* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download 260
Henipavirus wikipedia , lookup
Brucellosis wikipedia , lookup
Clostridium difficile infection wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Cross-species transmission wikipedia , lookup
Oesophagostomum wikipedia , lookup
Meningococcal disease wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Marburg virus disease wikipedia , lookup
Onchocerciasis wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Rocky Mountain spotted fever wikipedia , lookup
Sarcocystis wikipedia , lookup
Sexually transmitted infection wikipedia , lookup
Herpes simplex virus wikipedia , lookup
Hepatitis B wikipedia , lookup
Chagas disease wikipedia , lookup
Schistosoma mansoni wikipedia , lookup
Neisseria meningitidis wikipedia , lookup
Schistosomiasis wikipedia , lookup
Visceral leishmaniasis wikipedia , lookup
Leptospirosis wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
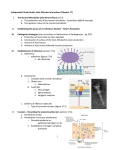
260 summer 2016 pathogenesis Clicker questions about viral replication • Which viruses can use the host’s replication enzymes to make new genomes • Which viruses have a genome that can be directly used as an mRNA • Which viruses require a RNA-dep RNA pol • Which viruses need to carry the RNA-dep RNA pol in the capsid • Reverse transcriptase uses a ____ template to make ____ A = DNA all RNA virusesC =C RNA = all RNA viruses except retroviruses DNAviruses DNA BBB === dsRNA DNA virus RNA DNA not RNA AA==dsDNA virus C = “+”sense RNA CD == RNA “-”sense RNA E= retrovirus D=retroviruses only About PCR • Compare replication to PCR • 1. list the things you need (reagents, enzymes) for replication and in what order • 2. list the things you put into your PCR tube (reagents, enzymes). • 3. compare – for the things in replication that are missing in the PCR tube, what did you add to fill that missing role? The study of disease Pathogenesis – the study of disease progression Next class – epidemiology we’ll study disease again but from a public health perspective Pathogenesis (chapter 16) Principles of disease aka The Chapter of Many Definitions Why do care? • What specific agent causes disease • How does the agent cause disease in the body • How infectious agents are spread A brief history • Diseases and plagues attributed to supernatural forces, incurable and terrifying • Observation: disease seems to be communicable • 1600s there are microbes • 1800s Microbes cause disease • Robert Koch (German physician 1843-1910) – systematic proof of causative agent Koch’s Postulates 1. The same pathogen must be present in every case of the disease 2. The pathogen must be isolated from the diseased host and grown in pure culture 3. The pathogen from the pure culture must cause the disease when it is inoculated into a healthy, susceptible lab animal 4. The pathogen must be isolated from the inoculated animal and must be shown to be the original organism Koch’s Postulates Obtain pure culture of the organism Same organism is present in every case of the disease Pure culture used to infect healthy lab animal causes the disease Figure 14.3 Koch’s Postulates Organism cultured from infected animal is identical to original infection Figure 14.3 Koch’s Postulates • Koch's postulates can be used to prove the cause of an infectious disease.. • But can Koch’s postulates be used to identify the agent/microbe responsible for all diseases? – Some pathogens can cause several disease conditions – Some pathogens cause disease only in humans – Some pathogens are not easily cultivated Pathology, Infection, and Disease • • • • • Pathology: The study of disease Etiology: The study of the cause of a disease Pathogenesis: The development of disease Infection: Colonization of the body by pathogens Disease: An abnormal state in which the body is not functioning normally Normal Microbiota and the Host • Transient microbiota may be present for days, weeks, or months then disappear • Normal microbiota permanently colonize the host • Symbiosis is the relationship between normal microbiota and the host Representative Normal Microbiota Figure 14.1 Is this bad news? Symbiosis • In commensalism, one organism benefits, and the other is unaffected • In mutualism, both organisms benefit • In parasitism, one organism benefits at the expense of the other • Some normal microbiota are opportunistic pathogens such as? Normal Microbiota on the Human Body Table 14.1 What is the role of normal microbiota? Normal Microbiota and the Host • Microbial antagonism is a competition between microbes. • Normal microbiota protect the host by – Occupying niches that pathogens might occupy – Producing waste eg. acids – Producing bacteriocins • Probiotics: Live microbes applied to or ingested into the body, intended to exert a beneficial effect Effect of antibiotics • Why are you at risk of a yeast infection or bacterial