* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Epicardial Fat Volume in Patients With COPD and Cor Pulmonale
Cardiovascular disease wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Jatene procedure wikipedia , lookup
Saturated fat and cardiovascular disease wikipedia , lookup
Coronary artery disease wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
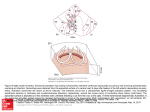
Epicardial Fat Thickness in Patients with Cor Pulmonale Dr Özgür Kaplan1* ([email protected]), Dr. Gökhan Gözübüyük1 ([email protected]), Dr. Zeydin Acar2 ([email protected]), Dr. Hasan Pekdemir3 ([email protected]), Dr.Ferhat Eyyüpkoca3 ([email protected]) *: Corresponding Author (Dr Özgür Kaplan1) *1 : MALATYA STATE HOSPITAL, Department of Cardiology *2: Ahi Evren Thorasic and Vascular Surgery Training and Research Hospital, Cardiology Trabzon, Turkey *3: İnönü University School of Medicine, CARDIOLOGY MALATYA, Turkey ABSTRACT The relation of epicardial-fat-tissue (EFT) with left-ventricular-dysfunction and cardiovascular metabolism and coronary artery disease has been known. The objective of this study is the evaluation of EFT in patients with cor-pulmonale (CP) who have an isolated right heart failure. 36 patients with CP and 30 healthy controls were included in the study. The patients’ with CP right ventricular fractional area change is less than 17%, however that of control group is between 32% and 60%. Patients with a history of CAD and left ventricular dysfunction were not included in the study. EFT was decreased (4,1 ±0,7 vs 6,1±1,2 p=0,001) in patients with CP compared to control group. The difference between the two groups was independent of body-mass-index. EFT is decreasing independently from BMI in the patients with right ventricular dysfunction who do not have left ventricular dysfunction. Epicardial fat thickness would be predictor for degree of right heart failure. Key Words; Epicardial fat tissue,Epicardial fat thickness, Cor Pulmonale Introduction Pulmonary arterial hypertension (PAH) in chronic obstructive pulmonary disease (COPD) is a frequently seen cardiovascular complication. With the growth of the PAH secondary to hypoxia, first right ventricular hypertrophy and / or dilatation or failure and then Chronic CP develop over the time (1-2). In these patients, measurement of epicardial fat and evaluating its relation with right heart functions by using echocardiography has great advantages in practice because of echocardiography’s quick, repeatable and non-invasive nature. Epicardial fat and its relation with coronary heart disease, metabolic syndrome and left ventricular dysfunction has been shown in previous studies (3-8). However, the relation between EFT and right heart functions has not been shown yet. In this study, we examined EFT in patients with cor pulmonale with isolated right heart failure. Methods and Procedures Study Population We have included 36 CP patients and 30 healthy subjects in our study, and those with CP were selected from the subjects who were previously diagnosed and put under treatment. BMI is calculated as weight in kilograms divided by the height in meters squared (kg/m2) and, normal weight is defined as BMI ≤25 kg/m2 and obesity is defined as BMI ≥30 kg/m2. Patients and controls with a history or clinical evidence of left ventricular (LV) wall motion abnormality or coronary artery disease, LV ejection fraction (EF) less than 50%, primary cardiomyopathy, valvular heart disease, congenital heart disease bundle branch block, atrioventricular conduction abnormalities on electrocardiogram, pericarditis, liver disease, chronic renal disease, thyroid dysfunction, anemia, electrolyte imbalance, systemic inflammatory disease and inadequate transthoracic echocardiographic imaging were excluded from study. All of the subjects have sinus rhythm. The study has been carried out according to the principles of the Declaration of Helsinki and approved by Malatya State Hospital investigational review board. Echocardiography In all subjects, echocardiographic examinations (Vivid 7pro,GE Vinmed ,Milwauke USA) were performed by a cardiologist who was blinded to the clinical details and results of the other investigations of each patient and control. During echocardiography examination, a 1lead ECG was recorded continuously. M-mode measurements were performed according to the criteria of American Society of Echocardiography. Three consecutive cycles were averaged for every parameter. Left atrial (LA) dimension, LV end-systolic and end-diastolic diameters were measured. LVEF was estimated by Simpson’s rule. Transmitral pulsed-wave Doppler velocities were recorded from the apical 4-chamber view with Doppler sample placed between the