* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Resolution of Mid-Peripheral Intraretinal Fluid in X
Mitochondrial optic neuropathies wikipedia , lookup
Visual impairment wikipedia , lookup
Photoreceptor cell wikipedia , lookup
Vision therapy wikipedia , lookup
Blast-related ocular trauma wikipedia , lookup
Eyeglass prescription wikipedia , lookup
Fundus photography wikipedia , lookup
Dry eye syndrome wikipedia , lookup
Visual impairment due to intracranial pressure wikipedia , lookup
Retinal waves wikipedia , lookup
Diabetic retinopathy wikipedia , lookup
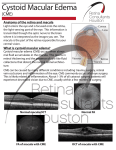
Resolution of Mid-Peripheral Intraretinal Fluid in X-Linked Retinoschisis with Use of Dorzolamide 2% Frederick T. Collison1, Gerald A. Fishman1,2 1 The Pangere Center for Hereditary Retinal Diseases, The Chicago Lighthouse for People who are Blind or Visually Impaired, Chicago, IL, USA. 2 Department of Ophthalmology and Visual Sciences, University of Illinois at Chicago, Chicago, IL, USA. INTRODUCTION X-linked retinoschisis (XLRS) is an early-onset hereditary retinal dystrophy caused by mutation(s) of the retinoschisin (RS1) gene1 In the first few decades of life, the layers of the macula are split and central visual acuity is decreased. In the fourth or fifth decades, the macular schisis may be replaced by an atrophic-appearing lesion accompanied by further visual acuity loss. Clinically detectable peripheral retinoschisis, most commonly observed bilaterally in the inferior-temporal retina, is often found in XLRS. RIGHT EYE a. Baseline right eye macula LEFT EYE a. Baseline left eye macula Topical carbonic anhydrase inhibitors have been found to reduce the intraretinal fluid in the majority of XLRS patients with macular cysts.2 In the current case report, we present a patient diagnosed with XLRS with intraretinal cysts in both the macula and the mid-peripheral retina, which resolved not only in the macula, but also in the mid-peripheral retina, with the use of topical dorzolamide 2% ophthalmic suspension. b. Follow-up right eye macula CASE REPORT Figure 1. Vertical SD-OCT line scans of the macula OD at baseline, prior to treatment (a) and after three months on topical ocular dorzolamide 2% tid OU (b). Intraretinal cysts/splitting are markedly reduced at follow-up in the fovea and macula out to the vascular arcades. b. Follow-up left eye macula Figure 2. Vertical SD-OCT line scans of the macula OS at baseline, prior to treatment (a) and after three months on topical ocular dorzolamide 2% tid OU (b). Intraretinal cysts/splitting are markedly reduced at follow-up in the fovea and macula out to the vascular arcades. Initial Visit A 34-year-old Caucasian male was referred to our clinic with a chief complaint of long-standing difficulty with distance and near central vision. Best-corrected visual acuity: 20/40-2 OD, OS. Color vision (Ishihara) and confrontation visual fields were normal. On dilated fundus exam, cystic-appearing lesions in a honeycomb pattern and some central hypopigmentation were seen in the macula of each eye. Electroretinogram OD showed selective b-wave reduction to a white single-flash stimulus, under both dark-adapted and lightadapted conditions SD-OCT (Heidelberg Spectralis HRA+OCT, Heidelberg, Germany) showed splitting of retinal layers in both eyes (Figures 1a and 2a), with a large cyst centrally in the right eye. Mid-peripheral SD-OCT line scan of the superior retina demonstrated intraretinal cysts in both eyes (Figures 3a and 4a). The patient was diagnosed with XLRS and prescribed topical dorzolamide 2% eye drops in both eyes three times a day as a treatment for the cysts in the macula. 3 Month Follow-up Visit The patient was uncertain of any definite visual change. Best-corrected visual acuity: 20/40+2 OD, OS. Dilated fundus exam still showed slight mottling in the macula, but no cysts. SD-OCT showed a marked reduction in the intraretinal macular cysts (Figures 1b and 2b) and superior retinal mid-periphery (Figures 3b and 4b) of each eye. DISCUSSION To our knowledge this is the first report of a reduction of intraretinal cysts outside the macula in XLRS with a pharmacologic treatment. This likely occurs in other patients with XLRS who have been treated with carbonic anhydrase inhibitors, but it remains unappreciated if the midperipheral region is not scanned with SDOCT. Treatment with topical dorzolamide can both reduce macular cysts and improve visual acuity in patients with XLRS.2 Some patients with XLRS have reduced sensitivity in the mid-periphery even in the absence of ophthalmoscopically detectable peripheral retinoschisis.3 It remains to be demonstrated whether the reduction of retinal cysts observed in the mid-peripheral retina results in a corresponding improvement in retinal function. • Carbonic anhydrase inhibitors may have a complementary role to gene therapy in XLRS and other retinal degenerations. REFERENCES a. Baseline right eye mid-periphery b. Follow-up right eye mid-periphery Figure 3. Vertical SD-OCT line scans of the superior mid-peripheral retina (about 10° to 40° from foveal center) OD at baseline (a), and after three months on topical dorzolamide (b). At baseline (a), note splitting of the retina in the outer nuclear layer (open arrow), inner nuclear layer (red line), and retinal nerve fiber layer (closed arrow). At follow-up, the splitting is markedly reduced in both the outer nuclear layer and the inner nuclear layer. The retinal thickness at the location on the marked by the red bar in the SD-OCT images is 233 microns at baseline (a) and 207 microns at follow-up (b). a. Baseline left eye mid-periphery b. Follow-up left eye mid-periphery Figure 4. Vertical SD-OCT line scans of the superior mid-peripheral retina OS at baseline (a), and after three months on topical dorzolamide (b). At baseline (a), note splitting of retinal layers primarily in the inner nuclear layer. Braces mark the same retinal location at both visits based on vessel location, demonstrating resolution of inner nuclear layer splitting. Retinal thicknesses at the center of the braces measure 232 microns at baseline (a) and 217 microns at follow-up (b). 1. Molday RS, et. al. X-linked juvenile retinoschisis: Clinical diagnosis, genetic analysis, and molecular mechanisms. Prog Retin Eye Res. 2012 May;31(3):195-212. Epub 2012 Jan 3. 2. Genead MA, et. al. Efficacy of Sustained Topical Dorzolamide Therapy for Cystic Macular Lesions in Patients With X-Linked Retinoschisis. Arch Ophthalmol. 2010;128(2):190-197 3. Peachey NS, et. al. Psychophysical and Electroretinographic Findings in X-linked Juvenile Retinoschisis. Arch Ophthalmol. 1987 Apr;105(4):513-516 SUPPORT Pangere Corporation; Grousbeck Foundation; Wynn-Gund Foundation;