GI illness after taking antibiotics? Principles of disease • Symptom: A subjective change in body function that is felt by a patient as a result of disease • Sign: An objective change in a body that can be measured or observed as a result of disease • Syndrome: A specific group of signs and symptoms that accompany a disease For example • You catch a respiratory virus • You feel tired, have a headache, your sinuses itch, you have a sore throat • The doctor finds swollen lymph nodes, notes an elevated body temperature and views redness in your throat and nasal passages • What are the symptoms, signs • How are the signs and symptoms related to the concept of a syndrome The Stages of a Disease Figure 14.5 Development of disease • Incubation period – from transmission to first symptoms • Prodromal period – early mild symptoms • Period of illness – period of severe symptoms • Period of decline – number of pathogens declines (may overlap with severe symptoms) • Period of convalescence (numbers continue to drop; mild or no symptoms) For example • • • • 10/8 – your partner sneezes on you 10/10 – sore throat 10/12 – liquid goo phase, sneezing, fever 10/17 – back to salsa dancing! Give the dates of the incubation period, prodromal period and period of illness Severity or Duration of a Disease • Acute disease: Symptoms develop rapidly • Chronic disease: Disease develops slowly • Subacute disease: Symptoms in between acute and chronic • Subclinical disease: infection without noticeable symptoms • Latent disease: Disease with a period of no symptoms when the causative agent is inactive Order of disease • Primary infection: Acute infection that causes the initial illness • Secondary infection: Opportunistic infection after a primary (predisposing) infection For example • 1. a few weeks after the salsa dancing success, you find you have a bacterial sinus infection • 2. a patient with HIV develops thrush Types of infection • Local infection: Pathogens are limited to a small area of the body • Systemic infection: Microbe or toxins spread throughout the body by the blood/lymph • Focal infection: Infection that began as a local infection spreads via the blood/lymph Spread of disease – inside the body • • • • Bacteremia: Bacteria present in the blood Toxemia: Toxins present in the blood Viremia: Viruses present in the blood Septicemia: “blood poisoning” - systemic infection arising from multiplication of pathogens in the blood Question • What’s the difference between bacteremia and bacterial septicemia • What’s the difference between bacteremia and toxemia Spread of disease – in the population • Communicable disease: A disease that is spread from one host to another • Contagious disease: A disease that is easily spread from one host to another • Noncommunicable disease: A disease that is not transmitted from one host to another – SUCH AS?? For example • Determine whether these are communicable or not and if so, are they contagious • HIV • Influenza • Botulism Mechanisms of Pathogenicity • Pathogenicity: Ability to cause disease • Are all microbes pathogens? • Virulence: The extent of pathogenicity – ID50: Dose that causes infection in 50% of population – LD50: Dose of toxin that is lethal for 50% of test population Questions • For a given microbe, is the ID50 the same in every situation? • Which is less likely to cause disease – a microbe with a higher ID50or lower ID50? Toxins Toxin Botulinum Shiga toxin Staphylococcal enterotoxin LD50 0.03 ng/kg 250 ng/kg 1350 ng/kg Which organism has the most potent toxin?? reservoirs • • • • • What do you think? Human Animal (zoonotic) Environment Carrier – human without symptoms For example • • • • • What is the reservoir for HIV Rabies Mycobacterium tuberculosis Clostridium botulinum Modes of transmission • Direct contact transmission – touch • Indirect contact transmission - fomite • Vehicle transmission – a vector brings the pathogen – Mechanical vector (rides the roof) – Biological vector (rides inside) question • What is the reservoir for malaria • What kind of transmission is it? – Direct contact, indirect contact, zoonotic, mechanical vector, biological vector – More than one right answer Portals of Entry • Preferred route of entry – Some have multiple routes (e.g. Yersina pestis causes plague; B. anthracis causes anthrax) – Other routes may not cause disease (e.g. Salmonella typhi on skin; Streptococci pneumoniae that are ingested) Portals of Entry • How do microbes get into your body? • Mucous membranes – GI tract, respiratory tract most common – Genitourinary tract, conjunctiva (membrane of eyes) • Skin – Major barrier to entry, mostly inaccessible to pathogens – Some openings: hair follicles, sweat gland ducts – Hookwork larvae can bore through skin; some fungi grow on keratin • Parenteral route – Penetration of skin /mucous membranes (punctures, cuts, bites, etc.) Bacillus