* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Structural Heart Disease - Circulation: Cardiovascular Interventions
Remote ischemic conditioning wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Turner syndrome wikipedia , lookup
Marfan syndrome wikipedia , lookup
Pericardial heart valves wikipedia , lookup
Artificial heart valve wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Mitral insufficiency wikipedia , lookup
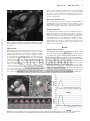
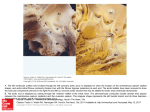
Structural Heart Disease Aortic Regurgitation and Left Ventricular Remodeling After Transcatheter Aortic Valve Implantation A Serial Cardiac Magnetic Resonance Imaging Study Constanze Merten, MD; Hans-Wilko Beurich, MD; Dirk Zachow, MD; Ahmad E. Mostafa, MD; Volker Geist, MD; Ralph Toelg, MD; Gert Richardt, MD; Mohamed Abdel-Wahab, MD Downloaded from http://circinterventions.ahajournals.org/ by guest on June 12, 2017 Background—Aortic regurgitation (AR) after transcatheter aortic valve implantation (TAVI) has been associated with poor outcomes, but little is known about how it evolves over time. We evaluated left ventricular (LV) function, remodeling, and the occurrence and evolution of AR after TAVI by using cardiac MRI. Methods and Results—Forty-three patients treated with transfemoral TAVI underwent cardiac MRI 1 week and 6 months after TAVI. LV volumes and function were assessed by using standard cine MRI sequences. Phase-contrast imaging was performed to quantify the degree of AR. The mean age of the evaluated patients was 80 years, and 65% of patients were women. At baseline MRI, the median LV ejection fraction was 58.1%, which improved significantly at follow-up to 63.4% (P<0.0001). A significant reduction of LV end-diastolic volume (149.7±41.4–140.1±43.9 mL; P=0.014) and of LV mass (156.3±32.8–142.7±39.3 g; P<0.001) was observed. Over time, aortic regurgitant fraction increased slightly but significantly from 5.2% to 7.8% (P=0.04). Subgroup analysis revealed that significant changes of LV ejection fraction, volumes, and mass only occurred in patients with no or mild AR at baseline MRI, whereas those parameters remained unchanged in patients with AR more than or equal to grade II. Conclusions—By using cardiac MRI in patients with TAVI, a significant improvement of LV function, volume, and mass can be documented. Mild-to-moderate AR is commonly seen, and AR shows a small increase over time. More-than-mild AR seems to prevent LV functional and structural recovery after TAVI. (Circ Cardiovasc Interv. 2013;6:00-00.) Key Words: aortic valve insufficiency ◼ cardiac MRI ◼ TAVI ◼ ventricular function, left T ranscatheter aortic valve implantation (TAVI) has recently emerged as an effective alternative therapy for patients with severe symptomatic aortic stenosis considered to be at high or prohibitive surgical risk.1,2 Mild paravalvular aortic regurgitation (AR) is frequent after TAVI with an incidence ranging from 40% to 94%3–8 probably because of the presence of the calcified native valve between the prosthesis and the aortic annulus preventing complete sealing of the paravalvular space. More-than-mild AR occurs in 7% to 19%3–5,8,9 and has been recently associated with an increased early and late mortality.8,10–12 Little is known about how AR after TAVI evolves over time. In addition, limited data are available about the impact of TAVI on left ventricular (LV) volumes, function, and mass, and whether residual AR influences change in LV structure and function. Cine cardiac MRI is the gold standard method for the assessment of LV function and can be combined with flow measurements over the aortic valve or prosthesis for the evaluation of AR.13–16 Compared with the evaluation of AR by echocardiography, MRI is more sensitive in patients with paravalvular, eccentric, or multiple jets like those frequently observed after TAVI.17 We therefore sought to evaluate LV function, LV remodeling, and the occurrence and evolution of AR in the early and medium-term follow-up after TAVI by using serial cardiac MRI. Methods Patient Population Between October 2008 and January 2012, all patients treated with TAVI at our institution were screened for inclusion into this prospective study (n=170; Figure 1). Indication for TAVI was in concordance with the recent consensus statement.18 Data collection was approved by the Institutional Review Board, and all patients signed an informed written consent. Patients with a contraindication to MRI (eg, pre- or post-TAVI pacemakers or MRI incompatible implants) and patients with claustrophobia, severe arrhythmias, or unstable clinical conditions were excluded from the study. Ultimately, a total of 55 consecutive patients treated with TAVI with the use of the 2 currently commercially available bioprostheses (Medtronic CoreValve, Received October 12, 2012; accepted July 17, 2013. From the Heart Center (C.M., H.-W.B., A.E.M., V.G., R.T., G.R., M.A.-W.), and Radiology Department (D.Z.), Segeberger Kliniken GmbH (Academic Teaching Hospital of the Universities of Kiel and Hamburg), Bad Segeberg, Germany. The online-only Data Supplement is available at http://circinterventions.ahajournals.org/lookup/suppl/doi:10.1161/CIRCINTERVENTIONS. 