* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Click Here for the Power Point - Pharmacists Society of the State of
Drug discovery wikipedia , lookup
Drug interaction wikipedia , lookup
Pharmaceutical marketing wikipedia , lookup
Polysubstance dependence wikipedia , lookup
Psychopharmacology wikipedia , lookup
Pharmacokinetics wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Compounding wikipedia , lookup
Adherence (medicine) wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Neuropharmacology wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Prescription costs wikipedia , lookup
Dextropropoxyphene wikipedia , lookup
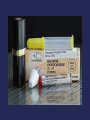
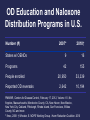
Role of Naloxone for Pharmacists John J. Faragon, Pharmacist, HIV Medicine Regional Pharmacy Director, NY/NJ AIDS Education and Training Center Objectives • Describe the correlation between prescription drug abuse and the rate of opioid related overdose deaths. • Discuss the pharmacology of naloxone and its use in the management of opioid overdose. • List and describe the currently available naloxone formulations and those under development. • Describe the role of the pharmacist in opioid overdose prevention and in the ESAP program. Overdose risk of those with prescriptions MMWR / January 13, 2012 / Vol. 61 / No. 1 Poisoning Deaths with Opioids NYSDOH Office of Quality and Patient Safety Bureau of Vital Statistics 2014 Rates of prescription painkiller sales, deaths and substance abuse treatment admissions (1999-2010) National Vital Statistics System, 1999-2008; Automation of Reports and Consolidated Orders System (ARCOS) of the Drug Enforcement Administration (DEA), 1999-2010; Treatment Episode Data Set, 1999-2009 Number of opioid-analgesic poisoning deaths, by involvement of benzodiazepines: United States, 1999–2011 Deaths from Opioid Overdoses are Preventable • Naloxone is the current antidote to reverse opioids and is safe and effective • First responders now use naloxone to immediately reverse the effects of opiate overdose What puts people at risk for overdose? • Mixing Drugs • Variation in strength and content of ‘street’ drugs (purity) • Tolerance changes • Using alone • Health issues, such as liver function, weight loss • Transient living – new dealers/new product • Thinking you “know everything” • Switching from sniffing/eating to injection What are the Signs/Symptoms of an OD? • Blue skin tinge- usually lips and fingertips show first • Body very limp • Face very pale • Passing out • Choking sounds or a gurgling/snoring noise • Breathing is very slow, irregular, or has stopped Strategies for Reducing Overdose Deaths • Prescription Monitoring Programs – Reduce diversion of prescription medications, not demonstrated to reduce overdose – Obvious concern about increase in heroin use • Methadone and Suboxone treatment • Abstinence-based drug treatment • Risk of overdose increases when relapse occurs • Community Based Education – Risk factors and identification of symptoms – Effective response, rescue breathing, 911 – Naloxone administration training • Naloxone Prescription Programs Why Are People Dying • Fear of stigma associated with drug use • Failure to recognize symptoms of overdose • Fear of police involvement • Bystanders not knowing what to do delays or provides ineffective response Opportunity for Family Intervention • Majority of ODs occur in the presence of others • ODs can be reversed by rescue breathing and/or Narcan (Naloxone) administration • Many younger drug users are still living at home or are still allowed to visit the home. • Treatment options can be discussed at the hospital with family present in the case of an overdose. • Realistic and useful education for families. ISTOP ISTOP - Benefits • Allows for better understanding of a patient’s controlled substance utilization based on recent controlled substance prescription history • Provides a quick, confidential online report to the practitioner and the pharmacist • Available 24/7 • Information is based on controlled substance prescription data received from nearly 5,000 pharmacies • Quick response at no cost to practitioner or pharmacists 911 Good Samaritan Law • Some individuals may fear that police will respond to a 911 call and that there will be criminal charges for themselves or for the person who overdosed. Those fears should NEVER keep anyone from calling 911 immediately. It may be a matter of life or death. • In September 2011, the 911 Good Samaritan Law went into effect to address fears about a police response to an overdose. This law provides significant legal protection against criminal charge and prosecution for possession of controlled substances, as well as possession of marijuana and drug paraphernalia. This protection applies to both the person seeking assistance in good faith as well as to the person who has overdosed. Class A-1 drug felonies as well as sale or