* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download outline24074
Survey
Document related concepts
Transcript
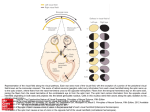
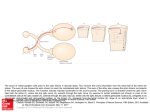
I. II. III. IV. Introduction a. Case History i. 36 YO WM referred for “visual disturbance”, OS only, x 1-3 weeks. ii. “Intermittent wavy lines”, worse a couple of days ago, with history of equal vision OD, OS iii. Denies pain, redness, photophobia but ? Associated headache. iv. POHX: Negative surgery or trauma v. Review of Systems: Depression with Wellbutrin prn tx. vi. FMHx/FOHx: Negative Playing the Field – A Review of the Visual Pathway and its Correlating Visual Field Defects a. Objectives i. Allows us to isolate the defect and its location in the visual pathway. ii. Allows us to describe the defect and monitor for stability, improvement, or progression. iii. Allows us to treat the defect and prevent progression b. Strategy for Lecture i. Review of visual pathway anatomy in the context of specific correlating visual fields. ii. Review how to select the appropriate visual field test. iii. Review how to interpret the selected visual field and watch for changes. “The Hill of Vision” a. Normal visual field (monocular) i. 50-60 degrees superiorly ii. 60 degrees nasally iii. 70-75 degrees inferiorly iv. 90-100 degrees temporally 1. Extent varies with stimulus size and age 2. Images on retina are projected opposite to the area of the retina being stimulated a. Example: Objects that stimulate nasal retina are situated in the temporal visual field. Analyzing data – static threshold a. Reliability Indices i. fixation losses ii. false positives iii. false negatives b. Decibel Values / Grey Scale c. Total Deviation d. Pattern Deviation e. Global Indices i. Mean Deviation (MD) ii. Pattern Standard Deviation (PSD) V. VI. iii. Short-term Fluctuation (SF) iv. Corrected Pattern Standard Deviation (CPSD) v. Probability (P) f. Glaucoma Hemifield test i. Five zones in the upper field and five zones in a mirror image location in the lower field are analyzed according to probabilities in pattern deviation plot 1. Results are summarized as a message 2. Not available for fastpac Comparison of multiple fields a. New defect b. Deepening of defect c. `Enlargement of defect d. General reduction of all points e. Progression is easy to over-call. If evidence of field progression is unexpected from other clinical findings, and especially if the change is only slightly greater than the minimal criteria, wait 3-6 months and repeat. f. Beware of: i. Learning curve ii. Effects of fatigue iii. Unexplained bad field iv. Long-term fluctuation v. Comparing two different perimeters vi. Comparing two different test algorithms Principles of Visual field Defects a. Monocular defect due to defect anterior to chiasm. b. Binocular defect due to either: i. Two lesions (one in each pre-chiasmal pathway) ii. One lesion in the chiasm or post chiasm pathway. VII. c. Congruity usually increases posteriorly Types of visual field Defects a. Altitudinal: Involves 2 quadrants of either the superior or inferior visual field i. Respects horizontal meridian (due to horizontal raphe) ii. Typically in ischemic optic neuropathies, sudden hypotension, hemorrhage, or anemia, or occipital lobe lesions affecting occipital lobe…and in ptosis. b. Arcuate: Due to selective damage to the superior or inferior NFL as they enter the optic nerve i. Common in glaucoma, optic neuritis, ischemic optic neuropathy, optic disc drusen c. Hemianopia: A complete defect involving half of visual field i. Congruous versus Incongruous VIII. IX. X. XI. ii. Heteronymous: Involves opposite sides of visual fields 1. Optic chiasm produces bitemporal defect iii. Homonymous: Involves same side of visual field in each eye 1. Lesions of retrochiasmal pathway d. Quadrantopsia: Complete defect involving a quadrant of each visual field. i. Heteronymous or Homonymous 1. Seen in Temporal, Parietal, or Occipital Lobe Lesions e. Scotomas: Absolute (all vision is lost) or Relative (variable vision