* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Undiagnosed type 2 diabetes: recognise risk factors
Survey
Document related concepts
Transcript
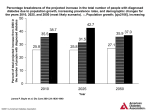
medication review The articles in this series are independently researched and compiled by PSA commissioned authors and peer reviewed. Undiagnosed type 2 diabetes: recognise risk factors Continuing Professional Development By Dr Shane Jackson Learning objectives After reading this article you should be able to: • Recognise risk factors for type 2 diabetes • Recognise signs and symptoms of type 2 diabetes • Describe the diagnostic pathway for diabetes • Discuss the possible risk of diabetes and weight gain with antipsychotic drugs • Recognise best practice management of diabetes. Competency standards (2010) addressed: 7.1.1, 7.1.2, 7.1.3, 7.2.3 Accreditation number: CAP110909f Case study Ms CW is a 55-year-old female resident of a rural aged care facility. She has the following medical conditions: • Mild intellectual disability • Epilepsy • Depression • Back pain • Hypertension. Ms CW takes the following medications: • Clonazepam 1mg twice a day, reduced two months ago from 2 mg twice a day. • Risperidone 0.5 mg at night commenced about six months ago • Ostevit D (cholecalciferol 1,000 IU) daily commenced 12 months ago – she refuses calcium supplements • Perindopril 4 mg daily • Oxcarbazepine (Trileptal) 600 mg twice a day • Paracetamol 500 mg, 1–2 tablets four times a day when necessary (frequency of use about twice a day) • Esomeprazole 20 mg daily • Folic acid 5 mg daily • Escitalopram 20 mg daily. Vol. 30 – September #09, 2011 Patient concerns Shane Jackson is a community pharmacy proprietor of two community pharmacies in Tasmania and is also a consultant pharmacist who performs medication reviews in aged care facilities. 778 Ms CW’s main concerns with regards to her health seemed to be increasing frequency of urination. There were also complaints of increasing urinary tract infections (UTIs), with four separate bouts of UTIs being treated with trimethoprim 300 mg daily for one week in the past five months. Ms CW’s current weight sits at 116 kg and this has increased by 11 kg over the past two years. Her last blood pressure when taken by the nursing staff was 155/60 mmHg and the previous one before that was 150/80 mmHg. Ms CW indicated that her pain is relatively well controlled with paracetamol when necessary. She has little, if any problems with reflux or indigestion since she was commenced on esomeprazole. According to her, she has not had any seizures for some time. When asked about her mood she says she feels fine, especially since the dose of escitalopram was increased a year or so ago. She is concerned about who is going to help her when her mother passes on (her mother also lives at the facility). She was also concerned about how well her mother was travelling with her diabetes. Some specific pathology tests results were: • Vitamin B12 224 pmol/L (>150 pmol/L) • Sodium 137 mmol/L (135–145 mmol/L) • Potassium 4.5 mmol/L (3.5–5.1 mmol/L) • Creatinine 64 micromol/L (44–80 micromol/L) • Hb 132 g/L (115–165 g/L) • MCV 91 fL (80–100 fL) Vitamin D 39 nmol/L (>75 nmol/L) prior to replacement therapy Upon discussion with the nursing staff regarding Ms CW they indicated that she is irritable and unsettled at times and that is why the doctor started risperidone. The nursing staff did not cite any specific concerns about Ms CW apart from her wandering around the facility and constant questioning Submit your answers online at www.psa.org.au and receive automatic feedback to better care for this resident. In addition, the use of clonazepam could be reviewed. She has tolerated a dose reduction in the past without recurrence of seizures and further dose reductions could be considered with modification of the oxcarbazepine dose if required. Benzodiazepines have significant adverse effects including excessive sedation, confusion, falls and can also increase the risk of agitation and depression. Drug related problem Inappropriate use of psychotropic medication and diabetes as a possible side effect of antipsychotic drug therapy. Ms CW appears to have a number of symptoms that may indicate possible diabetes. In addition to the symptoms she also has some risk factors that may increase the risk of developing diabetes. Inappropriate use of psychotropic medication use in aged care facilities has been an ongoing problem with multiple studies showing a high rate of benzodiazepine and antipsychotic use in aged care facilities.1–4 Previous Tasmanian research has shown that the prevalence of antipsychotic and benzodiazepine use in aged care facilities was 21% and 43% respectively.3 These medications are often used (sometimes inappropriately) to manage behavioural problems associated with dementia (BPSD), to treat anxiety and to assist with sleep disorders. These medications continue to be used in aged