* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Using Cone Beam CT in Clinical Practice
Proton therapy wikipedia , lookup
Radiation therapy wikipedia , lookup
Radiation burn wikipedia , lookup
Positron emission tomography wikipedia , lookup
Neutron capture therapy of cancer wikipedia , lookup
Industrial radiography wikipedia , lookup
Backscatter X-ray wikipedia , lookup
Center for Radiological Research wikipedia , lookup
Radiosurgery wikipedia , lookup
Nuclear medicine wikipedia , lookup
Medical imaging wikipedia , lookup
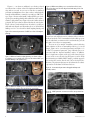
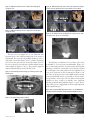
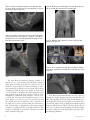
Earn 2 CE credits This course was written for dentists, dental hygienists, and assistants. Using Cone Beam CT in Clinical Practice A Peer-Reviewed Publication Written by Jeffery B. Price, DDS, MS Abstract As the 20th century ended and the 21st century began, research groups were developing an imaging technology that would forever change dentists’ ability to image their patients. This technology is known as cone beam computed tomography (CBCT).1-6 In this course we will explore the technology and principles of CBCT and we will compare the similarities and differences between multi-detector CT (MDCT) used in medical imaging and CBCT. We will also discuss some of the basics of radiation dosimetry, as well as a few tools dentists can use to educate their patients in the relative risks of CBCT. We will also look at how CBCT can assist the practitioner with advanced treatment planning. Finally, we will review some of the ethical and medicolegal issues related to the use of CBCT imaging in dentistry. Educational Objectives: At the end of this self-instructional education activity the participant will be able to: 1. Discuss the basic technology and principles of cone beam computed tomography (CBCT) for dental use. 2. Review the commonly administered doses of ionizing radiation patients receive during CBCT examinations 3. List key selection criteria and indications for the uses of CBCT in dental practice 4. Describe how CBCT examinations can enhance advanced treatment planning 5. Identify two medico-legal and ethical issues regarding the use of dental CBCT Author Profile Jeffery B. Price, DDS, MS is a Diplomate of the American Board of Oral & Maxillofacial Radiology. He is currently an Assistant Professor of Oral & Maxillofacial Radiology and Director of Oral & Maxillofacial Radiology at the Meharry Medical College School of Dentistry in Nashville, TN; in addition, he is an Adjunct Associate Professor of Oral & Maxillofacial Radiology at the UNC School of Dentistry in Chapel Hill, NC. Dr. Price practiced general and adult restorative dentistry in Hendersonville, NC for 24 years. While in practice, Dr. Price completed the continuum at the L.D. Pankey Institute in Key Biscayne, FL; in addition, he attained his Mastership in the Academy of General Dentistry as well as Diplomate status in the International Congress of Oral Implantologists. Dr. Price is currently on the editorial board of the ICOI-sponsored journal, Implant Dentistry; and, is a reviewer for IJOMS, JDE and JADA. He can be reached at [email protected] Author Disclosure Jeffrey B Price, DDS, MS discloses that he is a consultant to Sirona Dental, the commercial supporter of this educational activity. Dr. Price further discloses that he is a faculty member for Sirona Galileos new users training and operates an internet consultation service for Cone Beam CT interpretation. Go Green, Go Online to take your course Publication date: Apr. 2013 Expiration date: Mar. 2016 Supplement to PennWell Publications PennWell designates this activity for 2 Continuing Educational Credits Dental Board of California: Provider 4527, course registration number CA#: 02-4527-13018 “This course meets the Dental Board of California’s requirements for 2 units of continuing education.” The PennWell Corporation is designated as an Approved PACE Program Provider by the Academy of General Dentistry. The formal continuing dental education programs of this program provider are accepted by the AGD for Fellowship, Mastership and membership maintenance credit. Approval does not imply acceptance by a state or provincial board of dentistry or AGD endorsement. The current term of approval extends from (11/1/2011) to (10/31/2015) Provider ID# 320452. This course has been made possible through an unrestricted educational grant by Sirona Dental Systems. This course was written for dentists, dental hygienists and assistants, from novice to skilled. Educational Methods: This course is a self-instructional journal and web activity. Provider Disclosure: PennWell does not have a leadership position or a commercial interest in any products or services discussed or shared in this educational activity nor with the commercial supporter. No manufacturer or third party has had any input into the development of course content. Requirements for Successful Completion: To obtain 2 CE credits for this educational activity you must pay the required fee, review the material, complete the course evaluation and obtain a score of at least 70%. CE Planner Disclosure: Heather Hodges, CE Coordinator does not have a leadership or commercial interest with products or services discussed in this educational activity. Heather can be reached at [email protected] Educational Disclaimer: Completing a single continuing education course does not provide enough information to result in the participant being an expert in the field related to the course topic. It is a combination of many educational courses and clinical experience that allows the participant to develop skills and expertise. Image Authenticity Statement: The images in this educational activity have not been altered. Scientific Integrity Statement: Information shared in this CE course is developed from clinical research and represents the most current information available from evidence based dentistry. Known Benefits and Limitations of the Data: The information presented in this educational activity is derived from the data and information contained in reference section. The research data is extensive and provides direct benefit to the patient and improvements in oral health. Registration: The cost of this CE course is $49.00 for 2 CE credits. Cancellation/Refund Policy: Any participant who is not 100% satisfied with this course can request a full refund by contacting PennWell in writing. Educational Objectives At the end of this self-instructional education activity the participant will be able to: 1. Discuss the basic technology and principles of cone beam computed tomography (CBCT) for dental use. 2. Review the commonly administered doses of ionizing radiation patients receive during CBCT examinations 3. List key selection criteria and indications for the uses of CBCT in dental practice 4. Describe how CBCT examinations can enhance advanced treatment planning 5. Identify two medico-legal and ethical issues regarding the use of dental CBCT Image Authenticity Statement: The images in this educational activity have not been altered. Known Benefits and Limitations of the Data The information presented in this educational activity is derived from the data and information contained in reference section. The research data is extensive and provides direct benefit to the patient and improvements in oral health. Abstract As the 20th century ended and the 21st century began, research groups were developing an imaging technology that would forever change dentists’ ability to image their patients. This technology is known as cone beam computed tomography (CBCT).1-6 In this course we will explore the technology and principles of CBCT and we will compare the similarities and differences between multi-detector CT (MDCT) used in medical imaging and CBCT. We will also discuss some of the basics of radiation dosimetry, as well as a few tools dentists can use to educate their patients in the relative risks of CBCT. We will also look at how CBCT can assist the practitioner with advanced treatment planning. Finally, we will review some of the ethical and medicolegal issues related to the use of CBCT imaging in dentistry. Why CBCT? If you are a dentist who has not yet experienced CBCT imaging, you may be asking, “What is all this excitement about? Can CBCT really be that big of a deal?” Well, the excitement is