* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Dentistry
Forensic dentistry wikipedia , lookup
Water fluoridation wikipedia , lookup
Dental implant wikipedia , lookup
Water fluoridation in the United States wikipedia , lookup
Oral cancer wikipedia , lookup
Fluoride therapy wikipedia , lookup
Calculus (dental) wikipedia , lookup
Scaling and root planing wikipedia , lookup
Endodontic therapy wikipedia , lookup
Impacted wisdom teeth wikipedia , lookup
Dentistry throughout the world wikipedia , lookup
Crown (dentistry) wikipedia , lookup
Tooth whitening wikipedia , lookup
Dental hygienist wikipedia , lookup
Focal infection theory wikipedia , lookup
Tooth decay wikipedia , lookup
Dental degree wikipedia , lookup
Dental avulsion wikipedia , lookup
Special needs dentistry wikipedia , lookup
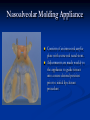
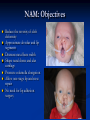
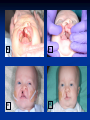
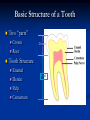
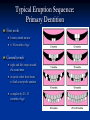
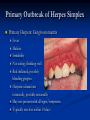
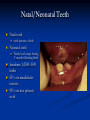
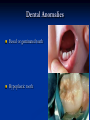
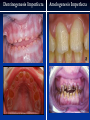
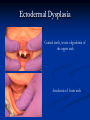
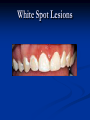
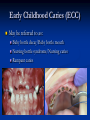
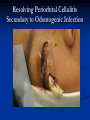
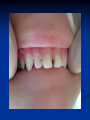
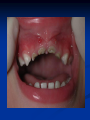
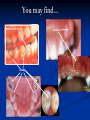
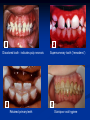
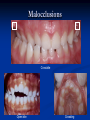
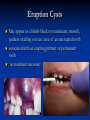
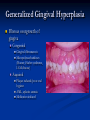
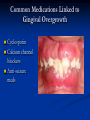
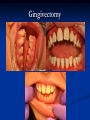
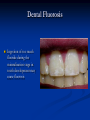
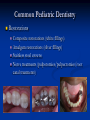
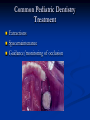
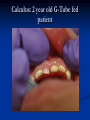
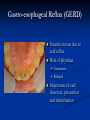
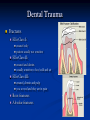
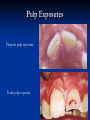
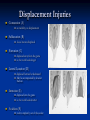
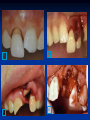
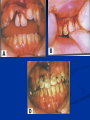
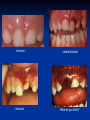
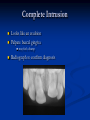
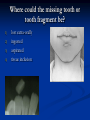
Pediatric Dentistry Seminar Dr. Christine Bell, DMD, Cert.Ped.Dent, FRCD(C) Pediatric Medical Residents Seminar Series January 2013 Objectives Provide a basic overview of pediatric dentistry Answer frequently asked questions raised by Family Medicine and Peds Medicine Residents Overview Normal Dental Development Abnormal Dental Development Early Childhood Caries Common Pediatric Dentistry Recommendations for Parents When to Refer and For What Special Needs Patients Trauma Education: General Dentist and Specialist Undergraduate Training 3-4 years Dental School 4 years General Dentist Specialty Training 2-4 years depending on the specialty and the program Dental Specialists Endodontist Oral and Maxillofacial Surgeon Orthodontist Pedodontist/Pediatric Dentist Periodontist Prosthodontist When should the first dental check up be? Age One The American & Canadian Academy of Pediatric Dentistry recommend a dental home be established as early as 6 months of age or 6 months after the eruption of the first tooth and definitely by 1 year of age First Dental Visit Comprehensive oral examination acute care, preventive services assess for oral diseases and conditions asses the need for fluoride Anticipatory guidance teething, digit/pacifier habits, trauma, prevention Oral hygiene instructions Dietary counseling Prolonged breast/bottle feeding, sippy cup, juice Caries- risk assessment determine individualized dental health plan Who can children see for dental exams/treatment? Family/General Dentist Pediatric Dentist Typically treats children from birth to age 18 Some offices stop seeing patients at an earlier age Hospital Pediatric Dentist Alberta Children’s Hospital Alberta Children’s Hospital Pediatric Dental Clinic Patients are seen by referral only Referrals Physicians/Medical Specialists Community physicians/pediatricians