* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download pacemaker malfunction
Survey
Document related concepts
Transcript
Pacemaker : overview
Chennai: Feb2017
The Implantable Pacemaker System
• The Implantable Pulse Generator (IPG) : metal can
(titanium) containing electronics/battery & an
electrode or lead connector header
• Lead : Electrical connection between the
pacemaker & the heart
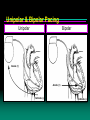
Unipolar & Bipolar Pacing
Bipolar
Unipolar
Anode (+)
Anode (+)
Cathode (-)
Cathode (-)
A Bipolar Pacing System Contains a Lead with Two Electrodes Within
the Heart. In This System, the Impulse:
• Flows through the tip
electrode located at
the end of the lead
wire
• Stimulates the heart
• Returns to the ring
Anode
Cathode
electrode above the
lead tip
Tip electrode coil
Indifferent electrode
coil
Pacemaker Functions
• Stimulation of Cardiac Tissue
• Sensing of natural (intrinsic) cardiac
depolarization or contraction
• Diagnostic information
Voltage, Current, and Impedance Are Interdependent
– Voltage represents the force with which . . .
– Current (water) is delivered through . . .
– A hose, or lead, where each component
represents the total impedance:
•
The nozzle, representing the electrode
•
The tubing, representing the lead wire
Ohm’s Law
Voltage = Current X Resistance (V=IR)
Current = Voltage/Resistance
As voltage increases, current increases
As resistance decreases, current increases
The Pacing Pulse
Output Voltage
Pacing Pulse
V = Pulse Amplitude in Volts (V) (say 2.5 V)
t = Pulse Duration or Width in milliseconds (ms)
(say 0.5 ms)
t
V
R = Impedance of Pacing Circuit (ohms)
(say 500 ohms)
t
Pulse Duration (Width)
I = V/R = Current through pacing circuit (mA)
= 2.5 V/ 500 ohms = 0.005 A = 5 mA
Stimulation Threshold
• Pacing Voltage Threshold – The minimum pacing
voltage at any given pulse width required to
consistently stimulate the heart causing it to
contract
Capture – Loss of Capture
Capture
VVI / 60
Non-Capture
NBG Code for Pacing
I
Chamber
Paced
II
Chamber
Sensed
III
Response
to Sensing
IV
Programmable
Functions/Rate
Modulation
V: Ventricle
V: Ventricle
T: Triggered P: Simple
programmable
A: Atrium
A: Atrium
I: Inhibited
M: Multiprogrammable
D: Dual (A+V) D: Dual (A+V) D: Dual (T+I) C: Communicating
O: None
O: None
S: Single
S: Single
(A or V)
(A or V)
O: None
V
Antitachy
Function(s)
P: Pace
S: Shock
D: Dual (P+S)
R: Rate modulating O: None
O: None
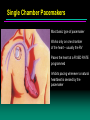
Single Chamber Pacemakers
Most basic type of pacemaker
Works only on one chamber
of the heart – usually the RV
Paces the heart at a FIXED RATE
programmed
Inhibits pacing whenever a natural
heartbeat is sensed by the
pacemaker
Single Chamber Pacemakers
Ventricular Single Chamber Pacing or VVI pacing
Pacing Rate
Pacing Rate
Pace
Pace
Sense
Pace
Single-Chamber System
AAI
VVI
Dual Chamber Pacemakers
• DDD, DDDR – sense & pace both atrium and
ventricle
• VDD – Sense atrium, pace ventricle
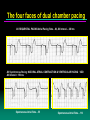
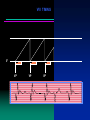
The four faces of dual chamber pacing
AV SEQUENTIAL PACING Atrial Pacing Rate – 60, AV Interval – 200 ms
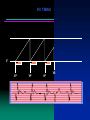
AV Synchronous Pacing :NATURAL ATRIAL CONTRACTION & VENTRICULAR PACING : VDD
AV Interval = 150 ms
Spontaneous Atrial Rate – 55
Spontaneous Atrial Rate – 110
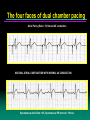
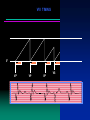
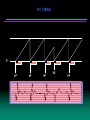
The four faces of dual chamber pacing
Atrial Pacing Rate = 70, Natural AV conduction
NATURAL ATRIAL CONTRACTION WITH NORMAL AV CONDUCTION
Spontanoeus Atrial Rate = 65, Spontaneous PR interval = 160 ms
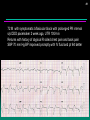
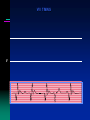
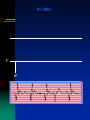
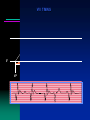
#1
72 M with symptomatic bifasicular block with prolonged PR interval
s/p DDD pacemaker 2 week ago, UTR 100/min
Returns with history of atypical R sided chest pain and back pain
SBP 70 mm Hg BP improved promptly with IV fluid and pt felt better
Typical values
• LRL : 50-60/mt
• URL : 110-130/mt
• AV delay : 120-200/ms
• PVARP : 250 ms
• VRP : 200 ms
• Blanking periods : < 50 ms
Sensing of intrinsic heartbeats
• Sensing is the ability of the pacemaker to “see” when a
natural (intrinsic) depolarization is occurring
– Pacemakers record the Intracardiac Electrogram (EGM)
by constantly recording the potential difference
between the cathode and anode
Depolarization Wave
Processed by
Device
Undersensing
• Pacemaker does not “see” the intrinsic beat, and
therefore does not respond appropriately
Intrinsic beat
Scheduled pace
delivered
VVI / 60
Oversensing
Marker channel
shows intrinsic
activity...