warranted because for the very first time in the history of dental radiography, we are able to generate three dimensional images of our three dimensional patients using x-ray machines in our own offices at radiation doses lower than a traditional D-speed FMX!!! No matter your perspective in dentistry, that is more than a big deal; that is an ENORMOUS DEAL and for many dentists, it is a practice and life altering experience!!! Let’s spend a little time together and learn how this technology makes it possible for dentists to improve treatment outcomes on a more predictable basis. First of all, what are some of the limitations of 2D imaging? The two most commonly used forms of 2D, or plain radiography used in dentistry are intraoral and panoramic imaging. Table 1 compares Table 1. Differences between 2D Radiography and CBCT Attribute 2D Imaging CBCT Depth of field ——— +++ Image magnification ——— +++ Connectivity w/ optical — +++ scans Easily available +++ + (increasing) Radiation dose — —— Key: +++ = excellent; ++ = very good; + = good; 0 = no effect; - = negative attribute; -- = poor; --- = very poor some of the advantages and disadvantages of 2D and 3D imaging. The most important missing piece of information in periapicals and panoramics or ‘2D problem’ if you will, is that the dentist does not know the depth of field of the image. To put it another way, the clinician does not know the width of the alveolar ridge in periapical or panoramic images when treatment planning for dental implant purposes; or, the mediolateral location of the mandibular canal when evaluating the location of the apices of mandibular third molars. Panoramic technology has innate imaging characteristics such as parallax and non-uniform magnification.7-9 These endemic problems result in images that are acceptable for the initial evaluation of our patients, but are inadequate for precise, detailed and reliable implant planning or impacted tooth localization.10 Over the years we have used localization techniques such as the buccal object rule or the ‘same lingual opposite buccal’ (SLOB) technique to localize root positions;9, 11-15 and we have worked around the limitations of using panoramic images by using arbitrary magnification ratios to compensate for the 10 to 25% inherent variable magnification seen in panoramic radiographs. When the task demands precise localization, CBCT provides for non-distorted, non-magnified reliable images for accurate diagnosis. What is Cone Beam Computed Tomography? Dental cone beam CT is a type of computed tomography that uses a cone shaped x-ray beam for image exposure instead of the standard fan shaped x-ray beam used in MDCT.9, 16-18 Figure 1 shows a typical CBCT machine with a schematic of the shape of the cone shaped x-ray beam. The use of a cone shaped primary x-ray beam to expose the patient results in raw images requires slightly different processing algorithms than those used in routine MDCT imaging since the x-ray beam is collimated to a fan shape in MDCT machines. Also, in CBCT imaging, the x-ray source and receptor rotate an arc between 180° and 360° around the patient while in MDCT, the x-ray source and receptor rotate many times around the patient depending upon the region of interest. Additionally, in MDCT imaging the primary x-ray beam and the remnant x-ray beam are both collimated, while in CBCT only the primary x-ray beam is collimated. These and other technique characteristics result in distinct physical differences between MDCT and CBCT images; the most significant of which is the difference in signal to noise ratio (SNR) between the two techniques. MDCT has a SNR of approximately 90% while the SNR for CBCT is approximately 15 to 20%. The result is that 2www.ineedce.com Figure 1: CBCT machine; note the schematic that outlines the cone shaped x-ray beam Figure 2. A Multiplanar Reconstruction (MPR) view consisting of panoramic, 3D, parasagittal, coronal cross-sections and axial reconstructions typical of most CBCT viewing software packages on the market today. Figure 3. A 3D volumetric rendering of a patient with multiple small sialoliths within the left parotid gland and the left submandibular salivary gland and duct. CBCT provides excellent images of dense objects such as teeth and bone while MDCT yields excellent images of the entire range of objects seen in the human body from low density fluids to soft tissues all the way to highly dense, calcified tissues.19-22 At first glance, this lack of soft tissue detail may seem to be a disadvantage for CBCT; however, in dentistry most of our diagnostic tasks are focused on teeth and bone—planning for implants, localizing impacted maxillary canines and mandibular third molars etc.; and as mentioned, CBCT imaging is an excellent choice for imaging these high density anatomic features. In addition, CBCT provides images with soft tissue outlines from which we can determine orthodontic and airway landmarks providing assistance with 3D diagnosis and planning. In actuality, most diagnostic problems do not require the additional information of soft tissue details that MDCT can offer. CBCT viewing software generally provides us with two types of images — multiplanar reconstructed images (MPR) or 3D volumetric reconstructions. Figures 2 and 3 are examples of the types of images you can expect from typical CBCT software. Once the volumetric image is obtained, the computer processes this volume into axial, coronal and sagittal slices which the user can then scroll through, slice by slice. Many volumes are approximately 512 x 512 x 512 slices; the actual number of slices is dependent on the scanning and reconstruction resolutions. Different types of 3D volumes are obtained depending on the diagnostic task. The clinician may want to see the mandible and the maxilla for instance, or may be interested in seeing outlines of the airway in an obstructive sleep apnea patient. In addition, many software packages on the market today are capable of virtual implant planning and placement whereby the user can place virtual implants into the CBCT volume. These implant positions can then be used to order the fabrication of surgical guides to replicate the fixture positions during implant surgery and guide the implant surgeon during surgery.23-28 www.ineedce.com Radiation Dosimetry Another major difference between CBCT and MDCT imaging technologies is the radiation dose required. Effective dose is a term used to describe the relative risk of exposures to ionizing radiation and is calculated in microSieverts (μSv). Standard MDCT images of the maxillofacial region result in radiation doses that may range approximately 10 to 20 times higher than CBCT images depending on the area imaged and the technique factors utilized.29-31 Even though F-speed film is recommended for routine use,32 many dentists still use D-speed film with round collimation for their full mouth series technique; this examination results in an effective dose of ~388 μSv; or, three to five times the radiation dose of many standard maxillofacial view CBCT images.9 This relationship along with radiation doses from other common radiographic examinations can be found in Table 2. One fact that many people, medical and dental professionals included, are not aware of is that we are exposed to ionizing radiation every day in our daily lives. Sources of background radiation include cosmic radiation (gamma-rays, x-rays and beta particles) and ingested food products, such as bananas with trace amounts of radioactive potassium, etc.; but, the largest source of ionizing radiation for many of us is radon which comes from basements of buildings and other terrestrial sources such as building materials; i.e., concrete.33 Although it is far from perfect, an easy to use tool for patient education is to use the average daily background ionizing radiation exposure of 8 μSv per day as the denominator 3 Table 2. Radiation doses from common radiographic examinations Effective Doses, Probability of Excess Fatal Cancer Risk per Million Examinations and Daily Background Equivalence from Dental and Maxillofacial X-Ray Examinations Technique Dose CA Risk per Million Exams Background Equivalency (microSieverts) CA Risk per 0.8 1.7 days Million Exams Background 0.3 15 hours Equivalency 35 2 4.4 days 8 μSv/day 171 9 21 days Panoramic—indirect digital 14 0.8 1.7 days Skull/Ceph—indirect digital 5 0.3 15 