* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Lyme Disease Signs and Symptoms
Innate immune system wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Atherosclerosis wikipedia , lookup
Neonatal infection wikipedia , lookup
Sociality and disease transmission wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Infection control wikipedia , lookup
Transmission (medicine) wikipedia , lookup
Onchocerciasis wikipedia , lookup
Germ theory of disease wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Chagas disease wikipedia , lookup
Mass drug administration wikipedia , lookup
Childhood immunizations in the United States wikipedia , lookup
Schistosomiasis wikipedia , lookup
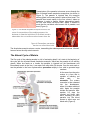
Lyme disease: a complex interaction between reservoirs en route to human infection. Lyme disease is currently one of the Center for Disease Control’s Top 10 emerging infectious diseases worldwide. It can be caused by at least 3 different Borrelia bacteria, which are Gram-negative spirochetes (spirilla). In the US Borrelia burgdorferi sensu lato is chiefly responsible. Lyme disease is named after the village of Lyme, Connecticut, where a cluster of cases was diagnosed in 1975. Intensive investigation into the cause began immediately. It was soon established that Lyme disease is carried by ticks; in fact it is the most common tick-borne disease in the Northern Hemisphere. Figure 1: Borrelia burgdorferi the major cause of Lyme disease in the Lyme disease is causing focal epidemics as it spreads in US1. the northeastern and upper midwestern US. These epidemics are thought to be a result of the large increase in deer in areas where humans are living. The deer tick needs the white-tailed deer to reproduce successfully. Reducing the numbers of primary hosts may help break the deer tick reproductive cycles and their ability to flourish in suburban and rural areas. In the US it has been suggested that reducing the deer population in areas with the highest Lyme disease rates from current levels of 60 or more deer per square mile to 8 to 10 per square mile could reduce tick numbers down to levels too low to spread Lyme and other tick-borne diseases. Lyme disease is a zoonosis, that is, B. burgdorferi is transmitted to humans and deer from a natural reservoir among rodents by the hard-bodied deer ticks that feed on both sets of hosts. Deer are the most common hosts for adult stage ticks; humans are “accidental” hosts because the bacteria from infected people are not transmitted to other hosts. B. burgdorferi bacteria are transmitted from nymph ticks to rodents like the white-footed mouse, and then back to larval ticks. The transmission is essential to maintain a reservoir of B. burgdorferi because there is no direct transmission of bacteria from female tick to her offspring. Rodents therefore form an essential bridge that allows bacteria to be transmitted from one generation of deer tick to the next. It works like this: The nymph tick typically feeds on the rodent for several days, so that it becomes chronically infected with B. burgdorferi, particularly in the skin. Figure 2: Black legged deer ticks maintain the Then the rodent efficiently passes the reservoir of B. burgdorferi in nature. The Nymph form bacteria back to the next generation of is most responsible for human infection because it is uninfected ticks when they are fed so small it often goes unnoticed. upon again months later. 1 The vector The nymph tick (as shown in figure 2) is also the major vector that transmits the bacteria to humans. When the tick bites a human two important events occur: First, the B. burgdorferi , still in the tick is exposed to warm mammalian blood. This causes it to change the surface protein it produces to a form that helps it transmit to humans. If the feeding ticks are removed before this activation within the tick is complete, i.e. within 24-36 hours, the bacteria will not transmit successfully to humans. In fact, human infection is quite rare, with only about 1% of recognized tick bites resulting in Lyme disease. The second event is that B. burgdorferi is injected into the human along with tick saliva. The saliva contains substances that disrupt the immune response at the site of the bite preventing the host feeling an itch or pain from the bite, and providing a protective environment that allows the bacteria to survive. Figure Error! No text of specified style in document.: The Life-cycle of Lyme Disease. The 2-year cycle of deer ticks has four stages: eggs, larvae, nymphs, and adults (as shown in figure 2). Larvae hatch in the summer. They are uninfected, but soon acquire B. burgdorferi by feeding on infected rodents. The infected larvae molt into nymphs in the fall and are dormant through the winter. Infected nymphs feed on rodents in the late