* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Dorsal Fixation of the Thoracic and Lumbar Spine Dorsal Fixation of
Survey
Document related concepts
Transcript
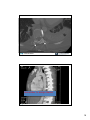
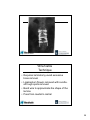
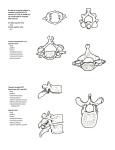
Dorsal Fixation of the Thoracic and Lumbar Spine Michael P. Steinmetz, MD Chairman, Department of Neurological Surgery Case Western Reserve University School of Medicine MetroHealth Medical Center Adjunct Staff Department of Neurosurgery Cleveland Clinic Cleveland, OH Dorsal Fixation of the Thoracic and Lumbar Spine Techniques • • • • • • Thoracic and Lumbar Pedicle Fixation Hook Placement Sublaminar Cable/Wire Transfacet Screws Spinous process plate Translaminar Screws (T1 / T2) 1 Thoracic Pedicle Fixation Relevant Anatomy • Three anatomic characteristics of the pedicle affect screw size and position – Pedicle diameter • Transverse width • Sagittal width – Angle of the pedicle trajectory • Transverse angle • Sagittal angle – Length of pedicle - vertebral body complex (chord length) • Varies for anatomic versus “straight forward” technique Thoracic Pedicle Fixation Relevant Anatomy • Pedicle is auricular in shape – Transverse diameter critical – determines screw diameter • “plasticity of pedicle” – Smallest diameter T4 – T8 – Transverse diameter T3 – T1 – Medial pedicle surface convex so cortex 2-3x thicker than lateral – Transverse diameter is often altered in deformity • Transverse angle changes – T12 pedicles neutral or even divergent and pedicles converge as progress cephalad with T1 pedicle trajectory approx 25 - 35O 2 Thoracic Pedicle Fixation Relevant Anatomy • Chord length generally increases as you progress caudally (body + pedicle length) – T1 – T3 26 – 34 mm – T4 – T6 34 - 44 mm – T7 – T12 36 – 50 mm • Pedicle to “neural” distance – Distance between pedicle and corresponding nerve root is equal along superior and inferior aspect – Dura touches medial pedicle • Worse at concavity in deformity • Relationship of pedicle to facet joint, lamina, and transverse process Lumbar Pedicle Anatomy • Less variability compared to thoracic spine • L1-L5 – Steady increase in transverse width – Slight decrease but fairly stable sag width – Significant increase in transverse angle – Only small changes in sagittal angle, neutral at L1 3 Lumbar Pedicle Anatomy Thoracic Pedicle Fixation Relevant Anatomy Soft Tissue and Vascular Structures T4 T5 T6 T7 T8 T9 T10 T11 T12 4 Thoracic and Lumbar Pedicle Fixation Pre Operative Assessment • Plain X-ray – Sagittal plane deformity • True AP view of pedicles difficult • Obtained only in the vertebral segments that are perpendicular to the x-ray beam (beam may need to be angled above and below the apex to visualize true pedicle dimensions • Supine / Push-prone x-rays may be helpful • Must have 36” standing films with knees/hips extended • Lying flex – ext films (lat decub) – Coronal plane defomity • Side bending views may be helpful • Pedicle assessment often difficult • 36” films and lying flex – ext films Thoracic and Lumbar Pedicle Fixation Pre Operative Assessment • CT scan – Best modality to evaluate pedicle anatomy (a “must” at T4 – T8) – Good visualization of both concave and convex pedicles in cases of coronal deformity – Sagittal / coronal recons often helpful – CT slightly underestimates pedicle width • Volume averaging on each window – Remember pedicles can “adapt” with “oversized screws” especially in adolescents (expansion or cutout by screw threads before fracture occurs) 5 Thoracic and Lumbar Pedicle Fixation Pre Operative Assessment • Image guidance – Flouroscopically assisted – Stereotactic systems • CT (3D CAS) • Computer assisted flouroscopy (2D CAS) • 3D flouroscopy (3D CAS) Thoracic Screw Placement • Two main trajectories of screw placement (often determined by pathology) Assisted free hand technique •Flouroscopy ( AP T1 T4) •Laminotomy (C7 and T1) – Straight forward trajectory (SFT) • Straight forward trajectory allows uniaxial or multiaxial screws (coronal / sagittal deformity) • 27% in pullout strength compared to AT Lehman et al Spine 2003 – Anatomic trajectory (AT) • Multiaxial screws much easier (stabilization for anterior / posterior pathology such as tumor, fracture, degenerative, iatrogenic) • Salvage (?) – 62% MIT Lehman et al Spine 2003 6 Thoracic Screw Placement Free Hand Technique • Starting points for AT and SFT for thoracic vertebrae are slightly variable and are based on posterior element anatomy that must be visualized intraop. (exposure, exposure, exposure) – Transverse