hours FMX (PSP or F-Speed film—Rectangular collimation) 35 2 4.4 days FMX (PSP or F-speed film—Round collimation) 171 9 21 days FMX (D-Speed film—Round collimation) 388 21 47 days One PA or BW (PSP or F-Speed; Rectangular Collimation) 2 0.1 6 hours One PA or BW (PSP or F-Speed; Round Collimation) 9.5 0.5 1 day One PA or BW (D-Speed; Round Collimation) 22 1.2 2.7 days 4 BWs (PSP or F-Speed-Rectangular Collimation) 5 0.3 15 hours 4 BWs (PSP or F-Speed-Round Collimation) 38 2 4.6 days 4 BWs (D-Speed-Round Collimation) 88 5 10.7 days Tomogram (8 cm x 8 cm field of view) 10 0.5 1.2 days Cone Beam CT exam (NewTom 3G — 12” FOV) 68 4 8.3 days Sirona GALILEOS Comfort 15 cm x 15 cm x 15 cm 61 3.3 7.6 days Sirona ORTHOPHOS XG 3D 8 cm x 8 cm 64 3.5 8 days Sirona ORTHOPHOS XG 3D 5.5 cm x 8 cm (Maxilla) 41 2.2 5.1 days Sirona ORTHOPHOS XG 3D 5.5 cm x 8 cm (Mandible) 52 2.9 6.5 days Sirona ORTHOPHOS XG 3D 5.5 cm x 5 cm 30 1.7 3.8 days Carestream 9300 8 cm x 8 cm of the Jaws 75 4.1 9.4 days Carestream 9300 10 cm x 5 cm of the Maxilla 30 1.7 3.8 days Carestream 9300 10 cm x 5 cm of the Mandible 56 3.1 7 days Siemens Somatom 64 MDCT MaxilloMandibular Scan 2100 153 256 days MDCT Maxilla Only 1400 102 171 days Courtesy of Dr. John Ludlow when determining the equivalent number of background days of radiation in a particular radiographic examination. For instance, if a CBCT resulted in a radiation dose of 80 μSv, the equation would be 80 μSv/8 μSv per day = 10 days of background radiation equivalence, for patient education purposes. This is not a perfect system since the background radiation in this example is spread out over ten days while the CBCT radiation is delivered in 15 to 20 seconds, but 80 μSv is considered a very low dose of radiation and again, the rationale for using this system is to provide for a patient education tool, not to defend a PhD dissertation in medical physics. To summarize radiation doses with CBCT—remember, as with most radiographic techniques, there is no ‘blanket’ statement—one must compare various factors such as field of view, scanning resolution, technique factors of kVp, mA and time, etc. In general, CBCT has significantly less radiation dose than MDCT; and, CBCT has a slightly greater radiation dose compared to panoramic radiology and optimized digital radiation with rectangular collimation. Selection Criteria and When to Use CBCT A common question that many dentists have when they begin using CBCT technology is how to decide when to use the technology. It’s one thing to have this wonderful piece of equipment, but how should a conscientious dentist who wants to avoid over-irradiating his or her patients decide when to order cone beam scans? We will look at what a few professional organizations have to say on the subject and then explore a few other areas of dentistry. In June 2012, the American Academy of Oral & Maxillofacial Radiology (AAOMR) updated their recommendation on the use of radiology for dental implantology purposes. Since 2000, the AAOMR has recommended using some type of cross-sectional imaging during definitive treatment planning for dental implantology cases.34 This recommendation originally referred to conventional tomography; but, now with the advent of cone beam CT, CBCT is currently recommended as the optimal imaging choice for the definitive treatment planning of dental implants by the AAOMR.35 The main point to remember is that this statement is not a standard of care; it is only a position statement and does not take the place of a clinical examination and clinical judgment rendered by a provider. Many authors outline the differing opinions and different types of implant cases for which to consider using CBCT examinations. Perhaps the most succinct summary was offered by Benavides et al in an article published in Implant Dentistry in April, 2012: “Because the 3D information obtained with CBCT cannot be obtained with other 2D imaging modalities, it is virtually impossible to predict which treatment cases would not benefit from having this additional information before obtaining it.”36 4www.ineedce.com In 2010, the American Association of Endodontists (AAE) released a joint position statement with the AAOMR outlining the use of cone beam CT for endodontic diagnosis and treatment planning.37 There are many indications for using CBCT, but a primary tenet is to avoid the routine use of CBCT for the initial evaluation of endodontic cases. In other words, use a low radiation dose technique, such as a periapical radiograph, for initial evaluation. If there are more advanced diagnostic problems such as a tooth that requires re-treatment, complex root anatomy, suspected root fracture or root resorption etc., then CBCT would be indicated. As with all radiographic examinations, ensuring that the potential diagnostic benefit of the CBCT outweighs the risks of the additional radiation exposure is important in endodontic imaging. Using CBCT to evaluate orthodontic patients is a topic of discussion among many clinicians. Several post-graduate orthodontic programs teach their residents to routinely expose a CBCT scan on all orthodontic patients,38 yet many practicing orthodontists do not support this approach. The crux of this issue revolves around patient selection and the question of whether 3D radiographic examinations with full 3D cephalometric analyses are indicated for routine, Class I malocclusion cases with mild to moderate crowding for example. There are arguments pro and con on whether to use CBCT routinely.39, 40 The official American Association of Orthodontists (AAO) policy at this time is to use CBCT imaging selectively based on clinical judgment using factors such as asymmetrical growth patterns, missing teeth etc.41 One significant factor in this issue is the use of higher dose CBCT examinations with younger patients who are more sensitive to ionizing radiation.42 Another factor is the lack of studies comparing the efficacy of treatment outcomes of patients managed with routine 2D versus 3D cephalometry derived from CBCT volumes. The results of these or similar studies have the potential to provide a great deal of guidance on this issue. There are many other uses for CBCT in the dental office— TMJ examinations, localization of impacted teeth, evaluation of pathology and areas of trauma etc. that are based on specific clinical histories and examination findings. The dental professional must use these findings in conjunction with an understanding of the risks and benefits of CBCT imaging when deciding whether to order a scan. Risk to Benefit Analysis The risk to benefit analysis is the key to making the decision to order a CBCT scan or any other radiograph.9, 43-45 When you see the word ‘risk,’ medical physicists actually mean the chance of developing a fatal cancer. Effective dose was mentioned earlier and values of effective dose for selected radiographic examinations are given in Table 2. Effective dose allows us to compare the risk of a dental CBCT with the risk of a chest x-ray or a MDCT of the head or chest or any other radiographic examination for that matter. For any diagnostic question the clinician needs to answer, if CBCT is the modality that provides that answer with the lowest radiation to the patient, then CBCT is the best radiographic examination to use. The benefit to the patient is that more accurate www.ineedce.com and/or more predictable treatment can be rendered in a safer, quicker or more efficacious manner as a result of using CBCT imaging. The final treatment is often the result of a more comprehensive diagnosis achievable only by the use of CBCT imaging. In summary, since the risks of CBCT imaging are small; and, if it is likely that the information provided by the CBCT scan will improve the treatment outcome, then order the scan; however, if the information will not affect the treatment outcome, then the scan should not be ordered. Advanced Treatment Planning The literature is rife with examples of how to use CBCT for dental implantology;23, 26, 46-56 therefore, we will focus on advanced treatment planning in other areas of dentistry. Figures 4 and 5 show a difficult to diagnose caries case in tooth #20. The reconstructed panoramic width can vary from a few millimeters to a centimeter or more and will appear similar to a routine panoramic within the alveolar ridge region. As you will notice, the coronal aspect of #20 in the panoramic view does not reveal any alarming amount of caries. In the cross-sectional view seen in Figure 5 you will see a different story. Now that all the superimposed tissues have been removed, you see a low density area representing deep occlusal caries encroaching upon the pulp. Clinically there was not a break in the enamel and although the referring clinicians suspected incipient caries, they were not expecting the tooth to require endodontic therapy. Figure 4. CBCT panoramic reconstruction; note the normal appearance of the coronal aspect of tooth #20 with mild periapical PDL space widening. Figure 5. Note the significant change in density of the dentin between the pulp chamber and the occlusal enamel, and proximity of the low density dentin to the pulp chamber; in addition, there is slight widening of the PDL space with mildly increased periapical bone density. 