...though no
activity is
present
VVI / 60
• An electrical signal other than the intended P or R
wave is detected
• Pacing is inhibited
Amplitude Threshold Testing
Keeping pulse width stable, decrement voltage until
loss of capture
@ 0.5ms
1.5V
1.0V
.5V
Intrinsic R wave Amplitude
• Typical intrinsic R wave amplitude measured
from pacing leads in the Right Ventricle are
more than 5 mV in amplitude
Intrinsic R wave in EGM
The Intrinsic R wave amplitude is usually much greater than the T wave amplitude
Sensitivity Setting
This is a value specified to the pacemaker in millivolts through programming.
All ventricular electrogram deflections seen by the pacing lead that exceed the
sensitivity setting will be identified by the pacemaker as intrinsic R waves
The typical sensitivity setting that is programmed for Ventricular sensing is 2.5 mV
Sensitivity Setting
2.5
1.25
Time
5.0
Amplitude (mV)
Amplitude (mV)
5.0
2.5
1.25
Time
Sensitivity settings less than 2.5 mv – High sensitivity – can lead
to oversensing
Sensitivity settings greater than 2.5 mV – Low sensitivity – can
lead to undersensing
VVI Mode
Lower Rate Interval
•
{
Pacing inhibited with intrinsic activity
VP
Blanking/Refractory
VVI / 60
VS
VP
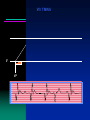
VVI TIMING
V
VP
VP
VP
VS
VP
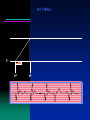
VVI TIMING
V
VP
VP
VP
VS
VP
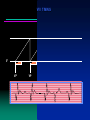
VVI TIMING
V
VP
VP
VP
VS
VP
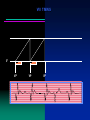
VVI TIMING
V
VP
VP
VP
VS
VP
VVI TIMING
V
VP
VP
VP
VS
VP
VVI TIMING
V
VP
VP
VP
VS
VP
VVI TIMING
V
VP
VP
VP
VS
VP
VVI TIMING
V
VP
VP
VP
VP
VVI TIMING
V
VP
VP
VP
VS
VP
VVI TIMING
V
VP
VP
VP
VS
VP
VVI TIMING
V
VP
VP
VP
VS
VP
VVI @ 65/mt
VVI
VVI
VVI
VVI
Fusion beat
Sensed native R waves reset VVI timing
Presenting Rhythm and Rate
Battery Status
Lead Status
Sensing
Threshold
Observation, Data, and Events
Program
39
UC200702005 EN
Medtronic, Inc. USA
September 2006
Diagnostic Information
Cardiac Compass®
Management of atrial
tachyarrhythmias
May help with assessment of:
• Rate-control therapy
• Rhythm-control therapy
• Risk for stroke1
1Glotzer
TV, Hellkamp AS, Zimmerman J. et al., Atrial high rate episodes detected by pacemaker diagnostics predict death
and stroke: Report of the Atrial Diagnostics Ancillary Study of the Mode Selection Trial (MOST).
Circulation 2003;107:1614-1619.
Potential Problems with Pacemakers
•
Battery Depletion
•
Lead displacement or perforation
– Loss of capture and/or sensing
•
Lead fracture or insulation break
– Loss of capture and/or sensing
•
Increase in thresholds due to
•
Drugs
•
Electrolyte imbalance
•
Interference from external electromagnetic sources
•
Device malfunction
Pacemaker Follow-up
•All the Information for Routine Follow-ups
Operating
Mode
Last Interrogation
Longevity
A&V Pacing
Thresholds
Arrhtymia
Summary
% Pace/Sense
Histograms
A&V Pacing
Lead
Impedance
P&R wave
Amplitudes
Alert of situations
that may require
further
investigation
Magnet Operation
• Varies across manufacturers and models
• Medtronic Normal
-
VOO, DOO mode 85 ppm
-
No sensing, asynchronous pacing
• Medtronic ERI – VOO, DOO mode 65 ppm
Special Precautions – EMI
•
General Principle
– Avoid proximity to powerful electric or magnetic fields
– Move away from the field if symptomatic
– Keep safe distance – 6 inches for electrical appliances
•
Safe from Interference
– Microwave, TV, Washing Machine, Fridge, Vacum cleaners etc.
– Cordless phones
– Computer, printer, scanner, photcopier
•
Possible interference
– Items with large magnets, e.g. speakers, car ignition systems
– Hand-held hair dryers
– Radiotransmitters
– Cellular Phones