process – Base of the superior articular process – Lateral portion of the lamina / pars 7 Thoracic Screw Placement Free Hand Technique • Exposure – Limit dissection to fusion levels (reduce junctional kyphosis or transition syndromes) – T-spine much easier to avoid facet disruption at termini than in LS spine – Expose to tip of T-piece bilaterally and lateral joint / lamina / pars • Facetectomy – Thoroughly clean facet joints – Osteotomize the inferior facet joint and remove articular cartillage on superior facet (3-4 mm) – Do not disrupt joint at UIV Thoracic Screw Placement Free Hand Technique • Facetectomy 8 Thoracic Screw Placement Free Hand Technique • Cortical burring – 3 mm bur creates 3-4 mm posterior cortical breach – Pedicle blush (cancellous bone) may be seen – Generally use gearshift to search for cancellous soft spot – Entrance point • Straight forward trajectory – Starting point varies slightly at each level – Place screw parallel to superior endplate. – If no lateral flouro (T1 – T4) or pre-op films you can probe perpendicular to the dorsal cortical surface of the superior facet T1, T2, T11, T12 Entry Point • SFT T1, T2,and T11, T12 – T1, T2,and T11, T12 transverse line passing through the middle of the transverse process and 3 - 4 mm lateral to the midpoint of the superior facet – T3 – T10 transverse line at the superior border of the transverse process (where it joins the lamina) and 2 mm lateral to the midpoint of the superior facet (this point is 2 – 3 mm caudal to the base of the superior facet) 9 Thoracic Screw Placement Free Hand Technique • Anatomic trajectory – Similar starting points at each level – Sagittal angle 20 – 25O inclination using the superior or inferior endplates Can utilize pre-op films or intra-op flouro (below T4) Mainly “feel” Transverse angulation increases as you go cephalad (0 – 15O with a “jump” at T1) Again mainly “feel” • SFT Entry Point – T1, T2,and T11, T12 transverse line passing through the middle of the transverse process and 3 - 4 mm lateral to the midpoint of the superior facet – T3 – T10 transverse line at the superior border of the transverse process (where it joins the lamina) and 2 mm lateral to the midpoint of the superior facet (this point is 2 – 3 mm caudal to the base of the superior facet) • AT – Same at each level – 2 – 3 mm cranial to base of superior facet and 2 mm lateral to midpoint of superior facet – Even at T1 T2 T11 T12 because of “large” sagittal diameter of pedicle 10 Thoracic Screw Placement Free Hand Technique • Gearshift probing – 2 mm blunt-tipped slightly curved probe – Ventral pressure as “search” for pedicle – Gearshift pointed laterally and insert to 15 – 20 mm – Remove probe and turn tip medially and place tip down to base of prior hole – Then continue path down medial into the body (sudden advancement suggests penetration into ST) • 35 – 40mm T7 – T12 • 30 – 35mm T4 – T6 • 20 – 25mm T1 – T3 Thoracic Screw Placement Free Hand Technique • Gearshift probing – 2 mm blunt-tipped slightly curved probe – Ventral pressure as “search” for pedicle – Gearshift pointed laterally and insert to 15 – 20 mm – Remove probe and turn tip medially and place tip down to base of prior hole – Then continue path down medial into the body (sudden advancement suggests penetration into ST) • 35 – 40mm T7 – T12 • 30 – 35mm T4 – T6 • 20 – 25mm T1 – T3 11 Thoracic Screw Placement Free Hand Technique • Gearshift probing – Sagittal inclination (AT) 20 – 25O inclination from a • Parallel to superior endplate or perpendicular to dorsal surface of line parallel to superior facet (pre-op films). the superior or Mainly “feel” with probe inferior endplates – Transverse inclination (SFT / AT) Can utilize pre-op • Increases from 0O – 15O from films or intra-op T12 – T2 with lami at T1 as big flouro (below T4) “jump” in inclination (pre-op films). Mainly “feel” Mainly “feel” with probe – Sagittal inclination (SFT) – Work from cranial to caudal or caudal to cranial to visualize trends of entry point at each successive level Thoracic Screw Placement Free Hand Technique • Palpation – Once probe removed observe for CSF (the “Trost” phenomenon) – Palpate all four “walls” and floor using flexible ball tipped probe • Majority of wall perforations are lateral • Can determine chord length with probe • If wall breach occurs can redirect screw with tap (utilize AT) – “Undertap” pedicle tract • 4.2 tap for 5.2 scew • 4.0 tap for 5.0 screw – Repalpate 12 What if you miss the pedicle? • Step 1 What if you miss the pedicle? • Step 1 SH*T! 13 What if you miss the pedicle? • Step 1 • Step 2 – Blame someone else What if you miss the pedicle? • Step 1 • Step 2 – Blame someone else • Resident/fellow • Rep • Anesthesia? 