5 Figures 6—9 are from an endodontic case showing selected screenshots from a volume referred for implant treatment planning and an over-read. As you can see from the reconstructed panoramic and multiplanar views, there are three endodontically treated teeth that illustrate commonly seen entities on CBCT images. Figure 7 shows tooth #10 with a widened PDL space in the apical region extending palatally with a mild effect on the endosteal surface of the palatal cortex. Figure 8 shows #15 with a widened periapical PDL space that has affected the buccal cortical plate. Figure 9 shows coronal and axial views of tooth #19, revealing an untreated mesiolingual canal. Remember, these are all incidental findings seen in a case referred for dental implant planning and Figure 9. MPR views including a cross-sectional view of #19; note the void in the area of the mesiolingual canal indicating a lack of an endodontic filling. Figure 6. Reconstructed panoramic of a CBCT case referred for implant planning. Figure 7. MPR views from the implant planning case shown in Figure 6, including a cross-sectional view of #10; note the widened PDL space and mild thinning of the palatal cortex. review by an oral radiologist, not for evaluation of these endodontically treated teeth. The recommendation in the radiology report was for endodontic re-treatment of #19 and monitoring of teeth #’s 10 & 15 since they were asymptomatic. The next case is an example of maxillary canine localization with evaluation of effects on surrounding teeth in a 15 year-old female. Figure 10 is a conventional panoramic and Figure 11 is a CBCT reconstructed panoramic. Large follicular spaces are associated with the impacted maxillary canines. In addition, there is significant resorption of the apices of the lateral incisors as seen on the cross-sectional views in Figures 12 and 13. With the information provided by CBCT imaging, a realistic approach for moving these canines into the arch can be developed. Furthermore, the patient and parents can be informed as to realistic expectations for the future of the lateral incisors. Figure 10. A conventional panoramic radiograph with impacted maxillary canines. Figure 8. MPR views including a cross-sectional view of #15; note the widened PDL space and the effect on the buccal cortical plate. Figure 11. A CBCT panoramic reconstruction of the same patient from Figure 10. 6www.ineedce.com Figure 12. MPR and volumetric views of impacted #6 with apical resorption of #7. Figure 16. MPR and volumetric views of the same patient from Figures 14 & 15; note the oblique fracture of the palatal root of tooth #4. Figure 13. MPR and volumetric views of impacted #11 with apical resorption of #10. Figure 17. The oblique fracture of the palatal root of #4 is more easily seen in this close-up cross-sectional view. The next case is an example of a 67 year-old female who presented to the clinic with intractable pain in the posterior right maxilla. She reported seeing multiple dentists as well as a neurologist. As noted in Figures 14 & 15, routine 2D imaging does not reveal an obvious cause for her discomfort; however, the cross-sectional view of tooth #4 revealed an oblique fracture of the palatal root (Figures 16 & 17). The patient’s symptoms improved dramatically upon removal of the tooth. Figure 14. Conventional panoramic image to evaluate posterior right maxillary pain. The following case illustrates an area that we all need to be mindful of—accessory neurovascular bundles. Figure 18 is the reconstructed panoramic of a patient referred for implant planning; a curvilinear corticated area of low density oriented in vertical plane was noted palatal to the #12 implant site as seen on the axial and coronal reconstructions (Figures 19 & 20). These are aberrant courses of the middle superior alveolar neurovascular bundle and are occasionally seen in the maxillary premolar to canine region. The size of these neurovascular channels are large enough to potentially cause significant bleeding if injured during implant surgery; so, prior knowledge of their presence and anatomic location is quite important for the implant surgeon.57-59 Figure 18. Reconstructed CBCT panoramic view of a case for implant planning. Note the fiduciary markers noting the planned implant locations. Figure 15. Periapical radiograph of tooth #4. www.ineedce.com 7 Figure 19. Axial slice through the maxilla; note the maxillary canine root apices and the corticated area of low density palatal to tooth #11 denoted by the dotted orange circle. Figure 20. A coronal reconstruction posterior to tooth #11 through the corticated low density seen in Figure 19; a curvilinear, corticated low density structure is seen coursing longitudinally through the maxilla in the first premolar/canine region. Figure 21. Routine periapical radiograph of tooth #9; this tooth had a history of trauma three months prior to this radiograph. Figure 22. MPR views with volumetric reconstruction of the trauma patient seen in Figure 21. Figure 23. Close-up sagittal views of tooth #9 revealing the communication of the endodontic lesion with the tissues within the floor of the nasal fossa. The final advanced treatment planning example is a trauma case. A 17 year-old male who had suffered a bicycle injury about 3 months previously was referred to the Oral Diagnostic Services Clinic for advanced imaging to determine whether the periapical lesion associated with tooth #9 communicated with the nasal fossa. Figure 21 shows a PA of tooth #9 with ~2 cm radiolucency in the periapical region that extended along the distal root surface. Figure 22 is the multiplanar reconstruction with panoramic, coronal, crosssectional and axial views showing different aspects of the lesion. Figure 23 is the close-up cross-sectional view that does indeed show decreased density of the cortical floor of the nasal fossa as well as changes within the nasal mucosa, both of which reflect a communication of this large periapical granuloma or perhaps radicular cyst with the nasal fossa. This tooth was treated with a conventional endodontic procedure and is currently healing well. These advanced treatment planning cases were chosen to illustrate the unique imaging principles and value that 3D CBCT imaging holds for the practicing dentist. Routine periapical and panoramic images were unable to provide the clinician with the advanced type of diagnostic information gained from these CBCT images. CBCT technology enhances the art and science of advanced interdisciplinary treatment planning in a manner which is not currently available from other officebased imaging modalities. 