* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download PAIN FOX FINAL
Drug discovery wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Drug design wikipedia , lookup
Prescription costs wikipedia , lookup
Drug interaction wikipedia , lookup
Pharmacokinetics wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
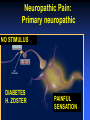
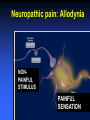
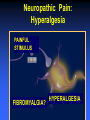
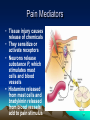
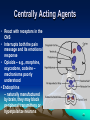
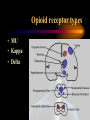
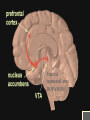
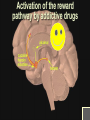
ANALGESIC PHARMACOLOGY Bruce Onofrey, OD, RPh, FAAO Professor, U. Houston 1 DISCLOSURE • I’m a suffering CUBS fan POSTER FROM 1923 A CLINICAL MOMENT: 80 y/o with severe temporal headache presents to ER ER DX:Migraine TX with Midrin Classical Migraine Symptoms? What IS the Differential? NOT the Rear-end of An Automobile • Do the facts support the DX? • What is the Differential DX? • Will this TX produce harm? • Any additional tests? The Differential • Cranial Arteritis • Arteritic Ischemic Optic Neuropathy • Temporal Arteritis • Carotid Artery Disease • Hypertensive Crisis • Impending CVA The Tests • • • • • • BP ESR CRP CBC ESR >47 CRP > 2.45 Pain is NOT a disease-It is a sign of a disorder that must be diagnosed in conjunction with the management of the pain. What is Pain? • Any unpleasant sensory and emotional experience associated with actual or potential tissue damage. • 75 million suffer from chronic pain • 1/3- 1/2 require daily pain management Pain Management • Acute — injury, inflammation (most ocular pain) • Chronic • Neuropathic — from diseases of the nerves or from injury to nerves • Cancer — pain related to malignant disease or tumors and their effects on the body 9 Neuropathic Pain: Primary neuropathic NO STIMULUS DIABETES H. ZOSTER PAINFUL SENSATION Neuropathic pain: Allodynia NONPAINFUL STIMULUS PAINFUL SENSATION Neuropathic Pain: Hyperalgesia PAINFUL STIMULUS FIBROMYALGIA? HYPERALGESIA Acute Pain • ~ specific and obvious cause (e.g. trauma, surgery)-ALWAYS FIND CAUSE • ~ limited duration • Resolves when the source of pain is detected and treated • ~ requires topical/local treatment – Fewer side effects/complications 13 Physiologic Effects of Pain • • • • Tachycardia Systemic hypertension Tachypnea Can exacerbate pre-existing cardiovascular disease 14 Psychological Effects of Pain • Poor sleep patterns • Anxiety • Uncooperativeness 15 Need for Pain • Short latency - warn the organism that it is in danger so it will alter the situation (e.g.,withdraw limb, take flight, respond with defensive maneuver). • Long latency - immobilize the organism so that recovery from injury can occur. 16 Pain Mediators • Tissue injury causes release of chemicals • They sensitize or activate receptors • Neurons release substance P, which stimulates mast cells and blood vessels • Histamine released from mast cells and bradykinin released from blood vessels add to pain stimulus 17 • Pain mechanisms are Why?? complex Why do I Have Pain? • Peripheral VS Central Pain • Direct nerve stimulation-Drop hammer on toe • Inflammatory painProstaglandins • Tissue damage-Via infection or trauma Indications • Abrasions • Lacerations • Thermal and Chemical injury • Dacryocystitis • Bacterial corneal ulcers • Cryo therapy • Micropuncture Corneal Erosion Infection Hurts Watch Out for those Air Bags • Blunt trauma to cornea produces a concussive trauma • Abrasive surface can denude the epithelium completely • Temporary to permanent stromal edema and hazing-decompensation due to endothelial shock • Often an associated uveitis/hyphema and other forms of blunt ocular traumatic injuries Pain