* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Chapter 10: Normal Anatomy of the Spine: What You Need to Know
Survey
Document related concepts
Transcript
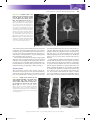
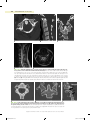
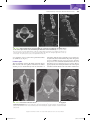
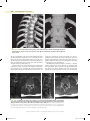
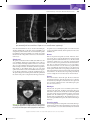
Normal Anatomy of the Spine: What You Need to Know 10 Bryan A. Pukenas, MD Learning Objectives 1.Understand relevant cervical, thoracic, and lumbar spinal anatomy. 2.Understand basic CT spinal imaging techniques. 3.Understand MRI pulse sequences relevant to spinal imaging. The spine is a vital functional unit that protects the spinal cord and supports the head, thorax, abdomen, and pelvis. Together, the rigid osseous structures combined with ligaments, disks, spinal cord, and spinal nerves facilitate complex motor and sensory functions required for life, be it work or play. Vertebral Body Anatomy Except in special circumstances, the vertebrae assume a relatively constant anatomic theme and consist of a vertebral body and a vertebral (neural) arch. The vertebral body serves as a pillar, supporting the head and trunk. The posterior margin of the bodies, along with the vertebral arches, forms the bony spinal canal, protecting the spinal cord. The neural arch is formed by paired pedicles and paired lamina. Seven processes arise from the vertebral arch: paired superior and inferior articular processes, paired transverse processes, and one spinous process. The intervertebral foramen, formed by two adjacent vertebrae, allows for passage of spinal nerves and vessels (1) (Fig. 10.1). The intervertebral disks consist of the inner nucleus pulposus and the outer annulus fibrosis. The main function of the disks is to distribute load and to allow flexion/extension and lateral bending. A remnant of the notochord, the nucleus pulposus, is usually located more dorsally compared to the center of the vertebral body. The annulus fibrosis attaches to the anterior longitudinal ligament (ALL) and posterior longitudinal ligament (PLL) and is also fused to the epiphyseal ring of the vertebral bodies. MRI of a normal disk demonstrates high signal on T2-weighted imaging related to the water content of the nucleus pulposus and inner annulus fibrosis. The outer annulus fibrosis demonstrates low signal on T1- and T2-weighted imaging (2) (Fig. 10.2). Cervical spine There are seven cervical vertebrae. The first and second cervical vertebrae are unique. The first cervical vertebra (axis or C1) has no body or spinous process and consists of an anterior and posterior arch. On the ventral surface of the anterior arch of C1 is the anterior tubercle, which serves as the attachment for the longus coli muscles. The dorsal concave aspect of the anterior arch articulates with the odontoid process of C2. Joining the anterior and posterior arches are the rather large lateral masses. The cup-shaped superior articular processes articulate with the occipital condyles to support the weight of the head. The flattened inferior articular processes articulate with C2, allowing for head rotation (1) (Fig. 10.3). The axis, or second cervical vertebra, forms from four ossification centers: two neural arches, the body, and the odontoid process. The dens, or odontoid process, projects superiorly from the body of the axis and serves as a pivot for the atlas (1). The os terminale is an additional ossification center at the tip of the dens that fuses with the odontoid process by age 3 to 6 (3). The pedicles and lamina are strong, and the vertebral canal is wide at this level, although smaller than at C1. The superior articular surfaces are rounded, directed superiorly and laterally, and supported by the body, pedicles, and transverse processes; the inferior articular surfaces assume a similar orientation to the adjacent lower vertebral body. The transverse processes end in a single tubercle and are small. The spinous process is large and usually bifid in nature (1) (Fig. 10.4). The C3 to C7 vertebral bodies are wider in the transverse diameter compared to the anteroposterior diameter with