* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download analg_opioide_Engl_2013
Survey
Document related concepts
NMDA receptor wikipedia , lookup
Discovery and development of ACE inhibitors wikipedia , lookup
5-HT2C receptor agonist wikipedia , lookup
5-HT3 antagonist wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Discovery and development of cyclooxygenase 2 inhibitors wikipedia , lookup
Discovery and development of angiotensin receptor blockers wikipedia , lookup
Nicotinic agonist wikipedia , lookup
Paracetamol wikipedia , lookup
Toxicodynamics wikipedia , lookup
Cannabinoid receptor antagonist wikipedia , lookup
Dextropropoxyphene wikipedia , lookup
Neuropharmacology wikipedia , lookup
NK1 receptor antagonist wikipedia , lookup
Transcript
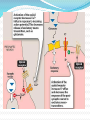
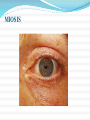
ANALGESICS TYPES OF PAIN symptom Pain disease physological pain acute Pain chronic pathological PAIN CLASIFICATION somatic nociceptive visceral pain neuropatic nonnociceptive psyhogenic R. Kannev, Pain Management Secrets, 1997 TREATMENT OF PAIN Local anesthetics Infiltration Intravenous Epidural Intrarahidian General anesthetics : Inhalatory Intravenous Intrarectal Epidural TREATMENT OF PAIN Analgesics Opioids Natural Semisynthetics synthetics Non-opioids Inhibitors of COX1,2,3 Alfa 2 agonists 5HT agonists NMDA antagonists TREATMENT OF PAIN Class/ Representatives Coanalgezics: Tricyclic antidepressants; neuroleptics; anticonvulsantants; Muscle rrelaxants; calcitonine; adenosinee; metoclopramide; Paraanalgessics: Corticoids (in inflammatory pain); nitrite (in pectoris angina); antacids (ulcer disease); acetazolamide (in glaucomas). Calcium channel blockers; cannabinoidds; GABA-agonists; L-dopa; capsaicine; anti-arrhythmias; antivirals. CHRONOLOGICAL MARKERS 1803 1874 1939 1952 1971-1974 1974 -1975 1976-1986 ↓ Morphin isolation from opium Heroine – semisynthesis Petidine – synthesis total synthesis of morphyn Isolation of opioid receptors Isolation of encephalins Isolation of endorphines the list goes on…. Non-opioid analgesics Opioid analgesics Drugs for neuropathic and functional pain Antimigraine drugs NONOPIOID ANALGESICS Acetaminophen (paracetamol) NSAIDs – non selective - Selective Cox 2 inhibitors ANALGESICS-ANTIPIRETICS-NONSTEROIDAL ANTIINFLAMMATORY AGENTS Non selective inhibitors of COX • Organic acids • Salicitats – acetic acid, sodium salicilate, diflunisal, sulfasalazine, olsalasine • Heteroaril acetic acid deriv – indometacin, sulindac • Aril propionic deriv – tolmetin, diclofenac, ketorolac • Arilpropionic deriv – ibuprofen, naproxen, flurbiprofen • Antranilic deriv (fenamats) – mefenamic acid, meclofenamic acid • Enolic acid deriv – piroxicam, meloxicam • Non acidic compounds • Pirazolone deriv – metamizol (dipyrone) • Para-amino-fenol deriv – acetaminofem, fenacetine • Fenazone deriv – fenazone, propifenazone ANALGESICS-ANTIPIRETICS-NONSTEROIDAL ANTIINFLAMMATORY AGENTS Selective inhibitors of COX2 • Sulfonanilide – nimesulide • Coxibi (furanone/pirazolone diaril-substitute) – rofecoxib, celecoxib • Indol-acetic acids - etodolac NSAIDs Classifications Mild to moderate anti-inflammatory action propionic acid derivatives ibuprofen, naproxen fenamic acids mefanamic acid Marked anti-inflammatory action - salicylic acids pyrazolone derivatives - acetic acid derivatives oxicam derivatives Selective COX2 inhibitors aspirin azapropazone, phenylbutazone diclofenac, indomethacin piroxicam celecoxib, rofecoxib Aspirin (acetyl salicylate) Actions Analgesic - central and peripheral action Antipyretic - act in hypothalamus to lower the set point of temperature control elevated by fever, also causes sweating anti-inflammatory - inhibition of peripheral prostaglandin synthesis respiratory stimulation - direct action on respiratory centre, indirectly by ↑ CO2 production Aspirin (acetyl salicylate) Metabolic effects ↑peripheral O2 consumption (uncoupled oxidative phosphorylation) hence ↑CO2 production with ↑ respiration, and direct analeptic action - respiratory alkalosis