* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download 9-13-04 Factors Affecting Action of Drugs
Survey
Document related concepts
Plateau principle wikipedia , lookup
Specialty drugs in the United States wikipedia , lookup
Compounding wikipedia , lookup
Polysubstance dependence wikipedia , lookup
Orphan drug wikipedia , lookup
Drug design wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Psychopharmacology wikipedia , lookup
Drug discovery wikipedia , lookup
Pharmacognosy wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Neuropharmacology wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Prescription costs wikipedia , lookup
Transcript
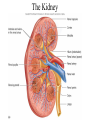
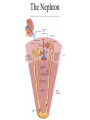
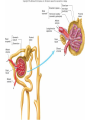
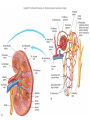
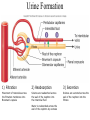
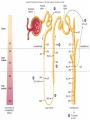
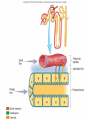
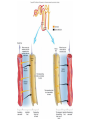
Absorption/Distribution • Drug effects are affected by Absorption and Distribution – Absorption refers to the entrance of drug into the blood stream – Distribution refers to distribution to the various tissues once in the blood Drug Forms • Aqueous – Water and sugar and added drug • Alcoholic – Drug dissolved in EtOH (520%) • Solid • Capsules – Gelatin dissolves in stomach releasing drug • Delayed –release – 2-3 single doses released over time • Enteric coated – Acid resistant covering prevents digestion in stomach • Suppositories – Self explanatory • Ointments – Petrolatum or lanolin for topical absorption • Transdermal – Bandage or patch and absorbed through skin for up to 24 h Routes of Administration • Oral (PO) – Safest and most convenient – Typically takes 30-60 min for appearance in blood – Can be removed by gastric lavage or induced vomiting • Parenteral – Any route that does not involve GI tract Parenteral Administration • IM – Intramuscular injections- short action (min) • Gluteals or deltoids – Gluteals and sciatic nerve • IV – Intravenous injection – immediate action • Directly into bloodstream • Drug cannot be withdrawn once administered • Inhalation – short action – Nose, mouth into lungs during inspiration The Five Rs • • • • • Right patient Right drug Right dose Right route Right time Absorption • Drug must be dissolved in body fluids • Drugs must pass through membranes (except IV administration) – GI – Blood vessels – Many drugs rely on passive diffusion to be absorbed (concentration gradient) • Absorption affected by – Lipid solubility • More fat soluble compounds diffuse easily across membranes – Drug ionization • Like Na+ and Cl- ions do not diffuse readily across membranes • Basic drugs (aspirin) are un-ionized in the stomach and more readily absorbed • Acidic drugs (morphine, streptomycin) un-ionized in lower GI and more readily absorbed • Liquid formulations are typically absorbed more quickly • Solid tablets or capsules must dissolve in body fluids before they can be absorbed – Slows down the absorption process Drug Distribution • Distribution of drug to tissues affected by factors such as – plasma protein binding – Blood flow – Blood brain barrier Plasma Protein Binding • Primarily albumin and globulins – Proteins help regulate osmotic balance • Many drugs attracted to proteins – Some are bound to proteins – Some are unbound (free to circulate) – Only unbound drugs exert effect Blood Flow • Various organs receive different blood flow • Liver, kidneys and brain have largest supply – These organs exposed to largest amounts of drugs • Adipose has poor supply – Does not receive large amounts of drugs – Lipid soluble drugs can accumulate Blood Brain Barrier • An extra layer of lipid membrane that protects the brain – Water soluble compounds do not cross blood brain barrier effectively – Drugs that are intended to act on the brain must have a lipid soluble chemistry • E.g benzodiazepines treat anxiety and convulsions • Some antibiotics are not lipid soluble and cannot treat infections of the brain Drug Metabolism • Conversion of foreign substances to chemical forms that can be eliminated (biotransformation) – Renal, intestinal, respiratory • Main organ of transformation is liver • Drug microsomal metabolizing system or cytochrome P450 system • Converts lipid soluble compounds to water soluble – Easily eliminated in the urine • Metabolic conversions can inactivate drugs by converting to more easily excretable form – Also typically less active at receptor • Conversions can also activate “pro-drugs” – E.g. codeine is metabolized to morphine a more potent form of opiates Phase I and Phase II reactions • Phase I – Drug is oxidized or reduced to more polar form • More readily excreted • Phase II – Drug is conjugated to glutathione • Increases the polarity of the drug even more • Phase II is not dependent on phase I although often happens after I Induction • Liver P450 system responsible for Phase I reactions • P450 can be induced by consistent drug administration – E.g. chronic alcohol use • Increases metabolism and excretion of drug resulting in tolerance Inhibition • Co-incidental administration of two drugs metabolized by same P450 system will result in inhibition of conversion of each of the drugs – Can result in increased potency, duration of action of drug – May often result in adverse effects First Pass Metabolism • Drugs that are orally administered are absorbed and pass into portal circulation • These drugs pass through liver prior to distribution • Many of these drugs are metabolized (activated or inactived) extensively • Protective mechanism Excretion • Three primary routes of excretion – Renal – urine – GI – feces – Respiratory – exhaled gases • Kidney is primary organ of excretion Renal Excretion • Blood is filtered through the glomerulus of the kidneys – Most filtered substances are eventually reabsorbed – exceptions- urinary waste products • Waste products are water soluble and usually ionized • So, .. Excreted drugs must be water soluble and ionizable The Kidney The Nephron Urine Formation 1) Filtration 2) Reabsorption 3) Secretion Movement of materials across the filtration membrane into Bowman’s capsule Solutes are reabsorbed across the wall of the nephron into the interstiial fluid Solutes are secreted across the wall of the nephron into the filtrate Water is reabsorbed across the wall of the nephron by osmosis GI Excretion • After oral administration, unabsorbed drug passes through GI tract and is excreted in feces • Some drugs can be reabsorbed in the intestinal tract Respiratory Excretion • Typically, general anesthetic gases are not totally absorbed – Remnants exhaled • Some drugs are metabolized to products that can leave exchange with blood and air in lungs – Exhaled also Half Life • Time required for the concentration of a drug in the blood to fall to half of its original level • Dependent on ADME • Affected by liver or kidney disease • Necessary to determine dosing regimen Bioavailability • Amount of drug that is actually absorbed into the blood stream • Dependent on route of administration – E.g. drugs with high First Pass metabolism will not have good oral bioavailability – Necessary to administer parenterally Patient Profile • • • • • • • Age Pregnancy Smoking and drinking Liver or kidney desease Pharmacogenetics Drug interactions Psychological factors Age • Drug metabolism (P450) enzymes – Underdeveloped in young – Compromised in elderly – Adult dosages may not be extrapolated to children or elderly Pregnancy • Drug effects in pregnant women can have drastic effects on unborn, or no effects at all – FDA pregnancy categories – Teratogenic drugs – Drugs affecting breast feeding Smoking and Drinking • Both induce P450 enzymes • Can effectively lower effective drug concentration in blood • Can more activate pro-drugs more effectively Liver or Kidney Disease • A damaged liver will metabolize drugs to a lesser extent – Can result in greater or lesser active drug • Damaged kidneys excrete less drug metabolites