a concave upper surface forming the paired uncinate processes. The uncinate processes articulate with the adjacent superior vertebral body’s inferolateral surface to form the uncovertebral joints, located at the posterior and lateral margin on the intervertebral disk. The superior and inferior articular processes are fused, forming the articular pillars. The articular processes are flattened and oval in shape. The vertebral foramen is triangular in shape, formed by the pedicles and lamina posterolaterally. The posterior directed spinous process is usually bifid from C3 to C6 (1,4) (Fig. 10.5). The first through sixth vertebrae contain the foramen transversarium (see Fig. 10.3), which is demarcated by the anterior and posterior tubercles of the transverse processes, encasing the V2 segment of the vertebral arteries, the vertebral venous plexus, and sympathetic nerves (1,4). In a study by Bruneau et al., a high incidence of variation of the entry level of the V2 vertebral artery segment was observed. Ninety-three percent of vertebral arteries 194 Copyright © 2015 Wolters Kluwer, Inc. Unauthorized reproduction of the content is prohibited. 0002524859.INDD 194 8/4/2015 12:58:01 PM Normal Anatomy of the Spine: What You Need to Know 195 FIG. 10.1 ● A: Sagittal CT MIP of the lumbar spine demonstrating the vertebral body (B), pedicle (P), superior articular process (SAP), inferior articular process (IAP), and zygapophyseal joint (Z). The superior articular processes extend superiorly from the junction of the laminae and pedicles, while the inferior articular processes extend inferiorly from the undersurface of each lamina. The zygapophyseal joints are formed by the superior articular facet and the inferior articular facet. The pars interarticularis (PI) is the portion of the lamina between the superior and inferior articular processes. The intervertebral foramen (F) allows for the passage of spinal nerves and vessels. B: Axial CT MIP of the lumbar spine demonstrating the vertebral body (B) and posterior neural arch. (P, pedicle; TP, transverse process; L, lamina; SP, spinous process.) entered the C6 foramen transversarium, but the entry level varied from the C3 to C7 foramen transversarium. In 2.0% of specimens, a medial loop was present medial to the border of the uncovertebral joint or into the intervertebral foramen (5). Reporting vascular variants to referring clinicians is of paramount importance when spinal interventions are planned. The cervical neural foramina are oriented at 45-degree angles with respect to the coronal plane and about 10 degrees downward with respect to the axial plane. In the neutral position, the cervical spinal nerves are located in the inferior neural foramen, at or below the disk level (6). However, their position and size of the neural foramina may vary depending on neck positioning (7). Thoracic spine There are 12 thoracic vertebrae, each consisting of a body, vertebral arches, and seven processes. The superior articular facets arise from the superior articular processes, and inferior articular facets arise from the inferior articular processes (4). The upper and midlevel paired thoracic facet joints are oriented in the coronal plane, while the cervicothoracic joints are oriented in the axial plane and the thoracolumbar joints are oriented in the sagittal plane (Fig. 10.6) (8). This relationship becomes important when contemplating thoracic facet joint injections. The thoracic spinous processes project from the vertebral arches and slope inferiorly. Located at the level of the intervertebral disk, the costal facets articulate with the rib heads. From T2 to T9 levels, these demifacets are paired, where the superior and inferior costal demifacets span two adjacent vertebral bodies (T2 to T9) and articulate with the rib heads. When there are paired demifacets, the more inferior vertebral body identifies its corresponding rib (the third rib articulates with the inferior costal facet of T2 and the superior costal facet of T3) (4). Four thoracic vertebral bodies (T1, T10, T11, T12) have variant anatomy. The superior costal facet of T1 is not a demifacet (i.e., the T1 