* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Functions
Survey
Document related concepts
Transcript
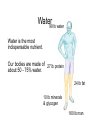
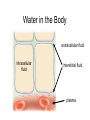
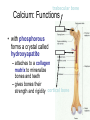
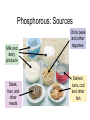
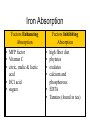
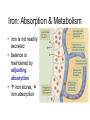
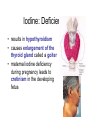
Water & the Minerals Readings – Chapter 11 & Chapter 12 – Omit details p 463 - 465 – Omit details in figs 11.4,11.6, 11.7, 11.10, 11.11, 11.21 – Omit the sections on “Manganese”, “Molybdenum”, and “Other Trace Elements and Ultratrace Elements” Water 99 lb water Water is the most indispensable nutrient. Our bodies are made of 27 lb protein about 50 - 75% water. 24 lb fat 10 lb minerals & glycogen 160 lb man Functions of Water • transport of nutrients & waste compounds throughout body • maintains the structure of large molecules • participation in metabolic reactions • solvent for minerals, vitamins, amino acids, glucose, and other small molecules • lubrication and cushioning of joints, eye, spinal cord • regulates body temperature • maintains blood volume & blood pressure Functions of Water Water in the Body extracellular fluid intracellular fluid interstitial fluid plasma Water Sources Liquids 550 - 1500 ml Metabolism 200 - 300 ml Foods 700 - 1000 ml Total = 1450 - 2800 ml Water in Selected Foods • • • • chicken breast or salmon = 60% cooked white rice = 70% bread = 40% pears = 85% Water Intake Recommendations • 1–1.5 ml water/kcal of energy expended Example • energy expenditure = 2000 kcal/day • water needs = 2000 - 3000 ml water/day Note • alcoholic beverages, soft drinks, and beverages containing caffeine are NOT good substitutes for water • act as diuretics Water Intake Healthy choices… Less healthy choices… Tap vs. Bottled Water? • in NA, bottled water is regulated by similar standards as for tap water • in fact, some tap regulations aren’t imposed on bottled water • ~40% of bottled water is just processed tap water • it costs ~10,000 times more to produce bottled than it does tap water • Some people do not like taste of tap water. – Leave on counter to allow chlorine to evaporate • GVRD recommends letting tap water run for a minute if it has been off for several hours. Is bottled water better? Water Excretion Feces 150 ml Kidneys 500 - 1,400 ml Lungs 350 ml Skin 450 - 900 ml Total = 1450 - 2800 ml Dehydration • occurs when water loss exceeds water intake • may result from excessive water loss or inadequate intake • onset & severity of symptoms depend on activity, fitness level, acclimatization, temperature, & humidity • leads to failure to regulate body temperature, causing hyperthermia • electrolyte imbalances contribute to cardiac arrhythmias & death Dehydration % Weight Lost Symptoms 1-2% • thirst, fatigue, vague discomfort, loss of appetite 3-4% • impaired physical performance, dry mouth, reduction in urine, flushed skin, impatience, apathy 5-6% • difficulty concentrating, headache, irritability, sleepiness, impaired temperature regulation, increased respiratory rate 7-10% • dizziness, muscle spasms, loss of balance, delirium, exhaustion, collapse Water Intoxication • excess consumption of water may lead to dilution of the sodium concentration in the blood causing hyponatremia • children, elderly are most at risk; problem also has a higher incidence in endurance athletes Thirst • most important stimulus for drinking • stimuli for thirst are: reduced blood volume & blood pressure - Athletics, infants, elderly, air travel, illness (fever, diarrhea) - Also triggered with high salt intake - dryness of the mouth & mucous membranes lining the esophagus • Response: – ADH (anti diuretic hormone) • • Triggers kidneys to conserve water Strong alcohol inhibits ADH, lose water, manifest symptoms of low water. Substances that Affect Fluid Balance Alcohol • suppresses ADH secretion, increasing fluid loss • excessive consumption can lead to dehydration, a key contributing factor to many of the symptoms of a hangover - Aspirin does not help hangovers • Drinking less alcohol does Caffeine • inhibits the activity of ADH, increasing fluid loss (still net gain of fluid) Introduction to the Minerals • inorganic elements • some travel freely, others