8www.ineedce.com Medicolegal Issues A recurring question at seminars and courses with clinicians is whether all of the images contained in a CBCT dataset needs to be reviewed. The AAOMR and many other authors have expressed the opinion that the entire CBCT dataset needs to be reviewed.35, 43, 45, 60, 61 The basic premise is that a dentist is responsible for interpreting the entire content of periapical, bitewing, panoramic and cephalometric radiographs. The only difference between these radiographs and a CBCT is the volume of information contained in the dataset. If the dentist does not feel comfortable assuming the responsibility for reviewing the entire volume, referral to an OMFR (Oral & Maxillofacial Radiologist) would be an option. Continuing dental education courses are available through the AAOMR and ADA Annual Sessions to assist CBCT machine owners with interpretation training. In addition, owners of CBCT machines should contact the manufacturer of their machine for information regarding training in not only operation of the machine, but also a review of 3D anatomy, basic interpretation of CBCT volumes as well as a review of oral pathology. A second question relates to management of incidental findings. An incidental finding can be defined as a radiographically or clinically significant condition seen on a radiograph that is unrelated to the original diagnostic question or original purpose for exposing the radiograph. Common incidental findings include thickened maxillary sinus mucosa, antral pseudocysts, concha bullosae, tonsiliths, enostoses, TMJ remodeling and undiagnosed periapical pathology,62, 63 Clinicians who are new owners of CBCT machines face not only the challenge of learning, or re-learning, these and other maxillofacial conditions, entities and anatomic features, but they or their office staff must also invest the added time and effort to manage referrals to the proper healthcare provider for evaluation and/or follow-up. This is an unexpected burden for many new CBCT machine owners. Summary Cone beam CT is arguably the greatest technological advancement that dental radiology has witnessed. The dental profession now has the ability in virtually any dental office, on a daily basis, to generate full 3D images of our patients’ dental and maxillofacial complex. These images are reliably accurate with no magnification and unfettered by superimposition from other anatomic structures. We can see individual teeth and supporting tissues from any and all angles providing previously impossible to achieve comprehensive oral and dental diagnoses. If you were not excited about the potential for CBCT in your practice before this course, I do hope that you now share the excitement of the dentists who own and use CBCT technology, and hope that you plan to utilize the technology in your practice!! Bibliography 1. Mozzo P, Procacci C, Tacconi A, Martini PT, Andreis IA. A new volumetric CT machine for dental imaging based on the cone-beam technique: preliminary results. Eur Radiol. 1998;8(9):1558-64. PubMed PMID: 9866761. www.ineedce.com Epub 1998/12/29. eng. 2. Hsieh J, editor A practical cone beam artifact correction algorithm. Nuclear Science Symposium Conference Record, 2000 IEEE; 2000: IEEE. 3. Hsieh J, Molthen RC, Dawson CA, Johnson RH. An iterative approach to the beam hardening correction in cone beam CT. Medical physics. 2000;27:23. 4.Jaffray DA, Siewerdsen J. Cone-beam computed tomography with a flat-panel imager: initial performance characterization. Medical physics. 2000;27:1311. 5. Endo M, Tsunoo T, Nakamori N, Yoshida K. Effect of scattered radiation on image noise in cone beam CT. Medical physics. 2001;28:469. 6.Siewerdsen JH, Jaffray DA. Cone-beam computed tomography with a flat-panel imager: magnitude and effects of x-ray scatter. Medical physics. 2001;28:220. 7. Langland OE, Langlais RP, McDavid WD, DelBalso AM. Panoramic Radiology. Second ed. Philadelphia, PA: Lea & Febiger; 1989. 440 p. 8.Farman AG. Panoramic Radiology: Seminars on Maxillofacial Imaging and Interpretation. Berlin, Germany: Springer-Verlag; 2007. 231 p. 9. White S, Pharoah M. Oral Radiology: Principles and Interpretation. Sixth ed. St. Louis, MO: Mosby Elsevier; 2009. 641 p. 10. Klinge B, Petersson A, Maly P. Location of the mandibular canal: comparison of macroscopic findings, conventional radiography, and computed tomography. Int J Oral Maxillofac Implants. 1989;4(4):327. 11.Ludlow JB, Nesbit SP. Teaching radiographic localization in dental schools in the United States and Canada. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1995 Mar;79(3):393-7. PubMed PMID: 7621017. Epub 1995/03/01. eng. 12. Jacobs S. Radiographic localization of unerupted teeth: Further findings about the vertical tube shift method and other localization techniques. American Journal of Orthodontics and Dentofacial Orthopedics. 2000;118(4):439-47. 13.Ludlow JB. Beam geometry and localization of structures. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2001 Oct;92(4):364-5. PubMed PMID: 11598565. Epub 2001/10/13. eng. 14.Richards A. The buccal object rule. Dental radiography and photography. 1980;53(3):37. 15.Richards AG. The Buccal Object Rule 1980 [April 10, 2013]. Available from: http://www.unc.edu/~jbl/ BuccalObjectRule.html. 16.Bushberg JT, Seibert JA, Leidholdt J, Edwin M., Boone JM. The Essential Physics of Medical Imaging [Kindle Edition]. Philadelphia, PA: Lippincott Williams & Wilkins, a Wolters Kluwer business; 2012. 17.Miles DA. Color Atlas of Cone Beam Volumetric Imaging for Dental Applications. Chicago: Quintessence Publishing Co, Inc; 2008. 310 p. 9 18.Scarfe WC, Farman AG. What is Cone-Beam CT and How Does it Work? Dental Clinics of North America: Contemporary Dental and Maxillfoacial Imaging. 2008 October 2008;52(4):24. 19.Koong B. Cone beam imaging: is this the ultimate imaging modality? Clinical Oral Implants Research. 2010;21(11):1201-8. 20.Mah P, Reeves TE, McDavid WD. Deriving Hounsfield units using grey levels in cone beam computed tomography. Dentomaxillofacial Radiology. 2010 September 1, 2010;39(6):323-35. 21.Reeves T, Mah P, McDavid W. Deriving Hounsfield units using grey levels in cone beam CT: a clinical application. Dentomaxillofacial Radiology. 2012 September 1, 2012;41(6):500-8. 22.Nomura Y, Watanabe H, Honda E, Kurabayashi T. Reliability of voxel values from cone-beam computed tomography for dental use in evaluating bone mineral density. Clinical Oral Implants Research. 2010;21(5):55862. 23. Sarment DP, Sukovic P, Clinthorne N. Accuracy of implant placement with a stereolithographic surgical guide. Int J Oral Maxillofac Implants. 2003 Jul-Aug;18(4):571-7. PubMed PMID: 12939011. Epub 2003/08/27. eng. 24.Benjamin L. The evolution of multiplanar diagnostic imaging: predictable transfer of preoperative analysis to the surgical site. Journal of Oral Implantology. 2002;28(3):13544. 25.Fortin T, Bosson JL, Coudert JL, Isidori M. Reliability of Preoperative Planning of an Image-Guided System for Oral Implant Placement Based on 3-dimensional Images: An In Vivo Study. Int J Oral Maxillofac Implants. 2003;18(6):886-93. 26. Tardieu PB, Rosenfeld AL, editors. The Art of ComputerGuided Implantology. Chicago IL: Quintessence Publishing Co, Inc; 2009. 27. Rosenfeld AL, Mandelaris GA, Tardieu PB. Prosthetically directed implant placement using computer software to ensure precise placement and predictable prosthetic outcomes. Part 1: diagnostics, imaging, and collaborative accountability. The International journal of periodontics & restorative dentistry. 2006;26(3):215. 28. Ganz SD. Computer-aided design/computer-aided manufacturing applications using CT and cone beam CT scanning technology. Dent Clin North Am. 2008 Oct;52(4):777-808, vii. PubMed PMID: 18805229. Epub 2008/09/23. eng. 29. Mettler FA, Huda W, Yoshizumi TT, Mahesh M. Effective Doses in Radiology and Diagnostic Nuclear Medicine: A Catalog1. Radiology. 2008;248(1):254. 30.Ludlow JB, Ivanovic M. Comparative dosimetry of dental CBCT devices and 64-slice CT for oral and maxillofacial radiology. Oral Surg Oral Med Oral Pathol. 2008 Jul;106(1):106-14. PubMed PMID: 18504152. Epub 2008/05/28. eng. 31. Loubele M, Bogaerts R,Van Dijck E, Pauwels R,Vanheusden S, Suetens P, et al. Comparison between effective radiation dose of CBCT and MSCT scanners for dentomaxillofacial applications. Eur J Radiol. 2009;71(3):461-8. 32.NCRP. NCRP Report #145: Radiation Protection in Dentistry. Bethesda, MD: National Council on Radiation Protection and Measurements; 2004. p. 1, 3, 14-6, 48, 80-4. 33.NCRP. NCRP Report #160: Ionizing Radiation Exposure of the Population of the United States. Bethesda, MD: National Council on Radiation Protection and Measurements, 2009 March 3, 2009. Report No. 34.Tyndall D, Brooks S. Selection criteria for dental implant site imaging: a position paper of the American Academy of Oral and Maxillofacial radiology. Oral surgery, oral medicine, oral pathology, oral radiology, and endodontics. 2000;89(5):630. 35.Tyndall DA, Price JB, Tetradis S, Ganz SD, Hildebolt C, Scarfe WC. Position statement of the American Academy of Oral and Maxillofacial Radiology on selection criteria for the use of radiology in dental implantology with emphasis on cone beam computed tomography. Oral Surgery, Oral Medicine, Oral Pathology and Oral Radiology. 