care facilities despite well‑known problems with falls, increased risk of cerebrovascular events and cognitive problems.5,6 In 2003, the FDA requested that additional warnings needed to be provided about the risk of diabetes with the use of risperidone.7 Lambert, et al.9 in 2007, identified that risperidone had a similar risk of causing diabetes as olanzapine and increased the risk of developing new onset diabetes by 1.6 compared to haloperidol.9 There have also been reports suggesting no link about a possible link between risperidone and diabetes, although weight gain has been shown with risperidone in these studies.10,11 In Ms CW’s case, because of a potential link between the development of diabetes, her weight gain and the inappropriate use of this agent, the risperidone should be ceased and her blood glucose level should be monitored accordingly. New-onset type 2 diabetes The Australian national prevalence study, AusDiab (the Australian Diabetes, Obesity and Lifestyle Study), showed that type 2 diabetes affects 7.4% of the Australian population in people aged 25 years or older and that there is one undiagnosed for every diagnosed person with type 2 diabetes.12 Case detection provides an opportunity to identify the estimated 500,000 Australians with undiagnosed type 2 diabetes.12 The AUSDRISK tool (www.health.gov.au) is used to identify those patients at high risk of having pre-diabetes or type 2 diabetes.13 Using this tool, Ms CW was identified at being at high risk of developing diabetes (score of 17) and this means that one in every Other high risk categories for type 2 diabetes include the following:14 • People with impaired glucose tolerance, and/or high impaired fasting glucose. • Aboriginal and Torres Strait Islanders aged 35 and over. • Certain high-risk non-English speaking background people aged 35 and over (specifically Pacific Islanders, people from the Indian subcontinent, people of Chinese origin). • People aged 45 and over who have one or more of the following risk factors: – Obesity (BMI ≥30 kg/m2 as an indicator) – Hypertension • All people with clinical cardiovascular disease (myocardial infarction, angina, stroke or peripheral vascular disease). • Women with polycystic ovarian syndrome who are obese (BMI ≥30 kg/m2 as an indicator). In conjunction with the nursing staff a fasting capillary glucose level was taken and the result was 10.2 mmol/L. The oral glucose tolerance test is not necessary for every individual to confirm a diagnosis of diabetes and may be used in cases where there is an equivocal result. The diagnosis of diabetes is made in the following ways:14 • Symptoms of diabetes (see Box 1) and a random (non fasting) blood glucose >11 mmol/L • Fasting plasma glucose ≥7.0 mmol/L • 2-hour plasma glucose >11 mmol/L during an oral glucose tolerance test (OGTT) 779 Vol. 30 – September #09, 2011 In Ms CW’s case it appears that there is no clear indication for the use of risperidone and that this is being used to manage behaviours that the nursing staff find troublesome. Antipsychotic medications are associated with significant adverse effects, such as an increase in mortality compared to placebo (mostly due to cardiovascular events (e.g. heart failure, sudden death) or infections (e.g. pneumonia).7 Other side effects include somnolence, gait disturbance, urinary incontinence, aggression and confusion.8 Given the consequences of using antipsychotic medication it would appear that the risperidone should be ceased and the nursing staff should manage any behavioural concerns that Ms CW has with diversional techniques. In this case, the diversional therapist from the facility was asked to develop a program to assist the nursing staff seven patients will develop diabetes with this score. The Australian Type 2 Diabetes Risk Assessment Tool was developed by the Baker IDI Heart and Diabetes Institute and is a validated tool that is useful for health professionals to use to inform and risk stratify patients for diabetes. The Management of Diabetes in General Practice Guidelines suggest that asymptomatic people at high risk of undiagnosed diabetes should be identified and screened by measurement of plasma glucose.14 Continuing Professional Development of care staff about what they were doing. They also said she is not very compliant with good dietary practices and they believed this was the reason behind her weight gain. They indicated that Ms CW and her mother are often found eating lollies and chocolates after they go on outings. A practising dietitian has not seen Ms CW or her mother since they have been at the facility. medication review The articles in this series are independently researched and compiled by PSA commissioned authors and peer reviewed. Box 1. Symptoms of diabetes Vol. 30 – September #09, 2011 Continuing Professional Development • • • • • • • • • • • • Excessive thirst Polyuria Tiredness and lethargy Hunger Slowly healing wounds Increased