112.000115/-/DC1. Correspondence to Mohamed Abdel-Wahab, MD, Herzzentrum, Segeberger Kliniken GmbH, Am Kurpark 1, 23795 Bad Segeberg, Germany. E-mail [email protected] © 2013 American Heart Association, Inc. Circ Cardiovasc Interv is available at http://circinterventions.ahajournals.org 1 DOI: 10.1161/CIRCINTERVENTIONS.112.000115 2 Circ Cardiovasc Interv August 2013 WHAT IS KNOWN • Paravalvular aortic regurgitation after transcatheter aortic valve implantation has been associated with poor outcomes, but little is known about how it evolves over time, and on its potential impact on left ventricular remodeling. • The assessment of aortic regurgitation after transcatheter aortic valve implantation by using echocardiography is complex and challenging. WHAT THE STUDY ADDS • By using cardiac MRI, significant positive left venDownloaded from http://circinterventions.ahajournals.org/ by guest on June 12, 2017 tricular remodeling occurs within 6 months after transcatheter aortic valve implantation. • Aortic regurgitation quantified by MRI does not decrease over time. • In patients with more-than-mild AR, no positive left ventricular remodeling is observed. Medtronic Inc, Minneapolis, MN and Edwards SAPIEN XT, Edwards Lifesciences, Irvine, CA) were included. Of these 55 patients, 43 patients with TAVI were included in the final analysis. The remaining 12 patients underwent baseline MRI examinations, but follow-up MRI scans could not be performed because of the following: death during the follow-up period (n=1), pacemaker implantation during the follow-up period (n=1), refusal of follow-up MRI (n=6), aborted followup MRI attributable to claustrophobia (n=2), and loss to follow-up (n=2; Figure 1). All patients who refused to undergo follow-up MRI were in good clinical condition and therefore refused the follow-up in-hospital visit or specifically the MRI examination. All patients who underwent only a baseline MRI study had grade 0 or I AR (Table in the online-only Data Supplement). TAVI Protocol After informed consent, TAVI with either device was performed via the transfemoral route. Description of both valves together with review of the implantation technique has been described elsewhere.3,19 Clinical and anatomic selection criteria and device size selection were in line with previously published recommendations.3,19 Selection of the prosthetic valve size was based on the measurements of the diameter of the aortic valve annulus obtained by transesophageal echocardiography. At the end of the TAVI procedure, a 5F pigtail catheter was placed in the upper part of the implanted valve above the leaflets in the ascending aorta, and an aortography in 30° right anterior oblique and 50° left anterior oblique projections was performed by using 35 mL of contrast at a flow rate of 16 mL/s. Qualitative assessment of the severity of AR was performed by visual estimation of the concentration of contrast medium in the left ventricle, with the method of Sellers et al20 by 2 independent interventional cardiologists. Baseline clinical, echocardiographic, and procedural characteristics were prospectively recorded for all enrolled patients and entered into an institutional database. Thirty-day and 6-month clinical assessment together with transthoracic echocardiography (TTE) and laboratory evaluation were performed for all patients. MRI Protocol The baseline MRI scan was performed 1 to 2 weeks after TAVI, the follow-up MRI 6 months later. Cardiac MRI was performed by using a clinical 1.5 Tesla whole-body scanner (Magnetom Espree, Siemens AG, Erlangen, Germany). All patients were investigated by ECG-gated cardiac MRI in the supine position with a 5-element cardiac phasedarray coil. The stent carrying the Medtronic CoreValve prosthesis is made up of nitinol, which is not ferromagnetic and can therefore be safely examined by MRI (Figure 2). The stent frame of Edwards valve is composed of cobalt chrome material; nonclinical testing revealed that it can be safely scanned under routine MRI conditions. LV volumes and function were determined by cine images using a standard steady-state free precession sequence in continuous shortaxis planes covering the whole left ventricle from base to apex. For flow measurements, a breath-hold velocity-encoded phase-contrast MR sequence was used (through plane, segmented fast low-angle shot 2-dimensional sequence, repetition time/echo time 46/2.7 ms, velocity encoding 150–300 cm·s−1, scan in expiration, scan duration ≈10 s). The slice was positioned perpendicular to the long axis of the ascending aorta closely beneath the upper margin of the stent holding the CoreValve prosthesis or at the corresponding distance from the aortic annulus for the Edwards valve, respectively. This position was chosen because it had proved to be less susceptible to artifacts caused by the valves and stent compared with a lower position, and a perpendicular cut through the ascending aorta could be achieved more accurately. In fact, no visible artifacts of valves and stents were present on the analyzed images. Contrast administration was not necessary for both cine imaging and flow measurements. Consequently, no patients were excluded because of impaired renal function. Figure 1. Study population. A detailed description of the study population as part of the overall transcatheter aortic valve implantation (TAVI) cohort treated during the study period. ICU indicates intensive care unit; PM, pacemaker; and SAVR, surgical aortic valve replacement. Merten et al MRI After TAVI 3 RF was calculated (Figure 