* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Opioid Overdose Costs - Michigan State University College of Nursing
Survey
Document related concepts
Pharmacognosy wikipedia , lookup
Neuropharmacology wikipedia , lookup
Drug design wikipedia , lookup
Drug discovery wikipedia , lookup
Drug interaction wikipedia , lookup
Electronic prescribing wikipedia , lookup
Theralizumab wikipedia , lookup
Dextropropoxyphene wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Pharmacokinetics wikipedia , lookup
Prescription costs wikipedia , lookup
Prescription drug prices in the United States wikipedia , lookup
Transcript
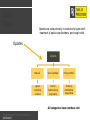
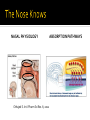
Deb Wagner, PharmD, FASHP Associate Professor Pharmacy/Anesthesiology October 2015 Review the background on the current opioid crisis Describe the recent interest in the use of prehospital naloxone for suspected opioid overdoses Identify risks and benefits associated with it’s use Identify it’s current role in practice WHO Library Cataloguing-in-Publication Data Community management of opioid overdose. 010 Deaths per 100,000 population 18 Motor vehicle traffic Poisoning 16 14 12 Drug poisoning Unintentional drug poisoning 10 8 6 4 2 0 1999 2000 2001 2002 2003 2004 2005 2006 2007 2008 2009 2010 NOTES: Drug poisoning deaths are a subset of poisoning deaths. Unintentional drug poisoning deaths are a subset of drug poisoning deaths. SOURCE: CDC/NCHS, National Vital Statistics System; and Warner M, Chen LH, Makuc DM, Anderson RN, Miniño AM. Drug poisoning deaths in the United States, 1980–2008. NCHS data brief, no 81. Hyattsville, MD: National Center for Health Statistics. 2011. http://www.cdc.gov/nchs/data/databriefs/db81.htm. Intercensal populations http://www.cdc.gov/nchs/nvss/bridged_race/data_documentation.htm Steady rise in drug overdose deaths since 1992 117% increase from 1999 to 2012 In the United States (US), 100 people die every day from opioid overdose >16,000 people died from an overdose of prescription opioids in US in 2013 NOTE: Access data table for Figure 3 at: http://www.cdc.gov/nchs/data/databriefs/db166_table.pdf#3.SOURCE: CDC/NCHS, National Vital Statistics System, Mortality File. NOTE: Access data table for Figure 3 at: http://www.cdc.gov/nchs/data/databriefs/db166_table.pdf#3.SOURCE: CDC/NCHS, National Vital Statistics System, Mortality File. JAMA. 2008;300(22):2613-2620. doi:10.1001/jama.2008.802 Data from Michigan Department of Community Health Approximately 2% of heroin users die each year ½-2/3 of heroin users experience at least one nonfatal overdose 80% have observed an overdose Sporer BMJ 2003, Coffin Acad Emerg Med 2007 People coming out of jail or treatment have highest risk of overdose Most deaths are among opiate users who are in their late twenties to early thirties and have been actively using for the past five to ten years Only 17 % of opiate related deaths are among new users. New Drug Use Patterns New Initiates to prescription drugs Vicodin/Percocet/oxycodone >>> heroin Heroin Availability/Purity/Lethal Mixture Heroin is the leading drug threat in New England From ‘93-’10 Heroin reported as primary drug increased from 20% - 40% of treatment admissions in MA Combination with Fentanyl Prescribing Patterns Schedule II Opioid prescriptions increased more than 4 fold from 1999- 2010 Male gender Older age Lower socioeconomic status Mental health disorders Higher doses ≥ 100mg morphine equivalents daily Polypharmacy JAMA. 2008;300(22):2613-2620. doi:10.1001/jama.2008.802 