infections Blurred vision Weight gain Mood abnormalities Headaches Dizziness Leg cramps. – Blood pressure – noting her target to minimise complications from diabetes (target <130/80 mmHg). In Mrs CW’s case an increase in her dose of perindopril may be necessary as ACE inhibitors and angiotensin II receptor antagonists have a beneficial effect on reducing cardiovascular and renal complications of diabetes.15 (See below for hypertension management steps) – Review immunisation status (influenza and pneumococcal) and ensure they are up to date.15 – Optometrist or ophthalmologist review.15 In Ms CW’s case, the risk factors and the finding of a random BSL measurement of 10.2 mmol/L it is possible that she has developed diabetes given her symptoms and risk factors. Recommendations from the Royal Australian College of General Practitioners and Diabetes Australia is that any diagnosis of diabetes is based on plasma blood glucose levels from a laboratory, and an oral glucose tolerance test if required, and in Ms CW’s case this will need to be confirmed by her GP. • Dietician and/or podiatry review if necessary.15 Recommendations to the GP Step 1 – Healthy eating, physical activity, weight control • In light of the possible link between risperidone and diabetes the risperidone should be ceased. Also, her behaviour, could be best managed with diversional therapy. • Whilst addressing the inappropriate use of psychotropic medications, clonazepam could be further reduced in dose as she has been seizure free for some time and a previous halving in dose was tolerated well. • Consider reviewing Mrs CW in light of her risk factors for diabetes and her most recent fasting blood glucose level of 10.2 mmol/L. • If her fasting plasma glucose confirms diabetes consider the following: – Pathology tests15 oo Hba1c oo Lipids – see below for dyslipidaemia targets and management. oo Albumin:creatinine ratio (detects presence of microalbuminuria) 780 • Consider the use of low dose aspirin for cardiovascular event prevention.15 Management targets and options for type 2 diabetes How to best achieve target blood pressure management in diabetes14 Step 2 – ACE inhibitor or ATII receptor antagonist if ACE inhibitor not tolerated Step 3 – ACE inhibitor (or ATII receptor antagonist as above) and thiazide diuretic Step 4 – Calcium channel blocker or beta-blocker Management of dyslipidaemia in diabetes Dyslipidaemia is common in patients with diabetes and is an independent risk factor for the macrovascular complications of diabetes. It is therefore important to identify and treat dyslipidaemia. Generally, dietary measures should be attempted for 3–6 months and if this is unsuccessful then pharmacological treatment can be implemented. The National Heart Foundation targets for lipids in patients with diabetes is as follows:16 • Total Cholesterol – <4.0 mmol/L • Triglycerides – <1.5 mmol/L • HDL – >1.0 mmol/L • LDL – <2.5 mmol/L Renal disease Detection of proteinuria (protein in the urine) is important to identify early renal damage from diabetes. Initially, low grade albuminuria (albumin in the urine) can occur and at this stage can often be managed with tight blood pressure and glycaemic control.14 The albumin:creatinine ratio (ACR) is useful for detecting and monitoring microalbuminuria. Outcomes of the medication review • Risperidone was ceased and the clonazepam dose was reduced initially to 0.5 mg in the morning and 1 mg at night – planned dose reductions of ~20% of the total dose per month. • The GP performed a fasting plasma glucose test – 11.4 mmol/L and a repeat test one week later – 11.7 mmol/L and a diagnosis of type 2 diabetes was made. • Hba1c performed – 8.3% • Lipids – HDL – 1.3 mmol/L – LDL – 4.5 mmol/L • ACR – 3.3 mg/mmol (0-3.5 mg/mmol) • Commencement of metformin 500 mg immediate release once a day • 3 months trial of diet and lifestyle modification (GP unconvinced that this will result in a discernable change and a statin will most likely be required) • Blood pressure – average taken by nursing staff and GP over a 2-week period was 147/87 mmHg. Dose increase of perindopril arginine to 10 mg daily. • Influenza and pneumococcal vaccination given. • Referral for dietitian and optometrist review. • Commencement of aspirin 100 mg daily. References 1. Westbury J, Tichelaar L, Peterson G, Gee P, Jackson S. A 12-month follow-up study of ‘RedUSe’: a trial aimed at reducing antipsychotic and benzodiazepine use in nursing homes. Int Psychogeriatr 2011;1-10. 2. Westbury J, Beld K, Jackson S, Peterson G. Review of psychotropic medication in Tasmanian residential aged care facilities. Australas J Ageing 2010;29:72–6. 3. Westbury JL, Jackson S, Peterson GM. Psycholeptic use in aged care homes in Tasmania, Australia. J Clin Pharm Ther 2010;35:189–93. medication review The articles in this series are independently researched and compiled by PSA commissioned authors and peer reviewed. Continuing Professional Development 4. Westbury J, Jackson S, Gee P, Peterson G. An effective approach to decrease antipsychotic and benzodiazepine use in nursing homes: the RedUSe project. Int Psychogeriatr 2010;22:26–36. 