3). An RF of ≤15% was graded I (mild), 16% to 30% was graded II (moderate), 31% to 50% was graded III (moderate to severe), and >50% was graded IV (severe) AR according to the standard grading criteria.13,21 A calculated RF<1% was classified as no AR (grade 0). Natriuretic Peptides Assay Blood samples were drawn preprocedurally, at baseline MRI and the MRI follow-up visit. N-terminal pro-brain natriuretic peptide (NT-proBNP) was analyzed by using a commercially available kit (The Elecsys proBNP, Roche Diagnostics, Mannheim, Germany). Statistical Analysis Downloaded from http://circinterventions.ahajournals.org/ by guest on June 12, 2017 Figure 2. Medtronic CoreValve prosthesis visualized with cardiac MRI. The Medtronic CoreValve prosthesis visualized in a 3-chamber view with a flow artifact caused by the jet of aortic regurgitation (arrow). MRI Analysis MRI data were analyzed by 2 independent and experienced observers. No formal blinding was performed, but observers had no access to the results of the baseline scan at the moment of evaluation of followup MRI. Global LV function was assessed by manually contouring the endocardial borders of end-diastolic and end-systolic images. For the computation of LV mass, the epicardial borders were additionally contoured at end diastole. LV volumes, mass, and ejection fraction were then automatically calculated by the software (Argus WIP 2.3, Siemens AG, Erlangen, Germany). An LV ejection fraction (LVEF) >55% was considered normal. For the assessment of the aortic regurgitant fraction (RF), the cross-sectional area of the ascending aorta was defined and manually corrected for motion artifacts that occurred during the breath-hold scan. By using the standard software (see above), the forward and reverse volumes within this region of interest were determined, and the For statistical analysis, MedCalc version 10.3.0 (MedCalc Software, Mariakerke, Belgium) was used. Descriptive results are expressed as numbers and percentages, and continuous variables are expressed as mean±SD or median and range. For comparison of initial and follow-up MRI parameters, paired Student t test or Wilcoxon signedrank test was used, based on the distribution of the change in value. Additionally, Pearson correlation coefficients were calculated to evaluate the relation of LV parameters and aortic regurgitation. A P value <0.05 was deemed significant. Results Baseline Characteristics Overall patient characteristics are summarized in Table 1. The mean age of the study patients was 79.9±5.5 years, and 65% of patients were women. Baseline New York Heart Association (NYHA) functional class was IV in 5 patients and III in 33 patients, and 5 patients had NYHA class II symptoms at baseline. The median logistic European System for Cardiac Operative Risk Evaluation (EuroSCORE) was 17% (range, 7%–82%). Thirty-five patients had a concomitant diagnosis of coronary artery disease; in 13 patients, a percutaneous coronary intervention was performed within 1 week before TAVI. Thirty-two patients (74%) were treated with the Medtronic CoreValve prosthesis, and 11 patients received the Edwards Sapien XT valve. Figure 3. Flow measurements. For flow measurements, the region of interest was placed along the vessel wall of the ascending aorta. Flow curves of a patient with no aortic regurgitation (upper curve) and moderate aortic regurgitation (lower curve) are shown. 4 Circ Cardiovasc Interv August 2013 Table 1. Baseline Patient Characteristics Before TAVI Age, y 79.9±5.5 Females (%) 28/43 (65) Diabetes mellitus (%) 11/43 (26) Hypertension (%) 37/43 (86) Hyperlipidemia (%) 28/43 (65) Obesity (%) 6/43 (14) BMI, kg/m 26.0 (17.3–57.2) 2 Logistic EuroSCORE (%) NT-proBNP, pg/mL 16.6 (7.8–82.0) 2842 (201–49 344) NYHA class II (%) 5/43 (12) NYHA class III (%) 33/43 (77) NYHA class IV (%) 5/43 (12) Downloaded from http://circinterventions.ahajournals.org/ by guest on June 12, 2017 Coronary artery disease (%) 35/43 (81) PCI during admission (%) 13/43 (30) Previous PCI (%) 16/43 (37) Previous CABG (%) 9/43 (21) Previous myocardial infarction (%) 8/43 (19) Data presented as mean±SD, median and range, or number and percentage. Obesity defined as BMI>30 kg/m2. BMI indicates body mass index; CABG, coronary artery bypass graft; EuroSCORE, European System for Cardiac Operative Risk Evaluation; NT-proBNP, N-terminal pro-brain natriuretic peptide; NYHA, New York Heart Association; PCI, percutaneous coronary intervention; and TAVI, transcatheter aortic valve implantation. Prosthetic Valve Function After TAVI The mean transvalvular pressure gradient decreased from 48.2±16.7 mm Hg before intervention to 9.1±4.7 mm Hg after TAVI (P<0.0001). Angiographic assessment of AR was performed immediately after the procedure. No AR was seen in 13 (30%) of the 43 patients. AR was mild (grade I) in 24 patients (56%), whereas in 6 patients (14%), a moderate AR (grade II) was observed. Baseline MRI Baseline MRI was performed at a median of 11 days after TAVI. At baseline examination, any AR (RF>1%) was present in 37 of the 43 patients (86%); in 6 patients (14%), no AR was observed. While mild AR was present in 29 patients (68%), moderate AR was observed in 7 patients (16%) and, in 1 patient (2%), moderate-to-severe AR was detected. The median RF of the entire cohort was 5.18% (range, 0.11%– 38.9%). The mean heart rate during flow measurements was 64.1±11.3 