* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download The sore throat
Survey
Document related concepts
Chagas disease wikipedia , lookup
Rocky Mountain spotted fever wikipedia , lookup
Orthohantavirus wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Herpes simplex virus wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Oesophagostomum wikipedia , lookup
West Nile fever wikipedia , lookup
Marburg virus disease wikipedia , lookup
Hepatitis B wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Schistosomiasis wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Leptospirosis wikipedia , lookup
Transcript
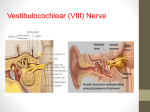
Contents Syllabus: Department Textbook Teaching: Daily teaching over 6 weeks in 3 sessions (2 weeks each) A. Ear Session B. Nose Session C. Throat Session Each day: A. 9-10 am (academic hour), B. 10-11 am diagnostic approach, C. 11 am to 12 pm clinical tour (according to schedule) Ear Diagnostic Approach "flowchart" a. Acute otitis media b. Facial weakness c. SNHL d. Vertigo Nose Diagnostic Approach "flowchart" a. Nasal obstruction b. Epistaxis c. Headache Throat Diagnostic Approach "flowchart" a. Sore throat b. Neck mass c. Stridor |Page1 Acute Otitis Media Flowchart >12 months, Immune-competent Analgesia, No antibiotics for 1st 24-48 hours Yes No Analgesia, Antibiotics: Amoxicillin 45 mg/kg/d/ 5days Amoxicillin-clavulanic acid 45 mg/kg/d/ 5days Ceftriaxone 50 mg/kg monotherapy (FDA) No Symptoms Resolved Yes Symptoms improved by 48 hours Yes Check for OME if HL or persistent irritability > 2-3 months No Alternative diagnosis None Double the dose of antibiotic for 5 days |Page2 Facial weakness and Bells palsy flowchart Gradual onset > few days or feeling unwell Yes Unlikely to be Bell,s Neurology No Is there any other Neurological deficit? Yes Neurology Neuro-imaging Yes Neurology Neuro-imaging No Spared forehead muscles? No Head & facial trauma? Yes Neurosurgery ENT surgery Plastic surgery Imaging No Signs of OM, Parotitis, Mastoiditis or Ear surgery? Yes ENT surgery No Blisters on ear or face? Yes Acyclovir for HSV or HZV No Treat as Bell's Palsy |Page3 Sensori-Neural Hearing Loss History & assessment Elderly: Presbyacusis Young / Middle age PTA Symmetric High frequency: Presbyacusis Systemic cause: Infective Metabolic Endocrine Haematologic Trauma Asymmetric Low frequency: Meniere's disease MRI: Rule out acoustic neuroma ECoG Caloric test, Blood Any Frequency Aetiology of SNHL Developmental and hereditary Nonsyndromic hereditary hearing loss Waardenburg’s syndrome Alport’s syndrome Usher’s syndrome Inner ear anomalies Infectious disorders Labrynthitis Otitis media Viral infections Bacterial-syphilis Drug induced Renal Trauma Irradiation Neurological |Page4 Vertigo: Differential diagnosis Vertigo does imply some form of illusion of movement, mostly spinning. All other symptoms are grouped under dizziness. After taking a history and doing an examination the clinician needs to decide the following: Illusion of movement Other (Dizziness) Spinning (Vertigo) Central Peripheral Unilateral Bilateral Brainstem Cerebellar Three typical forms of peripheral vestibular dysfunction can be identified, based on their characteristic symptoms and signs: 1. Acute or subacute unilateral vestibular failure: rotational vertigo, oscillopsia, and a tendency to fall toward the affected ear usually acute vestibular neuritis. 2. Bilateral peripheral vestibular failure (bilateral vestibulopathy): instability of gait and posture, and oscillopsia induced by head movement. 3. Paroxysmal peripheral vestibular stimulation or inhibition: attacks of vertigo and oscillopsia, e.g. in BPPV, Meniere’s disease, and vestibular paroxysmia. The patient who is having a first attack of acute spontaneous vertigo may have acute vestibular neuritis or a cerebellar infarction are commonly misdiagnosed in the casualty department as having ‘labyrinthitis’ or ‘middle-ear infection’. Acute vestibular neuritis will cause a unidirectional nystagmus pattern that improves with fixation, produces a positive head impulse test and mostly the patient will be able to stand alone, in contrast to cerebellar infarction in which they tend to fall when walking. Brainstem ischaemia symptoms such as diplopia, reduced vision, dysarthria, and dysphagia will be present in less than 50% of patients with cerebellar infarction. |Page5 It is estimated that approximately 90% of individuals over 65 years of age have visited their physician at least once with vertigo as their primary complaint. History A diagnosis can be made on: 1. History alone in 70% of patients. 