In-and Out-patient clinics/physicians Oncology, cardiology, nephrology, hematology, GI Perinatology, endocrinology, genetics, infectious disease Developmental Clinic, Neuromotor Clinic Cleft Palate & Craniofacial Clinic, ENT, Plastics Emergency Department Community general and pediatric dentists ACH Dental Clinic Patients Medically compromised and special needs patients from birth up to 18 years Children with craniofacial/structural anomalies Syndromes, autism Immune compromised Bleeding disorders Oncology, transplant patients Cardiac/vascular diseases Uncontrolled seizure disorders, etc… Genetic disorders, cleft lip and palate, craniofacial anomalies velopharyngeal incompetency, sleep apnea Healthy patients under the age of 4 years with significant dental issues Significant Dental Issues Urgent, extensive or special oral needs Early childhood caries Dental/periodontal abscesses, facial cellulitis Oral/dental trauma Oral surgery needs(surgical extraction, frenectomy, gingivectomy, soft tissue biopsy) Unusual/rare dental conditions (amelogenesis imperfecta, dentinogenisis imperfecta, ectodermal dysplasia, cleidocranial dysostosis etc) Cleft Lip and Palate Infants Cleft lip and palate infants are referred to the ACH Dental Clinic for consult by a Pediatric Dentist certified in Nasoalveolar Molding (NAM) Therapy Nasoalveolar Molding Appliance Consists of an intra-oral acrylic plate with extra-oral nasal stent. Adjustments are made weekly to the appliance to guide tissues into a more desired position prior to initial lip closure procedure NAM: Objectives Reduce the severity of cleft deformity Approximate alveolar and lip segments Decrease nasal base width Shape nasal dome and alar cartilage Promote columella elongation Allow one-stage lip and nose repair No need for lip adhesion surgery a c b d Behavior Management Options ACH Dental Clinic Non-pharmacologic techniques tell-show-do positive reinforcement voice control distraction medical stabilization Nitrous oxide inhalation sedation Oral conscious sedation Combination of oral and inhalation sedation General anesthesia Dental Development 2013 Pediatric Resident Seminar Series - Dr. Christine Bell Basic Structure of a Tooth Two “parts” Crown Root Crown Tooth Structure Enamel Dentin Pulp Cementum Root Dental Development Two sets of teeth: Primary Dentition ‘baby’ or ‘milk’ teeth 20 teeth Secondary Dentition ‘adult’ or ‘permanent’ teeth 32 teeth How are teeth numbered? Different tooth numbering systems Universal International (FDI) Palmer Typically in Canada we use the International Tooth Numbering System International Tooth Numbering System Two digit numbering system First number is the quadrant number Second number is the position/number of teeth from the midline Permanent Teeth Quadrant I Quadrant IV Quadrant II Quadrant III Primary Teeth Quadrant 5 Quadrant 6 Right Left Quadrant 8 Quadrant 7 Typical Eruption Sequence: Primary Dentition First tooth lower central incisor 6-10 months of age General trends right and left erupt around the same time erupt in order from front to back except the canines complete by 25 -33 months of age Timing of Tooth Eruption Permanent Dentition Primary Dentition Mixed Dentition Stage 6 yrs – 14 yrs of age typically initiated with eruption of the lower first permanent molar What to do for teething? Teething Massage the gums, have baby chew on cold wash cloth, cold teething rings, give tylenol if necessary We typically do not recommend oragel or baby oragel Lidocaine or benzocaine content Studies have not confirmed strong association between tooth eruption and a range of teething symptoms. Study by King et.al. 1992 found HSV associated with almost 50% of infants with teething difficulties Herpes Simplex Virus Everyone is exposed to it 1% present with primary herpetic gingivostomatitis Typically occurs in children <4 years of age 7-18% end up with recurrent herpes labialis (cold sores) Primary Outbreak of Herpes Simplex Primary Herpetic Gingivostomatitis Fever Malaise Irritability Not eating/drinking well Red inflamed, possibly