anthracis Portal of Entry Skin ID50 10–50 endospores Inhalation 10,000–20,000 endospores Ingestion 250,000–1,000,000 endospores Which portal is most likely to cause infection?? So for example • • • • • • Plasmodium (malaria) – what route? C botulinum (botulism) – what route? Influenzavirus – what route? HIV (AIDS) – what route? Bacillus anthracis (anthrax) – what route? Why are these routes different? biofilms • ~65% of infections – Dental plaque – Implants – Contact lenses Adherence capsules • Can prevent phagocytosis – make cells “invisible” Alveolar macrophage attacking E. coli; RBC at top left Capsules • Capsules prevent phagocytosis – Streptococcus pneumoniae; Haemophilus influenzae; Bacillus anthracis – Often avirulent without capsule since phagocytosed (eg S. pneumoniae) – Note - many nonpathogenic bacteria also produce capsules (capsulation alone is not sufficient to designate a pathogen) Alveolar macrophage attacking E. coli; RBC at top left Cell Wall Components – M protein resists phagocytosis • Surface of fimbriae Streptococcus pyogenes (strep throat, scarlet fever, TSS) – Opa protein inhibits T helper cells • fimbriae Neisseria gonorrhoeae – Mycolic acid resists digestion Waxy lipid where? Mycobacterium tuberculosis Hijacking host Cytoskeleton Cytoskeleton filament - actin Microbes (e.g. Salmonella; E. coli) produce invasins that rearrange actin filaments of cytoskeleton membrane ruffling, penetration of cell Some species use actin to propel themselves through and between cells (e.g. Shigella; Listeria; Ricksettia) Membrane Ruffling Invasins: alters host actin to enter host cell eg.Salmonella Figure 15.2 Comet tails Some bacteria organize actin behind them for propulsion eg.Listeria, Shigella, Ricksettia Damage to Host Cells • Consumption of host’s nutrients • Direct damage in vicinity of invasion • TOXINS blood/lymph distant sites Consumption of host nutrients • Lack of iron limits bacterial growth • Secrete siderophores to capture • Take up from blood; some lyse cells to release Direct damage • Disrupt host cell function • Release wastes • Rupture release more viruses/bacteria Human Herpes Virus 6 budding off Toxins • • • • • Toxin: Substance that contributes to pathogenicity Toxigenicity: Ability to produce a toxin Toxemia: Presence of toxin in the host's blood Toxoid: Inactivated toxin used in a vaccine Antitoxin: Antibodies against a specific toxin All about toxins • May be transported by blood or lymph what is the important implication? • May fever, diarrhea, shock, cardiovascular and nervous system disruption • ~220 known types; ~40% damage cell membranes • Two general types: Exotoxins Endotoxins What do you think the difference is? Exotoxins and Endotoxins Proteins produced by bacteria and secreted or released following lysis Lipid A of lipopolysaccharides (LPS) of outer membrane of Gram negatives Figure 15.4 Exotoxins • Specific for a structure or function in host cell Figure 15.4a Naming exotoxins • By type of cell affected – (e.g., neurotoxins, cardiotoxins, hepatotoxins, leukotoxins, enterotoxins, cytotoxins) – What does each affect? • By associated disease – (e.g., diphtheria toxin, tetanus toxin) – What disease is associated with each toxin? • By bacterium producing – (e.g., botulinum toxin, Vibrio enterotoxin – What organism produces each of these toxins? What are exotoxins, really? Proteins, usually enzymes even small amounts harmful 1 mg botulinum exotoxin can kill 1 million guinea pigs Genes usually carried on ?plasmids, phage – WHY?? Soluble in host fluids transported widely What are exotoxins, really? Proteins, usually enzymes even small amounts harmful 1 mg botulinum exotoxin can kill 1 million guinea pigs Genes usually carried on ?plasmids, phage Soluble in host fluids transported widely Mode of action– 3 main modes Inhibit metabolism (usually protein synthesis) Destroy parts of host cells overactivate immune system What are exotoxins, really? Proteins, usually enzymes even small amounts harmful 1 mg botulinum exotoxin can kill 1 million guinea pigs Genes usually carried on ?plasmids, phage Soluble in host fluids transported widely Mode of action Inhibit metabolism (usually protein synthesis) Destroy parts of host cells overactivate immune system Types A-B membrane-disrupting superantigen Exotoxin type: A-B Exotoxin eg. diptheria, botulinum, tetanus, vibrio (cholera) Two parts – A and B, proteins B (binding) – binds host receptor A-B enter A and B separate A – enzyme, usually inhibits protein synthesis Figure 15.5 Membrane-Disrupting exotoxin Lyse host’s cells in one of two ways Making protein channels in the plasma membrane – Leukocidins Why is this bad? – Hemolysins – Streptolysins (b-hemolysis Streptococcus) Disrupting phospholipid bilayer – Phospholipases remove polar head –gas gangrene (C. perfringens) Exotoxin type: Superantigens • • • • Evoke intense