rib only articulates with T1). The T1 inferior costal facet assumes the usual thoracic anatomy FIG. 10.2 ● Sagittal T2 fat-saturated (A) and axial T2-weighted (B) MRIs of the lumbar spine demonstrating high signal intensity in the nucleus pulposus (NP) and inner annulus fibrosis and decreased signal in the outer annulus fibrosis (AF). The anterior longitudinal ligament (ALL) is not well seen, but the posterior longitudinal ligament (PLL) is seen as a continuous band of signal hypointensity along the posterior vertebral body. The ligamentum flavum (LF) is also seen posteriorly in the spinal canal. Copyright © 2015 Wolters Kluwer, Inc. Unauthorized reproduction of the content is prohibited. 0002524859.INDD 195 8/4/2015 12:58:02 PM 196 NEUROIMAGING: The Essentials FIG. 10.3 ● Axial (A), sagittal (B), and coronal (C) cervical spine CTs demonstrating the anterior (A) and posterior (P) arches of C1 as well as the foramen transversarium (FT). Note the anterior tubercle (white arrow). Although the vertebral artery is not seen, its course runs through the arcuate foramen (AF), whose floor is present bilaterally. The cup-shaped superior articular processes (SAP) articulate with the occipital condyles (OC). The dens (D) is seen extending from the body of C2. Two small tubercles (black arrow) are seen on the medial borders of C1, serving as anchors for the transverse ligament, which secures the dens and allows for lateral rotation of C1 on C2. Sagittal (D) and axial (E) T2-weighted MRIs demonstrating the anterior (ALL) and posterior (PLL) longitudinal ligaments and the ligamentum flavum (LF). The vertebral artery (VA) flow voids are seen within the foramen transversarium. FIG. 10.4 ● Axial maximal intensity projection (MIP) (A), coronal (B), and sagittal (C) reformatted images of the cervical spine demonstrating the superiorly projecting odontoid process (O), pedicles (P), lamina (L), and the spinal canal (C) are also noted. Note the rounded shape of the superior articular process (SAP) and the more “normal” appearance of the inferior articular process (IAP) on the sagittal MIP. The transverse processes (TP) end in a single tubercle. The spinous process (SP) is bifid in nature. Copyright © 2015 Wolters Kluwer, Inc. Unauthorized reproduction of the content is prohibited. 0002524859.INDD 196 8/4/2015 12:58:02 PM Normal Anatomy of the Spine: What You Need to Know 197 FIG. 10.5 ● Axial maximal intensity projection (MIP) (A), coronal (B), and sagittal (C) reformatted images of the cervical spine inferior to C2 demonstrating the wide nature of the vertebral body. The paired uncinate processes (U) are seen articulating with the adjacent vertebral body, forming the uncovertebral joint (arrow). The superior and inferior articular processes form the articular pillars (AP). Notice the triangular appearance of the spinal canal (C). The spinous process (SP) is usually bifid from C3 to C6. (it is a demifacet). T10, T11, and T12 have paired bilateral facets (no demifacets) (4) (Fig. 10.7). Lumbar spine There are five lumbar vertebrae. The lumbar vertebral bodies are thick and wide, with short pedicles and laminae. The inferior articular processes extend inferiorly from the undersurface of A B each lamina, while the superior articular processes extend superiorly from the junction of the laminae and pedicles. The spinous processes, mamillary processes, accessory processes, and transverse processes serve as muscular attachments and, in the case of the transverse processes and spinous processes, as levers. The zygapophyseal joints are formed by the medial border of the superior articular facet and the lateral border of the inferior articular facet. C FIG. 10.6 ● A: Coronal CT of the cervicothoracic spine demonstrating the axial orientation of the zygapophyseal joints (arrow). B: Axial CT of the midthoracic spine demonstrating the coronal orientation of the zygapophyseal joints (arrow). C: Axial CT of the thoracolumbar junction demonstrating the sagittal orientation of the thoracolumbar joints (arrow). Copyright © 2015 Wolters Kluwer, Inc. Unauthorized reproduction of the content is prohibited. 