bpm. Baseline MRI showed a median LVEF of 58.1% (range, 22.1%–71.6%). A normal ejection fraction was seen in 23 patients, and another 10 patients had only slightly reduced systolic LV function with an LVEF of 50% to 55%; in 10 patients, the LVEF was more severely impaired. The mean end-diastolic volume (EDV) was 149.7±41.4 mL, the median end-systolic volume was 63.4 mL (range, 22.8– 203.0 mL). Early after TAVI, the mean myocardial mass was 156.3±32.8 g. Follow-up MRI Follow-up MRI was performed at a median of 6 months after TAVI (range, 5–12 months). AR of any grade was present in 39 of the 43 patients (91%). We observed grade I AR in 31 patients (72%), grade II AR in 5 patients (12%), and grade III AR in 3 patients (7%; Figure 4). Over time, the mediancalculated aortic RF increased slightly but significantly from 5.2% to 7.8% (P=0.04; Table 2; Figure 4). The mean heart rate during flow measurement at follow-up did not differ from baseline MRI (64.1±11.3 versus 64.0±11.7 bpm; P=0.94). On the contrary, we observed a significant increase of the median LVEF at follow-up MRI (58.1% versus 63.4%; P<0.0001). There was also a significant decrease of the EDV (149.7±41.4 versus 140.1±43.9 mL; P=0.014) and of the LV myocardial mass (156.3±32.8 versus 142.7±39.3 g; P<0.001; Table 2; Figure 5). The increase of LVEF was not affected by preTAVI revascularization with percutaneous coronary intervention. Impact of AR on LV Recovery No significant correlation was observed between RF and LV ejection fraction at baseline MRI (P=0.28), whereas a modest, but significant, correlation was seen between RF and LVEF at follow-up MRI (r=−0.37; P=0.017). There was no significant correlation between the RF at baseline and changes in LVEF (r=−0.18; P=0.24), but we observed a strong trend toward a correlation between baseline RF and changes in LV mass (r=0.30; P=0.053), and a significant correlation between RF at baseline and changes in EDV (r=0.40; P=0.008; Figure I in the online-only Data Supplement). Subgroup analysis revealed that significant changes of LVEF, EDV, and LV mass only occurred in patients with Figure 4. Aortic regurgitation at baseline and follow-up MRI. Bar diagrams showing the number of patients with different grades of aortic regurgitation (AR) at baseline and follow-up MRI. Merten et al MRI After TAVI 5 Table 2. Cardiac MRI and NT-proBNP Measurements Shortly After TAVI and at Follow-up LV ejection fraction, % Baseline MRI Follow-up MRI Sample Change P Value <0.0001 58.1 (22.1 to 71.6) 63.4 (24.0 to 74.2) 4.88 (−6.3 to 18.7) LV EDV, mL 149.7±41.4 140.1±43.9 −9.6±24.5 0.014 LV mass, g 156.3±32.8 142.7±39.3 −13.6±21.2 <0.001 Aortic RF, % 5.2 (0.1 to 38.9) 7.8 (0.0 to 41.9) 1.3 (−7.8 to 14.7) 0.04 2019 (328 to 23 529) 1336 (132 to 30 764) −579 (−8373 to 7235) 0.025 NT-proBNP, pg/mL Data presented as mean±SD or median and range. P value obtained by using either the paired Student t test or the Wilcoxon signed-rank test according to the distribution of the change in value. EDV indicates end-diastolic volume; LV, left ventricular; NT-proBNP, N-terminal pro-brain natriuretic peptide; RF, regurgitant fraction; and TAVI, transcatheter aortic valve implantation. no or mild AR at baseline MRI, whereas those parameters remained unchanged in patients with AR more than or equal to grade II (Table 3). Downloaded from http://circinterventions.ahajournals.org/ by guest on June 12, 2017 Plasma Concentrations of NT-proBNP Preinterventionally, NT-proBNP levels were considerably elevated with a median value of 2842 pg/mL (range, 201–49 344 pg/mL). In the early postinterventional period, we observed a significant reduction of NT-proBNP levels (2842 versus 2019 pg/mL; P=0.025). During a longer follow-up period, we found a further decrease of NT-proBNP serum levels compared with pre-TAVI levels (2842 versus 1336 pg/mL; P=0.0001) as well as a significant reduction between baseline and followup MRI (2019 versus 1336 pg/mL; P=0.017). Additionally, a moderate, but significant, correlation between the RF and NTproBNP levels was observed at baseline (r=0.33; P=0.046) and at follow-up (r=0.32; P=0.045; Figure II in the onlineonly Data Supplement). Discussion In recent years, TAVI has emerged as an alternative treatment to surgical aortic valve replacement for patients with severe symptomatic aortic stenosis and high or prohibitive surgical risk. Clinical short- and medium-term outcomes compare favorably with the outcome of surgical aortic valve replacement.1,2,12 Yet, most published series observed a high incidence of paravalvular AR after TAVI, which occurs in up to 94% of patients3–8 and is at least moderate in up to one fifth of them. The present study is the first to use cardiac MRI for the evaluation of the incidence and evolution of AR after TAVI and its impact on LV functional and structural recovery. By using cardiac MRI, we found AR of any grade in 86% of patients early after TAVI, and moderate or severe AR in 19%, which is concordant with previous studies. Similar to the surgical experience,22 postprocedural AR after TAVI has been recently associated with increased short- and intermediate-term mortality.8,12 Nevertheless, the few follow-up data available suggested a stable course or even a decrease in the incidence and severity of AR after TAVI.6,10,23 In contrast, we observed a small increase in the incidence and severity of paravalvular AR at