require transporters • often interact with each other • have many and various functions Mineral Bioavailability Nutritional status (needs) Interactions with other minerals Fibers, Phytates, Oxalates Factors that affect mineral bioavailability Intestinal Acidity Polyphenols Sodium (Na+) Functions • principle cation of the ECF & primary regulator of ECF volume • helps maintain acid-base balance • essential for electrical signaling in nerves and muscles Recommendations • Can: 115 mg/day minimum; US: 500 mg/day • AI = 1500 mg; Daily Value = 2400 mg • 1 tsp table salt = 2000 mg sodium Sodium in Foods • processed foods contain the most sodium – 75% of sodium in average North American diet from processed foods – 15% from salt added during cooking & at table – only 10% from sodium naturally present in food – 1 oz Cornflakes contains more sodium than 1 oz salted peanuts – ½ cup instant chocolate pudding contains more sodium than either the cornflakes or the peanuts Sodium in Foods Sodium (Na+) Deficiency • does not result from inadequate intake! • may occur due to excessive loss caused by: – vomiting – diarrhea – heavy sweating during physical activity • may lead to hyponaturemia – symptoms include muscle cramps, mental apathy, loss of appetite • replaced through food or beverages containing both sodium & glucose Sodium (Na+) Toxicity • acute symptoms include edema & hypertension • prolonged excessive intake MAY contribute to hypertension in salt-sensitive individuals • salt restriction in combination with a diet rich in fruits & vegetables decreases blood pressure in these individuals • high sodium intake also linked with an excess of calcium excretion in the urine Potassium (K+) • principle cation of the intracellular fluid • important for electrical signaling of nerves and muscles • helps regulate heart rate & blood pressure • a diet LOW in potassium is associated with an INCREASED risk of hypertension • potassium rich fruits and vegetables linked to a decreased risk of stroke • AI = 4700 mg; Daily Value = 3500 mg Potassium (K+): Food Sources • best food sources: – fresh foods, especially fruits and vegetables • potassium is LOST with food processing Potassium (K+) Deficiency • rare as a result of dietary insufficiency! • hypokalemia = most common electrolyte imbalance – may result from excessive loss associated with heavy sweating, vomiting, or diarrhea – symptoms include muscular weakness, paralysis, confusion Toxicity • result of consumption of supplements Effect of Food Processing on the Mineral Composition of Foods Chloride (Cl-) • important ion in the extracellular fluid • maintains fluid and electrolyte balance • forms part of hydrochloric acid (HCl) in the stomach • diets rarely lack chloride • losses may occur with excess sweating, chronic diarrhea, or vomiting – loss of Cl- & H+ produces metabolic alkalosis • blood concentrations may rise with severe dehydration Calcium (Ca2+) • most abundant mineral in the body (99% of calcium is contained within our bones) – maintains bone structure – serves as a pool to maintain calcium levels elsewhere in the body Recommendations • Adolescents: 1300 mg/day • Adults: 1000 mg/day trabecular bone Calcium: Functions • with phosphorous forms a crystal called hydroxyapatite – attaches to a collagen matrix to mineralize bones and teeth – gives bones their strength and rigidity cortical bone Calcium: Functions • ionized calcium also important for: – muscle contraction – heart function – nerve function: transmission of nerve impulses, release of neurotransmitters from nerve cells – blood clotting: formation of fibrin – regulation of blood pressure – intracellular signaling: binds with calmodulin • activating enzymes and regulating various processes ie. hormone secretion Calcium: Sources • most abundant in milk and other dairy products • non-dairy sources include: – – – – – – cauliflower bok choy broccoli fortified soy products canned fish with bones bone soup stock 50% absorbed cauliflower, watercress, Chinese cabbage, head cabbage, brussels sprouts, rutabaga, kolhrabi, kale, mustard greens, bok choy, broccoli, turnip greens, calcium fortified foods and beverages 30% absorbed milk, calcium-fortified soy milk, calcium-set tofu, cheese, yogurt 20% absorbed almonds, sesame seeds, pinto