5. Mansdorf IJ, Sharma R, Perez M, Lepore AM. Falls reduction in long-term care facilities: a preliminary report of a new internet-based behavioral technique. Journal of the American Medical Directors Association 2009;10:630–3. 6. Wilson KC, Mottram PG, Vassilas CA. Psychotherapeutic treatments for older depressed people. Cochrane database of systematic reviews 2008:CD004853. 7. US FDA. FDA Public Health Advisory: Deaths with antipsychotics in elderly patients with dementia; 2003. 8. Deberdt WG, Dysken MW, Rappaport SA, et al. Comparison of olanzapine and risperidone in the treatment of psychosis and associated behavioral disturbances in patients with dementia. Am J Geriatr Psychiatry 2005;13:722–30. 9. Lambert BL, Cunningham FE, Miller DR, Dalack GW, Hur K. Diabetes risk associated with use of olanzapine, quetiapine, and risperidone in veterans health administration patients with schizophrenia. Am J Epidemiol 2006;164:672–81. 10. Farwell WR, Stump TE, Wang J, Tafesse E, L’Italien G, Tierney WM. Weight gain and new onset diabetes associated with olanzapine and risperidone. J Gen Intern Med 2004;19:1200–5. 11. Moisan J, Gregoire JP, Gaudet M, Cooper D. Exploring the risk of diabetes mellitus and dyslipidemia among ambulatory users of atypical antipsychotics: a population-based comparison of risperidone and olanzapine. Pharmacoepidemiol Drug Saf 2005;14: 427–36. 12. Dunstan DW, Zimmet PZ, Welborn TA, et al. The rising prevalence of diabetes and impaired glucose tolerance: the Australian Diabetes, Obesity and Lifestyle Study. Diabetes Care 2002;25:829–34. Questions 13. Colagiuri S, Davies D, Girgis S, Colagiuri R. National Evidence Based Guideline For Case Detection and Diagnosis of Type 2 Diabetes. Canberra; 2009. 14. Diabetes Australia. Diabetes Management in General Practice 2009/2010; 2009. 15. Chadban S, Howell M, Twigg S, et al. National Evidence Based Guideline for Diagnosis, Prevention and Management of Chronic Kidney Disease in Type 2 Diabetes. Canberra; 2009. 16. Tonkin A, Barter P, Best J, et al. National Heart Foundation of Australia and the Cardiac Society of Australia and New Zealand: position statement on lipid management – 2005. Heart Lung Circ 2005;14:275–91. A score of 3 out of 4 attracts 0.75 CPD credits. 1. Which of the following is LEAST likely to be an adverse effect of risperidone? a) Weight gain. b)Falls. c) Unsteady gait. d) Leg cramps. 2. Approximately how many Australians are estimated to have UNDIAGNOSED type 2 diabetes? a)250,000. b)500,000. c)750,000. d)1,000,000. c) Perform a capillary BSL test for confirmation. d) Repeat the test in 12 months. 3. What would be the MOST appropriate assessment for a person with a laboratory performed fasting BSL of 9.3 mmol/L? a) Diagnosis of diabetes. b) Perform an oral glucose tolerance test. 4. Which of the following is NOT generally recognised as a symptom of type 2 diabetes? a)Hunger. b)Thirst. c) Weight loss. d) Blurred vision. e)Headaches. September 2011 Note: The CPD questions are now at the end of each article. Vol. 30 – September #09, 2011 PSA members can answer online at www.psa.org.au and receive automatic feedback. •You will need to login to submit your answers online. If you do not have member access details, you can request them via a link from the login page. •Select Pharmacist Members from the blue, left hand side menu. •Select Submit Answers. •Select Australian Pharmacist CPD. Submit your answers before 1 November 2011 or fax/mail to: PSA Fax: PSA Mail address: 782 Australian Pharmacist Continuing Professional Development (CPD) is a central element of PSA’s CPD&PI program. It is also part of the New Zealand College of Pharmacists (NZCP) education program for NZ pharmacists. The CPD section is recognised under the PSA CPD&PI program as a Group 2 activity. Members can choose which articles they want to answer questions on and get CPD credits based on the questions they answer. The credits allocated to each section and the pass mark are shown with the questions. CPD credits are allocated as follows: a minimum of 6 out of 8 questions correct attracts 1.5 credits, a minimum of 4 out of 5 questions correct attracts 1 credit, and a minimum of 3 out of 4 questions correct attracts three quarters of a credit. If not submitting online, write the correct answers in the spaces provided on the answer panel on the back of the address sheet, fill in your name, member number and address details, then either mail or fax the answer page to the relevant address and fax number for marking. online at www.psa.org.au and receive automatic feedback (03) 9389 4044 PSA CPD answers PSA Victorian Branch Level 1, 381 Royal Parade PARKVILLE VIC 3052 NZCP Fax: (04) 381 4786 NZCP Mail address: NZCP CPD answers PO Box 11 640 Wellington