0002524859.INDD 197 8/4/2015 12:58:04 PM 198 NEUROIMAGING: The Essentials B A FIG. 10.7 ● Coronal 3D volume rendered image of the midthoracic spine (A) demonstrating rib articulation with demifacets (arrows) and the lower thoracic spine (B) demonstrating rib articulation with “traditional” facets (arrow). The pars interarticularis is the portion of the lamina between the superior and inferior articular processes, an area that may experience excessive forces during spinal motion (9) (see Fig. 10.1). The intervertebral or neural foramen is larger than in the thoracic spine, but smaller than in the cervical spine, while the inferior vertebral notches are relatively large (1). The lateral recess is an area in the lumbar spine bordered laterally by the pedicle, posteriorly by the superior articular facet, and anteriorly by the vertebral body and intervertebral disk. Hypertrophy of the superior articular facet may cause nerve root compression at the superior border of the pedicle (10). The subpedicular notch, located in the anterior and superior portion of the intervertebral foramen, is the usual location of the dorsal root ganglion (DRG) and exiting nerve root, although its location may vary depending on the spinal level (11). The lumbar intervertebral foramen is a keyhole- or inverted teardrop–shaped area bordered anteriorly by vertebral bodies and intervertebral disk, posteriorly by the ligamentum flavum and superior and inferior articular facets, and superiorly and inferiorly by the adjacent pedicles (11) (Fig. 10.8). The foraminal FIG. 10.8 ● Sagittal T2- (A), axial T2- (B), sagittal T1- (C), and axial T1 (D)-weighted images of the lumbar spine at the level of the neural foramen demonstrate the key hole-shaped appearance of the neural foramen (NF) (A,C) with the exiting nerves (N) in the intervertebral foramen (B,D). Notice the U-shaped appearance of the spinal nerves within the thecal sac (black arrowhead). The ligamentum flavum (LF) is seen as a thick band of decreased signal along the ventral aspect of the lamina. The psoas (P) muscles are also well seen. Epidural fat is present as high signal intensity of T1- and T2-weighted images (black arrow). Copyright © 2015 Wolters Kluwer, Inc. Unauthorized reproduction of the content is prohibited. 0002524859.INDD 198 8/4/2015 12:58:05 PM Normal Anatomy of the Spine: What You Need to Know 199 FIG. 10.9 ● Sagittal (A) and axial (B) T2-weighted MRIs demonstrating the conus medullaris (arrow) in axial plane terminating at the level of the inferior endplate of L1 as correlated with the sagittal image. zone and extraforaminal zone are two locations that radiologists should be familiar with, as they have an increased likelihood of entrapment by disk herniation. The area underneath the pedicle but within the canal is the foraminal zone, and the area outside the lateral border of the pedicle is referred to as the extraforaminal zone (12). Spinal cord The spinal cord extends from the medulla at the skull base to the conus medullaris, which is the tapered distal portion of the spinal cord, usually terminating anywhere from T12 to L2-L3 level (Fig. 10.9). The centrally located gray matter appears as a hyperintense H-shaped structure surrounded by the more hypointense white matter on T2-weighted images (Fig. 10.10). The cauda equina extends inferior to the conus medullaris and often appears in a U-shaped configuration on axial T2-weighted imaging (2). The paired collagenous dentate ligaments divide the spinal canal into anterior and posterior compartments and may penetrate into the spinal cord (13). Caudally, the spinal cord is anchored to the coccyx by the filum terminale, which originates from the conus medullaris (14). Nerves There are 31 spinal cord segments (8 cervical, 12 thoracic, 5 lumbar, 5 sacral, and 1 coccygeal). All but the first cervical segment (C1) have paired dorsal and ventral nerve roots. The first cervical segment has ventral nerve roots only. These dorsal and ventral nerve roots unite to form a spinal nerve in the intervertebral foramen. Prior to joining the ventral nerve root, an ovoid enlargement of the dorsal nerve root, the dorsal root ganglion (DRG), can