2. Physical examination in 10% of patients. 3. Special tests in 20% of patients. The key history points are: 1. Is it vertigo? 2. What is the time course? 3. What are the precipitating/exacerbating factors? 4. Are there accompanying symptoms? Vertigo can be an illusion that the external world is moving relative to an individual or the individual relative to space. Rotational vertigo or other illusionary sensations of motion indicate vertigo (vestibular symptoms), whereas a sensation of light-headedness, giddiness, drowsiness, or impending fainting implies dizziness of non-vestibular origin. Non-spinning dizziness when standing or walking usually indicates a neurological gait problem rather than vestibular vertigo. Vertigo onset is usually sudden and comes in spells varying from seconds or minutes to hours. Some peripheral vertigo is brought on by a change in position and most patients will improve by lying still. Tinnitus, hearing loss, and aural fullness frequently accompany peripheral disease. Unlike peripheral vertigo, central causes of dizziness produce a more variable picture. Patients may describe it as spinning, tilting, forced to one side, light-headedness, clumsiness or blacking out. If loss of consciousness is documented, a peripheral aetiology for dizziness is rarely – if ever – the reason. The following symptoms also point to a central cause, i.e. dysarthria, dysphagia, diplopia, hemiparesis, severe localised cephalgia, seizures or memory loss. Some specific questions in the history can point to diagnosis: • Do you become dizzy just rolling over in bed? o Benign paroxysmal positional vertigo (BPPV) • Are you light sensitive during your dizzy spell? o Vestibular migraine • Does one ear feel full before or during an attack? o Meniere’s disease • Does a loud sound make you dizzy or make your world jiggle? o Superior semi-circular canal dehiscence • Did your first attack of severe vertigo last hours, with nausea and vomiting? o Vestibular neuritis • Are you light-headed when you get up from a bed or chair for a few seconds? o Blood pressure/cardiovascular disease (CVS) • Do you pass out completely with your dizziness? o CVS |Page6 Difference between peripheral and central vertigo Peripheral Definite Usually paroxysmal Usually severe Seconds to hours Frequently Present Uni-directional, increased by loss of fixation Hallucinations of movement Onset Intensity Duration Induced by head position Nystagmus Nystagmus pattern Autonomous nervous system symptoms Tinnitus Hearing loss Disturbance of consciousness Other neurological signs Definite Central Less definite Seldom paroxysmal Less severe Weeks to months Seldom Present or absent Direction changing, no change with fixation, other forms of nystagmus Less definite or absent Frequently present Frequently present Absent Usually absent Seldom present Seldom present More frequently present Frequently present Differential diagnosis of vertigo Peripheral Common BPPV • Vestibular neuritis • Meniere’s disease • Bilateral vestibulopathy • Vestibular schwannoma/acoustic neuroma Rare Superior semi-circular canal dehiscence (SSCD) • Vestibular paroxysmia (vascular loop compression) • Perilymph fistula • Labyrinthitis • Auto-immune inner-ear diseases Other problems (physiological/ pathological stimulation) Motion disease • Caloric stimulation • Water exposure • Wind exposure • Rotational stimulation • Flying • Driving • Pressure changes • Changes in specific gravity • Alcohol-induced vertigo Central Common • Phobic postural vertigo • Vestibular migraine • Pathological forms of nystagmus, e.g. • Down-beat nystagmus • Up-beat nystagmus • Gaze nystagmus Rare Central positioning vertigo • Dizziness syndromes of unclear aetiology/familial • Episodic ataxia type II • Arnold-Chiari malformation • Psychogenic dizziness CNS disease (causes) • Multiple sclerosis • Vascular disease • Tumours • Epilepsy • Infections • Medications |Page7 Is it vertigo? • Yes • Rotatory o Vestibular neuritis o BPPV o Meniere’s disease o Vestibular migraine • Sensation of boat o Bilateral vestibulopathy • No o Dizziness Duration • Seconds to minutes o BPPV o Vestibular paroxysmia • Minutes to hours o Meniere’s disease o Vestibular migraine • Hours to days o Vestibular neuritis • Varies o Fistula o SSCD Precipitating/exacerbating factors • Present in rest o Vestibular neuritis • Worse when walking o Bilateral vestibulopathy • Precipitated by turning the head to the left and right o Vestibular paroxysmia • Turning in bed to one side o BPPV • Coughing/pressing/sounds o Fistula o SSCD • Social or environmental