* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Case Study in Neuropathic Pain
Survey
Document related concepts
Transcript
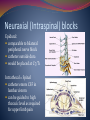
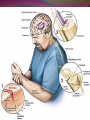
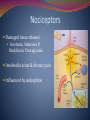
June 3, 2009 Palliative Care Team Drs. St. Godard, Loiselle, Hohl and Pilkey Objectives By the end of the hour the learner will be able to: Define neuropathic pain List at least 2 types of Pain receptors List at least 4 different types of adjuvant pain medications List the mechanisms of action, benefits, and side-effects of these 4 medications List 2 new/different adjuvant pain medications Talk Outline Case Study – Dr. Ted St. Godard & Dr. Joel Loiselle Pathophysiology of Neuropathic Pain – Dr. Jana Pilkey Adjuvant Medications – Dr. Chris Hohl What’s new/different in Neuropathic Pain – Dr. Jana Pilkey History Ms. G. D. 55 y.o with breast cancer Mets to bone Pain to left arm History 2 week hx of worsening pain Mid back – dull ache, Pressure Burning to L hand and arm Since 1997 brachial plexus neuropathy “Pins and needles” “Like dipped in acid” Morphine for 4 weeks not helping Cancer History Breast cancer dx 1997 Lumpectomy, tamoxifen x 2 yrs Mastectomy 1999 and LN dissection Oophorectomy 1999 Multiple courses of chemo 2008- mets to c-spine, ribs, sternum. Sept 2008 – Rx to spine Phx: PUD Physical Exam & Investigations Temp 37.2 Hr 100 Rr 18 Sao2 – 90% on RA BP 150/88 Lab work normal throughout Course in Hospital Admission orders: Methadone 5mg bid Dex 10mg bid Pariet 20mg po od Dilaudid 8 mg subcut q4h and q1prn Fentanyl 50 per IPP Course in Hospital Dec 30 Myoclonus noticed – hydrated Rotated to fentanyl patch Methadone increased Jan 14 CT head – mets to R cerebellum and R frontal lobe Pain better- on methadone 40 bid, dex 8 bid Starts 12 rdtx to whole brain Course in Hospital Jan 27 Pain Crisis Severe excruciating burning pain From neck to top of R shoulder Crying, screaming BT HM ineffective Slept with 5mg versed Methadone increased Ketamine added 2.5 mg subcut tid Pregabalin added 50mg bid Lidocaine 2% gel to shoulder qid prn Potentially useful Peripheral Nerve Block in this Case Interscalene block -Performed at root level -“Single shot” -only lasts 12 h. -Catheter techniques difficult to maintain (displacement). -Disease extent limits anesthetic flow. -Risk of bleeding /epidural hematoma is prohibitive in this case. Neuraxial (Intraspinal) blocks Epidural: comparable to bilateral peripheral nerve block catheter outside dura would be placed at C7/T1 Intrathecal = Spinal catheter enters CSF in lumbar cistern can be guided to high thoracic level as required for upper limb pain Contraindications to Neuraxial Analgesia in this Case - Extent of Disease involving C-spine: - Risk of epidural hematoma if needle at C7-T1. - Poor CSF flow impedes spread of analgesics - Brain Metastasis: - Posterior Fossa- increased risk of “coning” - Relative contraindication Remember coagulopathy (Plt <100; INR >1.3) and need for ongoing anticoagulation are contraindications. Course in Hospital Consult to Dr J. Loiselle Nerve-block or epidural too risky given fragility of spine and cerebellar mets Jan 28 Pain continues On Methadone 60mg bid Starts fentanyl 50mcg/hr IV HM stopped – twitching Ketamine 5 mg subcut tid Course in Hospital Jan 28 Family concerned about sedation on fentanyl Jan 29 RR 7 - fentanyl stopped, Pain again severe Fentanyl IV not restarted at family request Ativan started Jan 30 – Mini Case conference Ketamine IV @ 2.5mg/hr Gabapentin being lowered Course in Hospital Jan 31-Feb 5 – good pain control Feb 6 – weepy and tired, pain with movement Feb 9 – increase in ketamine IV 3.52mg/hr Feb 13 – increase in ketamine IV 6mg/hr Feb 17 – decrease po intake – deteriorating – ketamine 7.5mg/hr Course in Hospital Feb 19 – pt wishes she could sleep until death – tired of trying to “hold the pain in” Feb 23 – unresponsive Feb 26 – prognosis hrs to days/ discussed sedation Feb 28 – difficulty maintaining sedation Mar 4 – died sedated and comfortable What is Neuropathic Pain? Pain initiated or caused by a primary lesion or dysfunction in the nervous system Characterized by : Burning, Tingling, Electric ,Shooting Pain Pain Receptors A delta Mechanical sensation eg. Cut, prick C fibres Diffuse, respond to many stimuli Burning sensation Sleeping receptors Active in injured tissue only Acquire mechanical sensitivity (Almeida 2004) Nociceptors Damaged tissue releases: Serotonin, Substance P, Bradykinin, Prostaglandin Involved in acute & chronic pain Influenced by endorphins Sensitization Can be a tissue level (primary) or At CNS level (secondary) Results in: threshold of activation after injury intensity of a response to a noxious stimulus emergence of spontaneous activity (Aguggia 2003) Sensitization Primary sensitization Sympathetic activity and Inflammatory Mediators (Chong 2003) Secondary sensitization CNS changes in spinal cord and brain NMDA receptors activated “Wind-up” = increased amplitude and frequency summation in neurons after prolonged stimulation (Chong 2003) Blocked by NMDA antagonists, anti-inflammatories (McHugh 2000) The Dorsal Root Ganglion Tricyclic Antidepressants (TCAs) 40-60% efficacy for partial relief (NNT~2.5-3) Start 10-25 mg/d and 10-25mg each week Best effects: 50-150 mg/day Mechanism: NE & 5HT reuptake blockade +/- NMDA antagonism, +/- Na channel blockade Anticholinergic effects Secondary amine better tolerated Selective Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs) Duloxetine Venlafaxine NNT ~4-5 (~7 for SSRI) Start 37.5 mg/day Start & efficacious @ 60mg/day Increase by 37.5 mg weekly Effective @ 150-225 mg/d Antidepressant & anxiolytic Favorable side effect profile Limited long term data Lower doses – results inconsistent Short vs XR preps ά2-δ Ligands (Gabapentinoids) Bind to ά2-δ subunit of voltage gated Ca channels glutamate, NE, substance P release NNT ~3.5-4.5 Gabapentin Pregabalin No drug interactions Similar side effects to gaba Start 50-150mg divided Q8-12H Few drug interactions Dizziness & sleepiness Exacerbate cognitive impairment Start 100-300mg TID Titrate to 1800-3600 mg/d Peak effect in >2 weeks Titrate 50-150mg/day weekly Goal 300-600 mg/d in 1-2 weeks Peak effect in 2 weeks Opioids 20-30% pain reduction, NNT ~2.5 Provides rapid relief Rapid titration No ceiling effect Multiple forms & delivery methods More side effects than 1st line treatments Risk of misuse and abuse (5%) Methadone μ-receptor agonist + NMDA antagonist Very long half-life, variable in individuals Slow titration: start 2.5mg TID Increase 50-100% every 48-72 hours ~5:1 to ~30:1 morphine equivalency (depending on dose) Little literature support, ++ practical support NMDA Antagonists Ketamine Start 2.5-5mg PO TID Titrate by 50-100% dose to 1-2 mg/kg/day Start IV infusion @ 0.05-0.1mg/kg/hr IV bolus @ 0.1-0.2 mg/kg/dose over 20 minutes No NNT data Poor performance in studies, good efficacy in practice Topical or gargle preparations possible *opioid sparing effects Other/New Things to Try IV Lidocaine And po Mexilitine Cochrane Review 2005 Good quality evidence in neuropathic pain Both decrease VAS by 11 on 1-100 scale 47% of people in trials had a 30% decrease in pain (22% in placebo) 35% had Side –effects Numbness, dizziness, fatigue, metallic taste Authors conclude similar efficacy to other adjuvants and good safety profile Other/New Things to Try Capsaicin – High dose patch in PHN (640mcg/cm2) 1 – 60 min application Lasts up to 12 weeks Mean decrease in pain score of 29.6% Side-effects – Pain and erythema at site (Backonja – Lancet Neurology, 2008) Cannabis – Sativex - Neuropathic pain with Allodynia Improvements of 1.43 on 10 point VAS Good safety profile – SE include GI upset & drowsiness (Nurmikko – Pain 2007) Other/New Things to Try Intrathecal Ziconotide N-type Ca Channel blocker (NCCB) Median dose 6.48mcg/day Improved VASPI scores in 53.1% Decreased opioid usage in 9% Very expensive Side Effects: Memory loss, dizziness, nystagmus, somnolence, gait, CK rise (Pommer - J Pain Symptom – 2009) A Comparison of Adjuvants Drug NNT Titration Notes Side Effects TCA 2.5-3 2-15 wks Antidepressant, cheap Anticholinergic Duloxetine 4-5 none Anxiolytic, antidepressant few Venlafaxine 4-5 3-5 wks Antidepressant few Gabapentin 3.5-4.5 1.5-6 mo Min drug interactions Dizzy/sleepy Pregabalin 3.5-4.5 1-2 wks Min drug interactions Dizzy/sleepy Methadone ? variable Opioid, cheap Opioid, drug interactions Ketamine ? 1-4 wks Opioid sparing Hallucinations Tramadol 3.8 4-8 wks For Diabetes, PHN Anticholinergic Carbamezapine 1.7 1-4 wks For Trigeminal neuralgia Drug interactions Lidocaine/Mexilitine 4 none IV trial then po Cardiac, neurologic Capsaicin ? none/days Topical Burning, redness Cannabinoids ? none/days For MS, allodynia GI, drowsiness Clonidine ? none/days Effective IT, topical Hypotension Summary/Objectives By the end of the hour the learner will be able to: Define neuropathic pain List at least 2 types of Pain receptors List at least 4 different types of adjuvant pain medications List the mechanisms of action, benefits, and side-effects of these 4 medications List 2 new/different adjuvant pain medications Recommended References 1. 2. 3. Cruccum, G. Treatment of painful neuropathy. Current Opions in Neurology. 2007; 20; 531-535. Dworkin, R. et al. Pharmacologic management of neuropathic pain: evidence-based recommendations. Pain. 2007; 132; 237-251. Gilron, I. et al. Neuropathic pain: a practical guide for the clinician. CMAJ. 2006; 175(3); 265-275.