* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Case #1 - VCOMcc
Survey
Document related concepts
Transcript
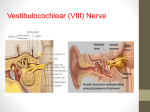
Vestibulitis, Labrynthitis, Meniere’s Disease, and Tinnitis Case Study Todd Zusmer, D.O. Clinical Medicine - EENT Case #1 Chief Complaint: Dizziness Mrs. White is a 67 yo retired psychologist who complains of a sensation of room spinning for the past 4-5 days. She denies any trauma, head injury, syncopal episode, chest pain, or new medications. She states the episodes last approximately 30 seconds to two minutes in duration during which time she feels nauseated What is your working differential diagnosis at this time? List all potential causes. Case#1 - Peripheral Causes Acute labyrinthitis Inflammation of the labyrinthine organs caused by viral or bacterial infection Acute vestibular neuronitis (vestibularneuritis) Inflammation of the vestibular nerve, usually caused by viral infection Benign positional paroxysmal vertigo (benign positionalvertigo) Transient episodes of vertigo caused by stimulation of vestibular sense organs by canalith; affects middle-age and older patients; affects twice as many women as men Cholesteatoma Cyst-like lesion filled with keratin debris, most often involving the middle ear and mastoid Herpes zoster oticus (RamsayHunt syndrome) Vesicular eruption affecting the ear; caused by reactivation of the varicella-zoster virus Ménière’s disease (Ménière’s syndrome, endolymphatic hydrops) Recurrent episodes of vertigo, hearing loss, tinnitus, or aural fullness caused by increased volume of endolymph in the semicircular canals Otosclerosis Hardening or thickening of the tympanic membrane caused by age or recurrent infections of the ear Perilymphatic fistula Breach between middle and inner ear often caused by trauma or excessive straining Case #1 – Central Causes Neoplastic Cerebellopontine angle tumor Vestibular schwannoma (i.e., acoustic neuroma) as well as infratentorial ependymoma, brainstem glioma, medulloblastoma, or neurofibromatosis Cerebrovascular disease Such as transient ischemic attack or stroke Arterial occlusion causing cerebral ischemia or infarction, especially if affecting the vertebrobasilar system Migraine Episodic headaches Usually unilateral, with throbbing accompanied by other symptoms such as nausea, vomiting, photophobia, or phonophobia; may be preceded by aura Multiple sclerosis Demyelinization of white matter in the central nervous system Other Causes Cervical vertigo Vertigo triggered by somatosensory input from head and neck movements Drug-induced Vertigo Adverse reaction to medications, Psychological Mood, anxiety, somatization Central vs. Peripheral Disease Inner ear disease (peripheral): Central “CNS” Disease: • • • • • Sudden onset of vertigo episodes Hearing loss, ear pressure, or tinnitus Lasts for seconds and is associated with position changes (suggests benign positional vertigo) Vertigo that lasts for hours or days is probably caused by Ménière disease or vestibular neuronitis • • Gradual and ill-defined symptoms are more common in CNS, cardiac, and systemic diseases. Vertigo of sudden onset that lasts for minutes can be due to vascular disease Central vertigo secondary to brainstem ischemia is often associated with other brainstem characteristics, including diplopia, autonomic symptoms, nausea, dysarthria, dysphagia, or focal weakness 5 Central vs. Peripheral Disease Inner Ear Disease: Central “CNS” Disease: • Prior viral illness, cold sores, or sensory changes in the cervical C2-C3 or trigeminal distributions usually indicate vestibular neuronitis or recurrent episodes of Ménière disease. • Patients with peripheral vertigo are usually able to ambulate during attacks and are consciously aware of their environment. • Dysdiadochokinesis and gait ataxia during episodes are more likely due to cerebellar diseases • Sensory and motor symptoms and signs are usually associated with CNS diseases • Common causes of central dizziness are migraine syndromes. Other central causes include demyelination, acoustic tumors, or cerebellar lesions. 