intent to sell controlled substances are not covered by the law. NALOXONE PHARMACOLOGY AND ADMINISTRATION What is an Opioid Overdose? Opioid fits exactly in receptor Opioid receptor on brain The brain has many, many receptors for opioids. Too much opioid fitting in too many receptors slow and stop the breathing. Naloxone • Naloxone is an opioid receptor antagonist at mu, kappa, and delta receptors • Works at the opioid receptor to displace opioid agonists • Shows little to no agonist activity • Shows little to no pharmacological effect in patients who have not received opioids Naloxone • Reverses clinical and toxic effects of opioid overdose • Reverses respiratory depression, hypotension, sedation • Restores breathing • Reverses analgesia • Patients can experience withdrawal after naloxone administration Rapid Withdrawal Symptoms • Use of naloxone can cause – Agitation – Tachycardia – Pulmonary Edema – Nausea – Vomiting – Seizures Narcan reversing an OD Opioid Narcan Opioid receptor Narcan has a stronger affinity to the opioid receptors than the opioid, so it knocks the opioid off the receptors for a short time and lets the person breathe again. Overdose Prevention Using Nasal Naloxone • Simple device, medication and nasal spray • Naloxone is a pure opiate antagonist • No physiological effect other than blocking opiates • No adverse reactions, except for potential withdrawal • No potential for abuse or potential for OD Standard Naloxone Kit Components Atomizer BOX Syringe Glass vial Instructions Intranasal Naloxone Instructions Intramuscular naloxone • • • • • • A face mask for rescue breathing Two safety syringes 2 pre-filled vials of Naloxone 2 alcohol swabs 2 latex gloves 1 brochure reviewing OD and rescue steps. • Contact information for program Evzio auto injector Evzio Instructions Nasal Naloxone – Fast Track from FDA • Developed by AntiOp, but Reckitt Benkiser to attain rights upon approval • Commercial Intranasal naloxone formulation • U.S. National Institutes of Health's National Institute on Drug Abuse provided – $3 million grant over 3 years to help develop the spray. – FDA previously agreed to waive its $2 million new drug application fee What Intranasal Naloxone Might Look Like SAMHSA Tool Kit Released August 28, 2013 5 guidance documents • Community Members • First Responders • Prescribers • Patients • Family Members • Overdose Survivors Essential Knowledge • What does naloxone do? • Overdose recognition • Action – Call EMS – Administer naloxone • Hands on practice with device if possible • Recovery position If an OD happens… NALOXONE PROGRAMS OD Education and Naloxone Distribution Programs in U.S. Number (#) States w/ OENDs Programs People enrolled Reported OD reversals 2007* 2010† 9 16 42 155 20,950 53,339 2,642 10,194 PMMWR, Centers for Disease Control, February 17, 2012, Volume 61, No. 6ngeles, Massachusetts, Mendocino County, CA, New Haven, New Mexico, New York City, Oakland, Pittsburgh, Rhode Island, San Francisco, Wilkes County, NC and more * Knox, 2008 † Wheeler, E. NOPE Working Group - Harm Reduction Coalition. 2010 Massachusetts • Massachusetts compared interrupted time series of towns by enrollment in Opioid Education and Naloxone Distribution programs • 2912 kits distributed • 327 rescues, 87% by drug users; 98% effective EMS revived the other 3 Walley et al BMJ 2013 Community results • Fatal opioid OD rates compared no implementation • Program enrollment 1-100 per 100k population (ARR: 0.73) • Program enrollment >100 per 100,000 (ARR:0.54) • Of the 325 with 2 points of data on drug use: – No increase in reported use of opioids, alcohol, cocaine or number of substances used Walley et al BMJ 2013, Doe-Simkins et al BMC Public Health 2014 Project Lazarus - North Carolina • In response to some of the highest drug overdose death rates in the country, Project Lazarus developed a community-based overdose prevention program with routine physician prescription of naloxone when opioids were prescribed for pain. • Overdose death rate dropped from 46.6 per 100,000 in 2009 to 29.0 per 100,000 in 2010. • Unpublished data indicates rate of death has continued to drop to 7 deaths per 100,000 is 2011. (2010-2011 rates based on provisional data from OCME via Wilkes Co. Health Department.) Pain Med. 2011 Jun;12 Suppl 2:S77-85 CURRENT NYS LEGISLATION Case • RJ comes into your pharmacy. His son is actively using heroin and while most days he is not home, there are times when he comes back to stay and he is concerned • He requests that you provide him a nasal naloxone kit that he heard about at a support group What can you do?? A) Tell him that its not FDA approved so you cant get it, even with a prescription B) Refer him to the local harm reduction coalition office for a free kit C) Offer to call his physician for a prescription and fill it once you order it D) B and C E) None of the above are legal NYS Opioid Overdose Prevention Programs • A life-saving law took