follow-up, with any grade of AR present in most examined patients. There are several possible reasons for this discrepancy. First, in previous studies, patients were examined by using echocardiography. Compared with TTE, MRI has a lower intraobserver and interobserver variability in the assessment of regurgitant volumes and might therefore be more reliable for serial measurements.24 In addition, we demonstrated in a previous study that conventional TTE has its limitations in detecting and quantifying post-TAVI AR compared with MRI.17 The limitations of TTE have been recently highlighted in the European Association of Echocardiography/American Society of Echocardiography recommendations for the use of Figure 5. Left ventricular (LV) function and aortic regurgitant fraction at baseline and follow-up MRI. Dot-and-line diagrams of parameters of LV function and mass and aortic regurgitant fraction at baseline and follow-up MRI demonstrating an increase of LV ejection fraction, a decrease of end-diastolic volumes and myocardial mass, as well as an increase of the aortic regurgitant fraction. EDV indicates end-diastolic volume; EF, ejection fraction; and RF, regurgitant fraction. 6 Circ Cardiovasc Interv August 2013 Table 3. Changes in LV Function and Structure Stratified by the Degree of Post-TAVI Aortic Regurgitation Baseline MRI Follow-up MRI Sample Change P Value AR grade 0 or I (n=35) LVEF, % 57.0±9.4 62.3±7.9 5.3±5.7 <0.001 EDV, mL 141.2±32.8 128.3±29.0 −12.9±18.8 <0.001 LV mass, g 150.8±31.6 135.0±33.4 −15.8±14.8 <0.001 AR grade ≥ II (n=8) LVEF, % 43.2±17.0 47.2±16.1 4.0±8.1 0.20 EDV, mL 186.7±55.9 191.7±61.1 4.9±39.8 0.74 LV mass, g 180.4±28.3 176.4±47.4 −4.0±38.8 0.78 Data presented as mean±SD. P value obtained by using the paired Student t test. AR indicates aortic regurgitation; EDV, end-diastolic volume; EF, ejection fraction; LV, left ventricular; and TAVI, transcatheter aortic valve implantation. Downloaded from http://circinterventions.ahajournals.org/ by guest on June 12, 2017 echocardiography in transcatheter valve interventions.25 TTE allows only semiquantitative estimation, and eccentric or multiple jets are possibly underestimated. In contrast, by using flow measurements by cardiac MRI, a quantitative assessment of AR is possible, which is independent of the number or eccentricity of the regurgitant jets.17 Another possible explanation for the increasing AR might be a higher compliance of the left ventricle attributable to the dwindling of LV mass after TAVI. This could also explain why this increase of AR was not observed after shorter periods of follow-up. A recently published study using standardized core echocardiography laboratory analysis revealed similar findings with a small, but significant, increase in AR during a 3-year observation period.26 However, on an individual basis, AR was stable in most patients with changes of only a few percentage of RF. Because of the grading of AR according to the absolute RF, very small changes of RF could nevertheless result in a different AR grade between baseline and follow-up MRI. The clinical value of these minor however statistically significant changes remains to be determined. Previously published data analyzing changes in LV systolic function after TAVI are conflicting. Several studies found unchanged LVEF during follow-up of up to 1 year after TAVI,27,28 whereas in others, a highly significant increase of LVEF was observed.29–33 In all of these studies, LV function was assessed by echocardiography. We herewith present the first analysis of temporal changes in LV function after TAVI by using MRI, which is considered the reference method for the evaluation of LV function, and we observed a significant increase of LVEF from 58% at baseline to 63% at followup. We also observed a decrease of LV EDV from baseline MRI to follow-up. Earlier echocardiography studies equally revealed inconsistent results on this topic with a reduction of LV diameters29,30 in some publications, whereas in others, no significant changes were found.27,28 Interestingly, this reduction of EDV could be observed despite a significant increase of AR in the entire cohort. This might be attributable to a statistical rather than a physiological effect because there was no decrease in EDV in the subgroup of patients with AR more than or equal to grade II; in the larger group of patients with AR less than or equal to grade I, however, the decrease was significant. This is also underscored by the significant correlation we observed between aortic RF and changes in EDV between baseline and follow-up MRI and the correlation between RF and NT-proBNP levels, both reflecting an increased volume overload associated with higher baseline RF. The lack of significant change in LV volumes in these patients may signal an important effect on LV structure during the long term; however, larger studies are needed to assess whether this would negatively impact the changes observed in LV function. Finally, our finding of a significant reduction of LV mass is in line with the results of previous echocardiography studies that gave homogeneous evidence of LV mass regression after TAVI.23,27–29 The rapid LV mass regression that is generally observed after TAVI, and much less after surgical aortic valve replacement, may be partly explained by the fact that both TAVI prostheses correspond to stentless surgical valves