condition o Phobic postural vertigo Accompanying symptoms • Inner ear o Tinnitus, hearing loss, aural fullness • Central nervous system o Diplopia, dysphagia, sensory disturbances, dysarthria, paralysis of arms or legs • Headache o Vestibular migraine |Page8 The sore throat Presentation of a patient with pharyngitis Viral A viral pharyngitis usually presents with mild symptoms, most patients complaining of a sore throat, dysphagia, fever and erythema of the pharyngeal mucosa with enlarged tonsils. There is normally not an exudate present, as would be seen with certain bacterial pharyngitis. Coxsackie virus causes small vesicles to form with erythematous bases that can ulcerate and spread over the anterior tonsillar pillars, palate and pharyngeal wall. Herpes simplex virus is normally associated with a ‘cold sore’. It affects older children and young adults, and may cause exudative or non-exudative pharyngitis. Epstein-Barr virus (EBV) infection is important for two characteristic clinical traits. Firstly, it can lead to very rapid enlargement of tonsils (sudden onset of snoring in patient with large dirty-gray tonsils). Petechiae at the junction of the hard and soft palate may be present. The airway obstruction may be life-threatening and should be managed promptly. Secondly, it can lead to the formation of a maculopapular rash in a large percentage of patients who are given penicillin (as high as 95%), even if no previous incidents of reactions against penicillin are documented. Influenza is readily transmitted and therefore of epidemiological importance. The sore throat associated with influenza may be distinguished from streptococcal pharyngitis by several features: The presence of influenza cases in the community (epidemic) Association with cough Myalgias. Bacterial Group A β-haemolytic Streptococcus (GABHS) is the most common cause of acute bacterial pharyngitis. Acute rheumatic fever and glomerulonephritis are part of the autoimmune-mediated group of complications due to GABHS infection and can occur after a latent period of 2 - 3 weeks. Acute rheumatic fever presents with various manifestations that may include carditis, chorea, arthritis, subcutaneous nodules and erythema marginatum. GABHS infection has a peak incidence at about 5 - 6 years of age but can occur in children younger than 3 and in adults older than 50. Acute symptoms include: dry throat, malaise, fever, odynophagia, dysphagia, otalgia, headache, body aches and pains and cervical lymphadenopathy. Examination of the mouth and pharynx may reveal a dry tongue and enlarged tonsils with yellowish white spots on the tonsils. A membrane or purulent exudates may be present over tonsils or pharynx. When symptoms that include coughing, diarrhoea, conjunctivitis and coryza are present, a viral aetiology is more likely. With other non-infective causes of pharyngitis (reflux, postnasal drip, cancer, fungal infections, cigarette smoke), the aetiology is normally identifiable and can be treated or avoided. |Page9 Approach (Algorithm) to a patient with a sore throat. The decision to treat with antimicrobials remains a difficult one despite the available special investigations, and most decisions are still made on clinical findings. This unfortunately leads to massive overtreatment of patients with antibiotics. 1. Listen to the patient – if the symptoms initially improved and then worsened, it may indicate an initial viral infection that became complicated by a secondary bacterial infection, which normally happens after 7 - 8 days. 2. GABHS remains the most prominent pathogen requiring treatment in patients of all ages, so the decision is whether or not the pharyngitis is attributable to group A streptococci. 3. Other pathogens that may require specific treatment are: EBV mononucleosis (splenic enlargement and airway obstruction) non-group A streptococci (confirmed by culture) influenza virus (high-risk patient with severe symptoms) primary HIV infection N. gonorrhoeae. Diagnosis of acute GABHS tonsillitis Most cases are diagnosed clinically, and the Centor criteria are based on clinical evaluation of symptoms and signs. It is widely used and accepted. The four criteria are: 1. 2. 3. 