be seen within the spinal canal. The C1 to C7 spinal nerves exit the spinal canal above the corresponding vertebral body. The 8th cervical spinal nerve exits between C7 and T1 levels. All spinal nerves inferior to T1 exit below the corresponding vertebral body (14). For example, the T1 nerve exits between T1 and T2 levels. Curves Three main curvatures exist in the spine. The most rostral is the cervical lordosis that arcs from the odontoid process to the midT2 vertebral body. The kyphosis of the thoracic curve spans from T2 to T12 levels, while the lordosis of the lumbar spine spans from T12 to the sacrum (1). Meninges Like the brain, the spinal cord is surrounded by three meningeal layers: the dura mater, arachnoid, and pia mater. The space between the vertebral bodies and the dura is called the epidural space and contains a layer of fat and Batson plexus, a network of epidural veins. The subdural space is a potential space between the dura mater and arachnoid layer. The subarachnoid space contains cerebrospinal fluid and separates the arachnoid from the pia mater (14). Vascular supply FIG. 10.10 ● Axial GRE T2* imaging of the cervical spine demonstrating the hyperintense H-shaped centrally located gray matter (arrow) surrounded by the relatively hypointense white matter. The arterial supply to the cervical spinal cord is variable, where spinal arteries may arise from the vertebral arteries, deep and ascending cervical arteries, costocervical trunk, and thyrocervical trunk. Copyright © 2015 Wolters Kluwer, Inc. Unauthorized reproduction of the content is prohibited. 0002524859.INDD 199 8/4/2015 12:58:05 PM 200 NEUROIMAGING: The Essentials Above the T3 level, the supreme intercostal arteries s upply the upper thoracic spine. These branches often arise from the costocervical trunks or aortic arch and rarely from the vertebral arteries. The paired segmental arteries, arising from the aorta, supply the spinal column, paraspinal muscles, dura, nerve roots, and spinal cord from the level of T3 inferiorly. A branch of the segmental artery, the spinal trunk, enters the intervertebral foramen and then divides into the anterior and posterior spinal arteries and a radicular artery that supplies the dura and nerve root at each level. At some levels, the radicular arteries supply the spinal cord and are denoted as radiculomedullary arteries, which in turn feed the anterior spinal artery (ASA). The ASA supplies the anterior two-thirds of the spinal cord and is formed at the level of the foramen magnum and traverses inferiorly along the surface of the spinal cord to the conus, where it terminates in a branch to the filum terminale. There are anterior radiculomedullary arteries supplying the ASA in the cervical region (Fig. 10.11) as well as the thoracic and lumbar regions. The two posterior spinal arteries also traverse from the foramen magnum and supply the posterior one-third of the spinal cord. The anterior median spinal vein runs with the ASA, and there are 2 to 3 posterior veins, the largest is typically the posterior median vein (15). The uppermost extension of the PLL, the tectorial membrane, attaches to the anterolateral foramen magnum. The transverse ligament courses between the tubercles of C1 and the apical ligament spans from the dens to the foramen magnum (1). The alar ligaments connect the lateral dens and the medial inferior occipital condyles (3). The ligamentum flavum, ALL, and PLL are linear low-signal intensity structures, best seen on sagittal MRI images (Fig. 10.2). Ligaments Magnetic resonance imaging The anterior and posterior atlanto-occipital membranes course from the upper portion of C1 to the anterior and posterior portions of the foramen magnum. The atlantoaxial ligament extends from the mid dens to the inferior aspect of the C1 anterior arch. The exquisite soft tissue contrast provided by MRI makes this modality particularly useful in the evaluation of the spine. Indications for spine evaluation with MRI include evaluation of degenerative conditions, trauma, and neoplastic disorders, among other indications. The lack of ionizing radiation afforded by MRI may play a role in