immune response Proliferation T cells (lymphocytes) excess cytokines Symptoms: fever, nausea, vomiting, diarrhea, shock, death Eg. Staphylococcus (food poisoning, toxic shock syndrome) Last words about exotoxins Exotoxins are disease specific Due to exotoxin, not bacterial infection foodborne intoxication botulism, staphylococcal food poisoning Fighting exotoxins Body makes antibodies (antitoxins) provide immunity Inactivate (heat, HCHO, iodine) toxoids Toxoids used as vaccine to stimulate antibody production tetanus, diphtheria Endotoxins – part of the cell • Part of outer membrane of Gram-negatives – Lipid portion of LPS, called lipid A – Death and lysis of bacteria; antibiotics can worsen • Stimulate macrophages -release high level cytokines – Fever, nausea, vomiting, diarrhea, sometimes shock, death (similar to but not as potent as superantigen exotoxins…) Remember this? Endotoxins and the Pyrogenic Response Figure 15.6 Damage to Host Cells Exotoxin Source Relation to microbe Chemistry Neutralized by antitoxin? LD50 Gram? ?made/part of What kind of molecule? Y/N? Need a little or a lot? Figure 15.4a Exotoxin Source Relation to microbe Chemistry Neutralized by antitoxin? LD50 Mostly Gram + Made by growing cell Protein Yes Small Figure 15.4a Endotoxins Source Gram? Relation to Microbe Made/part? Chemistry Molecule? Neutralized by Antitoxin? LD50 Y/N? How much you need? Figure 15.4b Endotoxins Source Relation to Microbe Chemistry Neutralized by Antitoxin? LD50 Gram Outer membrane Lipid A No Relatively large Figure 15.4b Horizontal transmission • Where do bacteria get their toxin genes? Horizontal transmission • Transformation • Conjugation • Transduction A word about plasmids • • • • • Circular small DNA containing 4-5 genes What did we just transform into E. coli in lab? What genes were on that plasmid? DIAGRAM WHITE BOARD Many antibiotic resistance genes are transmitted between species by sharing plasmids – Transformation and conjugation Plasmids can code for • Antibiotic resistance genes – An example from lab? • Metabolic enzymes – Examples from this class? • AND toxins – – – – – Tetanus neurotoxin Staphylococcal enterotoxin Dextransucrase (Streptococcus mutans tooth decay) Adhesins and coagulase (Staphylococcus aureus) Fimbria (Enteropathogenic E. coli) Other ways to get toxins: transduction • Lysogenic conversion: prophage in chromosome – – – – – Shiga toxin of E. coli O157 Virbrio enterotoxin of Vibrio cholerae (cholera) Botulinum neurotoxin Capsule of Streptococcus pneumoniae (virulence factor) Diphtheria toxin Exotoxins due to Lysogenic Conversion Exotoxin Corynebacterium diphtheriae A-B toxin Streptococcus pyogenes Membrane-disrupting erythrogenic toxin Clostridium botulinum A-B toxin; neurotoxin C. tetani A-B toxin; neurotoxin Vibrio cholerae A-B toxin; enterotoxin Staphylococcus aureus Superantigen Pathogenicity of Viruses • Gain entry via attachment sites for cell receptors • Resulting damage termed cytopathic effects – Production of virus particles (inclusion bodies) – Inhibition of biosynthesis (DNA, RNA, protein synthesis) – Host cell lysis Inclusion body in brain tissue of rabies victim Cytopathic effects • • • • • • Cause lysosomes to release enzymes Cause cells to fuse into syncytium Changes in host cell function Production of interferon Chromosomal damage Loss of contact inhibition Syncytium (giant cell) caused by measles virus Pathogenic Properties of Fungi • • • • May cause disease, but usually lack toxins Fungal waste products may cause symptoms Chronic infections provoke an allergic response Proteases – Candida • Capsule prevents phagocytosis – Cryptococcus (meningitis) Exceptions - Fungal toxins • Ergot toxin - hallucinations – Claviceps purpurea • Aflatoxin (peanut butter) – Aspergillus • Mycotoxins (mushrooms) – Neurotoxins: Phalloidin, amanitin – Amanita phalloides Pathogenic Properties of Protozoa • Presence of protozoa • Protozoan waste products may cause symptoms • Avoid host defenses by – Growing in phagocytes – Antigenic variation Plasmodium • What disease? • reproduction in host cells Giardia • Giardia lamblia (diarrhea) – digest cells and tissue fluids Trypanosomes • African trypanosomiasis – sleeping sickness • Chagas disease (US) • reproduction inside host Helminths • Use host tissue and resources • Interfere with host function • Waste can cause symptoms Algae • A few species produce toxins • Paralytic shellfish poisoning – “red tide” – Dinoflagellates – Saxitoxin Portals of Exit • Why do we care how the pathogen gets out? Portals of Exit • Important in spread of disease (epidemiology) • Respiratory tract – Coughing and sneezing • Gastrointestinal tract – Feces and saliva; “oral-fecal” • Genitourinary tract – STDs, urine • Skin – Wound infections; drainage • Blood vectors important – Biting arthropods and needles or syringes Mechanisms of Pathogenicity Figure 15.9