renal loss of bicarbonate with sodium, potassium and water Dehydration metabolic acidosis - effects on Krebs cycle, ↑ ketone body, salicylic acid in blood, renal insufficiency due to vascular collapse, dehydration hypoglycaemia or even hyperglycaemia can occur Aspirin (acetyl salicylate) Uricosuric effects reduces renal tubular reabsorption of urate but treatment of gout requires 5-8g/d, < 2g/d may cause retention of urate antagonises the uricosuric action of other drugs Reduced platelet adhesion – irreversible inhibition of COX by acetylation, prolongs bleeding time, useful in arterial disease Note: low doses are adequate for this purpose since the platelet has no biosynthetic capacity and can not regenerate the enzyme Hypothrombinaemia : occurs with large doses ie >5g/day Aspirin (acetyl salicylate) OVERDOSAGE Ingestion of > 10 g can cause moderate/severe poisoning in an adult Clinical features - ‘salicylism’ Tremor Tinnitus Hyperventilation Nausea Vomiting sweating Management- mainly supportive PARACETAMOL (acetaminophen) equivalent analgesic efficacy to aspirin no useful anti-inflammatory action used for mild to moderate pain, but aspirin is preferred if due to inflammatory process PARACETAMOL (acetaminophen) Metabolism is conjugated in the liver as the inactive glucuronide and sulphate a number of minor oxidation products N-acetylbenzoquinoneimine (NABQI) are also formed NABQI is highly chemically reactive and is usually inactivated by conjugation with SH (thiol) groups of glutathione Supply of glutathione is limited and exhausted in overdose NABQI then reacts with cellular macromolecules and causes cell death PARACETAMOL (acetaminophen) Adverse effects rare in therapeutic usage occasional skin rash and allergy overdose can result in fulminant hepatic necrosis and liver failure PARACETAMOL (acetaminophen) Paracetamol overdose Ingestion of >10g of paracetamol may be fatal may be lower in chronic alcoholics or subjects with underlying liver disease. Clinical features In severe poisoning up to 24 hours – none/nausea and vomiting > 24 hours nausea and vomiting Right upper quadrant pain jaundice encephalopathy PARACETAMOL (acetaminophen) Management Blood for paracetamol at 4 hours post ingestion Check treatment curve for N-acetylcysteine infusion ( if in doubt of severe poisoning, don’t delay) Check prothrombin time and plasma creatinine, pH acute renal (due to acute tubular necrosis) and hepatic failure and occur at 36-72 hours after ingestion Indications for referral to liver unit are rapid development of Grade 2 encephalopathy PTT >45 secs at 48 hours or >50 secs at 72 hours rising plasma creatinine Arterial pH <7.3 more than 24 hours after ingestion NSAIDs Mechanism of action inhibits cyclo-oxygenase (prostaglandin synthase) that is responsible for conversion of arachidonic acid to cyclic endoperoxides 2 isoforms of enzyme - COX-1 constitutive, present in platelets, stomach and kidney COX-2inducible by cytokines & endotoxins at sites of inflammation e.g., joints NSAIDs Main actions 1.) Analgesic -effective against mild to moderate pain, do not cause dependence 2.) Anti-inflammatory 3.) Anti-pyretic 4.)Anti-platelet- prevent thromboxane production, derived from prostaglandins and cause platelet aggregation Others 5.) Useful in treatment of dysmenorrhea, associated with increased prostaglandin synthesis and increased uterine contractility 6.) Used to close the patent ductus arteriosus NSAIDs Adverse effects 1.) Gastric or intestinal mucosal damage - mucosal prostaglandins inhibit acid secretion, promote mucus secretion, prevent back diffusion of acid into the gastric submucosa - Inhibition thus results in erosions, ulceration, bleeding, perforation 2.) Disturbances of fluid and electrolyte balance - inhibition of renal prostaglandin production results in sodium retention and oedema, possible hyponatraemia, hyperkalaemia, antagonism of anti-hypertensive agents NSAIDs Adverse effects 3.) Analgesic nephropathy - due to long term ingestion of mixtures of agents - chronic interstitial nephritis, renal