4. Tonsillar exudates Tender anterior cervical adenopathy (JDLN) Fever by history Absence of coughing. The presence of 3 - 4 of the criteria has a positive predictive value for GABHS of 40 - 60%. The absence of 3 - 4 of the criteria has negative predictive value of 80%. A rapid antigen test (RADT) for GABHS has been developed which has helped the decision whether or not to treat patients with antibiotics. Unfortunately even one prior dose of antibiotics may result in a negative test. It is highly specific but not as sensitive as a throat culture, which remains the gold standard, although results are delayed. Proper collection (vigorous swabbing of tonsils and posterior pharyngeal wall) and transport of the sample are keys to making a correct diagnosis. If the RADT is negative it should be followed by a throat swab for culture if streptococcal tonsillitis is strongly suspected. This, however, might lead to overtreating because it is difficult to reliably differentiate between acute and chronic infection from a throat culture. Reasons to treat GABHS: To prevent post-streptococcal sequelae − acute rheumatic fever is a significant problem in developing countries To prevent suppurative complications − peritonsillar abscess, sinusitis and | P a g e 10 retropharyngeal abscess To reduce symptoms − there is a modest (approximately one day) reduction in symptoms with early antibiotic treatment and for patients with more severe symptoms it might be two and a half days (severe symptoms ≥3 Centor criteria) To prevent transmission − while this is important in paediatrics, due to extensive exposures, it is considered far less important in adults. Management of a sore throat Symptomatic management The primary decision in these patients is whether to give antibiotics and to treat the specific underlying aetiology, e.g. reflux. If no antibiotics are given treatment is symptomatic. Basic principles remain: Rest Adequate fluid intake Antipyretics Pain management. Systemic treatment options include antimicrobial agents, pain medication and possibly anti-inflammatory agents. The use of glucocorticoids remains controversial and the benefit may be limited to infectious mononucleosis The local or topical treatment options include: Lozenges Sprays Oral rinses (gargles) Alternative medicines. Clinical and epidemiological findings and diagnosis of pharyngitis due to group A β-haemolytic streptococci (GABHS) Features suggestive of GABHS as aetiological agent A. The four criteria: 1. Patchy discrete exudate 2. Tender, enlarged anterior cervical nodes 3. Fever 4. No cough B. General constitutional S: 1. Headache, Nausea, vomiting, and abdominal pain C. Incidence: 1. Patient aged 5 - 15 years 2. Presentation in winter or early spring 3. History of exposure D. Local Symptoms: 1. Sudden onset 2. Sore throat 3. Inflammation of pharynx and tonsils . | P a g e 11 Clinical manifestations of specific organisms in acute pharyngitis Viruses Rhinovirus Coronavirus Adenovirus Influenza virus Para-influenza virus Coxsackie virus Herpes simplex virus Epstein-Barr virus Cytomegalovirus Human immunodeficiency virus Common cold Common cold Pharyngoconjunctival fever Influenza Cold, croup Herpangina, hand–foot–mouth disease Gingivostomatitis (primary infection) Infectious mononucleosis Mononucleosis-like syndrome Acute (primary) infection syndrome Bacteria Group A streptococci Group C and group G streptococci Mixed anaerobes Fusobacterium necrophorum Arcanobacterium haemolyticum Neisseria gonorrhoeae Treponema pallidum Francisella tularensis Corynebacterium diphtheria Yersinia enterocolitica Yersinia pestis Mycoplasma pneumonia Chlamydophila pneumonia chlamydophila psittaci Pharyngitis, scarlet fever Pharyngitis Vincent’s angina (ANUG) Lemierre’s syndrome (septic thrombophlebitis of the internal jugular vein) Pharyngitis, scarlatiniform rash Pharyngitis Secondary syphilis Pharyngeal tularemia Diphtheria Pharyngitis, enterocolitis Plague Bronchitis, pneumonia Bronchitis, pneumonia psittacosis | P a g e 12 Sore Throat If the patient is acutely ill? PPA, Retropharyngeal a, Epiglottitis, EBV Tonsillar hypertrophy, Diphtheria, Lemierre's No Yes Unilaterally enlarged tonsil Yes Peritonsillar abscess No Mucosal lesion Yes Systemic disease? Yes No Steven Jonson S Behcet S FB No FB Observed? Yes Herpes stomatitis Infectious pharyngitis NO Inflammation in pharynx Yes Not suggestive of GAS Pharyngitis Possible GAS Pharyngitis Irritative pharyngitis Referred pain Psychogenic If Negative Symptomatic ttt No Throat Culture If Positive If Negative RADT If Positive Antimicrobial therapy | P a g e 13 Evaluation of adenotonsillar hypertrophy Not severe, without episodes of apnea Resolves Witnessed apnea or snoring with severe obstruction Worsens Adenotonsillar hypertrophy on exam Adenotonsillar hypertrophy on exam Adenotonsillectomy Sleep Study Not Severe OSAS Observe Severe OSAS CPAP or Surgery | P a g e 14 Management of post-tonsillectomy bleeding Immediate Active Delayed Stops