Management The Drugs • Peripheral agents: NSAID’s • Acetaminophen? • Central Agents: Opiates 23 Peripherally Acting Agents • Prevent sensitization and discharge of the nociceptors • NSAIDs (including ASA) – Block the formation of inflammatory and pain mediatory (e.g. prostaglandins) at the cyclooxygenase pathway 24 THE INFLAMMATORY CASCADE Cellular phospholipid membrane ARACHIDONIC ACID CYCLOOXYGENASE LIPOXYGENASE PROSTAGLANDINS LEUKOTRIENES • COX: • COX-1: constitutive enzyme: is involved in tissue homeostasis. • COX-2: inducible enzyme: is responsible for the production of the prostanoid mediators of inflammation. Classification selection chemcial constitution Non-selective COX inhibitor Selective COX inhibitor Salicylates Acetaminophen Indomethacin et al NSAID’s: THE CYCLOOXYGENASE BLOCKERS Salicylates • Block cyclooxygenase • Analgesic vs Antiinflammatory dose • Acetylated vs non-acetylated Acetylated VS Non-acteylated Salicylates Non-acetylated developed to reduce: • GI bleeding • GI Upset Acetylated: ASA: Aspirin • Irreversible block of platelets • Best for use as an anti-coagulant • None are safe in potential bleeders THE SECOND GENERATION NSAID’s • • • • • Less bleeding potential Less GI Upset Greater efficacy Greater potency All second generation drugs have the same efficacy in EQUIVALENT DOSAGES AND THE SAME SIDEEFFECTS EQUIVALENT DOSAGES • 3200mg of ibuprofen = (800mg QID) • 20mg of Feldene = (20mg/D) • 750mg of Naprosyn per day (375mg BID) • Only differ in 1/2 life = Dosing frequency • Only differ in dosage = Potency NSAID SIDE-EFFECTS • Inhibit platelets: Only ASA is irreversible • Allergic to one, allergic to all • Avoid in asthmatics and those with nasal polyps-Increased incidence of allergy • Watch out for protein binding in Type II diabetics@@@@ • Renal insufficiency: ALL DIABETICS AT RISK • CHF NSAID SIDE-EFFECTS • Kids with fever: Avoid ASA • Avoid pregnant or nursing mothers • Those with GI problems New NSAIDS • • • • • • New COX-2 inhibitors for acute pain Vioxx , hopefully not the patient, is dead Celebrex 200mg/D max dose Celebrex is a sulfonamide Look close-they will soon be gone Don’t prescribe them GONE Ibuprofen-The Best of the NSAID’s • Cheap • Flexible dosage Schedule The Ophthalmic NSAID’s Use of topical NSAID’s for acute pain other than cataract surgery is: OFF-LABEL Diclofenac 0.1% (VoltarenCiba) • Generic associated with corneal melting (never able to prove association) • Pain and inflammation associated with cataract surgery • Dosage: QID Flubiprofen 0.03% (Ocufen-Allergan) • ONLY INDICATION-Interoperative miosis • 1 drop Q 30min X 4 total 2 hours prior to surgery Ketorolac 0.5% and 0.4% (Acular, Acular PF, Acular LS-Allergan) • • • • Really know how to extend a patent Only NSAID indicated for ocular allergy Marked stinging Dosage: QID Brofenac 0.09%(Bromday – B and L) • First “once daily” post-op cataract treatment Nepafenac 0.1% (NevanacAlcon) • Only “Pro-drug” NSAID • Not available as generic • Dosage TID Analgesic Pharmacology • Tylenol/Acetaminophen/(N-Acetyl-Paminophenol)/APAP • Unknown central mechanism • Anti-pyretic: Hypothalmus • No anti-inflammatory effect@@@@ • No inhibition of platelets@@@@ Acetaminophen is a Safe Drug? Drug of Choice (DOC) in: • Children • Viral induced fever • Pregnancy@@@@ • Nursing mothers • No GI distress • No Increase in Bleeding?