bleeding gingiva Herpetic ulcerations intraorally, possibly extraorally May not present with all signs/symptoms Typically resolves within 14 days Treatment of Primary Herpetic Gingivostomatitis Encourage fluids Treat fever (Tylenol) Encourage good hand hygiene Educate family: viral, can spread/inoculate other sites (eyes, herpetic whitlow), contagious (others can acquire) Antiviral meds of limited value typically prescribed if outbreak is severe or patient is immune compromised (acyclovir) Dental Development Prior to Eruption Dental Development Initiation of all primary teeth occurs while IU Initiation of most permanent teeth occurs IU (with exception of the premolars, 2nd and 3rd molars) Dental Development All primary teeth begin to calcify at 4 months IU 1st permanent tooth to undergo calcification is the 1st permanent molar (birth) All permanent teeth with the exception of the wisdom teeth are calcified by 6-7 years of age Dental Development Complication or interruption of any of the processes of development (initiation, histodifferentiation, calcification or maturation) could result in dental issues Abnormal Dental Development 2013 ACH Pediatric Resident Seminar Series - Dr. Christine Bell Dental Anomalies Natal/Neonatal teeth Extra/supernumerary teeth Missing teeth Malformed teeth Anodontia/oligodontia Microdont/macrodont/conical/twinning/genination Structural/mineralization anomalies Hypocalcification/hypoplasia/fluorisis/amelogenesis imprefecta/dentinogenesis imperfecta Natal/Neonatal Teeth Natal teeth Neonatal teeth teeth present at birth Teeth/tooth erupt during 1st month following birth Incidence 1:2500-3500 births 85% are mandibular incisors 90% are true primary teeth Treatment Monitor vs extraction Indications for extraction hyper-mobility difficulties with breast feeding traumatic ulcerations on tongue (Riga Fede Disease) Dental Anomalies Fused or geminated teeth Hypoplastic tooth Some dental development issues may be linked to genetics &/or medical conditions Dentinogenesis imperfecta Oligodontia, conical teeth Osteogenesis imperfecta Ectodermal dysplasia Multiple supernumerary teeth Cleidocranial dysostosis Dentinogenesis Imperfecta Amelogenesis Imperfecta Ectodermal Dysplasia Conical teeth, severe oligodontia of the upper arch Anodontia of lower arch 4 year old male with Ectodermal Dysplasia and severe oligodontia Dental Caries (Cavities) 2013 ACH Pediatric Resident Seminar Series - Dr. Christine Bell Dental Caries/Cavities The Centre for Disease Control & Prevention reports Dental Caries as being the ‘most prevalent infectious disease in our Nation’s children’ 5x more common than asthma Estimated that >40 % of children have caries by kindergarten Preventable disease Etiology of Dental Caries Multifactorial TIME Bacteria C A R I E S Tooth Fermentable Carbohydrate The Caries Process Streptococcus mutans Main bacteria responsible for causing tooth decay Part of natural oral flora Can be acquired Acquisition of Cariogenic Bacteria Vertical Transmission Passing of bacteria from caregiver to child Studies have shown the strain of S.mutans in the mouths of children are the same strain as that found in the mouths of their caregivers Horizontal transmission Passing of bacteria from someone other than a caregiver Studies have found that in the environment of daycares, the same strains of S.mutans are found among the children Strategies to minimize transmission from primary caregivers improve caregivers oral hygiene and dental health do not share utensils or tooth brushes do not clean soother with your mouth Pre-chewing food is not recommended this is a practice in some cultures Demineralization First stage of tooth decay white spot lesion Chalky white area usually following curvature of the gum line demineralized enamel As the demineralization progresses, the surface layer becomes weaker and eventually collapses resulting in a cavity White Spot Lesions The Caries Process Dental decay is associated with frequency and duration of exposure to cariogenic substances more frequent and longer duration of sugar