spontaneously Clot in fossa Control in OR Screen for Clotting defect Overnight observation in Hosp If No Further bleeding discharge Screen for Clotting defect No Active bleeding Active bleeding Control in OR Screen for Clotting defect Recurrent bleeding Consider angiogram Un-controllable bleeding ECA Ligation If patient stable: angiogram | P a g e 15 Hoarseness Onset Acute Viral & bacterial laryngitis (self-limited) Epiglottitis (high fevers, sore throat, drooling) Surgery FB ingestion Chronic Voice abuse, Smoke exposure, GE, LP reflux, Neoplasm Any patient with a significant history of smoking and drinking alcoholic beverages Who has unremitting and worsening hoarseness Accompanied by throat pain Should be considered to have laryngeal cancer until it is proven otherwise Constant: (Anatomic deficit) Benign VC (nodules, polyps) Malignant (SCC Course the improved Monday-morning voice of someone whose weekday job requires frequent voice use. larynx). Traumatic VC injury. Behavioral (functional aphonia): rarely Postnasal drip Timing Worst in the morning: GE or LP reflux Benign or malignant lesions: rough or harsh voice can result VC paresis or abductor spasmodic dysphonia: breathy or weak voice as the vocal cords fail to meet at midline Intermittent or fluctuating: Periodic voice abuse, eg. by Voice Quality Progressively worsens throughout the day: Voice abuse, Myasthenia gravis A laryngitis: whisper because of the pain & discomfort Adductor spasmodic dysphonia: tense, high-pitched voice with frequent breaks | P a g e 16 FLOW DIAGRAM FOR EPISTAXIS MANAGEMENT Active bleeding History Clinical examination: Anterior rhinoscopy Rigid/flexible nasendoscopy Assess for hypovolaemic shock Identify site of bleeding: Anterior Posterior Anteroposterior Suction and VC: 5% cocaine solution Adrenaline Phenylephrine Stop the bleeding Pinch nostrils Assess: hypovolaemic shock Resuscitat e Nasal packing Posterior packing Balloon packing Tamponade with BIPP/Vaseline Anterior packing BIPP Vaseline gauze Merocel Surgicel Remove packing Unsuccessful Repacking Nasal Cautery: Electrocautery. Chemical cautery: "Trichloracetic acid, Silver nitrate" Remove packing Idiopathic causes: Ointment Successful Re-bleeding Bleeding disorder: Refer to haematologist Identify cause Surgical intervention Arterial ligation Submucosal resection Endoscopic cautery Re-bleeding Advice No further bleeding Infective, Trauma, Druginduced, Neoplasm: Manage accordingly/ Refer to ENT surg No further treatment Embolization | P a g e 17 Neck Masses – Diagnostic approach Etiology of a neck mass is most closely linked to age: Pediatrics ~ 80 - 90% benign Adult ~ 80% neoplastic (except thyroid masses) 80% of those are malignant (except thyroid and parotid masses) Location is a key factor in developing differential diagnosis: Any new lateral neck mass in an adult > 40 years old is likely to be malignant Many upper aerodigestive tract cancers present with the chief concern of a painless neck mass Location helps guide differential dx: •Lateral neck most common site for metastatic disease from UADT - upper neck anterior/deep to SCM • Midline neck masses likely related to thyroid, elevates with swallowing Neck Masses – Differential Dx Inflammatory/infectious - Lymphadenopathy/lymphadenitis LN > 1.5 cm bacterial, viral, fungal, parasitic can become neck abscess - Infectious granulomatous disease TB, atypical mycobacteria, cat scratch - Non - infectious granulomatous disease sarcoidosis, Kawasaki, Castleman, Kikuchi, Kimura - Sialadenitis/sialolithiasis Congenital - Branchial cleft cysts very rare in adults > 40 - Laryngocele Traumatic Vascular Neoplastic - Metastatic disease usually from lesion of mucosa of upper aerodigestive tract , skin - Primary neoplasms • Lymphoma • Thyroid • Salivary gland • Neurogenic • Paraganglioma • Lipoma • Sarcoma • Other | P a g e 18 LN Levels of the Neck Level I: A: submebntal, B: submandibular Level II: Upper deep cervical Level III: Middle deep cervical Level Level VI: Anterior triangle Level V: Posterior triangle Level IV: Lower deep cervical Silent areas in head and neck Thyroid gland Nasopharynx Base of the tongue Valleculae Ventricle and saccule of the larynx Maxillary sinus Valleculae Pyriform fossa, and postcricoid area | P a g e 19 New Neck Mass Young adult (16-40) Y Pediatric <15 Y Older Adult > 40 Y Infectious Symptoms Order Imaging Order Imaging No Yes Antibiotic trial Cystic? Vascular origin (paraganglioma, Hemangioma) Yes No Resolution? No Yes Yes No Do imaging characteristics fit with congenital origin (TGDC, Branchial cyst, etc) Yes No FNA | P a g e 20