spring and early summer. This sets up a natural reservoir of B. burgdorferi. The chronically infected rodents then transmit B. burgdorferi to the next generation of The natural larval-stage cycle of B. ticks. burgdorferi is ticks important in how disease inoccurs. First, Lyme uninfected Nymph can also feedLyme on humans the late spring disease is endemic only in regions were all the essential elements of the natural cycle exist, and summer causing a peak of human Lyme disease. The nymph ticks molt into adultsi.e. in the fall - their preferred host is deer. 2 the northeast and mid-Atlantic coastal states, and the Great Lakes regions in the US. Second, most human infections occur in the spring and summer months, when outdoor activities bring people into contact with feeding nymph ticks. These ticks are extremely small (approximately 1 mm in length) and are often not discovered for several days, allowing the B. burgdorferi to be activated and transmitted. Lyme Disease Signs and Symptoms Like syphilis, which is also caused by B. burgdorferi bacteria, Lyme disease progresses through several stages and affects many organs. The incubation period from infection to the onset of symptoms is usually one to two weeks, but can be much shorter (days), or much longer (months to years). The classic sign of Stage 1 infection is a circular ‘bull’s eye’ rash at the site of the bite caused by an inflammatory response to the bacteria. The ‘bull’s eye’ rash is seen in about 80% of patients. During Stage 2 the bacteria enter the bloodstream and spread to the joints, heart, nervous system, and distant skin sites where they cause a variety of symptoms such as fever, headache, muscle soreness and fatigue. Some patients also suffer from neurological problems like facial paralysis (Bell’s palsy) and encephalitis leading to memory loss. Left untreated, Stage 2 symptoms may progress to Stage 3 that involves chronic inflammation of the joints, the heart, the central nervous system and the skin. (this process if summarized in Figure 4). Figure 4: Stages of Lyme disease: Lyme can persist for many years and infects a large number of organs. It can be extremely difficult to eradicate once the bacteria have entered the brain, joints and heart. Diagnosing Lyme Disease Lyme disease is usually first diagnosed by the ‘bulls eye’ rash, facial paralysis or arthritis together with a history of possible exposure to infected ticks. Most but not all patients with Lyme disease will develop the bulls-eye rash, but many may not recall a tick bite. Since Borrelia bacteria are very hard to grow in the laboratory, serological tests measuring antibody levels are used to confirm infection. Clinical samples are taken from blood or from cerebrospinal fluid (CSF) via lumbar puncture. Unfortunately, the blood screens only detect 64% of all infections at early stages of the disease. This rises to 100% in people with advanced symptoms, such as arthritis. For this reason more sensitive and accurate methods of identification are needed. 3 Preventing Lyme Disease Infection Personal Removing ticks within 36 hours can reduce transmission rates to close to zero. Protective clothing should include a hat and long-sleeved shirts and long trousers that are tucked into socks or boots. Outdoor pets can bring ticks into the house. Treatment Antibiotics are the primary treatment for Lyme disease, but not always very effective. Up to one third of Lyme disease patients who have completed a course of antibiotic treatment continue to have symptoms. A few doctors attribute these symptoms to persistent infection with Borrelia, or coinfection with other tick-borne infections. Other doctors believe that the initial infection may cause an autoimmune reaction that continues to cause serious symptoms even after the bacteria have been eliminated. Lyme Disease vocabulary Figure 5: Adult ticks overwinter on white-tailed deer, which are pests in areas were Lyme disease is endemic Gram-negative Spirochete Zoonosis, Borella burgdorferi Endemic Inflammatory response Neurological problems Encephalitis Serological tests Cerebrospinal fluid (CSF) Lumbar puncture Autoimmune reaction 4 Malaria: The most important of all the parasitic diseases Malaria, the most important of all parasitic diseases, occurs in many tropical and semitropical regions. There are approximately 200 million to 300 million new cases annually, and an estimated 2 million to 3 million people die of malaria each year. About 89% of these deaths occur in Africa, and mostly to children under the age of 5. Of all infectious diseases malaria is considered to have caused the greatest harm to the greatest number of people. Malaria was endemic in some areas of the US in the 1800s but has since been eradicated with DDT (as discussed later). Currently, the 1000 or so cases that are diagnosed