tips of the mitral leaflets. Early (E) and late (A) wave velocities, E/A ratio, E deceleration time (DT) and isovolumetric relaxation time (IVRT) were measured from the mitral inflow profile. Right ventricular systolic function measured with right ventricular fractional area change. EFT was measured according to the method previously described and validated (9). The epicardial fat was identified as the echo-free space between the outer wall of the myocardium and visseral layer of pericardium. EFT was measured perpendicularly on the free wall of right ventricle at end diastole in 3 cardiac cycle. The maximum value at any site was measured and the avarage value was calculated. We have divided the patients into groups with respect to fractional area changes in order to evaluate right ventricular functions. Right ventricular fractional area change was calculated in apical four chamber view by the ratio of the difference between end-diastolic and endsystolic right ventricular areas to the end-diastolic right ventricular area. Normal range of right ventricular fractional area change is between 32-60% , the values between 25-31% were considered as mild and with values ≤ 17 were considered as severe right ventricular systolic dysfunction (10). The patients with a right ventricular area change <17% accompanied by a mean pulmonary artery pressure> 45 mmHg were considered as cor pulmonale patients. By placing pulsed-wave Doppler to right ventricular free wall and tricuspid annulus junction in apical four-chamber view, isovolemic acceleration time (IVA) were measured by dividing the baseline-peak velocity during isovolumic contraction to the peak myocardial velocity during isovolumic contraction.In addition; by placing M-mode tracing at lateral free wall and tricuspid annulus junction in apical four-chamber view, tricuspid annular plane systolic excursion (TAPSE) were measured and right ventricular dysfunction was defined as TAPSE value less than 2 cm (11). Myocardial performance index (MPI) were calculated by dividing sum of right ventricle lateral wall interventricular contraction time (IVCT) and IVRT to total ejection time (ET) with tissue wave Doppler and normal values accepted for right ventricule were 0.28 ± 0.04 (12). Statistical Analysis Statistical analysis was performed using SPSS for Windows version 15.0 software (SPSS Inc, Chicago, IL). All continuous variables were expressed as mean ± SD, and categorical variables were defined as percentages. Categorical data was compared using the chi-square test. Continuous variables were compared between the groups using the Student’s t-test or Mann-Whitney U test, depending on whether they distributed normally or not, as tested by the Shapiro-Wilk test. Pearson’s correlation analysis was used to estimate the relationship between the test parameters. A P value <0.05 was considered to be statistically significant. Results Clinical characteristics and laboratory data of 36 CP patients (mean age 67 ± 9.9) and 30 normal healthy subjects (mean age 70± 5.7) are listed in Table 1. Obese subjects and the controls were similar regarding to the age, gender, diabetes mellitus, hypertension, dyslipidemia and BMI. However there exist only significant difference was in smoking habits and it was higher in CP patients (p= 0.01). The results of right ventricule echocardiographic parameters and EFT are shown in Table 2. When right ventricle echocardiographic parameters of patients with CP were compared to controls; IVA, TAPSE and MPI values were significantly lower (1.9 ± 0.3 vs 2.6± 0.4 p=0.001; 17 ± 2.4 vs 25 ± 2.2 p=0,001; 0,71 ± 0.12 vs 0.48±0.10 p=0.001; respectively) in the patient group. When it is compared with controls, EFT were found to be thinner in patients with CP (4.1 ± 0.7 vs 6.1±1.2 p=0.001) (Table 2, Figure 1). A significant positive correlation was detected among EFT and both TAPSE and IVA (r=0.653 p=0,001 and r=0.377 p=0.02, respectively) and also, there was a significant negative correlation between EFT and MPI (r=-0.543 p=0.001) (Table 3). EFT / BMI ratio were measured in each group by dividing EFT to BMI in order to show EFT in each group is independently from BMI values. EFT / BMI was found 0.239 ± 0.417 in control group, however its value in cor pulmonale group was found 0.173 ± 0.38. Difference between two groups (p = 0.001) was significant (Fig. 2). Table 1. Demographic and laboratory variables of the patients with CP and the controls Age Cor Pulmonale (n=36) 67 ± 9,9 Control Group (n=30) 70± 5,7 P value 0,16 Gender (female/male) 10/26 12/18 0.3 BMI 23,9±3,3 25,3±3,3 0,08 Diabetes, n(%) 2(%5,6) 0 0,22 Dyslipidemia, n(%) 0 2(%6,7) 0,22 Hypertension, n(%) 11(%30,6) 16(%53,3) 0,06 Smoker, n(%) 20(%55,6) 8(%26,7) 0,01 