beans, sweet potatoes 5% absorbed spinach, rhubarb, Swiss chard Calcium: Deficiency • low calcium intake during growth prevents bone from reaching optimal mass and density development of osteoporosis later in life • with inadequate calcium intake, blood calcium concentrations are maintained at the expense of bones • low blood calcium = hypocalcemia – not a result of low calcium intake! – causes include kidney failure, parathyroid disorders, Vitamin D deficiency – may lead to muscle spasms, convulsions Calcium: Toxicity • symptoms include constipation and increased risk of kidney stones • excess calcium also interferes with the absorption of other minerals – e.g. iron, magnesium, zinc • high blood calcium = hypercalcemia – not caused by excessive intake! – primary causes usually cancer, overproduction of PTH, or excess Vitamin D – effects include fatigue, confusion, loss of appetite, constipation, and calcification of tissues Phosphorous (P) • second most abundant mineral in the body • with calcium forms hydroxyapatite crystals of bones and teeth • other important functions include: – buffers pH – part of DNA, RNA, phospholipids, and some proteins – assists in energy metabolism: part of ATP – activation and deactivation of enzymes through phosphorylation reactions • deficiency and toxicity are rare Phosphorous: Sources Milk and dairy products Steak, liver, and other meats Chick peas and other legumes Salmon, tuna, cod and other fish Hypophosphatemia • = low blood phosphate • not a result of dietary insufficiency! • common causes include: – hyperparathyroidism, Vitamin D deficiency, overuse of antacids that bind phosphate • symptoms may include: – anorexia, dizziness, bone pain, muscle weakness, waddling gait • chronic hypophosphatemia leads to: – muscle weakness and damage, respiratory problems, rickets, osteomalacia Hyperphosphatemia • • • • = high blood phosphate not a result of excess consumption commonly a consequence of kidney disease may also result from: – an underactive parathyroid gland, excess Vitamin D supplements, or overuse of phosphatecontaining laxatives • excess phosphate may bind calcium leading to muscle spasms and convulsions Magnesium: Functions • important as a cofactor for metabolism and required for protein synthesis – essential for the production of ATP by the electron transport chain • holds calcium in tooth enamel • participates in muscle contraction and blood clotting • protects against hypertension & heart disease • supports normal functioning of the immune system Magnesium: Sources Legumes Oysters Spinach Sunflower seeds Figs Potatoes Magnesium: Sources • refined foods lose Mg2+ during processing – not added back with enrichment • “hard” tap water may be a significant source • about 50% of magnesium is absorbed – high fiber foods containing fermentable carbohydrates (resistant starches, oligosaccharides, and pectin) increase magnesium absorption • high Ca2+ intake (e.g. from supplements) can interfere with absorption of Mg2+ Hypomagnesia • usually only occurs with disease (e.g. kidney, alcoholism, prolonged diarrhea) • symptoms include weakness, tetany, impaired functioning of the central nervous system, cardiac arrhythmias Hypermagnesia • uncommon in the absence of kidney disease • results in nausea, weakness, diarrhea, dehydration and alkalosis Sulfur • not found alone as a nutrient • in body, exists as a component of other organic compounds (e.g. thiamin, biotin, methionine, cysteine) • important for protein structure – permits the formation of disulfide bridges that help proteins fold in specific ways • obtained in diet through consumption of sulfur containing amino acids – deficiency is unknown in humans Trace Minerals: An Overview • only in miniscule amounts • content in foods depends on soil content, water composition, & food processing • interactions among trace minerals are common • the trace minerals include: iron, zinc, iodine, selenium, copper, fluoride, chromium, molybdenum & manganese Iron • exists in two forms: – “reduced” or ferrous iron (Fe2+) – “oxidized” or ferric iron (Fe3+) Functions • forms part of electron carriers called cytochromes in the ETC (metabolism) • forms part of proteins hemoglobin & myoglobin • required by enzymes that synthesize collagen, hormones, neurotransmitters, and