in the US arise from travelers who have been in an endemic area, or, rarely from infected mosquitoes that have arrived in planes. But this may not necessarily continue. If climate change continues along its current trajectory mosquitoes are expected to regain a foothold in many areas (in red on the map) currently considered too temperate to support them. Figure 1: Climate Change and Malaria The Malaria parasite and its vector Malaria in humans is caused by 4 species of parasites: Plasmodium protozoa ( P. falciparum, P. vivax, P. ovale, and P. malariae). The four species vary in their ability to cause disease because they prefer red blood cells of different ages. Plasmodium falciparum is the most deadly because it invades red blood cells of all ages. Figure 2: Plasmodium falciparum, one of the 4 plasmodium protozoa that causes malaria seen in a blood culture with red blood cells 5 Transmission of the parasite to humans occurs through the bite of infected female anopheles mosquitoes (as shown in Figure 3). The parasite is injected from the mosquito salivary gland into humans when it takes a blood meal. The parasite then travels rapidly to the liver, where it takes up residence in order to mature. Mature plasmodium leaves the liver and enters red blood cells, where it divides so much that the red blood cells become full of parasite, and burst (Figure 4). Figure 3: The female anopheles mosquito that acts as a vector for transmission of the malaria protozoa. Her abdomen is distended with blood. If the blood contains plasmodium she can reinfect another human when she feeds again. Figure 4: Plasmodium merozoites bursting out of red blood cells. The Anopheles mosquito acts as a vector, transmitting the malaria parasite to humans. Infected humans act as the only actual reservoir. The Natural Cycle of Malaria The life cycle of the malaria parasite is rich in fascinating detail. Let’s start at the beginning of the cycle with the infected female Anopheles mosquito, which has the parasite in her salivary glands. When she feeds on a human the parasite is injected into the bloodstream and immediately travels to the liver. It can enter liver cells within 30 minutes. Over the next week or two the parasite in the form of plasmodium sporozites multiply in liver cells to generate large numbers. At the same time they also mature to a form that is capable of infecting red blood cells the merozoite. The mature merozoite is then released into the bloodstream, where it invades red blood cells. Again the parasite divides and matures. After another 2-3 days the infected red blood cells burst, releasing yet more parasite into the blood stream to infect more red blood cells (Figure 5). 6 Figure 5: Life cycle of the Plasmodium parasite. While this is happening a small number of the merozoites develop further into male and female forms. If a mosquito feeds again from the human reservoir it can take in the male and female forms. They then develop in the mosquito into the sporozites and the cycle repeats itself. Malaria Signs and Symptoms The symptoms of malaria are intense and generally show up within a month of infection as a very high fever, chills and, later on, anemia (low numbers of red blood cells). The symptoms coincide with the release of large numbers of merozoites from the red blood cells, and occur because the immune system has recognized the presence of a foreign invader and has put its defense mechanisms on high alert. After the first parasites replicate in the red blood cells, the infection becomes synchronized so that all infected red blood cells lyse at the same time. Other symptoms of malaria are also caused by the immune system response and resemble influenza (fever, muscle aches and generally feeling ill). Stomach pain can also occur because of liver damage. Patients with symptoms of malaria are often misdiagnosed, especially if they don’t live where malaria is endemic and if the physician does not ask about travel. Diagnosing Malaria Malaria is diagnosed in the laboratory by taking a thick smear of blood (8-12 cells deep) onto a microscope slide and then using a Giemsa stain, which dyes the plasmodium merozoites blue (As shown in Figure 6). Different types of plasmodia give different patterns of staining. PCR analysis is more accurate than blood tests but is expensive and requires expertise. It isn’t useful in developing countries. Unlike Lyme disease serological testing for malaria antibodies is of little use for someone with acute infection because antibodies to the parasite do not develop for 3 – 5 weeks, but treatment must begin within 1 – 2 days to stop the infection from spreading to the liver. Figure 6: Giesma stain of thin blood film showing P.falciparum merozoites infecting red blood cells Treatments and Prevention Natural immunity to malaria is