in the mouth produces a lower pH and longer exposure to the change in pH (favoring demineralization) Stephan Curve 7 pH Re-mineralization 6 5.5 5 Critical pH Demineralization 0 10 20 30 40 Minutes - The average baseline oral pH is ~7 - pH of 5.5 is considered the critical pH - The Stephan Curve shows changes in oral pH following exposure to a sucrose solution - pH drops significantly below the critical pH on initial exposure - takes ~20 minutes to recover to the critical pH and ~40 minutes to return to baseline Early Childhood Caries (ECC) May be referred to as: Baby bottle decay/Baby bottle mouth Nursing bottle syndrome/Nursing caries Rampant caries What is the impact of ECC on a Child’s quality of life? Pre-school children do not necessarily complain of tooth pain they manifest the effects of pain by changing eating and sleeping patterns Reported effects of untreated caries include: Low percentile weights or failure to thrive Risk of delayed physical growth and development Loss of school days Diminished ability to learn: irritability, inability to concentrate Pain Risk of dental abscess, facial cellulitis and potentially life threatening infections (Ludwig’s angina, cavernous sinus thrombosis) Hospitalizations and emergency room visits Resolving Periorbital Cellulitis Secondary to Odontogenic Infection We need to work together to help decrease the prevalence of this preventable disease Physician’s Role in Caries Prevention Early identification and referral of high risk children Discuss caries prevention information with families Caries Risk Assessment A systematic evaluation looks at the presence and intensity of etiologic disease factors It is designed to provide an estimation of disease susceptibility aids in formulating preventative and treatment strategies Caries Risk Screening Tool Caries-risk Assessment tool (CAT): Check list Gather information from a primary caregiver Conduct clinical evaluation of child’s mouth Can be used by dental and non-dental health care providers American Academy of Pediatric Dentistry website: www.aapd.org Provides a current caries risk assessment form Risk Factors for Caries Development Primary caregiver or sibling with active caries Low socioeconomic status Child has >3 between meal sugar containing snacks/beverages per day Child is put to bed with bottle/cup containing something other than water Not receiving optimally fluoridated drinking water or fluoride supplements White spot lesions on teeth Visible cavities or fillings Visible plaque on teeth (poor oral hygiene) special health care needs Recent immigrant Other Risk Factors for Caries Development Breast or bottle feeding beyond 12 months of age feeding throughout the night or allowing baby to fall asleep for the night while feeding Oral medications (suspensions, inhalers) Nutritional supplements such as Pediasure or Nutren Junior etc. Physician’s Role with Dental Caries Prevention Ask families if they have a dentist for their child Review feeding habits are they seeing a dentist regularly recommend first dental visit by age one Prolonged breast/bottle/sippy cup use and feeding throughout the night juice, grazing habits, hidden sugars Discuss oral hygiene practices Brush 2x day by parent Start using fluoride toothpaste at age 3 (1/2 pea sized amount) <3 years of age; fluoride use is prescribed on an individual basis by the dentist Do not share tooth brushes Lift the Lip Look for… Dental caries at any stage of progression Chipped or broken teeth Crooked/crowded teeth Discolored teeth Abscesses Poor oral hygiene Red inflamed gums Anomalies You may find… White spot lesion decay abscess 1 2 Discolored tooth - indicates pulp necrosis 3 Supernumerary tooth (“mesodens”) 4 Retained primary teeth Stain/poor oral hygiene Malocclusions R L Crossbite Open bite Crowding Eruption Cysts May appear as a bluish-black or translucent, smooth, painless swelling over an area of an unerupted tooth associated with an erupting primary or permanent tooth no treatment necessary Generalized Gingival Hyperplasia Fibrous overgrowth of gingiva