and have larger valve areas and lower transvalvular gradients.29 Previous work demonstrated the association of LV fibrosis in patients with severe aortic stenosis and functional recovery after surgical aortic valve replacement.34 In the elderly population receiving TAVI, a higher degree of myocardial fibrosis might be assumed, so that the findings of early improvement of systolic LV function and mass regression are even more interesting. But again, these positive changes were not observed in patients with more-than-mild AR. Study Limitations There are several limitations to our study. First, we could not obtain follow-up data for all initially examined patients, and only 20% of those examined showed more-than-mild AR. Therefore, the exact influence of significant AR after TAVI on temporal changes of LV function, volumes, and mass cannot be determined because the study population was too small for robust subgroup analyses. Second, because the presence of cardiac devices such as pacemakers is a contraindication for cardiac MRI, all patients with such devices had to be excluded from the study. This lowered the number of eligible patients because atrioventricular block or bundle–branch block is a common complication of TAVI. Additionally, only clinically stable patients participated in this MRI study, so that patients with severe AR or severely impaired LV function might have been excluded. The slightly different hemodynamics of the CoreValve prosthesis compared with the Edwards Sapien XT valve might impact AR and functional recovery. However, because of the small number of patients receiving the Edwards valve (n=11), no subgroup analysis was performed to compare both prostheses. Conclusions By using cardiac MRI in patients with TAVI, a significant improvement of LV function, volume, and mass can be documented 6 months after valve implantation. Mild-to-moderate AR is commonly seen after TAVI, and AR shows a small increase over time. More-than-mild AR seems to prevent LV functional and structural recovery after TAVI. Acknowledgments We thank Dr Derek R. Robinson (senior lecturer of statistics, University of Sussex, Brighton, England) for his professional statistical support. We are grateful to Dr Judith Hummerjohann and Kathrin Merten et al MRI After TAVI 7 Lehmann (Radiology Department, Segeberger Kliniken GmbH) for their professional support during the performance of this work. Likewise, we thank the clinical research group at the Heart Center, Segeberger Kliniken GmbH, especially Susanne Sachse and Daniela Schuermann-Kuchenbrandt. Disclosures Drs Richardt and Abdel-Wahab report receiving a research grant from Medtronic. The other authors report no conflict. References Downloaded from http://circinterventions.ahajournals.org/ by guest on June 12, 2017 1. Leon MB, Smith CR, Mack M, Miller DC, Moses JW, Svensson LG, Tuzcu EM, Webb JG, Fontana GP, Makkar RR, Brown DL, Block PC, Guyton RA, Pichard AD, Bavaria JE, Herrmann HC, Douglas PS, Petersen JL, Akin JJ, Anderson WN, Wang D, Pocock S; PARTNER Trial Investigators. Transcatheter aortic-valve implantation for aortic stenosis in patients who cannot undergo surgery. N Engl J Med. 2010;363:1597–1607. 2. Smith CR, Leon MB, Mack MJ, Miller DC, Moses JW, Svensson LG, Tuzcu EM, Webb JG, Fontana GP, Makkar RR, Williams M, Dewey T, Kapadia S, Babaliaros V, Thourani VH, Corso P, Pichard AD, Bavaria JE, Herrmann HC, Akin JJ, Anderson WN, Wang D, Pocock SJ; PARTNER Trial Investigators. Transcatheter versus surgical aortic-valve replacement in high-risk patients. N Engl J Med. 2011;364:2187–2198. 3. Webb JG, Pasupati S, Humphries K, Thompson C, Altwegg L, Moss R, Sinhal A, Carere RG, Munt B, Ricci D, Ye J, Cheung A, Lichtenstein SV. Percutaneous transarterial aortic valve replacement in selected high-risk patients with aortic stenosis. Circulation. 2007;116:755–763. 4. Walther T, Simon P, Dewey T, Wimmer-Greinecker G, Falk V, Kasimir MT, Doss M, Borger MA, Schuler G, Glogar D, Fehske W, Wolner E, Mohr FW, Mack M. Transapical minimally invasive aortic valve implantation: multicenter experience. Circulation. 2007;116(11 suppl):I240–I245. 5. De Jaegere PP, Piazza N, Galema TW, Otten A, Soliman OI, Van Dalen BM, Geleijnse ML, Kappetein AP, Garcia HM, Van Es GA, Serruys PW. Early echocardiographic evaluation following percutaneous implantation with the self-expanding CoreValve Revalving System aortic valve bioprosthesis. EuroIntervention. 2008;4:351–357. 6. Rajani R, Kakad M, Khawaja MZ, Lee L, James R, Saha M, HildickSmith D. Paravalvular regurgitation one year after transcatheter aortic valve implantation. Catheter Cardiovasc Interv. 2010;75:868–872. 7. Sherif MA, Abdel-Wahab M, Stöcker B, Geist V, Richardt D, Tölg R, Richardt G. Anatomic and procedural predictors of paravalvular aortic regurgitation after implantation of the Medtronic CoreValve bioprosthesis. J Am Coll Cardiol. 2010;56:1623–1629. 8. Abdel-Wahab M, Zahn R, Horack M, Gerckens U, Schuler G, Sievert H, Eggebrecht H, Senges J, Richardt G; German transcatheter aortic valve interventions registry investigators. Aortic regurgitation after transcatheter aortic valve implantation: incidence and early outcome. Results from the German transcatheter aortic valve interventions registry. Heart. 2011;97:899–906. 