effect on April 1, 2006, making it legal in New York State for non-medical persons to be provided with naloxone and to administer it to another individual to prevent an opioid/heroin overdose from becoming fatal NYS Opioid Prevention Programs • Programs must register with the New York State Department of Health to operate an Opioid Overdose Prevention Program • Eligible providers include – – – – – – licensed health care facilities Individual health care practitioners drug treatment programs not-for-profit community-based Government agencies (state and local) Pharmacies • These programs train individuals how to respond to suspected overdoses including the administration of naloxone. Approximately 200 programs currently throughout the State. Over 1,000 reversals have been reported from these programs. 2014 Revisions to Law & Regs • Regulated programs through their prescribers may issue patient specific and non-patient specific prescriptions for naloxone. • Someone other than the prescriber or a pharmacist can be designated in the non-patient specific prescription to furnish the naloxone. • A non-patient specific prescription can be issued to an organization, with trained individuals in that organization having shared access to, and use of, that naloxone). • Shared access is beneficial to public safety and firefighting personnel, as well as staff in agencies serving individuals at risk for overdose. These responders no longer need to have unique, personal overdose kits dispensed to them under a patient-specific prescription. • They can instead share the naloxone dispensed to the organization for which they work under a non-patient-specific prescription. The advisability of shared versus individual overdose kits is determined by the prescription of the practitioner who authorized the drug to be dispensed. 2014 Revisions to Law & Regs • Pharmacists are able to dispense naloxone pursuant to patient-specific and non-patient specific prescriptions. • No dispensing should take place absent the recipient having had a training which includes how to recognize an overdose and how to respond to it appropriately. • Those appropriate responses should always include summoning EMS (calling 911), if it has not already taken place, and administering naloxone Opioid Overdose Prevention Program - Requirements • To operate Opioid Overdose Prevention Program, eligible providers must: – Register with the NYSDOH – Have a Program Director who has overall responsibility for the Program; – Have a Clinical Director (i.e., physician, physician assistant or nurse practitioner) who provides clinical oversight of the Program; – Recruit and train overdose responders; – Dispense opioid antagonists (i.e., naloxone) to trained responders – Establish and maintain a record keeping system and – Report administrations of opioid antagonists to NYSDOH – Report on quarterly basis number of kits distributed and responders trained Pharmacy Role Non-Patient Specific Prescriptions Model I • A pharmacy may register as an opioid overdose prevention program. – would need to identify a prescriber to act as its opioid overdose program clinical director. – clinical director could then issue a non‐patient specific prescription covering potential witnesses to an overdose as well as persons who may be at risk of experiencing an opioid overdose Pharmacy role Non-Patient Specific Prescriptions Model II • Pharmacists may work with non-pharmacy currently registered opioid overdose programs and dispense naloxone pursuant to a non‐patient specific prescription issued by the clinical directors of the registered programs Essential Knowledge Patients may need to be trained- there are videos available • What does naloxone do? • Overdose recognition • Action – Call EMS – Administer naloxone • Hands on practice with device if possible • Recovery position Pharmacy role Patient-Specific Dispensing • Pharmacists may dispense naloxone pursuant to a patient‐specific prescription in the same manner as any other prescription medication • Pharmacists may be pro-active in recommending co-prescribing to physicians • The New York State Department of Health is working with community pharmacies to ensure that naloxone in its various formulations is more routinely stocked Formulation • When being dispensed as a pharmacy benefit, community pharmacies can bill Medicaid FFS for up to 2 x 0.4mg/ml naloxone single-use pre-filled syringes or single-use vials only with a valid prescription from a Medicaid enrolled prescriber. • Up to 5 refills are allowed per prescription. Separate prescriptions are required for the drug vs. needles or syringe w/needle. Prescribetoprevent.org Summary • Role of naloxone crucial for prevention of opioid overdose related deaths • Programs from other states support both role of community and pharmacy involvement • Future formulations promising • Legislation supports non specific patient prescription and pharmacy involvement