@@@@ If They Like to Drink, Think Twice About Acetaminophen • Acetaminophen associated with liver failure in alcoholics (>3 drinks/d) • Liver failure = decreased drug metabolism = overdose • Reduced vitamin K clotting factors = increased bleeding • Max adult dose = 4gm/D = 8 extrastrength Tylenol per 24 hours (2.6gms?) • 5% of metabolites hepatotoxic APAP Liver Metabolism 1. Major pathway —Majority of drug is metabolized to produce a non-toxic metabolite 2. Minor pathway —Produces a highly reactive intermediate (acetylimidoquinone) that conjugates with glutathione and is inactivated. • At toxic APAP levels, minor pathway metabolism cannot keep up (liver’s supply of glutathione is limited), causing an increase in the reactive intermediate which leads to hepatic toxicity and necrosis Acetaminophen toxicity Centrally Acting Agents • React with receptors in the CNS • Interrupts both the pain message and its emotional response • Opioids – e.g., morphine, oxycodone, codeine – mechanisms poorly understood • Endorphins – naturally manufactured by brain, they may block peripheral transmitters or hyperpolarize neurons 49 OOOHHH, That’s GOT to Hurt!! Opioid receptor types • MU • Kappa • Delta Ventral tegmental area DOPAMINE movement Dopam motivation ine addiction Reward & well-being Most strongly binds morphine Best bet for a safe analgesic Receptor Location type Effects μ Brain, spinal cord Analgesia, Respiratory depression, euphoria, addiction, ALL pain messages blocked κ Brain, spinal cord Analgesia, sedation, all nonthermal pain messages blocked δ Brain Analgesia, antidepression, dependence MU Opioid receptors • • • • Classic morphine receptor Located in brain and spinal cord Stimulated by endogenous endorphins Binding of drug to these receptors produces analgesia/sedation/decreased BP/itching/nausea/euphoria/decreased respiration/ • Effects decline as drug tolerance develops • Narcotic antagonists block these receptors Why you feel “happy” Kappa Opioid receptors • Novel receptors • Stimulation relieves pain, but produces nausea and sweating (dysphoria) • Endogenous transmitters are dynorphins • Located in the periphery by pain neurons • Not associated with euphoria response Delta Opioid receptors • Stimulated by endogenous enkephalins • Produces “ischemic preconditioning” • Stimulation induced protective increase in blood flow to tissues surrounding an ischemic area • May have cardioprotective effect Opiate Analgesics • Block central pain receptors, reduce perception of pain-They feel pain, but don’t care • Inhibits descending pain pathways • Allergic to one opiate, allergic to all opiates • Know your schedules • Schedule II, high abuse, V= low abuse • Know your side-effects/autonomics Side-effects • Respiration-sleep apnea/COPD • Urinary tract/the big prostate/incontinance TX • GI Tract: The food stops here • Interaction with other anticholinergics/ • DRY/DROWSINESS/GLC Is Constipation a Side-effect or Indication-Depends on your point of view INDICATION SIDE-EFFECT Tolerance and Dependence Tolerance • Tolerance is a diminished responsiveness to the drug’s action that is seen with many compounds • Tolerance can be demonstrated by a decreased effect from a constant dose of drug or by an increase in the minimum drug dose required to produce a given level of effect • Physiological tolerance involves changes in the binding of a drug to receptors or changes in receptor transductional processes related to the drug of action • This type of tolerance occurs in opioids Dependence • Physiological dependence occurs when the drug is necessary for normal physiological functioning – this is demonstrated by the withdrawl reactions • Withdrawl reactions are usually the opposite of the physiological effects produced by the drug Withdrawl Reactions Acute Action • • • • • • • • • • • • Analgesia Respiratory Depression Euphoria Relaxation and sleep Tranquilization Decreased blood pressure Constipation Pupillary constriction Hypothermia Drying of secretions Reduced sex drive Flushed and warm skin Withdrawl Sign • • • • • • • • • • • • Pain and irritability Hyperventilation Dysphoria and depression Restlessness and insomnia