Knowlton A. Prehospital Emergency Care. 17; 2013 Knowlton A. Prehospital Emergency Care. 17; 2013 Knowlton A. Prehospital Emergency Care. 17; 2013 $20.4 billion per year in 2009 $2.2 billion direct costs ▪ inpatient, ED, MDs, ambulance $18.2 billion indirect costs ▪ lost productivity from absenteeism and mortality $37,274 cost per opioid overdose event Inocencio TJ et al. Pain Medicine 2013 Inocencio. Pain Med. 14; 2013 One heroin overdose death prevented for every 164 kits distributed Cost for naloxone distribution would range between: $438-$14,000 (best-worst case scenario) for every qualityadjusted life year gained Generally accepted threshold is $50,000/year For dialysis: recently calculated as $129,000 ▪ Lee et al. Value Health 2009;12(1): 80-7. For primary care-based SBIRT: recently calculated as $6960 ▪ Tariq et al. PLoS One 2009;4(5) Coffin and Sullivan. Ann Intern Med. 2013; 158: 1-9. Inocencio TJ. Pain Med. 14; 2013 WHO PAYS? All 53 jurisdictions permit Paramedics to administer naloxone Of the 48 jurisdictions with mid-level EMS personnel, all but one authorize those personnel to administer naloxone Only twelve jurisdictions explicitly permit EMTs to administer naloxone Five additional states permit some or all EMTs to administer the drug through pilot programs or agency medical director authority Davis, Walley, Dailey, Southwell, Neihaus, “EMS Naloxone Access: A National Systematic Legal Review”, Academic EM, August 2014 Opioids are used primarily in medicine for pain relief, treatment of opioid use disorders, and cough relief. Opiates Opioids Natural Semi-synthetic Fully synthetic opium morphine codeine heroin hydrocodone oxycodone fentanyl methadone meperidine All categories have overdose risk Weak/Thready pulse Slow or Absent Respirations Constricted Pupils Weakness Unresponsiveness MOA: Competitively displaces opioids from receptors Half-life: ~ 30 min-1 hour Complete, temporary reversal of opioid overdose effects May cause acute and severe opioid withdrawal Inactivated by first pass metabolism Grassin-Delyle S. Pharmacol Therap. 134; 2012 NASAL PHYSIOLOGY Chhajed S. Int J Pharm Sci Res. 6; 2012 ABSORPTION PATHWAYS NOSE TO BRAIN TRANSPORT PLASMA VS CSF CONCENTRATIONS NI IV Illum L. Eur J Pharm Sci. 11; 2000 The more lipophilic the better Smaller is better Volume is important Increase nasal residual time Enhance nasal absorption Modify drug to change the physiochemical properties Product Route of Administration Available Strengths Dosing Advantage Price per Dose* (7/2015) FDA Status Autoinjector IM 0.4mg/ml 0.4mg No training required Easy to use No assembly Decreased risk of needle stick $345 Yes Multi-use Vial IM, IV, SC 0.4mg/ml 0.4mg Multiple doses $11.84 Yes Single Dose Vial IM, IV, SC 0.4mg/ml 0.4mg Individual dose $18.99 Yes Prefilled Syringe Intranasal 1mg/ml 1mg Easy to use Decreased risk of needle stick $19.80 Yes Robertson TM. Prehospital Emergency Care 13; 2009 LEVEL OF CONSCIOUSNESS RESPONSE COMPARISON NS Sabzghabaee AM. Arch Med Sci 10; 2014 Kelly A. MJA. 182; 2005 0.15mg/kg Morphine 0.4mg Naloxone Dahan A Anesthesiology. 2010;112 Dahan A. Anesthesiology. 