the evaluation of the cervical, thoracic, and lumbar spine, by avoiding radiation exposure to the thyroid gland and gonads, respectively. A variety of pulse sequences are available for MRI spine evaluation, but commonly, axial and sagittal T1 and T2-weighted sequences are performed. Depending on the indication, additional sequences may be obtained, including short tau inversion recovery (STIR) or pre- and postcontrast fat-saturated images. Since CSF flow in the cervical and thoracic spine is more dynamic than in the lumbar spine, T2* sequences are usually obtained since they are less sensitive to CSF flow-related artifacts than T2 fast spin-echo sequences. In the lumbar spine, T1 axial images show excellent tissue contrast between the highsignal epidural fat, low-signal CSF, and intermediate-signal disks (18). Bone marrow imaging is important when assessing patients with suspected infiltrating processes such as infections and metastatic disease. Standard T1- and T2-weighted images can be used to detect abnormalities in the marrow. However, these routine sequences are often nonspecific, since many process that replaces the normal fatty marrow can be seen as low signal on T1-weighted imaging (19). Fat-suppressed imaging, including STIR imaging, can increase lesion conspicuity (20); however, T2-weighted fatsaturated and STIR images may be degraded by variations in the local magnetic field and uneven fat suppression (19). Gradient in-phase and out-of-phase imaging is another tool to help distinguish between physiologic and pathologic processes in the bone marrow. In the adult, hematopoietic marrow contains both watercontaining elements and fat-containing elements. Since water and fat resonate at slightly different frequencies, the signal within the voxel will decrease when comparing out-of-phase to in-phase images when both water and fat elements are present in the same FIG. 10.11 ● Coronal MIP dynamic contrast MRA of the cervical spine demonstrating the artery of cervical enlargement (arrow) supplying the anterior spinal artery (arrowheads, ASA). Imaging Computed tomography CT is the modality of choice for imaging bony structures of the spine, particularly in the setting of trauma and postsurgical evaluations. The advantages of CT include rapid image acquisition and the ability to reconstruct and reformat images in different planes. Images are typically acquired using contiguous or overlapping axial slices with orthogonal reconstructed images. Reconstructed scan thickness should be no greater than 3 mm, and depending on the specific imaging indication, the slice thickness should range from 1 to 3 mm (16,17). Copyright © 2015 Wolters Kluwer, Inc. Unauthorized reproduction of the content is prohibited. 0002524859.INDD 200 8/4/2015 12:58:05 PM Normal Anatomy of the Spine: What You Need to Know 201 FIG. 10.12 ● Sagittal in-phase (A) and out-of-phase (B) T1-weighted images demonstrating normal signal dropout on out-of-phase imaging in the normal bone marrow caused by the presence of fat- and water-containing molecules in the same voxel (rectangles). voxel (19) (see Fig. 10.12). Normal or benign marrow has a signal intensity ratio of less than 0.8 (in-phase/opposed phase), while lesions with a signal intensity ratio of greater than 0.8 are considered malignant (sensitivity 0.95; specificity 0.89) (21). Conclusion Imaging of the spine plays an ever increasingly important role in the diagnosis and treatment of spinal disorders. Familiarity with basic anatomy and imaging techniques allows the radiologist to tailor image acquisition for specific disease indications and provides a solid foundation when evaluating pathologic conditions. Take Home Points 1. C1 and C2 are unique in their anatomy and function. 2. The remaining vertebral bodies are similar in form, with variations depending on function (cervical spine allows for head movement, thoracic spine is more rigid to provide protection of vital organs, while the lumbar spine supports most of the weight of the torso.) 3. CT evaluation of the spine should be performed in 3 planes. 