Fearfulness and hostility Increased blood pressure Diarrhea Pupillary dilation Hyperthermia Lacrimation, runny nose Spontaneous ejaculation Chilliness and “gooseflesh” COMBINATION OPIATE ANALGESICS • • • • • • Propoxyphene + Propoxyphene + Codeine + Hydrocodone + Oxycodone + Oxycodone + • • • • • • ASA = Darvon cmpd APAP = Darvocett Tylenol 1,2,3,4 APAP = Vicodin ASA = Percodan APAP = Percocett PROPOXYPHENE = DARVON • • • • Relatively poor analgesia Lots of sedation Neurological side-effects Use if you want them to sleep a lot • Darvocett N 50 and 100 are the best of group = propoxypene napsylate with acetaminophen Which Tylenol with Codeine Should You Use? All contain 5 grains of APAP (325mg) WITH: • Tylenol #4 = 1 grain (60mg) codeine • Tylenol #3 = 1/2 grain (30mg) codeine@@@@ • Tylenol #2 = 1/4 grain (15mg) codeine • Tylenol #1 = 1/8 grain 7.5mg) codeine A CLINICAL MOMENT 36 Y/O construction worker suffers an orbital blow-out fracture, complains about severe pain, requests pain reliever Write him a prescription for acetaminophen with codeine-give him the maximum pain relieving dosage of the drug John Doe 7/20/00 100 Low Life Ln. Acetaminophen with Codeine #3 #20 (Twenty) SIG: i-ii tabs q 4-6H prn pain Refills: Zero B. Onofrey MO 0182597 ALWAYS PRESCRIBE FROM THE BIG BOTTLE Oxycodone, The “BIG GUN” • With ASA = Percodan • With APAP = Percocett • Schedule II drug = High abuse • Better alternative with a schedule III drug 5MG/300MG That all fine and good butttt: • • • • • • My Patients a drug abuser My Patient’s allergic to opiates I CAN’T prescribe Narcotic agents I don’t want to prescribe narcotic agents My patient doesn’t want to use dope @@@@@@@@ + Ibuprofen/acetaminophen • • • • • • Incredible synergism@@@@@@ Non-narcotic drugs Non RX drugs Inexpensive Monitor for sensitivity to either drug No motrin in pregnancy/with blood thinners/GI problems/renal disease/CHF Ibuprofen/Acetaminophen Indication/dosage forms • • • • Indications: Mild to severe pain Dosage forms 400-600mg motrin with 500-1000mg acetaminophen (Do not exceed 4 gms acetaminophen/day) • No acetaminophen for persons that regularly consume daily alcohol A Potential Dis-zoster Trigeminal N.-The 5th Cranial N The three divisions of the trigeminal nerve come together in an area called the Gasserion ganglion. From there, the trigeminal nerve root continues back towards the side of the brain stem, and inserts into the pons. Within the brain stem, the signals traveling through the trigeminal nerve reach specialized clusters of neurons called the trigeminal nerve nucleus. Information brought to the brain stem by the trigeminal nerve is then processed before being sent up to the brain and cerebral cortex, where a conscious perception of facial sensation is generated. Who gets Post-herpetic Neuralgia • Immunocompromised folk • The elderly • Best treatment is prophylactic TX Prevention is Critical • Acyclovir • Famcyclovir • Valcyclovir Manage Potential Post-herpetic Neuralgia • • • • • Oral acyclovir 800mg 5X daily Valacyclovir 1000mg TID Famcyclovir 500mg TID Zostrix creme 3-4 times daily Low dose tricyclic antidepressantamitryptyline 25mg/day Anti-depressant for pain relief? • Very good neural pain relief • “GOOD” anticholinergic side-effects Neurontin: The New “Big Dog” for chronic pain • Huge dosage range: 100-5000mg/d • Must start slow • Must give enough Seratonin (5HT Agonists) • The “triptan drugs” • Sulfonamides-beware of allergy\Beware of heart disease • Prevent BV Spasm (Vasoconstrictive effect) • Inhibit trigeminal nerve THE HEADACHE PILLSNEVER USE THEM • HA is a DX of exclusion • Don’t cover-up undiagnosed pain • We must exclude other causes, but WE don’t make the final DX • Let PCP or neurologist manage pain AFTER final DX made