* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Wong, L
Survey
Document related concepts
Transcript
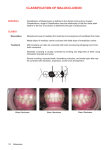
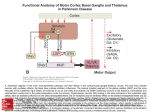
Lisa Wong, OD Vision Therapy and Low Vision Rehabilitation Resident Southern College of Optometry I. Case History Patient demographics: 42 year-old white male Chief complaint: Constant diplopia, horizontal and vertical Ocular, medical history: o First seen 7/10/15 for an optometric consult at a rehabilitation facility after suffering a thalamic hemorrhage on 7/2/15. o No previous eye examinations o Medical history remarkable for sleep apnea, no other known conditions. Medications: None currently Other salient information: o Inpatient at rehabilitation hospital 7/8-7/22/15, presented to SCO on 7/23/15 for visual efficiency examination. II. Pertinent Findings Clinical: o Refractive: Emmetropic with early presbyopia. o Ocular motility: Horizontal eye movements: full Vertical eye movements: 7/10: 30% past midline superiorly and inferiorly 7/21: 25% inferiorly 7/23: 10% superiorly and inferiorly 8/20: 50% superiorly, 40% inferior Saccades: 5/2/5/5 on NSUCO Pursuits: Unable to complete test due to vertical gaze palsy, no head or body movement o Ocular alignment: 7/10: 20Δ IAXT with 5 Δ right hypertropia at near 7/21: 9 Δ right hypertropia 7/23: 18 Δ CAXT, 10 Δ right hypertropia distance and near 8/20: 6 Δ CAXT with 4 Δ right hypertropia at near, 4 Δ CAXT with 5 Δ right hypertropia at distance o Motor-Free Visual Perceptual Test-3 Raw Score=50, Standard Score=81, percentile rank 10% Difficulty with figure-ground and short term memory o Rapid Automatized Naming/Rapid Alternating Stimulus Test Numbers (SS=107), Letters (SS=101), 2-set (SS=107) and 3-set (SS=109): Average Colors (SS=87): Below average Objects (SS=67): Very poor o King-Devick: Test I: 26s; test II: 25s, Test III: 26s. Total: 77 seconds o Humphrey Visual Field 24-2: Scattered defect inferior OD, no defect OS. Questionable reliability. Physical: o Patent foramen ovale o Unknown cerebral vasculature abnormality (updated medical records will be requested) Laboratory studies: o Sodium, chloride, potassium, bicarbonate, platelets, hematocrit, white blood count, BUN: normal o ALT: high o Blood toxicity screen: barbiturates Radiology studies: MRI/CT – consistent with thalamic hemorrhage Others: N/A III. Differential Diagnosis Vertical gaze palsy secondary to bilateral medial thalamic hemorrhage IV. Diagnosis and Discussion Thalamic infarctions comprise 11% of all vertebrobasilar infarctions, and are categorized based on the four main thalamic arterial blood supplies. Inferolateral infarcts are the most common (45%), followed by areas supplied by the paramedian artery (35%)— which includes the medial area—and polar arteries (12.5%). In one third of the population, the polar artery is missing and its territory is supplied by the paramedian artery. Medial thalamic infarcts are characterized by deficiencies in short term memory, attention, intellect, and vertical gaze. Mild hemiparesis or hemiataxia may be involved, but were not seen in this case. Unilateral thalamic lesions typically cause upgaze palsies, while bilateral lesions cause upgaze, downgaze, or combined vertical palsies with other abnormalities such as convergence paralysis, bilateral internuclear ophthalmoplegia, and a Horners syndrome. a. A study by FJ Rowe and the VIS Group in 2009 found that strabismus occurred in 16.5% of patients after a stroke, with 24% of those attributed to insults to subcortical areas (cerebellum, brainstem, basal ganglia, or thalamus). 64% of their study sample (n=512) received intervention (Fresnel prism, orthoptic exercises, spectacles, total or sector occlusion) to alleviate diplopia. Some patients may show improvement in symptoms with little to no intervention. In patients with thalamic strokes, evidence of spontaneous recovery of downward eye movements has been reported; however, the upgaze palsy appears more persistent (Clark and Albers). V. Treatment, Management Treatment: o 60mm binasal occlusion with inferior sector occlusion prescribed at rehabilitation hospital. Initially attempted 10 Δ BI OD, OS Fresnel prism, but patient preferred binasals. o Vision therapy with binasal occlusion began on 7/30/15 Week 1: Thumb rotations, head rotations, vertical saccades, closed eye rotations, vertical OKN Vertical OKN reflex absent Week 2: Thumb rotations, vertical saccades, VO star, vertically split Marsden ball Unable to vertically align Marsden ball, with or without binasal occlusion at any distance. Week 3: Thumb rotations, vertical saccades, VO star Week 4: Thumb rotations, vertical saccades, vertically split Marsden ball, vertical OKN Vertical OKN response present superior to inferior OD, OS. Able to vertically align Marsden ball easily, with 37mm binasal occlusion, from 6 inches to 8 feet away. Response to treatment: o Patient has decreased binasal occlusion from 60mm to 37mm, with a marked reduction in exotropia. He is able to fuse at arm’s length without binasal occlusion. VI. Conclusion Clinical Pearls: o Vertical gaze palsies are the most common ocular motility defect in a thalamic insult. Vision therapy can be an effective treatment to improve ocular motility ranges. o Binasal occlusion may help fusion in these patients with vertical diplopia. Bibliography: 1. Adamec, I., Barun, B., Lakusic, DM., Ozretic, D., Brinar, VV., and Habek, M. “Neuro-ophthalmic Manifestations of Thalamic Stroke.” Neuro-Ophthalmology. 2011; 35(3): 121-124 2. Afifi, AK., Bergman, RA. Functional Neuroanatomy: Text and Atlas, 2nd edition. New York: Lange Medical Books/McGraw-Hill. 2005. Print. 3. Clark, JM., Albers, GW. “Vertical Gaze Palsies from Medial Thalamic Infarctions Without Midbrain Involvement.” Stroke. 1995; 26: 1467-1470. 4. Jones, E. and Rowe, FJ. “Ocular motility consequences following lesions of the thalamus: a literature review.” British and Irish Orthoptics Journal. 2009; 6: 40-46. 5. Perren, F., Clarke, S., Bogousslavsky, J. “The Syndrome of Combined Polar and Paramedian Thalamic Infarction.” Archives of Neurology. 2005; 62(8): 1212-1216 6. Rowe, FJ and VIS Group UK. “The profile of strabismus in stroke survivors.” Eye. 2010; 24: 682685 7. Wians, FH. “Blood Tests: Normal Values.” Merck Manual Online, Professional Version. Accessed online 24 Aug 2015. <http://www.merckmanuals.com/professional/appendixes/normallaboratory-values/blood-tests-normal-values#v8508814>