14 Missing the Pedicle • Most often too lateral • Look at other successful holes/screws – Importance for moving in a uniform fashion • Assess landmarks – Move starting point more medial – Aim medial Missing the Pedicle • If successfully locate – Make sure utilize correct pedicle hole – Use a k-wire, cannulated tap and/or screw • If can’t easily locate pedicle – Most often skip unless at ends of construct 15 Missing the Pedicle • Don’t be afraid (really proud) to perform laminotomy, fluoroscopy • Use salvage technique – Anatomic trajectory – In out in – Etc. In Out In 16 Thoracic Screw Placement Free Hand Technique • Confirmation of screw placement – Imaging • True AP and lateral flouroscopy (T1 – T4 AP) • Screw crossing midline of body (? medial wall breach) • Screw not crossing medial cortical wall of the pedicle (? lateral wall breach) • Screws that intersect an endplate (SFT) and should not extend beyond 75-80% of vertebral body sagittal distance (T1 – T4) • Rod contouring and correction – 3D contouring – useful to have 2 or more rod holders – EMG • Useful T6 – T12 • Stimulate screws intra-op and monitor rectus abdominis muscle 17 Remember to assign blame! 18 Lumbar Pedicle Screw Free Hand Technique • Entry point classically described as intersection of TP and infer lateral facet margin Trajectory – Roy-camille: medial entry “straight ahead” technique – Wienstien: lateral entry with converging screws – Kraig : “up and in” to obtain sub-chondral purchase 19 Placement • Decorticate entry point with burr • Use pedicle probe or curette to advance down pedicle into body. Placement • Use ball-tipped probe to feel for cortical breech • Place screw +/tapping • Adjuncts: image guidance, fluoroscopy, direct visualization of pedicle 20 Placement • Screw size? – Pedicle diameter measured at isthmus – Pick largest diameter screw that will fit inner cortical diameter (C) – Length 5 mm short of ant cortex on lateral xray Application Strategies • Triangulation – Increases pull-out strength • Start low, aim high at most rostral level to avoid damaging facet 21 Cortical Lumbar Screws Mobbs TJ.Orthopedic Surgery 2013 Technique • Starting point is medial pars 22 Hook Fixation HOOK FIXATION • Location – Sublaminar • Upgoing / Downgoing – Transverse process • Downgoing – Pedicle •Strength varies with hook type: Lamina Pedicle Transverse process • Upgoing • Application of corrective forces – Good for applying distraction / compression / lateral translation – Poor at applying rotational forces 23 Dorsal Fixation of the Lumbar and Thoracic Spine Hook Fixation • Advantages – Increased pullout resistance in osteoporotic bone – “Easier” technical application than pedicle screws • However much greater construct design planning – No risk to anterior structures • Disadvantages – Places hardware in the canal – Posterior elements required for fixation – Force exerted at a distance from the IAR • Short segment fixation less beneficial (except compression) – Some loss of correction compared to pedicle fixation Dorsal Fixation of the Thoracic Spine Hook Fixation 24 Dorsal Fixation of the Thoracic Spine Sublaminar Hooks • Increased risk of neurologic injury from canal compromise – Hook must conform to size/shape of lamina – Avoid bilateral hooks – Safe if complete spinal cord injury • Increased bone/implant interface – Increased strength (osteoporosis) but requires laminotomy – Decreased surface area for bone fusion • Since upgoing / downgoing can apply distractive and compressive forces Dorsal Fixation of the Thoracic Spine Sublaminar Hooks • Perform laminotomy • Insert trial feeler – Several sizes • Hook must conform to size/shape of lamina 25 Dorsal Fixation of the Thoracic and Lumbar Spine Offset Sublaminar Hooks • Allows for mismatch between implants – pedicle hook/screw and a lamina or T- piece hook • More bone / fusion surface coverage Dorsal Fixation of the Thoracic Spine Pedicle Hooks • Pedicle is mechanically strong – Good purchase even at T5 – “Less” hardware in canal than sublam. • Should not be used bilateral at the same level due to pseudoarthrosis risk • Cannot be at the caudal end of a construct (joint disruption) • Only provides distractive force – Unless combined with laminar / T-piece hook / pedicle screw 26 Dorsal Fixation of the Thoracic Spine Pedicle Hooks • Trial introduced into facet joint • Remove inferior facet with ¼ inch osteotome • Hook blade engages pedicle • Hook throat engages