* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Pulmonary circulation Systemic circulation
Management of acute coronary syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Jatene procedure wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Cardiac surgery wikipedia , lookup
Myocardial infarction wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
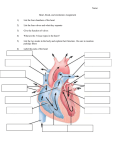
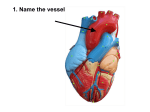
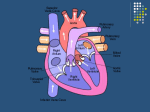
Lecture 37 Introduction to Circulation BY DR QAZI IMTIAZ RASOOL OBJECTIVES 1. Identify the two divisions of circulation and track the pathway of the blood through both circulations. 2. Outline the various parts of circulation and identify the differences in structure, function, pressure and velocity of blood in different vessels. 3. Describe the physiological anatomy of the heart and identify its various specialized functional parts. Functions of the Heart 1. Generating blood pressure 2. Routing blood: separates pulmonary and systemic circulations 3. Ensuring one-way blood flow: valves 4. Regulating blood supply 1.Changes in contraction rate and force match blood delivery to changing metabolic needs Circulatory System Function Move circulatory fluid (blood) around body 1. Gas Transport 2. Nutrient Transport 3. Excretory Product Transport 4. Cell Signal Transport 5. Distribute secretions of endocrine glands, 6. Production/Synthesis 7. Hydraulic Force 8. Heat Conductance 9. Immunity Overview of the Cardiovascular System 1. Heart- circulates blood through vessels 2. Vascular System /Blood vessels 3. 4. 5. Arteries- away from heart Veins- towards heart Capillaries- location of internal respiration, are tiny, thin-walled blood vessels that connect arteries to veins and are located in all body tissues. - in diameter that blood cells pass through in a single file. 3. Blood- transport medium Path of Blood Pulmonary Circuit Blood flow between the lungs and heart Systemic Circuit Blood flow between the rest of the body and heart Supplied by the Right side of the heart Supplied by the Left side of the heart Pulmonary circulation Systemic circulation /greater circulation / peripheral circulation. Venous return is aided by both structural modifications and functional adaptations. 1. Structural -Large lumen -Valves - present mostly in extremities, none in ventral body cavity 2. Functional -Respiratory Pump -Muscular Pump -Smooth muscle layer under sympathetic control Physiological- anatomy Structure of Blood Vessel Walls except the smallest consist of three layers: 1.Tunica intima reduces friction between the vessel walls and blood; 2. Tunica media controls vasoconstriction and vasodilation of the vessel; 3. Tunica externa protects, reinforces, and anchors the vessel to surrounding structures 1.Blood flow is the volume of blood flowing through a vessel, organ, or the entire circulation ml/min (controlled in relation to the tissue need) 2. Blood pressure is the force per unit area exerted by the blood against a vessel wall (mm Hg). (by the tension at the end of the arterioles) 3. Resistance is friction between blood and the vessel wall,. Systemic Blood Pressure Functional Anatomy of the Heart Chambers 1. 4 chambers 1. 2 Atria 2. 2 Ventricles 2. 2 systems 1. Pulmonary 2. Systemic Functional Anatomy of the Heart Cardiac Muscle 1. Characteristics 1. Striated 2. Short branched cells 3. Uninucleate 4. Intercalated discs 5. T-tubules larger and over z-discs Functional Anatomy of the Heart Valves 1. Function is to prevent backflow 1. Atrioventricular Valves 1. Prevent backflow to the atria 2. Prolapse is prevented by the chordae tendinae 1. Tensioned by the papillary muscles 2. Semilunar Valves 1. Prevent backflow into ventricles The Conduction System of the Heart 1. 2. Conduction pathways Depolarization spreads throughout the heart very rapidly facilitating a coordinated contraction pattern 3. Intercalated disks 1. Form junctions between adjacent cardiac muscle fibers 2. Contain a high concentration of gap junctions for rapid transmission of the action potential Myocardial Physiology Contractile Cells 1. 2. Plateau phase prevents summation due to the elongated refractory period No summation capacity = no tetanus (Which would be fatal) Myocardial Physiology Autorhythmic Cells (Pacemaker Cells) 1. Altering Activity of Pacemaker Cells 1. Sympathetic activity 1. NE and E increase If channel activity 1. 2. Binds to β1 adrenergic receptors which activate cAMP and increase If channel open time Causes more rapid pacemaker potential and faster rate of action potentials Sympathetic Activity Summary: increased chronotropic effects heart rate increased dromotropic effects conduction of APs increased inotropic effects contractility Myocardial Physiology Autorhythmic Cells (Pacemaker Cells) 1. Altering Activity of Pacemaker Cells 1. Parasympathetic activity 1. ACh binds to muscarinic receptors 1. Increases K+ permeability and decreases Ca2+ permeability = hyperpolarizing the membrane 1. Longer time to threshold = slower rate of action potentials Parasympathetic Activity Summary: decreased chronotropic effects heart rate decreased dromotropic effects conduction of APs decreased inotropic effects contractility Aging and the CVS Changes occur in the blood, heart, and BVs 1. Blood changes – HCT; thrombi and emboli form more easily; blood pools in leg 2. Heart changes – efficiency and elasticity; atherosclerosis of coronary vessels; scar tissue forms 3. Blood vessel changes – loss of elasticity; calcium deposits damage vessel walls 4. Gradual changes in heart function, minor under resting condition, more significant during exercise 5. Hypertrophy of L ventricle 6. Maximum heart rate decreases 7. tendency for valves to function abnormally and arrhythmias to occur 8. O2 consumption required to pump same amount of blood