4. MRI should be tailored toward the clinical question (for example, in-/out-of-phase imaging for marrow evaluation). References 1. Gray H. Anatomy of the Human Body. Philadelphia, PA: Lea & Febiger; 1918. 2. Harnsberger HO, Ross JS, Moore KR, eds. Diagnostic and Surgical Imaging and Anatomy. Salt Lake City, UT: Amirsys; 2006. 3. Lustrin ES, Karakas SP, Ortiz AO, et al. Pediatric cervical spine: normal anatomy, variants, and trauma. Radiographics. 2003;23(3):539–560. 4. Moore KL, Dalley AF, Agur AM. Clinically Oriented Anatomy. Philadelphia, PA: Wolters Kluwer Health; 2013. 5. Bruneau M, Cornelius JF, Marneffe V, et al. Anatomical variations of the V2 segment of the vertebral artery. Neurosurgery. 2006;59 (1 suppl 1):ONS20–ONS24. 6. Pech P, Daniels DL, Williams AL, et al. The cervical neural foramina: correlation of microtomy and CT anatomy. Radiology. 1985;155(1):143–146. 7. Reid JD. Effects of flexion-extension movements of the head and spine upon the spinal cord and nerve roots. J Neurol Neurosurg Psychiatry. 1960;23(3):214–221. 8. McLain RF, Pickar JG. Mechanoreceptor endings in human thoracic and lumbar facet joints. Spine (Phila Pa 1976). 1998;23(2):168–173. 9. Bogduk N. Clinical Anatomy of the Lumbar Spine and Sacrum. Philadelphia, PA: Elsevier; 2005. 10. Ciric I, Mikhael MA, Tarkington JA, et al. The lateral recess syndrome: a variant of spinal stenosis. J Neurosurg. 1980;53(4):433–443. 11. Jenis LG, An HS. Spine update. Lumbar foraminal stenosis. Spine (Phila Pa 1976). 2000;25(3):389–394. 12. Arslan M, Comert A, Acar HI, et al. Nerve root to lumbar disc relationships at the intervertebral foramen from a surgical viewpoint: an anatomical study. Clin Anat. 2012;25(2):218–223. 13. Ceylan D, Tatarli N, Abdullaev T, et al. The denticulate ligament: anatomical properties, functional and clinical significance. Acta Neurochir (Wien). 2012;154(7):1229–1234. 14. Bican O, Minagar A, Pruitt AA. The spinal cord: a review of functional neuroanatomy. Neurol Clin. 2013;31(1):1–18. 15. Santillan A, Nacarino V, Greenberg E, et al. Vascular anatomy of the spinal cord. J Neurointerv Surg. 2012;4(1):67–74. 16. Sixta S, Moore FO, Ditillo MF, et al. Screening for thoracolumbar spinal injuries in blunt trauma: an Eastern Association for the Surgery of Trauma practice management guideline. J Trauma Acute Care Surg. 2012;73(5 suppl 4):S326–S332. 17. ACR–ASNR–ASSR–SPR practice parameter for the performance of computed tomography (CT) of the spine; 2011. Amended 2014 (Resolution 39). 18. ACR–ASNR–SCBT-MR practice guideline for the performance of magnetic resonance imaging (MRI) of the adult spine; 2012. Amended 2014 (Resolution 39). 19. Plecha DM. Imaging of bone marrow disease in the spine. Semin Musculoskelet Radiol. 2000;4(3):321–327. 20. Mirowitz SA, Apicella P, Reinus WR, et al. MR imaging of bone marrow lesions: relative conspicuousness on T1-weighted, fat-suppressed T2-weighted, and STIR images. AJR Am J Roentgenol. 1994;162(1): 215–221. 21. Erly W, Oh E, Outwater E. The utility of in-phase/opposed-phase imaging in differentiating malignancy from acute benign compression fractures of the spine. AJNR Am J Neuroradiol. 2006;27(6):1183–1188. Copyright © 2015 Wolters Kluwer, Inc. Unauthorized reproduction of the content is prohibited. 0002524859.INDD 201 8/4/2015 12:58:06 PM 202 NEUROIMAGING: The Essentials Chapter Self-Assessment Questions 1. The abnormality is in what space? A. Epidural B. Subdural C. Subarachnoid D. Prevertebral E. Paravertebral 2. The black arrow indicates which of the following normal anatomic structures? A. An uncovertebral joint B. The C6 foramen transversarium C. The C7 spinal nerve D. The deep cervical artery E. The lamina Answers to Chapter Self-Assessment Questions 1. A Epidural. An extra-axial lesion is present, consistent with an epidural hematoma. 2. B The left vertebral artery is seen in the foramen transversarium. The patient is slightly rotated, and the right vertebral artery is seen just prior to entering the foramen. The vast majority of vertebral arteries enter the foramina transversarium at the C6 level. Copyright © 2015 Wolters Kluwer, Inc. Unauthorized reproduction of the content is prohibited. 0002524859.INDD 202 8/4/2015 12:58:07 PM