amino acids • important for immune function Iron in Foods Types of Iron • heme – from food derived from animal food sources – 25% absorption • non-heme – from both animal and plant derived foods – only 10% is absorbed Iron: Sources 3 oz steak = 3 mg 3 oz liver = 3 mg ½ cup clams = 22 mg 3 oz shrimp = 2 mg Best source per kcal Iron: Sources Others • broccoli, spinach, dried fruits, eggs, legumes, enriched grains and cereals Contamination Iron • iron found in foods as the result of contamination by inorganic iron salts from iron cookware or iron containing soils Recommendations • Men: 8 mg per day • Women: 18 mg per day Iron Absorption Factors Enhancing Absorption • MFP factor • Vitamin C • citric, malic & lactic acid • HCl acid • sugars Factors Inhibiting Absorption • • • • high fiber diet phytates oxalates calcium and phosphorous • EDTA • Tannins (found in tea) Iron: Absorption & Metabolism • iron is not readily excreted • balance is maintained by adjusting absorption • iron stores, iron absorption Iron: Transport & Storage • the intestine absorbs iron and stores it in protein called mucosal ferritin – iron that is not needed is lost when intestinal cells are shed • when body needs iron, it is moved to another protein transferrin – transports iron to the rest of the body where it is needed, such as the bone marrow where red blood cells are synthesized – think “transferrin” = “transport” Iron: Transport & Storage cont. • surplus is stored in ferritin in the liver, bone marrow and spleen • even greater concentrations of iron lead to storage of iron in another protein called hemosiderin • storage important to prevent free iron from acting as a free radical Iron: Deficiency • most common nutrient deficiency world wide Ways Iron is Lost from the Body… • some iron is lost daily from the digestive tract • only tiny amounts lost through feces, urine, sweat and shedding skin • blood loss Iron: Deficiency cont. Stages in the Development of Deficiency • iron stores diminish – measured by assessing serum ferritin • levels of functional iron decrease – decreased transferrin saturation – accumulation of erythrocyte protoporphyrin • iron deficiency anemia: “microcytic hypochromic anemia” – production of hemoglobin decreases – decrease in hematocrit – decrease in red blood cell size Iron: Deficiency cont. Symptoms • microcytic hypochromic anemia – red blood cells are small and pale – results in fatigue, weakness, headaches, pallor, poor resistance to cold Normal Anemic • cognitive impairment, behavioural changes, reduced learning ability Iron: Toxicity • iron absorption decreases when body needs decrease • excess iron is referred to as “iron overload” – Hemochromatosis • hereditary disorder characterized by enhanced iron absorption – Hemosiderosis • due to long-term overconsumption of iron • characterized by deposits of hemosiderin in tissues Iron: Toxicity cont. Symptoms & Consequences • tissue damage, deposits of iron • apathy, lethargy and fatigue • increased infections • increased risk of heart disease: – free iron acts as a pro-oxidant – may oxidize LDL and contribute to development of atherosclerosis • increased risk of cancer – increased free radical formation may contribute to DNA damage Iron: Toxicity cont. Symptoms & Consequences • poisoning in children if ingest supplements Which are candies and which are supplements? Iron Supplements Zinc: Functions • acts as a cofactor for many enzymes Example: metalloenzymes • assists in immune function • important for growth and development – required for DNA and RNA synthesis • synthesis of heme in hemoglobin • releases Vitamin A from stores and converts to its active form • forms part of an antioxidant enzyme that protects from free radicals = zinc superoxide dismutase Zinc: Functions cont. • stabilizes cell membranes and helps protect them from free radical attack • interacts with platelets in blood clotting • required for the synthesis, storage, and release of the hormone insulin • regulates thyroid hormone function • influences behaviour and learning performance • plays important role in protein synthesis • participates in carbohydrate, fatty acids and alcohol metabolism • others: sperm production, fetal development, taste Zinc: Absorption & Metabolism • absorption rate