2012;113(6):817-26. 36. Benavides E, Rios HF, Ganz SD, An CH, Resnik R, Reardon GT, et al. Use of cone beam computed tomography in implant dentistry: the International Congress of Oral Implantologists Consensus Report. Implant Dentistry. 2012;21(2):78-86. 37.Use of cone-beam computed tomography in endodontics Joint Position Statement of the American Association of Endodontists and the American Academy of Oral and Maxillofacial Radiology. Oral surgery, oral medicine, oral pathology, oral radiology, and endodontics. 2011;111(2):234-7. 38.Smith BR, Park JH, Cederberg RA. An Evaluation of Cone-Beam Computed Tomography Use in Postgraduate Orthodontic Programs in the United States and Canada. Journal of Dental Education. 2011;75(1):98. 39. Larson BE. Cone-beam computed tomography is the imaging technique of choice for comprehensive orthodontic assessment. American Journal of Orthodontics and Dentofacial Orthopedics. 2012;141(4):402-10. 40.Halazonetis DJ. Cone-beam computed tomography is not the imaging technique of choice for comprehensive orthodontic assessment. American Journal of Orthodontics and Dentofacial Orthopedics. 2012;141(4):403-11. 41.Orthodontists AAo. Statement on the role of CBCT in orthodontics (26—10H) [eBulletin]. 2010 [updated May 7, 2010January 7, 2013]. Available from: https:// http://www.aaomembers.org/Resources/Publications/ ebulletin-05-06-10.cfm? 42. Brenner D, Hall E. Computed tomography--an increasing source of radiation exposure. The New England Journal of Medicine. 2007;357(22):2277. 43.Affairs TADACoS. The use of cone-beam computed 10www.ineedce.com tomography in dentistry: An advisory statement from the American Dental Association Council on Scientific Affairs. The Journal of the American Dental Association. 2012 August 1, 2012;143(8):899-902. 44. Schueler B, Abbara S, Bettmann M, Hevezi J, Madsen M, Morin R, et al. ACR Appropriateness Criteria Radiation Dose Assessment Introduction: American College of Radiology; 2012 [updated 2012; cited 2012 September 9, 2012]. Available from: http://www.acr.org/%7E/media/ A27A29133302408BB86888EAFD460A1F.pdf. 45.Carter L, Farman A, Geist J, Scarfe W, Angelopoulos C, Nair M, et al. American Academy of Oral and Maxillofacial Radiology executive opinion statement on performing and interpreting diagnostic cone beam computed tomography. Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, & Endodontics. 2008;106(4):561-2. 46. Fortin T, Champleboux G, Bianchi T, Buatois H, Coudert H. Precision of transfer of preoperative planning for oral implants based on cone-beam CT-scan images through a robotic drilling machine. Clinical Oral Implants Research. 2002;13(6):651-6. 47.Hatcher D, Dial C, Mayorga C. Cone beam CT for presurgical assessment of implant sites. CDA. 2003;31(11):82534. 48.Almog D, LaMar J, LaMar F, LaMar F. Cone beam computerized tomography-based dental imaging for implant planning and surgical guidance, Part 1: Single implant in the mandibular molar region. Journal of Oral Implantology. 2006;32(2):77-81. 49.Nickenig HJ, Eitner S. Reliability of implant placement after virtual planning of implant positions using cone beam CT data and surgical (guide) templates. J Craniomaxillofac Surg. 2007 Jun-Jul;35(4-5):207-11. PubMed PMID: 17576068. Epub 2007/06/20. eng. 50.Ganz SD. The use of CT/CBCT and interactive virtual treatment planning and the triangle of bone: defining new paradigms for assessment of implant receptor sites. In: Babbush CA, Hahn JA, Krauser JT, Rosenlicht JL, editors. Dental Implants: The Art and Science. Philadelphia, PA: Saunders; 2010. p. 146-66. 51.Katsoulis J, Pazera P, Mericske-Stern R. Prosthetically driven, computer-guided implant planning for the edentulous maxilla: a model study. Clinical Implant Dentistry and Related Research. 2009;11(3):238-45. 52.Kau CH, Richmond S. Three-dimensional imaging for orthodontics and maxillofacial surgery: Wiley-Blackwell; 2010. 53.Singh PP, Cranin AN. Atlas of oral implantology: Mosby; 2009. 54. Zoller JE, Neugebauer J. Cone-beam Volumetric Imaging in Dental, Oral and Maxillofacial Medicine: Fundamentals, Diagnostics and Treatment Planning. Londone: Quintessence Publishing Co. Ltd.; 2008. 214 p. 55. Brown J, Clark F. Galileos Cone-Beam & CEREC Integration [iBook]. iBookstore: Apple; 2013 April 10, 2013]. www.ineedce.com 56.August de Oliveira D. Implants Made Easy: Implants Made Easy; 2010. 57. Romanos G, Greenstein G. The incisive canal. Considerations during implant placement: case report and literature review. Int J Oral Maxillofac Implants. 2009;24(4):740. 58.Makris N, Stamatakis H, Syriopoulos K, Tsiklakis K, van der Stelt P. Evaluation of the visibility and the course of the mandibular incisive canal and the lingual foramen using cone-beam computed tomography. Clinical Oral Implants Research. 2010. 59. Greenstein G, Cavallaro J, Romanos G, Tarnow D. Clinical recommendations for avoiding and managing surgical complications associated with implant dentistry: a review. J Periodontol. 2008 Aug;79(8):1317-29. PubMed PMID: 18672980. Epub 2008/08/05. eng. 60. Zinman E, White S, Tetradis S. Legal considerations in the use of cone beam computer tomography imaging. Journal of the California Dental Association. 2010;38(1):49. 61.Friedland B, editor Medicolegal issues related to cone beam CT2009: Elsevier. 62.Price JB, Thaw KL, Tyndall DA, Ludlow JB, Padilla RJ. Incidental findings from cone beam computed tomography of the maxillofacial region: a descriptive retrospective study. Clinical Oral Implants Research. 2012;23(11):1261-8. 63.Cha J, Mah J, Sinclair P. Incidental findings in the maxillofacial area with 3-dimensional cone-beam imaging. American Journal of Orthodontics and Dentofacial Orthopedics. 2007;132(1):7-14. Author Profile Jeffery B. Price, DDS, MS is a Diplomate of the American Board of Oral & Maxillofacial Radiology. He is currently an Assistant Professor of Oral & Maxillofacial Radiology and Director of Oral & Maxillofacial Radiology at the Meharry Medical College School of Dentistry in Nashville, TN; in addition, he is an Adjunct Associate Professor of Oral & Maxillofacial Radiology at the UNC School of Dentistry in Chapel Hill, NC. Dr. Price is also a consultant with Sirona Dental and teaches many of their Galileos new users training courses. He also has an internet-based Cone Beam CT interpretation practice. Dr. Price practiced general and adult restorative dentistry in Hendersonville, NC for 24 years. While in practice, Dr. Price completed the continuum at the L.D. Pankey Institute in Key Biscayne, FL; in addition, he attained his Mastership in the Academy of General Dentistry as well as Diplomate status in the International Congress of Oral Implantologists. Dr. Price is currently on the editorial board of the ICOI-sponsored journal, Implant Dentistry; and, is a reviewer for IJOMS, JDE and JADA. Disclaimer Jeffrey B Price, DDS, MS discloses that he is a consultant to Sirona Dental, the commercial supporter of this educational activity. Dr. Price further discloses that he is a faculty member for Sirona Galileos new users training and operates an internet consultation service for Cone Beam CT interpretation. Reader Feedback We encourage your comments on this or any PennWell course. For your convenience, an online feedback form is available at www. ineedce.com. 11 Online Completion Use this page to review the questions and answers. Return to www.ineedce.com and sign in. If you have not previously purchased the program select it from the “Online Courses” listing and complete the online purchase. Once purchased the exam will be added to your Archives page where a Take Exam link will be provided. Click on the “Take Exam” link, complete all the program questions and submit your answers. An immediate grade report will be provided and upon receiving a passing grade your “Verification Form” will be provided immediately for viewing and/or printing. Verification Forms can be viewed and/or printed anytime in the future by returning to the site, sign in and return to your Archives Page. Questions 1.The single most significant feature of cone beam CT imaging is its ability to generate what type of images? a. b. c. d. Multiple panoramic images with different focal troughs Accurate, non-magnified 3D images Full face images with lateral and PA cephs 3D images of hard and soft tissues with equal diagnostic efficacy 2.What feature makes CBCT different from MDCT? a. The type of x-ray photons b. The shape of the x-ray beam—cone-shaped for CBCT and fan-shaped for MDCT c. The type of patient being imaged d. The area of the patient being imaged 3.The ‘2D Problem’ refers to which of the following? a. The inability of 2D images such as periapicals and panoramics to give information on the depth of objects being imaged b. Problems keeping the x-ray beam perpendicular to the receptor c. The problem of accurately tracking radiation doses d. The two problems of magnification and geometric distortion 4.Signal to noise ratio refers to _________________? a. The actual anatomic information (signal) contained in an x-ray beam or image as compared to the amount of scattered x-rays (noise). b. The ability of an x-ray detector to determine hard tissues from soft tissues. c. The ability of CBCT to provide images with excellent soft tissue contrast. d. The ability of CBCT to improve noisy images so that they can be of diagnostic quality. 