2010; 112 First case in 1977 Occurs with doses as low as 80mcg IV Onset within 1-60 minutes Majority in healthy men < 50 yo Congeni A. Em-News.com. July 2015 Increases catecholamine release especially in the presence of hypercapnoea The correction of of hypercapnoea reduces haemodynamic effects. ▪ Mills CA (1988) There is no clinical evidence to support hypercapnoea correction prior to administration of naloxone. Mills CA. Anesth Anal. 1988 Mills CA. Anesth Anal. 1988 The Solution • A multi-faceted approach to overdose prevention is required. PREVENTION & E D U C AT I O N MONITORING & DIVERSION CONTROL INTERVENTION & T R E AT M E N T Prescription monitoring programs ▪ Paulozzi et al. Pain Medicine 2011 Prescription drug take back events Safe disposal Safe opioid prescribing education ▪ Albert et al. Pain Medicine 2011; 12: S77-S85 Expansion of opioid agonist treatment ▪ Clausen et al. Addiction 2009:104;1356-62 Safe injection facilities ▪ Marshall et al. Lancet 2011:377;1429-37 Feasibility ▪ ▪ ▪ ▪ ▪ Piper et al. Subst Use Misuse 2008: 43; 858-70 Doe-Simkins et al. Am J Public Health 2009: 99: 788-791 Enteen et al. J Urban Health 2010:87: 931-41 Bennett et al. J Urban Health. 2011: 88; 1020-30 Walley et al. JSAT 2013; 44:241-7 (Methadone and detox programs) Increased knowledge and skills ▪ Green et al. Addiction 2008: 103;979-89 ▪ Tobin et al. Int J Drug Policy 2009: 20; 131-6 ▪ Wagner et al. Int J Drug Policy 2010: 21: 186-93 No increase in use, increase in drug treatment ▪ Seal et al. J Urban Health 2005:82:303-11 Reduction in overdose in communities ▪ Maxwell et al. J Addict Dis 2006:25; 89-96 ▪ Evans et al. Am J Epidemiol 2012; 174: 302-8 ▪ Walley et al. BMJ 2013; 346: f174 TO 1999-2004 Largest increase in drug overdose mortality rates 295 unintentional deaths from pharmaceutical overdose 93% from opioids 90% were men age 18-70 yo 63% were associated with drug diversion 21% due to doctor shopping Substance abuse indicators present in 95% Cobaugh DJ. AJHP. 71; 2014 Enrollments 16,379 individuals >10 per day • • • • • • • • • • • • • • • AIDS Action Committee AIDS Project Worcester AIDS Support Group of Cape Cod Brockton Area Multi-Services Inc. (BAMSI) Bay State Community Services Boston Public Health Commission Greater Lawrence Family Health Center Holyoke Health Center Learn to Cope Lowell House/ Lowell Community Health Center Manet Community Health Center Northeast Behavioral Health Seven Hills Behavioral Health Tapestry Health SPHERE • Rescues – 1,741 reported – >1 per day Witnessed overdose ever Lifetime history of overdose Received naloxone ever Inpatient detox, past year Incarcerated, past year Reported at least one overdose rescue User n=11,002 75% 49% 41% 64% 28% Non-User n=5,377 42% 7.5% 2.0% Program data N=1,741 Deaths 7 / 1729 0.4% OD requiring 3 or more doses 72 / 1604 4% Recurrent overdose 3/1741 0.2% Withdrawal symptoms after naloxone 107/219 49% Difficulty with device 11/1741 0.6% Negative interactions with public safety 114/ 466 24% 205 / 5271 4% Confiscations Program data NALOXONE COVERAGE PER 100K 250 OPIOID OVERDOSE DEATH RATE 100% 90% 200 80% 70% 150 60% 50% 100 50 40% No coverage 30% 1-100 ppl 20% 10% 0 27% reduction 46% reduction 100+ ppl 0% Walley et al. BMJ 2013; 346: f174. Prescription and prescriber typically required Naloxone cost is increasing, funding is minimal Missing people who don’t identify as drug users, but have high risk CBOs target IDU, people w/ substance use disorders, HIV prevention • Co-prescribe naloxone with opioids for pain • Co-prescribe with methadone/ buprenorphine for addiction • Insurance should fund this • Increase patient, provider & pharmacist awareness • Universalize overdose risk Opioid overdose is a public health crisis Naloxone is a safe and effective opioid reversal agent Multiple routes of administration are available Diversion and prescribing of opioids must be addressed