is lost) area of depressed visual sensitivity surrounded by normal vision. i. Central: Involves fixation 1. Could be absolute or relative 2. Optic neuritis, ischemic and compressive optic nerve lesions f. Paracentral: An area of visual field defect within the central 30 degrees i. Usually elongated circumferentially ii. Glaucoma or papilledema g. Cecocentral: Visual field defect extending from fixation to the blind spot i. Due to disease of papillomacular bundle (toxic optic neuropathies, congenital optic disc pits with associated serous detachment, optic nerve tumors, toxic amblyopia Factors that affect sensitivity a. Anatomical facial features (prominent nose, brow) b. Ptosis: recommend taping lids c. Miotic Pupil (esp <2mm): depresses VF and can exaggerate size/depth of existing VF defect d. Uncorrected refractive error: enlarged blind spot or enlarged VF defects; correct >1D of error, age e. Cataract: reduces illumination, therefore general depression f. Attention g. Age of patient: sensitivity decreases with age due to NFL loss h. Technique of examiner Nerve Fiber PATTERN OF THE RETINA a. Retinal Visual field defects The Optic Disc and optic nerve a. All axons of NFL come together at optic disc in specific pattern (Fig A) and gradually move to final position in the optic nerve. i. Macular fibers take up ~1/3 of disc (although only accounts for 1/20 of retinal area) ii. Temporal and nasal fibers account for remaining 1/3 of disc each b. Optic nerve Visual Field Defects The Optic Chiasm a. Nasal fibers decussate to contralateral optic tract(~53%) and temporal fibers remain on ipsilateral side (~47%) XII. XIII. XIV. XV. i. Inf-nasal fibers loop anteriorly into the opposite posterior optic nerve and superior nasal fibers loop posteriorly prior to decussation. ii. Nasal macular fibers cross primarily in the posterior aspect of the chiasm iii. Most commonly due to pituitary adenomas but can include 1. Aneurysms 2. Multiple sclerosis 3. Craniopharyngiomas 4. Hydrocephalus 5. Optic nerve or chiasmal gliomas a. Can present as binasal or bitemporal defects (usually crossed fibers damaged first in compressive lesions). The Optic Tract a. Crossed and uncrossed fibers mingle en route to Lateral Geniculate Body to form superior peripheral, inferior peripheral, and macular fibers b. Optic tract Visual field Defects i. A homonymous visual field defect will occur postchiasmal…even with 20/20 vision. ii. Optic tract lesion will eventually result in optic atrophy iii. May produce a relative APD in the contralateral eye because the crossed fibers outnumber the uncrossed fibers. The lateral Geniculate Body a. Site of visual information processing (not just relay station) as retinal axons terminate here. i. Exiting fibers project to higher cortical centers ii. Layers 1,2= magnocellular layers iii. Faster speed of conduction iv. Mediates moving targets v. Layers 3-6= Parvocellular layers vi. Responsible for high-spatial-frequency contrast sensitivity b. Lateral Geniculate Body defects i. Lesions would affect contralateral field with associated optic atrophy but usually no pupillary defects Optic Radiations a. Radiates from LGB into the cerebral hemispheres, temporal lobe, or parietal lobe before terminating in the occipital lobe. i. Optic radiation visual field defects ii. Does NOT cause optic atrophy because it does not include retinal ganglion cell nerve fibers. iii. Results in contralateral homonymous field defect, usually only affecting one quadrant because the fibers are so spread out. Striate Cortex XVI. XVII. XVIII. XIX. a. Magno- and parvo-cellular layers of LGB project to specific areas and layers of the primary striate cortex (Brodman area 17) i. Performs basic analysis of information obtained from LGB and transmits on to higher visual association for further evaluation (Area 18, 19) Visual field defects of the Visual Cortex a. Cortex lesions usually produce highly congruous visual field defects b. Visual Field Defects of the Visual cortex MRI results of case history in Introduction Quiz slide References