5.Cone beam CT contains more scattered radiation (more noise) than MDCT techniques; how does this limit images taken with CBCT machines? a. CBCT images provide for excellent soft tissue contrast. b. CBCT images provide for excellent hard tissue contrast (bone and teeth). c. CBCT images can provide excellent contrast for both hard and soft tissues. d. CBCT is a poor imaging technique because of this noise and should no longer be used. 6.MPR is an acronym used in CBCT imaging; what does MPR mean? a. b. c. d. Most Pixel Reduction Many Pixel Resolution MultiPlanar Reconstruction Maximum Postal Reshaping 7.Which of the following statements best describes the term effective dose? a. A way to determine the penetrating ability, or effectiveness, of a radiation beam. b. The dose of ionizing radiation as measured at the skin. c. A dose of ionizing radiation measured in the organ; also known as the organ dose, such as the thyroid dose in dental x-rays. d. A calculated, estimated radiation dose used to compare the relative risks of various radiographic examinations from chest x-rays to CBCT scans and dental BWs. 8.Which of the following has the highest effective dose? a. b. c. d. D-speed FMX with round collimation A maxillofacial CBCT of 75 microSieverts An average maxillofacial multidetector CT An average panoramic x-ray 9.Background ionizing radiation is endemic; which of the following is the largest source of background radiation for the average person in the U.S.? a. Hydroxyl ions in water b. Radioactive uranium from nuclear power plants c. Radon from basements and building supplies like concrete d. Sunburns in the summer 10. The average daily background dose of ionizing radiation for the average person in the U.S. is approximately ________. a. b. c. d. 1 microSv 3 microSv 8 microSv 20 microSv 11. Approximately how many standard maxillofacial CBCT scans would equal the radiation dose of one FMX series taken with D-speed film using round collimation? a. About one maxillofacial CBCT scan per two D-speed film-based, round collimation FMX series b. About one maxillofacial CBCT scan per one D-speed film-based, round collimation FMX c. About two maxillofacial CBCT scans per one D-speed film-based, round collimation FMX d. About three to five maxillofacial CBCT scans per one D-speed film-based, round collimation FMX 12. If the field of view of a standard panoramic radiograph is used for comparison purposes, which of the following types of radiographic examinations would have the highest amount of radiation per volume of tissue exposed? a. Routine panoramic b. A standard maxillofacial CBCT scan of 300 micron resolution c. A high resolution maxillofacial CBCT scan of 100 micron resolution d. Medical MDCT 13. The AAOMR (American Academy of Oral & Maxillofacial Radiology) has recommended cross-sectional imaging for dental implantology since ________? a.1995 b.2000 c.2005 d.2010 14. The AAOMR currently recommends _________ as the imaging modality of choice for definitive dental implant treatment planning. a. Magnetic resonance imaging b.MDCT c. Periapical radiographs d.CBCT 15. A guideline for use of CBCT in endodontics as well as other areas of dentistry is: . a. First use a low-dose technique such as a periapical radiograph for the initial evaluation of patients to avoid routinely exposing CBCT scans on all patients b. CBCT scans should be used routinely as the initial radiographic examination for all patients c. CBCT use is indicated as a screening tool when new patients first come to the dental office d. Use CBCT on any patient to replace BW’s, PA’s or panoramic radiographs 16. A major principle of all radiographic examinations is:. a. To make sure the patient’s insurance will pay for the x-ray. b. To ensure that there is a reasonable expectation that the radiographic examination will provide a diagnostic benefit that will outweigh the risk of the radiation. c. Use good batteries in your exposure controller. d. Do not take the time to educate patients about radiation safety. 17. All of the following may be reasons for orthodontists to use CBCT technology; which ONE is generally NOT agreed upon by all orthodontists? a. b. c. d. Evaluate asymmetrical growth pattern Localizing impacted teeth Evaluate condylar growth Routine CBCT use on all orthodontic patients 18. Which of the following office routines is considered the optimal routine when considering radiographic examinations? a. Take CBCTs on all new patients b. Take a medical and dental history, perform a clinical examination and then decide on the appropriate radiographic examination to order c. Use CBCT examinations just to see what you might find d. CBCT scans are indicated for all endodontic diagnoses 19. The key to making the decision to order a CBCT scan is the ___________? a. b. c. d. Risk to benefit analysis Risk = return curve Return on investment analysis Radiation dose curve 20. According to medical physicists, the term ‘radiation risk’ means what? a. The chance of developing a radiation skin reaction after an x-ray exposure b. The opportunistic infection that occurs after an x-ray exposure c. The chance of developing a fatal cancer after an x-ray exposure d. The chance that vascular disease will develop in the area of an x-ray exposure. 21. A clinician should strongly consider ordering a CBCT scan if which of the following is true? a. The CBCT machine has not been used very much recently. b. The information provided by the scan will improve the treatment outcome. c. The information provided by the scan will not affect the treatment outcome. d. The patient requests a CBCT scan. 12www.ineedce.com Questions 22. One of the treatment planning examples showed a case of deep caries that was obscured on the reconstructed panoramic but visible on the cross-sectional images. Why do you think the cross-sectional images were better able to show the caries than the panoramic image? a. The panoramic image had more magnification b. The panoramic image had more geometric distortion c. The panoramic image had a thicker image layer and therefore had more superimposed tissues within the image thereby obscuring the caries d. The cross-sectional image was a more accurate image 23. According to the case discussed in the course, what difficulties do clinicians face when using CBCT imaging to evaluate endodontically treated teeth? a. b. c. d. Widened periapical PDL spaces Evaluate crown margins Evaluate fit of custom posts Evaluate for root resorption 24. Another treatment planning example using CBCT imaging was maxillary canine localization. What valuable pathologic feature besides canine localization was mentioned during the discussion of that case? a. b. c. d. Premolar transposition Pulpal recession Gingival recession Resorption of the apices of the lateral incisors 25. One of the treatment planning cases showed a fractured root on a maxillary premolar. Why do you think routine 2D imaging did not identify this fractured root? a. Sclerotic pulp chambers b. 2D imaging could not show the fracture within the correct long axis of the fracture; while in CBCT imaging, we can see teeth from any view, at any angle c. Poor radiographic technique by previous clinicians d. Dense bone overlying the roots 26. What is the significance of undiagnosed neurovascular bundles in proximity to implant osteotomy sites? a. There is no significance b. Implants should not be placed