imperfect. The malaria parasite has evolved several strategies to evade the immune system. As a result, people who have lived where malaria is endemic all their lives and show evidence of immune response will nonetheless still get infected on a regular basis. However their infections are usually less severe, suggesting that the immune system can control the infection somewhat. Antimalarial drugs are based on quinine (a molecule isolated from tree bark), which stops the parasite from degrading the hemoglobin in red blood cells, thereby blocking a major source of nutrition. The major antimalarial drug used to be chloroquine, a quinine derivative, which accounts for the popularity of gin and tonic in the tropics - tonic contains quinine (Figure 7). Unfortunately, the parasite can develop resistance to the drug. Chloroquine-resistant malaria is 7 now widespread in most of Southeast Asia, South America and Africa, and a cocktail of other anti-malarials a must be used. Figure 7: Gin and tonic was a popular cocktail in the tropics because tonic contains quinine – at the time an effective antimalarial Malaria Control - DDT - For and Against Malaria remains a major public health challenge in many parts of the world. The World Health Organization (WHO) estimates that in 2008 there were 243 million cases, resulting in 863,000 deaths. One way to eliminate infection is to eradicate the mosquito vector. Spraying with pesticide, especially DDT has been effective but controversial: Its use in this context has been called everything from a "miracle weapon [that is] like Kryptonite to the mosquitoes," to "toxic colonialism”. DDT (dichlorodiphenyltrichloroethane) was first used with great success to control malaria among civilians and troops in the second half of World War II. In response the WHO started an anti-malaria campaign in the 1950s and 1960s that relied heavily on DDT. Initially the results were promising. For example, in Sri Lanka, the program reduced cases from about 3 million per year before spraying to just 29 in 1964. Then the program was halted to save money, and malaria rebounded to 600,000 cases in 1968 - 1969. About the same time public awareness that DTT can persist in both humans and the environment led many governments to restrict or curtail its use. Once the mainstay of anti-malaria campaigns, as of 2008 only 12 countries still use DDT, including India and some southern African states. Figure 8: After DDT was a success against malaria and typhoid in WW2 the WHO instigated malaria eradication programs to spray mosquitoes. There is no doubt that when used properly DTT can significantly curb malaria, however DDT resistance in mosquitoes, which is largely due to its overuse in agriculture, has greatly reduced its effectiveness in many parts of the world. Current WHO guidelines require that before DTT is used in any area it must first be confirmed that local mosquitoes are susceptible to it. Some countries that still use DDT have shown that alternative insecticides are less effective – in South Africa malaria incidence increased dramatically when the insecticide was switched, but returning to DDT and introducing new drugs brought malaria back under control. Similarly malaria cases increased in South America after DDT use was stopped. Between 1993 and 1995 Ecuador increased its use of DDT and saw a 61% reduction in malaria rates, while other countries that gradually decreased DDT use at the same time saw large increases in malaria. 8 For spraying to be effective, at least 80% of homes and barns in an area must be sprayed, so if enough residents refuse spraying, the effectiveness of the whole program can be jeopardized. Resistance to DDT spraying comes from the realization that people living in spraying areas have levels of DTT and its breakdown products in their bodies that are several orders of magnitude higher than people who live elsewhere. In addition, animal studies have shown that DTT is a carcinogen. And there is also some evidence in humans that DDT can cause cancer of the liver pancreas and breast. Figure 10: A mosquito bed net soaked in Currently DDT remains on the WHO's list of insecticide can give reasonable recommended insecticides and its policy has protection, if used properly, for $5. shifted from recommending spraying only in areas of seasonal or episodic transmission of malaria, to also advocating it in areas of continuous, intense transmission, so DDT use is expected to rise. The major reason is the failure to curtail malaria through drug treatment to kill the parasite, because of the increasing prevalence of drug-resistant forms. Malaria vocabulary Endemic Plasmodium protozoa Salivary gland Anopheles mosquito Sporozite Merozoite Giemsa stain PCR analysis Serological tests Chloroquine DDT (dichlorodiphenyltrichloroethane) Carcinogen. 9