BMI= Body mass index. Table 2. Right ventricle parameters and epicardial fat tissue TAPSE MPI IVA EFT Cor Pulmonale (n=36) 17±2,4 0,71±12 1,9±0,3 4,1±0,7 Control Group (n=30) 25±2,2 0,48±10 2,6±0,4 6,1±1,2 P value 0,001 0,001 0,001 0,001 MPI=Myocardial performance index, IVA=Isovolumic acceleration time,TAPSE= Tricuspid annular plane systolic excursion, EFT= Epicardial fat tissue. Table 3. Correlation between epicardial fat tissue and other measured variables Correlation coefficient P value 0,653 0,001 TAPSE -0,543 0,001 MPI 0,377 0,02 IVA MPI=Myocardial performance index, IVA=Isovolumic acceleration time,TAPSE= Tricuspid annular plane systolic excursion. Table 4. Correlation between epicardial fat tissue/body mass index ratio and other measured variables. Epikardial fat thickness (mm) Correlation coefficient P value 0,599 0,001 TAPSE -0,587 0,001 MPI 0,379 0,02 IVA MPI=Myocardial performance index, IVA=Isovolumic acceleration time,TAPSE= Tricuspid annular plane systolic excursion. 7 6 p=0,001 5 4 3 2 1 0 CONTROL COR PULMONALE Figure 1: Analysis of epicardial fat thicknes in patients with cor pulmonale compared to controls. EFT/BMI(mm/kg/m2 0.3 0.25 p=0,001 0.2 0.15 0.1 0.05 0 CONTROL COR PULMONALE Figure 2: Epicardial fat thicknes corrected for body mass index in patients with cor pulmonale compared to controls. DISCUSSION Epicardial adipose tissue has a smaller adipocyte size but higher rates of fatty acid uptake and secretion than other visceral fat depots (13-14). Epicardial fat has some vital benefits such as being a buffer, absorbing fatty acids and protecting the heart against high fatty acids levels. In addition it is used as a local energy source at times of high demand, channeling fatty acids to the myocardium (13). A body of evidence shows that epicardial fat is an extremely active organ that produces several bioactive adipokines. In earlier studies, it was shown that epicardial fat reduction in heart failure, coronary heart disease and metabolic syndrome had a direct relation with the increase in cardiovascular events(3-7). Also, many complex and diverse metabolic processes are known that plays role in increase and decrease of EFT. However, we set our control groups that did not have a difference with CP in terms of DM, hypertension, dyslipidemia, BMI, age and gender because of the effect of direct metabolic events on EFT. CP is known to have systemic effects like that of COPD. These are: systemic inflammation, nutritional changes and effects on the cardiovascular system. Systemic inflammation is discriminated by oxidative stress, activated inflammatory cells and cytokines and an increase of plasma levels of acute phase proteins. In the meantime, an imbalance between oxidant-antioxidant status could be observed (15). All of these metabolic processes could be effective on EFT. Nutritional changes, especially weight loss, are seen in patients with CP. However, herein weight loss is due to the loss of skeletal muscle mass rather than the loss of fat mass (16). Decreament of EFT in CP group may indicate that EFT is different from other fat tissues. In an earlier studies, epicardial fat has been shown to be associated with left ventricular volume and dysfunction independently from BMI. Left ventricular dysfunction has shown to be significantly decreased in patients group(8). In our study, EFT and RV dysfunction showed a similar relationship independent of BMI. That is, EFT has shown a similar change with a dysfunction in any part of the heart. Because of its anatomical and functional proximity to the myocardium and its intense metabolic activity, some interactions between the heart and its visceral fat depot have been suggested. In another study, EFT was evaluated in patients with obstructive sleep apnea. Thinning of EFT was seen with an increase in the degree of sleep apnea, independent of BMI. Although EFT is associated with general adiposity, it was tought that it was related with visceral adiposity (17, 18). These results support the results of our study. We suspect that this relation may represent a continuum in epicardial fat dynamics. As the myocardium becomes more dysfunctional and develops abnormal metabolic needs, the role for epicardial fat as a source of energy or cytokine hemeostasis would decrease,and as such, less would be found.