9. Grube E, Schuler G, Buellesfeld L, Gerckens U, Linke A, Wenaweser P, Sauren B, Mohr FW, Walther T, Zickmann B, Iversen S, Felderhoff T, Cartier R, Bonan R. Percutaneous aortic valve replacement for severe aortic stenosis in high-risk patients using the second- and current thirdgeneration self-expanding CoreValve prosthesis: device success and 30day clinical outcome. J Am Coll Cardiol. 2007;50:69–76. 10. Tamburino C, Capodanno D, Ramondo A, Petronio AS, Ettori F, Santoro G, Klugmann S, Bedogni F, Maisano F, Marzocchi A, Poli A, Antoniucci D, Napodano M, De Carlo M, Fiorina C, Ussia GP. Incidence and predictors of early and late mortality after transcatheter aortic valve implantation in 663 patients with severe aortic stenosis. Circulation. 2011;123:299–308. 11. Moat NE, Ludman P, de Belder MA, Bridgewater B, Cunningham AD, Young CP, Thomas M, Kovac J, Spyt T, MacCarthy PA, Wendler O, Hildick-Smith D, Davies SW, Trivedi U, Blackman DJ, Levy RD, Brecker SJ, Baumbach A, Daniel T, Gray H, Mullen MJ. Long-term outcomes after transcatheter aortic valve implantation in high-risk patients with severe aortic stenosis: the U.K. TAVI (United Kingdom Transcatheter Aortic Valve Implantation) Registry. J Am Coll Cardiol. 2011;58:2130–2138. 12. Kodali SK, Williams MR, Smith CR, Svensson LG, Webb JG, Makkar RR, Fontana GP, Dewey TM, Thourani VH, Pichard AD, Fischbein M, Szeto WY, Lim S, Greason KL, Teirstein PS, Malaisrie SC, Douglas PS, Hahn RT, Whisenant B, Zajarias A, Wang D, Akin JJ, Anderson WN, Leon MB; PARTNER Trial Investigators. Two-year outcomes after transcatheter or surgical aortic-valve replacement. N Engl J Med. 2012;366:1686–1695. 13. Gelfand EV, Hughes S, Hauser TH, Yeon SB, Goepfert L, Kissinger KV, Rofsky NM, Manning WJ. Severity of mitral and aortic regurgitation as assessed by cardiovascular magnetic resonance: optimizing correlation with Doppler echocardiography. J Cardiovasc Magn Reson. 2006;8:503–507. 14. Chatzimavroudis GP, Oshinski JN, Franch RH, Walker PG, Yoganathan AP, Pettigrew RI. Evaluation of the precision of magnetic resonance phase velocity mapping for blood flow measurements. J Cardiovasc Magn Reson. 2001;3:11–19. 15. Uretsky S, Supariwala A, Nidadovolu P, Khokhar SS, Comeau C, Shubayev O, Campanile F, Wolff SD. Quantification of left ventricular remodeling in response to isolated aortic or mitral regurgitation. J Cardiovasc Magn Reson. 2010;12:32. 16. Wittlinger T, Dzemali O, Bakhtiary F, Moritz A, Kleine P. Hemodynamic evaluation of aortic regurgitation by magnetic resonance imaging. Asian Cardiovasc Thorac Ann. 2008;16:278–283. 17. Sherif MA, Abdel-Wahab M, Beurich HW, Stöcker B, Zachow D, Geist V, Tölg R, Richardt G. Haemodynamic evaluation of aortic regurgitation after transcatheter aortic valve implantation using cardiovascular magnetic resonance. EuroIntervention. 2011;7:57–63. 18. Vahanian A, Alfieri O, Al-Attar N, Antunes M, Bax J, Cormier B, Cribier A, De Jaegere P, Fournial G, Kappetein AP, Kovac J, Ludgate S, Maisano F, Moat N, Mohr F, Nataf P, Piérard L, Pomar JL, Schofer J, Tornos P, Tuzcu M, van Hout B, Von Segesser LK, Walther T. Transcatheter valve implantation for patients with aortic stenosis: a position statement from the European Association of Cardio-Thoracic Surgery (EACTS) and the European Society of Cardiology (ESC), in collaboration with the European Association of Percutaneous Cardiovascular Interventions (EAPCI). Eur Heart J. 2008;29:1463–70. 19.Grube E, Buellesfeld L, Mueller R, Sauren B, Zickmann B, Nair D, Beucher H, Felderhoff T, Iversen S, Gerckens U. Progress and current status of percutaneous aortic valve replacement: results of three device generations of the CoreValve Revalving system. Circ Cardiovasc Interv. 2008;1:167–175. 20. Sellers RD, Levy MJ, Amplatz K, Lillehei CW. Left retrograde cardioangiography in acquired cardiac disease: technic, indications and interpretations in 700 cases. Am J Cardiol. 1964;14:437–447. 21. Zoghbi WA, Enriquez-Sarano M, Foster E, Grayburn PA, Kraft CD, Levine RA, Nihoyannopoulos P, Otto CM, Quinones MA, Rakowski H, Stewart WJ, Waggoner A, Weissman NJ; American Society of Echocardiography. Recommendations for evaluation of the severity of native valvular regurgitation with two-dimensional and Doppler echocardiography. J Am Soc Echocardiogr. 2003;16:777–802. 22. Rallidis LS, Moyssakis IE, Ikonomidis I, Nihoyannopoulos P. Natural history of early aortic paraprosthetic regurgitation: a five-year follow-up. Am Heart J. 1999;138(2 pt 1):351–357. 23. Tzikas A, Geleijnse ML, Van Mieghem NM, Schultz CJ, Nuis RJ, van Dalen BM, Sarno G, van Domburg RT, Serruys PW, de Jaegere PP. Left ventricular mass regression one year after transcatheter aortic valve implantation. Ann Thorac Surg. 2011;91:685–691. 24. Cawley PJ, Hamilton-Craig C, Owens DS, Krieger EV, Strugnell WE, Mitsumori L, D’Jang CL, Schwaegler RG, Nguyen KQ, Nguyen B, Maki JH, Otto CM. Prospective comparison of valve regurgitation quantitation by cardiac magnetic resonance imaging and transthoracic echocardiography. Circ Cardiovasc Imaging. 2013;6:48–57. 25. Zamorano JL, Badano LP, Bruce C, Chan KL, Gonçalves A, Hahn RT, Keane MG, La Canna G, Monaghan MJ, Nihoyannopoulos P, Silvestry FE, Vanoverschelde JL, Gillam LD. EAE/ASE recommendations for the use of echocardiography in new transcatheter interventions for valvular heart disease. Eur Heart J. 2011;32:2189–2214. 26.Yared K, Garcia-Camarero T, Fernandez-Friera L, Llano M, Durst R, Reddy AA, O’Neill WW, Picard MH. Impact of aortic regurgitation after transcatheter aortic valve implantation: results from the REVIVAL trial. JACC Cardiovasc Imaging. 