inferior facet • Superior facet sandwiches hook • Place hook + screw Dorsal Fixation of the Thoracic Spine Transverse Process Hooks • Not as strong purchase as laminar or pedicle hook so limited correction – However T2 - T5 can withstand some corrective forces applied (holding power) • Easy to isolate and prepare • Placed in down going direction – Compressive forces • Blades typically short/stout – risk of pullout / dislodgement • Blades angulated for medial attachment of rod 27 Dorsal Fixation of the Thoracic Spine Transverse Process Hooks • Must strip costotransverse ligament • Placed in down going direction • Blades typically short/stout • Blades angulated for medial attachment of rod Application Strategies • Laminar claw • Pedicle screw – Laminar hook – provide additional fixation for osteoperotic bone 28 Wire/Cable Technique • Requires laminotomy-avoid excessive bone removal • Ligamentum flavum removed with curetteall rough spots removed • Bend wire to approximate the shape of the lamina • Pass from caudal to rostral 29 30 FACET SCREWS 31 History • Boucher first described true transfacet fixation in 1959 • Magerl described translaminar facet screw fixation in 1984 Clinical Data Lumbar cadavers tested in short term and long term cyclic loading conditions Results Short term NO DIFFERENCE between fixation except in flexion-STIFFER with facet screws Long term NO DIFFERNCE, no decrease in fixation FACET SCREWS PROVIDE EQUAL FIXATION TO PSF-BETTER IN FLEXION 32 33 Percutaneous Transfacet Fusion 34 35 ILIF™ CASE • L4-5 ILIF with 45mm plate and 14mm H2 36 Conclusions • Pedicle screw fixation is work horse – Different trajectories depending on anatomy and situation – Key to safe placement is a clear understanding of the relevant anatomy – Bail-out options available • Many fixation options available – May be better in certain circumstances • Laminar hooks and osteoporosis THANK YOU 37 Dorsal Fixation of the Thoracic Spine Construct Design Strategies Dorsal Fixation of the Thoracic Spine Construct Design Strategies • Pre-op plan Application Strategies – Goals • Neurologic – Decompression • Restore stability / maintain stability • Alignment – Sagittal balance (kyphosis begets kyphosis) – Coronal balance • Fusion 38 Construct Planning • Most may be figured out preoperatively • Use map or white board in OR • Fixation points and types – Anatomic variants – Construct length – Anterior column support General Prinicples Construct Design Strategies • Construct length – How long is long enough ? – Always depends on availability of intermediate points of fixation, level of spine, anterior column support – 2A – 2B – Rostral failure at cervico-thoracic thoraco-lumbar junction especially when sagittal balance not fully restored has led to 3A – 2B constructs • Don’t do this – When adequate anterior column load bearing is not fully restored or multilevel instability exists consider 4 point bending constructs • 4A – 3B (must prevent both translational deformation and provide axial load bearing) 39 General Principles • Ensure anterior column support – Allows for shorter dorsal construct – Improved stability – Add it if required • With poor anterior column support – Need long dorsal construct General Principles Construct Design Strategies Application Strategies • Avoid ending long constructs at junctional regions • End construct at most neutral VB as possible – Never apex of curves (sag and coronal) – Minimal to no rotation 40 General Principles Construct Design Strategies Application Strategies • Cross – fixation – Cross-links resist torsional deformation – This especially helps to minimize the chance of hook – bone interface failure – Terminal cross-links are not as effective as more intermediately placed cross members – However often “positional” placement to prevent hook dislodgement • Below but abutting up-going laminar or T-piece hook General Principles Construct Design Strategies Application Strategies • Osteoporosis – Hooks (wires) resist pullout better than screws – Use multiple hooks for load sharing because they apply forces to the spine at a considerable distance from the IAR ( bending moments) • Pedicle Hook-TP Hook • “Laminar claw” – alternate levels – Utilize hooks to help prevent screw pullout • Construct terminus : pedicle screw – laminar hook 41 Thoracic Screw Placement Remember some people have anatomy incompatible with placement of thoracic pedicle screws • Salvage and other techniques available – Hooks – Sublaminar wires/cables – Alternative screw techniques • In out in • Rib head • costotransverse 42 THANK YOU 43