Congenital Gingival fibromatosis Mucopolysaccharidoses (Hunter, Hurler syndrome, I-Cell disease) Acquired Plaque induced/poor oral hygiene AML, aplastic anemia Medication induced Common Medications Linked to Gingival Overgrowth Cyclosporin Calcium channel blockers Anti-seizure meds Gingivectomy When to refer Recommend they see a dentist if they do not have one and: No sign of decay No significant findings Low risk for caries Refer to a dentist Obvious decay or dental trauma Significant findings High risk for caries Oral Hygiene 2013 ACH Pediatric Resident Seminar Series - Dr. Christine Bell Oral Hygiene Recommendations Parents should brush their children’s teeth until they are about 8 yrs old Always use a soft bristled toothbrush Floss teeth that are contacting one another Rule of 2’s Brush 2x a day, for 2 minutes and visit the a dentist 2x a year for regular check-ups Oral Hygiene Recommendations Prior to eruption of first tooth Eruption of first tooth wipe gums with wet washcloth at least 1x day Wipe tooth and gums with a wet washcloth 2x day or after every feed Be aware that feeding during the night or at bedtime can cause tooth decay Eruption of molars Use toothbrush with water or ‘safe to swallow’ toothpaste 2x daily Recommendations: Fluoride Use Under 3 years of age non-fluoridated toothpaste is recommended fluoride recommendations based on caries risk assessment dentist develops an individualized caries prevention plan and recommendations for fluoride use Recommendations: Oral Hygiene and Fluoride Use Age 3-6 Brushing 2x day using fluoride toothpaste (grain of rice sized to half the size of a pea amount of toothpaste) Flossing 1x day where teeth are contacting > 6 years of age Brushing 2x day using fluoride toothpaste (pea sized amount of toothpaste) Flossing 1x day Mechanism of Action of Fluoride Topical and Post-eruptive Increases the remineralization process Prevents demineralization Catalyst for remineralization (Ca, PO4) Decreases tooth solubility Decreases bacterial acid production Inhibits enolase, enzyme required in glycolysis Water Fluoridation Optimum water fluoride level 1 ppm (1.0mgF/L) recommended range = 0.7-1.2 ppm Fluoride Supplement Schedule Fluoride concentration in community drinking H2O Age < 0.3 ppm 0.3-0.6 ppm > 0.6 ppm none none 0-6 months none 6mo-3yr 0.25mg/day none 3-6yr 0.50mg/day 0.25mg/day none 6-16yr 1.0mg/ day 0.50mg/day none none Fluoride Supplements Very rarely do we Rx systemic fluoride supplements Consider all sources of fluoride Young children with incipient decay (white spot lesions) may benefit from application of fluoride varnish Dental Fluorosis Ingestion of too much fluoride during the mineralization stage in tooth development may cause fluorosis Common Pediatric Dentistry 2013 ACH Pediatric Residency Seminar Series - Dr. Christine Bell Common Pediatric Dentistry Prevention Routine dental exams, cleanings, fluoride application Sealants (recommended on molars with deep grooves) Common Pediatric Dentistry Restorations Composite restorations (white fillings) Amalgam restorations (silver fillings) Stainless steel crowns Nerve treatments (pulpotomies/pulpectomies/root canal treatments) Common Pediatric Dentistry Treatment Extractions Spacemaintenance Guidance/monitoring of occlusion Why fix a baby tooth? They just fall out, don’t they? Primary teeth are important: Chewing Speaking Esthetics Hold space for the adult teeth Gives face shape and form If not restored, decay will continue to worsen and eventually lead to pain, discomfort and infection Special Needs and Medically Compromised Children Special Needs and Medically Compromised Children Unique medical and dental needs May not be the most cooperative dental patients Best seen by a Pediatric Dentist Private practice Pediatric Dentist Hospital based Pediatric Dentist Children with Special Health Care Needs Typically have one or more risk factors predisposing them to dental disease Delayed first dental visit Complex medical needs Parents overwhelmed with medical issues Limited cooperation for home oral hygiene