* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Desai, H
Survey
Document related concepts
Fetal origins hypothesis wikipedia , lookup
Compartmental models in epidemiology wikipedia , lookup
Dental emergency wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Public health genomics wikipedia , lookup
Focal infection theory wikipedia , lookup
Transcript
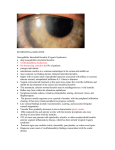
AAO 2015 Resident’s Day Case Report Submission Authors: Heema Desai, O.D. (1); Alanna Khattar, O.D. (2); Dennis Chui, O.D. (3) (1) Bronx Lebanon Hospital Center, optometry resident (2) Bronx Lebanon Hospital Center, optometry resident (3) Bronx Lebanon Hospital Center, optometry attending Title: Scleritis Associated Early Onset Peripheral Ulcerative Keratitis Abstract: A 41-year-old female with unilateral mild scleritis presents with an early onset peripheral ulcerative keratitis without systemic inflammation. We discuss how early diagnosis and treatment can help discover widespread vasculitis and prevent serious complications. Outline: I. Case History a. 41 y/o Black Female b. Complains of redness and severe pain OS for 1 week. Reports decreased vision OS as well. c. Ocular history: i. H/o episcleritis OS in January 2015 (6 months prior to exam) d. Medical history: i. Positive PPD, Negative chest x-ray, Negative Quantiferon Gold ii. Prediabetes iii. Iron deficiency iv. Benign Goiter e. No reported allergies f. Medications: i. Nilfuril (French NSAID) ii. Feosol 325mg iii. Artificial tears iv. Pred Forte 1% ophthalmic solution g. From West Africa II. Pertinent findings a. VA OD: 20/20, OS: 20/30+ b. PERRL(-)APD, EOMs are full OU c. Anterior segment findings: i. OD: Cornea: - Nasal and temporal opacity with no cellularity - 2+ punctate epitheliopathy inferiorly ii. OS: Conjunctiva/Sclera: - 1+ erythema, no tenderness. - Punctate staining of limbal pterygium Cornea: - Nasal circumferential infiltrate from 7-11 with no corneal staining - 2+ cellularity in adjacent stroma d. Posterior segment unremarkable e. Corneal topography: no significant thinning OD/OS f. Laboratory findings: i. Sjogren’s Ab: negative ii. ESR/CRP: within normal limits iii. HLA-B27: negative iv. RF/CCP: negative v. Lysozyme: within normal limits vi. HSV, EBV: negative for acute infection, (+) exposure vii. Lyme: negative viii. PPD: positive, CXR: negative, Quantiferon: negative ix. Anti-streptolysin O (ASLO): High x. Throat culture: negative III. Differential diagnosis a. Peripheral ulcerative keratitis (PUK) b. Mooren’s ulcer c. Terrien’s marginal degeneration d. Marginal keratitis e. Phlyctenular ulcers IV. Diagnosis and discussion a. PUK is often contiguous with adjacent conjunctival, episcleral, and scleral inflammation (1, 5). b. Pathogenesis: unclear i. Hypothesized that vascular architecture of the limbus is suitable for accumulation of IgM. Classical pathway of complement system results in chemotaxis of inflammatory cells in the peripheral cornea. These cells release collagenases and proteases that destroy corneal stroma. Proinflammatory cytokines such as interleukin-1 enables stromal keratocytes to produce matrix metalloproteinase-1 and matrix metalloproteinase-2, which can accelerate matrix destruction process (2, 5). c. Stages of PUK: i. Opacity due to cellular infiltrates within the stroma adjacent to the limbus, without initial epithelial defect (5). ii. After some time, crescent-shaped corneal ulcers can develop with breakdown of overlying epithelium. (1) iii. Varying degrees of vascularization and corneal thinning due to tissue loss in the underlying stroma can occur (1,4) d. PUK is the initial manifestation of collagen vascular disease in 50% of cases (1, 5) i. Rheumatoid arthritis (RA) is the most commonly associated systemic disease. PUK usually presents at the later stages of RA ii. PUK occurs at the earlier stages in patients with Wegener granulomatosis, PUK is often the presenting sign of Wegeners. e. Proper diagnosis is critical in order to determine treatment. Essential to rule out: i. Mooren’s ulcer: form of PUK, but is not associated with scleritis (5) ii. Terrien’s marginal degeneration: inflammation and epithelial defects are not hallmarks of Terrien’s marginal degeneration (1) iii. Marginal keratitis: usually space is present between the ulcer and the limbus. The signs are less severe and are usually self-limited. Will also respond rapidly to topical treatment, whereas PUK, it might worsen (5) iv. Phlyctenular keratitis: less severe and self-limiting. e. Early treatment is critical to prevent corneal complications such as (3, 4): i. Corneal perforation ii. Anterior uveitis iii. Decreased vision iv. PUK is often associated with systemic morbidity, when PUK is in the setting of systemic disease. f. Treatment options include (5): i. Systemic glucocorticoids (Methylprednisone) ii. Alkylating agents (Cyclophosphamide, Chlorambucil) iii. Antimetabolites (Methotrexate, Azathioprine) iv. T-cell inhibitors v. Biologic agents (Infliximab) V. Treatment and management a. Day 1: Pred Forte oph soln 6x/day OS (topical glucocorticoid appropriate due to lack of epithelial defect) b. Day 2: Bloodwork to rule out any systemic inflammation. Continue Pred Forte oph soln 6x/day c. Day 25: After consultation due to positive PPD, patient will report to infectious disease. Consider starting course of Isoniazid and Vitamin B6 before initiating Methotrexate for long-term treatment d. Punctal plugs LLL and LUL for treatment of dry eyes e. Consult Rheumatology for monitoring and long-term immunosuppression after Infectious Disease exam VI. Conclusion a. Peripheral ulcerative keratitis is a rare condition usually associated with increased ocular morbidity and also mortality b. Early cases of peripheral ulcerative keratitis can present as an opacity due to cellular infiltrates within the stroma adjacent to the limbus, without ulceration. c. Early diagnosis and treatment is critical to prevent ulceration and other corneal complications. It can also potentially catch a more severe systemic inflammation such as Rheumatoid arthritis, Wegener’s granulomatosis, polyarteritis nodosa and systemic lupus erythematosus. i. Extensive laboratory testing is important for the proper diagnosis ii. Systemic glucocorticoids and long-term immunosuppressive/immunomodulators are the mainstay of treatment d. Role of optometry: i. Good case history to indicate widespread systemic inflammation, rule out conditions such as Tuberculosis ii. Proper bloodwork and diagnosis iii. Co-management as a multidisciplinary team with Internal Medicine, Rheumatology and Infectious Disease iv. Close follow-up to monitor and ensure resolution References: 1. Galor, A. and Jennifer E. Thorne. “Scleritis and Peripheral Ulcerative Keratitis.” Rhuem Dis Clin North Am. 2007 November; 33(4): 835-854. 2. Gomes B., Priscilla Almeida Jorge, et al. “Corneal Involvement in Systemic Inflammatory Diseases.” Eye & Contact Lenses. May 2015; Volume 41, Number 3. 3. Okhravi, N., Bola Odufuwa, et al. “Scleritis.” Survey of Ophthalmology. July-August 2005. Volume 50, Number 4. 4. Sainz de la Maza M., Stephen Foster, et al. “Ocular Characteristics and Disease Associations in Scleritis-Associated Peripheral Keratopathy.” Arch Opthalmol. 2002; 120:15-19. 5. Yagci, Ayse. “Update on Peripheral Ulcerative Keratitis.” Clinical Ophthalmology. 2012:6 747-754.