streptocerca coexists with O.volvulus but its nuclear columns and tail of the microfilariae differ. Microfilariae might also appear in the urine or blood in heavy infections. G. Treatment A dosage of 150 µg/kg body weight of ivermectin (Mectizan®) is used to slowly eliminate skin microfilariae and also suppress release of microfilariae from the female worm for 1-2 years. Repeated dosages slowly kill the worms. Other drugs that are used but have sever side effects include Di-ethylcarbamazine-citrate (DEC) and suramine, which is toxic. Excision of nodules around the head may effectively lower rate of eye damage and also reduce new infections in the population. H. Public Health and Eradication. Treatment of individuals seems to be the most effective way of preventing new infections. It was predicted that the disease would not be a public health problem by 2002 in OCP (Onchocerciasis Control Programme) countries because of treatments provided for individuals. OCP is aiming for virtually eliminated from the western hemisphere by 2007. Killing of the black fly larva in streams by DDT is also a mean of eradication but has environmental consequences. It is advised to use screens to prevent fly bites. 5 References Carlo Denegri Foundation. “Skin and Eye Parasites.” <http://www.cdfound.to.it/HTML/onc1.htm.> Accessed February 27, 2005. Center for Disease Control and Prevention, National Center for Infectious Diseases, Division of Parasitic Diseases, Image Library. <http://www.dpd.cdc.gov/dpdx/HTML/Filariasis.asp?body=Frames/AF/Filariasis/body_Filariasis_o_volvulus.htm> Graphic Images of Parasites. “Onchocerca Volvulus.” < http://www.biosci.ohiostate.edu/~parasite/onchocerca.html> Accessed February 27, 2005. Janovy, Robert. Foundations of Parasitology 6ed. McGraw Hill Higher Education, New York. 2000. Okulicz, Jason. May 9, 2002. Onchocerciasis (River Blindness). E-Medicine. <http://www.emedicine.com/derm/topic637.htm> 2/26/05. Schmidt, D.Gerald & Roberts, Larry S. Foundation of Parasitology. 8th ed. USA. 2000. Zeibig, Elizabeth A. Clinical parasitology: A Practical Approach. W.B Saunders Company. USA. 1997 Markell and Voger. Medical parasitoloy. 8th ed. WB Saunders Company 1999 B. Thylefors. “Eliminating onchocerciasis as a public health problem.” Tropical Medicine and International Health. vol 9 no 4 pp a1–a3 suppl April 2004. <http://www.mectizan.org/library/eliminating_oncho.pdf> University of South Carolina- Microbiology and Immunology Online. “Parasitology.” < www.med.sc.edu:85/ parasitology/nematodes.htm> Accessed February 27, 2005. Bareza Rasoul Sasha McClain Kay Magnuson March 2005 6