2012;5:469–477. 27.Gotzmann M, Lindstaedt M, Bojara W, Mügge A, Germing A. Hemodynamic results and changes in myocardial function after transcatheter aortic valve implantation. Am Heart J. 2010;159:926–932. 28. Gotzmann M, Bojara W, Lindstaedt M, Ewers A, Bösche L, Germing A, Lawo T, Bechtel M, Laczkovics A, Mügge A. One-year results of transcatheter aortic valve implantation in severe symptomatic aortic valve stenosis. Am J Cardiol. 2011;107:1687–1692. 29. Sherif MA, Abdel-Wahab M, Awad O, Geist V, El-Shahed G, Semmler R, Tawfik M, Khattab AA, Richardt D, Richardt G, Tölg R. Early hemodynamic and neurohormonal response after transcatheter aortic valve implantation. Am Heart J. 2010;160:862–869. 8 Circ Cardiovasc Interv August 2013 30.Clavel MA, Webb JG, Rodés-Cabau J, Masson JB, Dumont E, De Larochellière R, Doyle D, Bergeron S, Baumgartner H, Burwash IG, Dumesnil JG, Mundigler G, Moss R, Kempny A, Bagur R, Bergler-Klein J, Gurvitch R, Mathieu P, Pibarot P. Comparison between transcatheter and surgical prosthetic valve implantation in patients with severe aortic stenosis and reduced left ventricular ejection fraction. Circulation. 2010;122:1928–1936. 31.Giannini C, Petronio AS, Nardi C, De Carlo M, Guarracino F, Delle Donne MG, Talini E, Minzioni G, Bortolotti U, Cucco C, Marzilli M, Di Bello V. Left ventricular reverse remodeling in percutaneous and surgical aortic bioprostheses: an echocardiographic study. J Am Soc Echocardiogr. 2011;24:28–36. 32. Zhao Y, Lindqvist P, Nilsson J, Holmgren A, Näslund U, Henein MY. Trans-catheter aortic valve implantation–early recovery of left and preservation of right ventricular function. Interact Cardiovasc Thorac Surg. 2011;12:35–39. 33. Gotzmann M, Lindstaedt M, Bojara W, Ewers A, Mügge A. Clinical outcome of transcatheter aortic valve implantation in patients with low-flow, low gradient aortic stenosis. Catheter Cardiovasc Interv. 2012;79:693–701. 34. Azevedo CF, Nigri M, Higuchi ML, Pomerantzeff PM, Spina GS, Sampaio RO, Tarasoutchi F, Grinberg M, Rochitte CE. Prognostic significance of myocardial fibrosis quantification by histopathology and magnetic resonance imaging in patients with severe aortic valve disease. J Am Coll Cardiol. 2010;56:278–287. Downloaded from http://circinterventions.ahajournals.org/ by guest on June 12, 2017 Aortic Regurgitation and Left Ventricular Remodeling After Transcatheter Aortic Valve Implantation: A Serial Cardiac Magnetic Resonance Imaging Study Constanze Merten, Hans-Wilko Beurich, Dirk Zachow, Ahmad E. Mostafa, Volker Geist, Ralph Toelg, Gert Richardt and Mohamed Abdel-Wahab Downloaded from http://circinterventions.ahajournals.org/ by guest on June 12, 2017 Circ Cardiovasc Interv. published online August 13, 2013; Circulation: Cardiovascular Interventions is published by the American Heart Association, 7272 Greenville Avenue, Dallas, TX 75231 Copyright © 2013 American Heart Association, Inc. All rights reserved. Print ISSN: 1941-7640. Online ISSN: 1941-7632 The online version of this article, along with updated information and services, is located on the World Wide Web at: http://circinterventions.ahajournals.org/content/early/2013/08/13/CIRCINTERVENTIONS.112.000115 Data Supplement (unedited) at: http://circinterventions.ahajournals.org/content/suppl/2013/08/13/CIRCINTERVENTIONS.112.000115.DC1 Permissions: Requests for permissions to reproduce figures, tables, or portions of articles originally published in Circulation: Cardiovascular Interventions can be obtained via RightsLink, a service of the Copyright Clearance Center, not the Editorial Office. Once the online version of the published article for which permission is being requested is located, click Request Permissions in the middle column of the Web page under Services. Further information about this process is available in the Permissions and Rights Question and Answer document. Reprints: Information about reprints can be found online at: http://www.lww.com/reprints Subscriptions: Information about subscribing to Circulation: Cardiovascular Interventions is online at: http://circinterventions.ahajournals.org//subscriptions/ SUPPLEMENTAL MATERIAL Supplemental table Baseline demographics and cardiac MRI measurements of the study cohort compared to patients who only underwent baseline MRI Age (years) Females (%) Logistic EuroSCORE (%) Study cohort (n=43) 79.9 ± 5.5 28/43 (65) 16.6 (7.8 – 82.0) Baseline MRI only (n=12) 83.7 ± 5.3 8/12 (67) 22.3 (11.4 – 54.4) p 0.04 0.60 0.12 LV ejection fraction (%) LV EDV (ml) LV mass (g) Aortic RF (%) 58.1 (22.1 – 71.6) 149.7 ± 41.9 156.3 ± 32.8 5.2 (0.1 – 38.9) 53.0 (32.1 – 65.8) 146.4 ± 39.6 133.5 ± 16.7 5.5 (1.0 – 13.3) 0.35 0.80 0.02 0.53 Data presented as mean ± SD, median and range, or number and percent MRI = magnetic resonance imaging; LV = left ventricular; EDV = enddiastolic volume; RF = regurgitant fraction 1 Supplemental figures and figure legends Supplemental figure 1: Correlation between regurgitant fraction at baseline MRI and changes in enddiastolic volume. EDV = enddiastolic volume, RF1 = regurgitant fraction at baseline MRI 2 Supplemental figure 2: Correlation between regurgitant fraction and NT-proBNP levels at baseline and follow-up MRI RF 1 = regurgitant fraction at baseline MRI; RF 2 = regurgitant fraction at follow-up MRI 3