c. With proper technique, implant surgeons can vary placement, if necessary, so that large neurovascular bundles can be avoided to prevent intra- or postoperative bleeding d. Since most of these are actually benign bone marrow spaces and do not contain nerves and blood vessels, no special notice is required 27. In general, why would a clinician choose to use CBCT technology instead of 2D technology? a. To be able to see the patient in 3D so that advanced diagnostic information can be obtained b. Just to impress the patient with 3D images during the consultation c. To stay current with technology d. To use the latest equipment 28. When considering the topic of whether to look at only the area that the clinician is interested in, or evaluating all the images in a CBCT dataset, which of the following statements best describes the recommendation by the AAOMR? a. Practicing clinicians only need to look at the region of interest in the CBCT scan and not bother with looking at areas outside the region of interest. b. Clinicians need to look at all the images in a CBCT dataset; if they do not want to accept this responsibility, referral to an OMFR is an option. c. Clinicians only need to look at the 3D volume plus the area of interest in the CBCT images and not the entire CBCT dataset. d. Clinicians only need to look at the panoramic reconstruction and the area of interest in the CBCT images and not the entire CBCT dataset. 29. Common incidental findings seen on CBCT images include all of the following except which ONE? a. Thickened maxillary sinus mucosa b. Antral pseudocysts c.Tonsiliths d. Intracranial aneurysms 30. Which of the following is the greatest technological advancement in dental radiology? a. b. c. d. D-speed film Automatic daylight loaders XCP film holders Dental Cone Beam Computed Tomography Notes www.ineedce.com 13 Notes 14www.ineedce.com ANSWER SHEET Using Cone Beam CT in Clinical Practice Name: Title: Specialty: Address:E-mail: City: State:ZIP:Country: Telephone: Home ( ) Office ( Lic. Renewal Date: ) AGD Member ID: Requirements for successful completion of the course and to obtain dental continuing education credits: 1) Read the entire course. 2) Complete all information above. 3) Complete answer sheets in either pen or pencil. 4) Mark only one answer for each question. 5) A score of 70% on this test will earn you 2 CE credits. 6) Complete the Course Evaluation below. 7) Make check payable to PennWell Corp. For Questions Call 216.398.7822 If not taking online, mail completed answer sheet to Educational Objectives Academy of Dental Therapeutics and Stomatology, 1. Discuss the basic technology and principles of cone beam computed tomography (CBCT) for dental use. A Division of PennWell Corp. P.O. Box 116, Chesterland, OH 44026 or fax to: (440) 845-3447 2. Review the commonly administered doses of ionizing radiation patients receive during CBCT examinations 3. List key selection criteria and indications for the uses of CBCT in dental practice 4. Describe how CBCT examinations can enhance advanced treatment planning For immediate results, go to www.ineedce.com to take tests online. Answer sheets can be faxed with credit card payment to (440) 845-3447, (216) 398-7922, or (216) 255-6619. 5. Identify two medico-legal and ethical issues regarding the use of dental CBCT Course Evaluation 1. Were the individual course objectives met?Objective #1: Yes No Objective #2: Yes No Objective #3: Yes No Objective #4: Yes No Objective #5: Yes No P ayment of $49.00 is enclosed. (Checks and credit cards are accepted.) If paying by credit card, please complete the following: MC Visa AmEx Discover Please evaluate this course by responding to the following statements, using a scale of Excellent = 5 to Poor = 0. 2. To what extent were the course objectives accomplished overall? 5 4 3 2 1 0 Acct. Number: ______________________________ 3. Please rate your personal mastery of the course objectives. 5 4 3 2 1 0 Exp. Date: _____________________ 4. How would you rate the objectives and educational methods? 5 4 3 2 1 0 5. How do you rate the author’s grasp of the topic? 5 4 3 2 1 0 6. Please rate the instructor’s effectiveness. 5 4 3 2 1 0 7. Was the overall administration of the course effective? 5 4 3 2 1 0 8. Please rate the usefulness and clinical applicability of this course. 5 4 3 2 1 0 9. Please rate the usefulness of the supplemental webliography. 4 3 2 1 0 5 10. Do you feel that the references were adequate? Yes No 11. Would you participate in a similar program on a different topic? Yes No Charges on your statement will show up as PennWell 12. If any of the continuing education questions were unclear or ambiguous, please list them. ___________________________________________________________________ 13. Was there any subject matter you found confusing? Please describe. ___________________________________________________________________ ___________________________________________________________________ 14. How long did it take you to complete this course? ___________________________________________________________________ ___________________________________________________________________ 15. What additional continuing dental education topics would you like to see? ___________________________________________________________________ ___________________________________________________________________ AGD Code 165 PLEASE PHOTOCOPY ANSWER SHEET FOR ADDITIONAL PARTICIPANTS. COURSE EVALUATION and PARTICIPANT FEEDBACK We encourage participant feedback pertaining to all courses. Please be sure to complete the survey included with the course. Please e-mail all questions to: [email protected]. INSTRUCTIONS All questions should have only one answer. Grading of this examination is done manually. Participants will receive confirmation of passing by receipt of a verification form. Verification of Participation forms will be mailed within two weeks after taking an examination. COURSE CREDITS/COST All participants scoring at least 70% on the examination will receive a verification form verifying 2 CE credits. The formal continuing education program of this sponsor is accepted by the AGD for Fellowship/ Mastership credit. Please contact PennWell for current term of acceptance. Participants are urged to contact their state dental boards for continuing education requirements. PennWell is a California Provider. The California Provider number is 4527. The cost for courses ranges from $20.00 to $110.00. Provider Information PennWell is an ADA CERP Recognized Provider. ADA CERP is a service of the American Dental Association to assist dental professionals in identifying quality providers of continuing dental education. ADA CERP does not approve or endorse individual courses or instructors, nor does it imply acceptance of credit hours by boards of dentistry. Concerns or complaints about a CE Provider may be directed to the provider or to ADA CERP at www.ada. org/cotocerp/. The PennWell Corporation is designated as an Approved PACE Program Provider by the Academy of General Dentistry. The formal continuing dental education programs of this program provider are accepted by the AGD for Fellowship, Mastership and membership maintenance credit. Approval does not imply acceptance by a state or provincial board of dentistry or AGD endorsement. The current term of approval extends from (11/1/2011) to (10/31/2015) Provider ID# 320452. RECORD KEEPING PennWell maintains records of your successful completion of any exam for a minimum of six years. Please contact our offices for a copy of your continuing education credits report. This report, which will list all credits earned to date, will be generated and mailed to you within five business days of receipt. Completing a single continuing education course does not provide enough information to give the participant the feeling that s/he is an expert in the field related to the course topic. It is a combination of many educational courses and clinical experience that allows the participant to develop skills and expertise. CANCELLATION/REFUND POLICY Any participant who is not 100% satisfied with this course can request a full refund by contacting PennWell in writing. Image Authenticity The images provided and included in this course have not been altered. © 2013 by the Academy of Dental Therapeutics and Stomatology, a division of PennWell CT413PAT Customer Service 216.398.7822