papillary necrosis, acute renal failure NSAIDs Non selective Vs selective COX2 inhibitors ↑ risk of cardiovascular adverse events with COX 2 inhibitors Rofecoxib was withdrawn from the market Higher BP, incidence of myocardial infarction, stroke Mechanism _ ? Unopposed effect of cox 1 action - ? Block protective effect of COX2 on ishaemic myocardium or atherogenesis OPIOID ANALGESICS SOURCE Opium is obtained from the opium poppy by incision of the seed pod after the petals of the flower have dropped. The white latex that oozes out turns brown and hardens on standing. This sticky brown gum is opium. It contains about 20 alkaloids, including morphine, codeine etc. The principal alkaloid in opium is morphine, present in a concentration of about 10%. OPIOID AGONISTS Morphine (strong mu receptor agonist) Codeine Heroin Meperidine (pethidine) Fentanyl Loperamide (over the counter for diarrhea) Diphenoxylate Dextromethorphan OPIOID AGONIST-ANTAGONIST /PARTIAL AGONIST Nalbuphine Pentazocine OPIOID ANTAGONISTS Nalorphine Naloxone Naltrexone OPIATE ANALGESICS Routes of administration Oral Parenteral Suppositories Transdermal- Patch s/c Syringe driver Opioid Analgesics-Pethidine Pethidine/meperidine and fentanyl are the most widely used agents in this family of synthetic opioids The principal effects of pethidine with affinity for mu receptors are on the central nervous system. Pharmacological Effects • the pharmacological effects of Pethidine is similar to morphine, primarily at the mu receptor •it has less potent analgesics than morphine and has a shorter duration of action •Pethidine dosn`t delay delivery The Opioid Antagonists The opioid antagonist drugs naloxone and naltrexone are morphine derivatives. When given in the absence of an agonist drug these antagonists are almost inert at doses that produce marked antagonism of agonist effects. When given intravenously to a morphine-treated subject, the antagonist will completely and dramatically reverse the opioid effects within 1-3 min. Mechanism of action Opioid agonists produce analgesia by binding to specific receptors, located primarily in brain and spinal cord regions involved in the transmission and modulation of pain. Mechanism of action Receptor types: The major classes of receptors are µ (mu for morphine) delta (δ) Kappa (κ) All are members of the G-proteincoupled family of receptors. Mechanism of action Analgesia, as well as the euphoriant, respiratory depressant, and physiologic dependence properties of morphine result principally from actions at mu receptors. Most of the currently available opioid analgesics act primarily at the mu receptor. OPIOID RECEPTORS Certain opioid receptors are located: on primary afferent and spinal cord pain transmission neurons (ascending pathways) in the midbrain and medulla (descending pathways) that function in pain modulation All 3 receptors appear to be involved in anti nociceptive and analgesics mechanisms OPIOID RECEPTORS Presynaptically: Opioid receptor activation can close voltage – gated calcium ion channels to inhibit neurotransmitter release (serotonin, glutamate and substance P) OPIOID RECEPTORS Postsynaptically: Activation of these receptors can open potassium ion channels to cause membrane hyperpolarization (inhibitory post synaptic potential). Direct inhibition of neurons in ascending pathways PHARMACOLOGICAL EFFECTS CNS: Analgesia: most powerful drug available for relief of pain Euphoria: addict experiences a pleasant floating sensation and freedom from anxiety and distress. Sedation Respiratory depression: main cause of death from opioid overdose due to reduced responsiveness of respiratory centre in brainstem to blood levels of CO2 PHARMACOLOGICAL EFFECTS Increase arterial CO2 retention causes cerebral vasodilation resulting in increase intracranial pressure Cough suppression: suppression of cough centre in nucleus of tractus solitarius Miosis: results from stimulation of Edinger- Westphal nucleus causing pin-point pupils except meperidine. Emesis: due to stimulation of brainstem chemoreceptor