varies between 15 - 35% – dependant on zinc status – absorption inhibited by fibers and phytates • after absorption may be stored by the protein metallothionein • transported in the blood by several proteins including: – albumin – alpha2-macroglobulin – transferrin Zinc Interactions • an excess of dietary iron may reduce zinc absorption – a dietary iron : zinc ratio > 2 : 1 decreases zinc absorption • large doses of zinc: – inhibit iron absorption – interferes with copper absorption Zinc: Sources • richest sources are protein rich foods Examples oysters 3 oz > 12 mg crab 3 oz = 4.5 mg lean ground beef 3 oz = 4 mg yogurt 1 cup = 2 mg Recommendations Men = 11 mg/day Women = 8 mg/day Zinc: Deficiency • most vulnerable: pregnant women, young children, the elderly, poor • may result from other disease conditions that affect absorption or excretion Symptoms • extreme deficiency leads to severe growth retardation and arrested sexual development during growth = dwarfism Zinc: Deficiency cont. Symptoms cont. • impaired immune function • altered taste perception • diarrhea • symptoms of a Vitamin A deficiency • impaired thyroid function • anorexia • impaired glucose tolerance • slowed wound healing Zinc: Toxicity • toxicity from a high dietary intake is rare • acute excessive doses may result in nausea, vomiting, abdominal cramps, diarrhea, headaches • may interfere with iron and copper absorption and metabolism • chronic elevated intake may depress immune function in elderly individuals Selenium Functions • forms part of the enzyme glutathione peroxidase – an antioxidant – important for protection from OFR • important for thyroid hormone function Food Sources • protein rich foods such as tuna, lobster, pork, eggs, also grains such as oatmeal, whole wheat bread, brown rice and others Selenium Deficiency • associated with a predisposition to a type of heart disease called Keshan disease Toxicity • chronic high doses lead to brittle hair and nails • high doses produce vomiting, diarrhea, hair loss, skin lesions and neurological problems Iodine • iodine in foods is converted to its ionic form iodide by the body Functions • an integral part of thyroid hormone • thyroid hormone has many important functions including: – regulation of basal metabolic rate – regulation of body temperature – necessary for reproduction and growth Iodine: Sources • iodized salt, ocean fish, plants grown in iodine rich soil, milk • average intake of North Americans is above recommendation but below toxic levels Iodine: Deficiency • results in hypothyroidism • causes enlargement of the thyroid gland called a goiter • maternal iodine deficiency during pregnancy leads to cretinism in the developing fetus Iodine: Toxicity • also enlarges the thyroid gland causing a goiter • poses risk of suffocation for a fetus if excess consumed during pregnancy – goiter may block airways • upper limit is 1000 mg per day Note • a goiter may also develop from excess consumption of goitrogens, an anti-thyroid substance found in plants of the cabbage family Copper Functions • forms part of several enzymes – e.g. superoxide dismutase, which functions as an antioxidant enzyme • important for the synthesis of hemoglobin Sources • legumes, whole grains, nuts, shellfish, organ meats, seeds, water Copper Deficiency • rare, may be associated with excess Vitamin C or zinc which interfere with absorption • symptoms include microcytic anemia • in animals leads to increased blood cholesterol and damage to blood vessels Toxicity • rare, may interfere with iron and zinc metabolism Fluoride Functions • forms fluorapatite crystals in teeth – replaces the hydroxyl (OH-) in hydroxyapatite crystals Deficiency • associated with dental decay • 1 part fluoride to 1 million parts water = best protection • primary source of fluoride is drinking water; also in tea and seafood Fluoride Toxicity • fluorosis: damage to teeth that pits and stains the enamel • also leads to nausea, vomiting, diarrhea, chest pain, and itching Chromium Functions • regulates carbohydrate & lipid metabolism • enhances insulin activity Sources • present in a wide variety of foods (e.g. liver, brewer’s yeast, whole grains, nuts and seeds) Deficiency • produces a diabetes-like condition marked by an inability to use glucose normally