6 Case #1 – Medical History After repeated questioning Mrs. White states she has had no headaches, vision changes, hearing loss, or tinnitus. She denies any recent illness but now seems to think the episodes occur with changes in head position. She has had no spontaneous episodes. Medical History • PMHx – She has no hx of Diabetes, hypertension, or CAD, menopause at age 52 • PSugHx – cholecystectomy, age 47 • FamHx – There is no family hx of migraines or head and neck cancer. She is a retired psychologist. – – – – • • Father deceased at age 84 of MI Mother decease at age 82 pneumonia Brother alive age 64 - HTN Sister alive age 65 - obese Meds – She again states she takes no medications other than OTC vitamin D and calcium. SocHx – married , social ETOH < 2x/month, non smoker OccHx – psychologist, retired Case #1 – Physical Examination Objective Parameters – Ht 5'2" wt 140lbs BP 124/81 P 76 reg R 16 HEENT – – E – atraumatic, normocephalic, TM’s clear with effusion or exudate, external ear canal clear E - PERRLA, EOMI, nonystagmus fundoscopic exam reveals sharp disc margins and no vessel nicking Vascular Exam – Carotid pulses are strong, equal and no bruits Neuro Exam – – Cranial Nerves – no palsies, weakness or sensorineural hearing loss is noted Gait is normal, mental status appears normal Cardio Exam – Cardiac regular rate and rhythm without rubs, clicks or murmurs Diagnostic Maneuvers – You perform a Dix- Hallpike maneuver and note the patient develops torsional upbeat and horizontal nystagmus. Could you refine your diagnosis at this time? List your most probable cause. Case #1 – Diagnosis Dx. Benign Positional Paroxysmal Vertigo • Obtain history, especially of timing and duration, provoking and aggravating factors, associated symptoms, and risk factors for cerebrovascular disease. • No Continue diagnostic work-up as appropriate for lightheadedness, presyncope, or dysequilibrium. Perform physical examination with special attention to head and neck, cardiovascular, neurologic systems, and provocative diagnostic tests such as Dix-Hallpike. • Consider brain MRI in patients with focal neurologic findings, risk factors for cerebrovascular disease, or other findings suggesting a central cause of vertigo. No Proceed as outlined right. • Consider other laboratory and radiologic studies as indicated (e.g., cervical spine series in patients with findings suggesting cervical vertigo). Considerations on Diagnosing Vertigo Patient complains of dizziness Does the patient have vertigo? Yes Is the patient taking a drug that can cause vertigo? Yes Consider stopping medication, if possible. Case #1 – Treatment You decide to treat the patient with physical therapy (Epley maneuver) and modified home Epley maneuver. This patient does not have: severe carotid stenosis, unstable heart disease, cervical spondylosis, or advanced rheumatoid arthritis which are contraindications to treatment. Older patients are at risk with use of vestibular suppressant medications (sedation, falls, and urinary retention). Now that you have made your diagnosis what signs and symptoms would prompt you to order laboratory or imaging studies? Case #1 – Additional Plans • With current diagnosis no labs or imaging are needed. • Consider labs if a an underlying illness is suspected. Considerations of underlying illness for imaging: 1. Neurologic symptoms and signs are present. 2. The patient has risks for CVA. 3. There is progressive unilateral hearing loss. Case #1 – Learning Outcomes Associated progressive hearing loss is not present in this case but can refine your diagnosis. Name causes of vertigo associated with hearing loss. Associated hearing loss is found in: • • • • • • • Ménière’s disease perilymphatic fistula acoustic neuroma cholesteatoma otosclerosis transient ischemic attack or stroke involving anterior inferior cerebellar artery herpes zoster oticus Case #1 – Follow Up Your patient returns three weeks later and has noticed improvement of symptoms with physical therapy. She denies any headaches, hearing loss, or tinnitus. What are the characteristics of peripheral vs. central vertigo? Diagnostic Characteristics Central vs. Peripheral Vertigo Peripheral Central Nystagmus Combined horizontal and torsional; inhibited by fixation of eyes onto object; fades after a few days; does not change direction with gaze to either side. Purely vertical, horizontal, or torsional; not inhibited by fixation of eyes onto object; may last weeks to months; may change direction with gaze towards fast phase of nystagmus. Imbalance Mild to moderate; able to walk. Severe; unable to stand still or walk. Nausea Vomiting; may be severe Variable Hearing Loss Common Rare Non-Auditory Neurologic Symptoms Rare Common Latency Following VertigoProvocative Diagnostic Maneuver Longer; up to 20 seconds Shorter; up to 5 seconds Case #1 – Special Considerations Specialty referral when diagnosis is unclear, if diagnosis is in doubt or indicated by findings. Medical diagnosis is made requiring specialty input.