(19, 20). One limitation of our study is that there was not any evaluation of patients for CAD and the number of patients studied. Conclusions Echocardiographic determination of EFT is important because of its inexpensive, reproducible and non-invasive nature. EFT evaluation is a very easy technigue and gives valuable information in terms of its relation with cardiovascular events especially in debilitated patients and those with chronic diseases. In this study we have showed that the patients with CP have thinner EFT than healty persons. In addition, epicardial fat thickness would be a predictor of the degree of right heart failure. This contribution was done by only using echocardiography. One other important contribution of this study is reproducibiality of it because of usage easily found devices during the diagnosis. REFERENCES 1.Mohsenin V Sleep in Choronic Obstructive Pulmonary Disease,Sleep and Respiration;Editor in Chief,Lynch JP,;Guest Editors , Lee-chiong Jr TL,Collop NA, Seminars in Respiratory and Critical Care Medicine 2005,26:1 2.Mcnicholas WT. İmpact of sleep in COPD. Chest 2000;117;48-53 3. Shirani J, Berezowski K, Roberts WC. Quantitative measurement of normal and excessive (cor adiposum) subepicardial adipose tissue, its clinical significance, and its effect on electrocardiographic QRS voltage. Am J Cardiol 1995;76:414–418. 4. Ding J, Kritchevsky SB, Harris TB, Burke GL, Detrano RC, Szklo M, Jeffrey Carr J. The association of pericardial fat with calcified coronary plaque. Obesity (Silver Spring) 2008;16:1914 –1919. 5. Wheeler GL, Shi R, Beck SR, Langefeld CD, Lenchik L, Wagenknecht LE, Freedman BI, Rich SS, Bowden DW, Chen MY, Carr JJ. Pericardial and visceral adipose tissues measured volumetrically with computed tomography are highly associated in type 2 diabetic families. Invest Radiol 2005;40:97–101 6. Taguchi R, Takasu J, Itani Y, Yamamoto R, Yokoyama K, Watanabe S, Masuda Y. Pericardial fat accumulation in men as a risk factor for coronary artery disease. Atherosclerosis 2001;157:203–209. 7. Gorter PM, de Vos AM, van der Graaf Y, Stella PR, Doevendans PA, Meijs MF, Prokop M, Visseren FL. Relation of epicardial and pericoronary fat to coronary atherosclerosis and coronary artery calcium in patients undergoing coronary angiography. Am J Cardiol 2008;102: 380–385. 8. Tuba Khawaja, MD, Christine Greer, BS, Aalap Chokshi, BS, Nelson Chavarria, MD, Samir Thadani, MD, Meaghan Jones, BS, Kenneth Schaefle, BS, Ketan Bhatia, BS, J. Elias Collado, MD, Daichi Shimbo, MD, Andrew J. Einstein, MD, PhD, and P. Christian Schulze, MD, PhD ,Epicardial Fat Volume in Patients With Left Ventricular Systolic Dysfunction (AmJ Cardiol 2011;108:397– 401) 9.Iacobellis,G. Ribaudo,M.C.,Assael,F.,Vecci,e.,Tiberti,C.,Zappaterreno,A.,Di Mario,U. And Leonetti ,F.(2003 echocardiographic epicardial adipose tissue is related to anthropometric an clinical parameters of metabolic syndrome:a new indicator of cardiovascular risk.J.Clin.Endocrinol. Metab., 88,5163-5168 10.Hinderliter AL, Willis PW 4th, Barst RJ, Rich S, Rubin LJ, Badesch DB, et al. Effects of long-term infusion of prostacyclin (epoprostenol) on echocardiographic measures of right ventricular structure and function in primary pulmonary hypertension. Primary Pulmonary Hypertension Study Group. Circulation 1997; 95: 1479-86. 11. Rushmer RF, Crystal DK, Wagner C. The functional anatomy of ventricular contraction. Circ Res 1953;1(2):162-70. 12. Eidem BW, Tei C, O'Leary PW, Cetta F, Seward JB. Nongeometric quantitative assessment of right and left ventricular function: myocardial performance index in normal children and patients with Ebstein anomaly. J Am Soc Echocardiogr. 1998 Sep;11:849-56. 13. Marchington JM, Pond CM. Site specific properties of pericardial and epicardial adipose tissue: the effects of insulin and high-fat feeding on lipogenesis and the incorporation of fatty acids in vivo. Int J Obesity 1990;14:1013-22. 14. Iacobellis G, Barbaro G. The double role of epicardial adipose tissue as proand anti-inflammatory organ. Horm Metab Res 2008;40:442-5 15.RahmanI, MorisonD,Donalson K,et al. Systemic oxidative stres in asthma,COPD, and smokers Am J Respir Crit Care Med 1996;154:1055-60 16.Schols AM ,Nutrition in chronic obstructive pulmonary disease. Curr opin pulm med 2000;6:110-5. 17.Stefania Mariani, Daniela Fiore, Giuseppe Barbaro, Sabrina Basciani et all, Association of epicardial fat thickness with the severity of obstructive sleep apnea in obese patients, IJCA-14968; No of Pages 6 18.Iacobellis G, Willens HJ. Echocardiographic epicardial fat: a review of research and clinical applications. J Am Soc Echocardiogr 2009;22:1311–9 19. Mazurek T, Zhang L, Zalewski A, Mannion JD, Diehl JT, Arafat H,Sarov-Blat L, O’Brien S, Keiper EA, Johnson AG, Martin J, Goldstein BJ, Shi Y. Human epicardial adipose tissue is a source of inflammatory mediators. Circulation 2003;108:2460 –2466. 20. Baker AR, Silva NF, Quinn DW, Harte AL, Pagano D, Bonser RS, Kumar S, McTernan PG. Human epicardial adipose tissue expresses a pathogenic profile of adipocytokines in patients with cardiovascular disease. Cardiovasc Diabetol 2006;5:1–7.