Mental and/or physical disability complicates oral hygiene process Perioral sensitivity Behavior issues Possible Risk Factors of Children with Special Health Care Needs Dietary Need for frequent high calorie feedings, night feedings Tube feeding Behavior reinforcing therapy with sweet treats Greater exposure to medications Xerostomia is common side effect of many medications Suspensions contain sugar Oral steroids/inhalers linked to tooth decay Possible Risk Factors of Children with Special Health Care Needs Oral motor dysfunction/parafunction Chewing, swallowing problems Grinding/clenching Self biting (lip, cheek) Chewing objects Pouching of food Gastro-esophageal reflux, frequent vomiting Greater susceptibility Periodontal disease (Down Syndrome) Trauma (CP, seizure disorder) Neglect and abuse Tube Fed Children Oral aversions Aspiration risk Parents afraid to brush teeth as worried about secretions No oral feeds Uncooperative for tooth brushing Parents incorrectly think they are not eating so no need to brush teeth May take tastes, usually sweet foods/drinks Common Oral Findings with Tube Fed Children Significant calculus build-up Gingivitis Periodontal disease Possible GERD Acid erosion of teeth Calculus: 2 year old G-Tube fed patient Gastro-esophageal Reflux (GERD) Enamel erosion due to acid reflux Role of physician Awareness Referral Importance of early detection, prevention and rehabilitation Cardiac Patients Some are at risk of Bacterial Endocarditis Prophylactic antibiotic coverage may be indicated prior to dental treatment Prior to open heart surgery patients require dental clearance letter Cardiac surgery may be cancelled if unable to complete dental work before scheduled surgery Transplant Patients Will be immune suppressed Should have all dental treatment completed prior to transplant bone marrow or organ transplant may be postponed if oral health is not satisfactory Immune Compromised Patients and Oncology Patients Issues with low counts (CBC) Issues with low platelets Unable to deal with infection Septicemia/Bacteremia Delayed healing Other serious complications Prior to Dental Work Consult specialist team Proper timing for safe dental treatment Blood work, medications/antibiotics, transfusion etc may be necessary pre and post dental treatment Dental work, dental cleanings etc may need to be postponed until health of patient is more ideal Absolute Neutrophil Count (ANC) and Dental Treatment ANC >1000/mm3 ANC of 500-1000/mm3 No antibiotic prophylaxis necessary unless infection present Antibiotics indicated, may defer treatment ANC <500/mm3 Defer elective dental treatment Platelet Count and Dental Treatment >75, 000 40, 000-75,000 no additional support except aggressive local measures consider platelet transfusion prior to and 24 hrs post dental treatment <40, 000 defer care Considerations: Bleeding Disorders May need factors, transfusions etc Early detection and early treatment allows for minor procedures and less bleeding issues/complications Antibiotics in Dentistry 2013 ACH Pediatric Resident Seminar Series - Dr. Christine Bell Antibiotic Prophylaxis May be indicated for some patients: Cardiac conditions at risk for sub-acute bacterial endocarditis Immune compromised patients Patients with VA (ventricular-arterial) shunts, indwelling vascular catheters (central line, chemoport) Some orthopedic patients (VEPTR, joint replacements) Antibiotic Coverage Cardiac and Immune Compromised Patients: Follow American Heart Association Guidelines – reviewed/revised 2007 Amoxicillin: 50mg/kg (max 2g) 1 hr prior to dental procedure Clindamycin: 20mg/kg (600mgs) 1 hr prior Orthopedic Patients: Follow the American Academy of Orthopedic Surgeons Guidelines 50mg/kg Keflex 1 hr prior; amoxicillin or clindamycin could be given instead Reason for coverage Dental procedures may cause a transient bacteremia Prevent seeding of bacteria in susceptible area Vulnerable areas of the heart Certain implanted hardware (VEPTR) Central lines, etc Those with compromised immune systems may be unable to handle a transient