trigger zone results in nause and vomiting MIOSIS PHARMACOLOGICAL EFFECTS CVS: No significant direct effect on CVS Hypotension may occur if CVS is already stressed. Due to the peripheral arterial and venous dilation resulting from histamine release. GIT: Decrease intestinal propulsive peristalsis and stomach motility leads to constipation Biliary tract: Constriction of biliary smooth muscles leads to biliary colic except meperidine Constriction of sphincter of oddi leads to increase biliary pressure, reflux of biliary and pancreatic secretions and elevated plasma and lipase levels PHARMACOLOGICAL EFFECTS Renal functions: depressed due to decrease renal plasma flow. Also has antidiuretic effect. Mechanism involve both CNS and peripheral site Ureteral and bladder tone is increased Increased sphincter tone….urinary retention Occasionally, ureteral colic caused by renal calculus is made worse by opioid induced increase in ureteral tone PHARMACOLOGICAL EFFECTS Uterus: decrease uterine tone lead to prolong labor Skin: flushing and warming, sweating, itching due to histamine release CLINICAL USES Analgesia for MI terminal illness surgery obstetrical procedures cancer Cough Diarrhea CLINICAL USES Acute pulmonary edema: decrease dyspnea Proposed mechanism: Reduced anxiety (perception of shortness of breath) Reduced cardiac preload (reduced venous tone) Reduced afterload (decreased peripheral resistance) If respiratory depression is there then use furosemide Clincal Use The major application of naloxone is in the treatment of acute opioid overdose In individuals who are acutely depressed by an overdose of an opioid, the antagonist will effectively normalize respiration, level of consciousness, pupil size More recently, considerable interest has been aroused by reports that naltrexone decreases craving for alcohol in chronic alcoholics, and it has been approved by the FDA for this purpose. ADVERSE EFFECTS OPIOID ANALGESICS Morphine Morphin 6 glucuronid - 3.7 s.c. 45 i.c.v. Foley 1993 Dosage form with slow release Bashford 2001 Roxanol SR (8 ore) MS Contin (12 ore) MST Heroine – metabolit: Morphine im 2 - 6 acetil morphine (link to opioid receptors) OPIOID ANALGESICS Hydromorphon 5 - benefits the elderly (t1/2 1.5-2 ore) - excellent analgesia - minimal side effects (Brose 1991) Levorphanol 2 - in chronic pain who can not tolerate morphyne - affinity for receptor Codeine – for stage II– in combinations DH codeina Oxycodone 10 codeine – moderate and severe pain - present in combination OPIOID ANALGESICS Meperidine – 75 mg = 10 mg morphine i.m. - normepteridine: activ metabolit – convulsant 2 - analgezic ½ Metadone - 10mg = 10mg morphine - analges stage II - addiction therapy Propoxifen – moderate pain 1/2 – 1/3 from codeine -metabolit: norpropoxifen (convulsant) Fentanyl – 1:20, 1:30 from morphine - intra and post operative pain - various routes of administration - inactive metabolites AGONISTS /ANTAGONISTS Pentazocine 35 mg = 10 mg morphine. Receptors , BP – disphoria, psyhotic effects Nalbufina – equivalent to morphine - for postoperative pain effects) - substitute for morphine (fewer side - lower potential for abuse as morphine - Potential low psyhotic edffect Butorfanol – 2 mg i.m. = 10 mg morphine - low physical dependence potential - useful for acute pain in patients who have not received opioids TOLERANCE TOLERANCE Tolerance occur due to receptor uncoupling. Physical dependence: It results in withdrawal (abstinence) syndrome if there is failure to continue administer drug. Sudden withdrawal (abstinence syndrome) has following signs/symptoms: lacrimation yawning chills hyperventilation hyperthermia diarrhea,vomiting anxiety SYMPTOMS OF WITHDRAWAL TOLERANCE Psychological dependence: euphoria indifference to stimuli sedation Morphine poisoning….antidote is naloxone Toxicity Acute morphine poisoning: Coma Severe respiratory depression Miosis with blood pressure decreased Urinary retention. Respiratory paralysis often is the mainly lethal reason. Treatment: respiratory support intravenous injection of naloxone.