bacteremia Potential Oral Source of Bacteremia Routine tooth brushing or chewing Poor oral/dental hygiene Periodontal or dental infections Oral/dental procedures associated with bleeding Immune Compromised Includes but not limited to: Chemotherapy, radiation, bone marrow transplant HIV, diabetes Neutropenia Chronic steroid use Hemodialysis Status post splenectomy Organ transplant Consultation with medical specialist indicated Standard AHA prophylactic regimen recommended Hemodialysis: Coverage is two fold Immune suppressed At risk of infective endocarditis even in the absence of a structural cardiac defect Altered host defence Altered cardiac output and mechanical stresses Bacterial seeding and growth on shunts Peritoneal Dialysis Lower risk for infection of catheter from transient bacteremia Have altered host defences Antibiotic prophylaxis may be recommended; consultation is indicated Considerations when Prescribing Prophylactic Antibiotics Patients already receiving antibiotics select drug of different class, or delay procedure 10-14 days after completion of the antibiotic Need for multiple visits wait 10-14 days between appointments Unanticipated bleeding effective prophylaxis up to 2 hrs post-op Antibiotics and Dental Infections Dental abscess Antibiotics typically if systemically involved Pen VK, Amoxicillin, Clindamycin Facial cellulitis Mild-Moderate: PO antibiotics (eg. Clindamycin) Moderate-severe: IV antibiotics (eg. Clindamycin or Flagyl/ancef) Dental Infections Dental treatment necessary primary tooth: extraction permanent tooth: extraction vs root canal treatment Dental infections will return if tooth is not treated appropriately Seek the most up-to-date information for antibiotic recommendations It is possible that these current recommendations may change as the result of more advanced research and of the ongoing clinical guidelines development of professional associations and academies Therefore, clinicians are encouraged to consider the recommendations in the context of their specific clinical situation and consult, where appropriate, other sources of clinical, scientific, or regulatory information prior to making a treatment decision and seek most-up-to-date information Dental Trauma 2013 ACH Pediatric Resident Seminar Series - Dr. Christine Bell Dental Trauma Fractures Ellis Class I: Ellis Class II: enamel and dentin usually sensitive to hot/cold and air Ellis Class III: enamel only patient usually not sensitive enamel, dentin and pulp you see red and they are in pain Root fractures Alveolar fractures Pulp Exposures Pinpoint pulp exposure Frank pulp exposure Displacement Injuries Concussion (A) Subluxation (B) displaced forward or backward May be accompanied by alveolar fracture Intrusion (E) displaced away from the gums ie. the tooth looks longer Lateral Luxation (D) loose but not displaced Extrusion (C) no mobility, no displacement displaced into the gums ie. the tooth looks shorter Avulsion (F) tooth completely out of the socket 1 3 2 4 Dental trauma that shouldn’t wait till tomorrow for treatment Patient cannot close teeth all the way together Fractures involving pulp Mobility greater than 3mm Intruded teeth Extruded teeth Avulsions This is a true dental emergency survival is dependant on time out of the mouth immediately place tooth in milk ideally, place tooth back in the socket (permanent teeth) DO NOT replant primary teeth Intrusion Intrusion Lateral luxation What do you think? Complete Intrusion Looks like an avulsion Palpate buccal gingiva may feel a bump Radiograph to confirm diagnosis Where could the missing tooth or tooth fragment be? 1) 2) 3) 4) lost extra-orally ingested aspirated tissue inclusion Alberta Children’s Hospital Dental trauma Pediatric Dentist is on call 24/7 at ACH Facial cellulitis/odontogenic infections Emergency department physicians may Rx antibiotics (IV/ PO). Patients are instructed to follow up with their dentist, or referred to a dentist (possibly the one on call) Questions? Thank you ! 2013 ACH Pediatric Resident Seminar Series - Dr. Christine Bell